Pan-cancer efficacy of pralsetinib in patients with RET fusion–positive solid tumors from the phase 1/2 ARROW trial
Published in Cancer
Tissue agnostic treatment for RET fusion–positive solid tumors
Historically, cancers have been classified and treated based on the site of origin e.g., lung, breast, thyroid etc. With the arrival of powerful next generation sequencing technologies that have unravelled the molecular underpinnings of cancer, a different approach to treating cancers is emerging, one based on the underlying genetic abnormalities. There is emerging data that many of these alterations are present across tumor types and this has led to tissue agnostic drug development.
Activating RET fusions have been seen in the development of many variations of solid tumors, including non-small cell lung cancer (NSCLC; 1–2%), papillary thyroid cancer (20%), ovarian cancer, pancreatic cancer, and colorectal cancer (all <1%).1-5 An unmet need exists for therapies that can target RET with high potency and selectivity across a broad range of tumor types. Pre-clinical and early data indicated that RET fusions are potential targets for selective RET inhibitors and several tumor-agnostic drug approvals have brought the development of versatile, molecularly targeted therapies to the fore.6-10 In our study, that was published and featured in the cover image in Nature Medicine (https://www.nature.com/articles/s41591-022-01931-y), the drug was pralsetinib, a selective and potent inhibitor of RET kinases, including RET fusion proteins, which had been approved in several indications including metastatic RET fusion–positive NSCLC, advanced or metastatic RET-mutant medullary thyroid cancer, and RET fusion–positive thyroid cancer in the USA,11 and advanced RET fusion–positive NSCLC in the EU.12 As a subsequent step to these approvals and the encouraging data shown in these trials, we aimed to evaluate efficacy and safety data of pralsetinib in a population of patients with a variety of RET fusion–positive solid tumors in a tissue agnostic manner excluding NSCLC and thyroid cancer.

Pralsetinib for a diverse range of tumors
We administered pralsetinib to 29 patients from a specific subgroup of the open-label, international, phase 1/2 ARROW study (NCT03037385) to assess their response and safety characteristics. Twenty-eight of these patients were administered with starting doses of 400 mg once-daily, the recommended phase 2 dose determined in phase 1 of ARROW,13 whilst one patient was carried over from this dose escalation phase and therefore received 200/100 mg twice-daily initially before transitioning to 400 mg once-daily. Twelve tumor types were treated including pancreatic, cholangiocarcinoma, neuroendocrine, sarcomas, head and neck, colorectal, small cell lung, an unknown primary tumor, gastric, ovarian, thymic and central nervous system tumors. Twenty-three patients were assessed for tumor response and measures of overall and progression-free survival based on criteria developed in the course of the study protocol. The key primary endpoint of this study was overall response rate (ORR) per Response Evaluation Criteria in Solid Tumors version 1.1.
What do our findings show?
Irrespective of tumor type or RET fusion partner, pralsetinib exhibited robust and durable antitumor activity with tumor shrinkage observed in all but 2 patients out of the 23 evaluated for efficacy (Figure 1). An ORR of 57% was observed for pralsetinib in these RET fusion–positive tumor types, compared to previously published data from ARROW where ORRs of 61% and 70% for RET fusion–positive NSCLC patients who received prior platinum therapy and no prior systemic treatment,13 respectively, and an ORR of 89% for RET fusion–positive thyroid cancer patients, were observed.14 Of the patients with tumor responses, we identified 3 patients that stood out and had experienced limited success with prior therapies until treatment with pralsetinib. The first, a man in his early 30s with pancreatic cancer and multiple metastases, had progressed and experienced toxicity on 1 prior line of chemotherapy (capecitabine), but experienced a 100% decrease in target lesions and an ongoing complete response (CR) after 33.1 months of pralsetinib treatment. An intrahepatic cholangiocarcinoma patient in her early 50s with liver and bone metastases had experienced progressive disease (PD) on all 3 prior lines of therapy (gemcitabine/cisplatin/abraxane, erlotinib/bevacizumab, osimertinib), but had continued tumor shrinkage to a maximum 77% reduction after 20.7 months of pralsetinib before disease progression (Figure 2a and 2b). Before enrolment to the clinical trial the patient’s performance status was rapidly declining and was wheelchair bound. After initiation of therapy she experienced a dramatic clinical recovery, that she could go on a skiing trip. This once-a-day oral targeted therapy undoubtedly conferred clinical benefit and the “gift of time” to the patient and the family.
