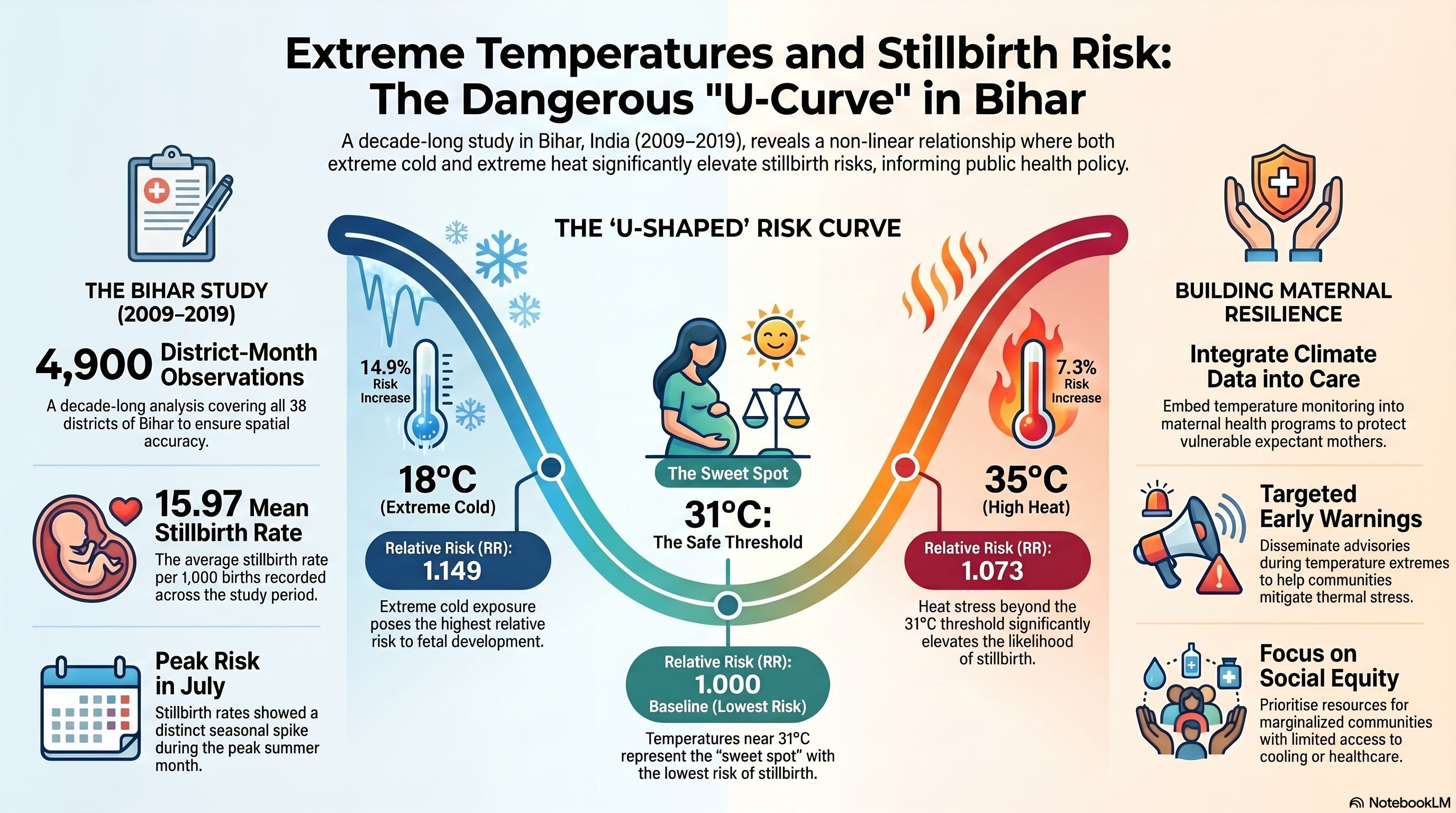
🌡️ The Thermal Squeeze on Maternal Health: Extreme Temperatures and Stillbirth Risks in India 🤰🏾
Published in Public Health
Follow the Topic
-
BMC Pregnancy and Childbirth
This is an open access, peer-reviewed journal that considers articles on all aspects of pregnancy and childbirth. It welcomes submissions on the biomedical aspects of pregnancy, breastfeeding, labor, maternal health, maternity care, trends and sociological aspects of pregnancy and childbirth.
Related Collections
With Collections, you can get published faster and increase your visibility.
Respectful maternity care - Part II
BMC Pregnancy and Childbirth is calling for submissions to our Collection on Respectful maternity care - Part II.
The World Health Organization defines respectful maternity care (RMC) as care that maintains dignity, privacy, and confidentiality of pregnant and birthing women, ensures freedom from harm and mistreatment, and enables informed choice and continuous support during labor and birth. RMC is considered a fundamental human right. Despite the acknowledged importance of providing RMC to all women, many women still experience disrespect and abuse during labor and birth across global contexts.
BMC Pregnancy and Childbirth is calling for submissions on ‘Respectful maternity care’ to bring together research on the benefits of respectful maternity care and the challenges in its implementation, both at the provider level and the system level. Both qualitative and quantitative research are welcome. Topics of interest include, but are not limited to, prevalence of disrespect and abuse in maternity care, implementation of respectful maternity care, RMC and maternal and neonatal outcomes, interventions to enhance and promote RMC, RMC in postnatal care, and effective communication and informed choice.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Aug 12, 2026
Innovations in successful pregnancies for patients with polycystic ovary syndrome
BMC Pregnancy and Childbirth is calling for submissions to our Collection on Innovations in successful pregnancies for patients with polycystic ovary syndrome.
Polycystic Ovary Syndrome (PCOS) is a prevalent endocrine disorder that affects a significant proportion of women of reproductive age and is associated with various reproductive and metabolic challenges. Women with PCOS are predisposed to difficulties in achieving and maintaining pregnancy due to factors such as hormonal imbalances, insulin resistance, and associated comorbidities. Recent advances in assisted reproduction technologies, lifestyle interventions, and personalized medicine have shown promise in improving obstetric outcomes and perinatal health for women with PCOS. Understanding the clinical strategies used to manage PCOS for maternal and fetal health is crucial for developing targeted strategies that enhance pregnancy outcomes.
The Collection invites researchers and clinicians in fields including obstetrics, maternal-fetal medicine, midwifery, endocrinology, neonatology, and gynecology to contribute research that explores topics including, but not limited to, evaluations of clinical practices for managing maternal PCOS, long-term health implications for both mothers and their offspring, the role of epigenetics in PCOS, innovative approaches to regulating insulin resistance, and the effectiveness of integrative medicine practices in improving reproductive health.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jun 30, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in