The final patient was in her early 60s, had a sarcoma and had progressed on first-line imatinib, another tyrosine kinase inhibitor, but experienced a partial response after 1.9 months of pralsetinib which evolved to an ongoing CR after 19.4 months (Figure 2c).
Notably, all 4 patients with pancreatic cancer and 2 of 3 patients with cholangiocarcinoma experienced a response, which highlighted the potential of pralsetinib as a treatment option for these patients as their tumor types are notoriously difficult to treat. Standard-of-care therapies have shown response rates of only 26% in biliary cancer and 23–32% in pancreatic cancer.15-17 Selpercatinib, another RET inhibitor, has also displayed encouraging results in tumor agnostic studies across non-lung/non-thyroid RET fusion–positive solid tumors with an ORR of 47%,18 confirming RET fusions as a tissue agnostic target. In this study of pralsetinib, median duration of response, progression-free survival, and overall survival were 11.7, 7.4, and 13.6 months, respectively, and pralsetinib also had a consistent safety profile to NSCLC and thyroid cancer populations previously reported in ARROW with no new safety signals.13,14
A path to future research
Here, the heterogenous set of RET fusions and tumor types targeted by pralsetinib validate RET as a tumor agnostic target, with tumor shrinkage seen across all but 2 patients with tumors that differed in histology. Our findings open the door to further trials to investigate tumor agnostic therapies across various solid tumors that harbor RET fusions, and also blaze the broader trail for genomically targeted treatments following the identification of oncogenic drivers.
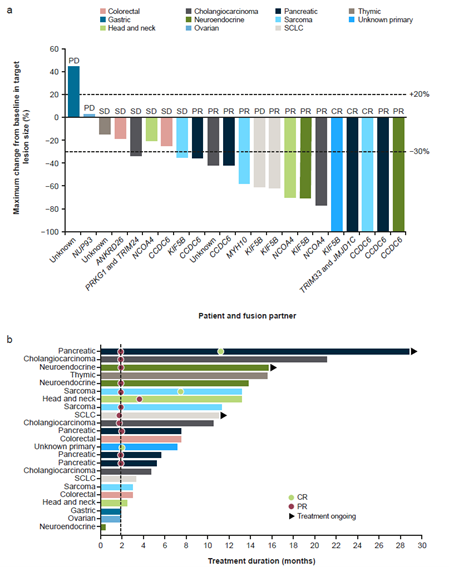
Fig. 1. Individual tumor response and treatment duration waterfall and swimlane plots for the efficacy-evaluable population. In 23 patients eligible for efficacy analyses: (a) tumor response by blinded independent central review and maximum change from baseline in target lesion size, showing each patient’s tumor type and RET fusion partner; (b) treatment duration, indicating the corresponding tumor type and the timeline for response, where the dotted line represents median time to response (1.9 months). One patient with progression based on a new site of disease did not have post-baseline assessment of RECIST target lesions, and so is not shown in Figure 1a. CR, complete response; PD, progressive disease; PR, partial response; SCLC, small-cell lung cancer; SD, stable disease.
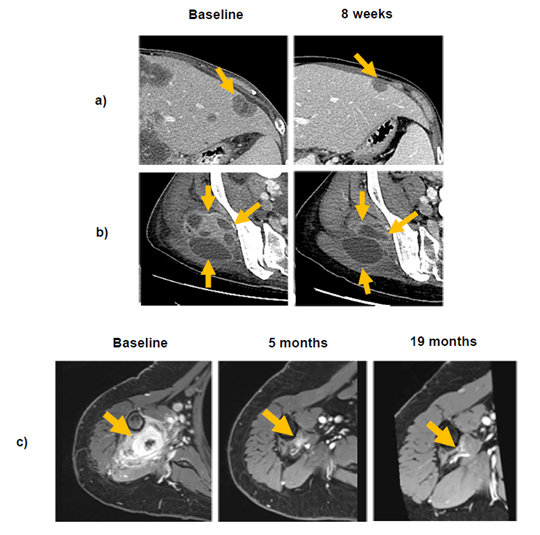
Fig. 2. Time-dependent disease evaluations in two patients following pralsetinib treatment. Baseline and 8-week disease evaluation in a 51-year-old woman with RET-NCOA4 fusion–positive cholangiocarcinoma: (a) at first disease evaluation after 8 weeks receiving pralsetinib, a left hepatic lobe lesion measuring 2×3 cm at baseline had reduced to 1.2×1.9 cm; (b) a prior heterogeneously enhancing soft tissue mass in the right gluteal muscles had decreased in size and enhancement, and showed increased cystic and necrotic components compared with baseline scans. (c) Baseline, 5-month, and 19-month disease evaluation in a 60-year-old woman with a RET-CCDC6 fusion–positive sarcoma presenting as 2 muscular masses in the right upper arm.
References
- Kato, S. et al. RET aberrations in diverse cancers: next-generation sequencing of 4,871 patients. Clin Cancer Res 23, 1988-1997 (2017).
- Ciampi, R. & Nikiforov, Y.E. RET/PTC rearrangements and BRAF mutations in thyroid tumorigenesis. Endocrinology 148, 936-941 (2007).
- Kohno, T. et al. KIF5B-RET fusions in lung adenocarcinoma. Nat Med 18, 375-377 (2012).
- Lipson, D. et al. Identification of new ALK and RET gene fusions from colorectal and lung cancer biopsies. Nat Med 18, 382-384 (2012).
- Le Rolle, A.F. et al. Identification and characterization of RET fusions in advanced colorectal cancer. Oncotarget 6, 28929-28937 (2015).
- Looney, A.M., Nawaz, K. & Webster, R.M. Tumour-agnostic therapies. Nat Rev Drug Discov 19, 383-384 (2020).
- Genentech USA Inc. ROZLYTREK (entrectinib) capsules. Prescribing information, https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/212725s000lbl.pdf (2019, accessed April 14, 2020.
- Bayer Healthcare Pharmaceuticals Inc. VITRAKVI (larotrectinib). Prescribing information, http://labeling.bayerhealthcare.com/html/products/pi/vitrakvi_PI.pdf (2020, accessed May 13, 2020.
- MSD Corp. KEYTRUDA (pembrolizumab) injection. Prescribing information, https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/212725s000lbl.pdf (2019, accessed April 14, 2020.
- GlaxoSmithKline. JEMPERLI® (dostarlimab-gxly). Prescribing information, https://www.accessdata.fda.gov/drugsatfda_docs/label/2020/761223s000lbl.pdf (2021, accessed October 2021.
- Blueprint Medicines Corporation. GAVRETO® (pralsetinib). Prescribing information, https://www.accessdata.fda.gov/drugsatfda_docs/label/2020/214701s000lbl.pdf (2020, accessed December 2020.
- Roche Registration GmbH. GAVRETO (pralsetinib). Summary of Product Characteristics, https://www.ema.europa.eu/en/documents/product-information/gavreto-epar-product-information_en.pdf (2021, accessed December 13, 2021.
- Gainor, J.F. et al. Pralsetinib for RET fusion-positive non-small-cell lung cancer (ARROW): a multi-cohort, open-label, phase 1/2 study. The Lancet Oncology 22, 959-969 (2021).
- Subbiah, V. et al. Pralsetinib for patients with advanced or metastatic RET-altered thyroid cancer (ARROW): a multi-cohort, open-label, registrational, phase 1/2 study. Lancet Diabetes Endocrinol 9, 491-501 (2021).
- Valle, J. et al. Cisplatin plus Gemcitabine versus Gemcitabine for Biliary Tract Cancer. New England Journal of Medicine 362, 1273-1281 (2010).
- Conroy, T. et al. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. New England Journal of Medicine 364, 1817-1825 (2011).
- Von Hoff, D.D. et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. New England Journal of Medicine 369, 1691-1703 (2013).
- Subbiah, V. et al. Efficacy and Safety of Selpercatinib in RET Fusion-Positive Cancers Other than Lung or Thyroid Cancers. in Annual Meeting of the American Association for Cancer Research (Virtual, 2021).
Follow the Topic
-
Nature Medicine
This journal encompasses original research ranging from new concepts in human biology and disease pathogenesis to new therapeutic modalities and drug development, to all phases of clinical work, as well as innovative technologies aimed at improving human health.
Related Collections
With Collections, you can get published faster and increase your visibility.
Microbiome and energy metabolism
Publishing Model: Hybrid
Deadline: Dec 06, 2026
The expanding therapeutic landscape of GLP 1 receptor agonists
Publishing Model: Hybrid
Deadline: Jan 23, 2027





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in