Why quality measures for chiropractic care are important and what we’re doing about it
Published in Healthcare & Nursing and Mechanical Engineering
Scientific evidence supporting chiropractic care has grown substantially over the past several decades. Likewise, care standards now describe key aspects of how care should be delivered. Though much more research will always be needed, current knowledge should not be ignored. Instead, there is a responsibility to pay attention to it, to use it to inform and improve clinical practice.
Quality improvement is a time-honored way to apply current knowledge to improve healthcare. It is achieved by measuring features of health organizations, clinical processes, outcomes, and patient experiences to obtain data about what is working well, what isn’t, and what changes are needed. Quality improvement depends on objective and valid measures called quality indicators/measures.
Why we started
Several years ago, we recognized that no broad set of quality measures for chiropractic care were available. Without these measures, quality improvement may not occur. Failing to act avoids an ethical obligation to objectively evaluate and improve care. Organizations that assessed quality lacked valid measures, which limited interpretation and prevented comparison across settings. Neither option adequately supported objective and sustained improvement over time.
In North America, the Council on Chiropractic Education (CCE) is the main accreditor for Doctor of Chiropractic degree and residency programs. Accredited programs must demonstrate quality improvement in clinical care settings. Standardized, evidence-based, and valid quality measures are ideal for supporting such processes. Several other reasons for developing quality measures include:
- Offering objective data on the effectiveness of care
- Revealing inefficiencies and ineffective policies, infrastructure, and practices
- Providing data to facilitate compliance with regulatory bodies
- Supplying a method to help assess chiropractic integration into a health organization
- Learning from patients about the experience of seeking and receiving care
- Informing strategic planning, policy development, resource allocation, and process adjustments
- Supporting a culture of continuous improvement
- Fostering patient and public trust
The validity of quality measures is compromised without transparency and input from key interest-holders. Therefore, we chose a stepwise and transparent process, published our findings in peer reviewed journals, and obtained input from relevant groups like researchers, providers, and administrators.
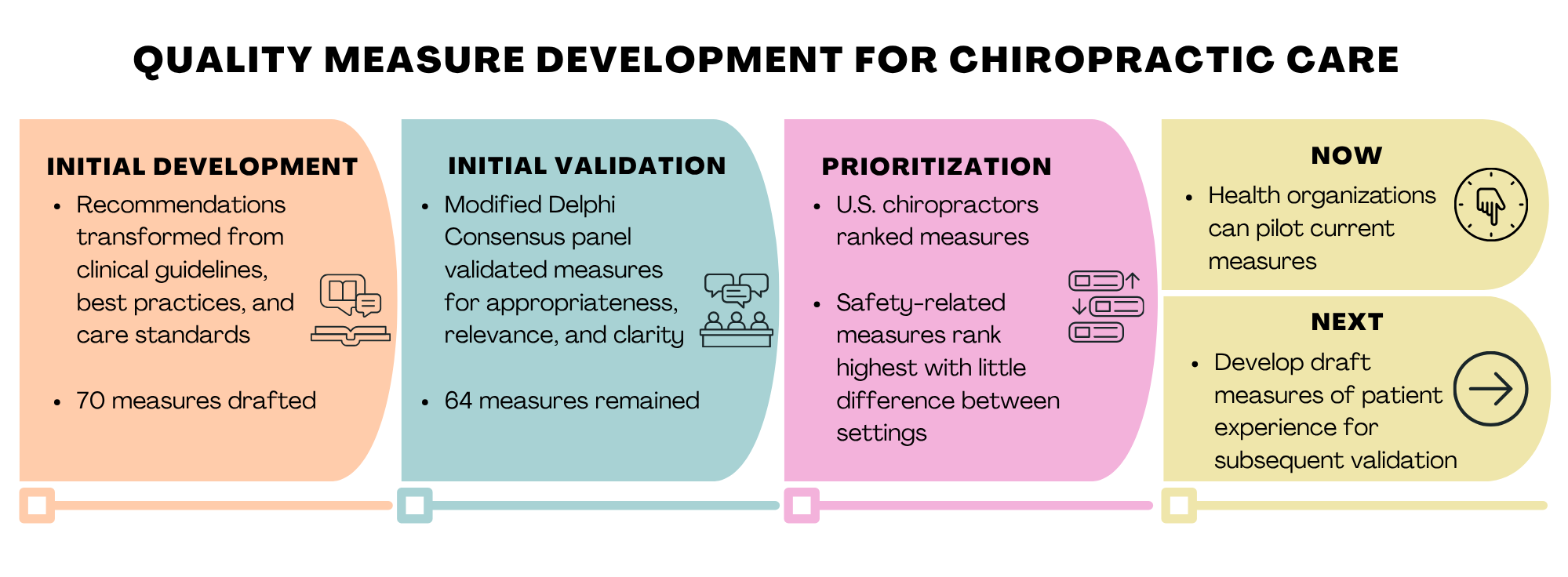
Preliminary measure development
Following published guidance on quality measure development, we conducted a scoping review to obtain current clinical guidelines, best practices, and care standards relevant to chiropractic care. We then transformed recommendations from these sources into a draft set of 70 measures. Because the measures were supported by scientific literature and care standards, some validity was already present. But greater validation was needed, requiring input from an essential group of professionals.
Initial validation
The next step was drawing from the wisdom of a select group of practitioners and administrators to validate the appropriateness, relevance, and clarity of draft measures. We accomplished this by convening a Modified Delphi Consensus panel comprised of 46 clinical administrators from CCE-accredited institutions and residency programs, and practitioners and administrators in integrated care settings. Panelists were invited because they worked in settings which use quality measures or other administrative data to assess care for accreditation and other regulatory purposes. After the process was complete, 64 measures remained.
Prioritizing
Though more validation is needed, the current set of 64 measures is ready for pilot testing. But which ones are best to start with? The technical capacity to measure clinical processes varies across organizations. Some measures are highly feasible, others less so. And though quality is a universal concept, patient population needs and organizational characteristics can influence the relative importance and feasibility of some measures.
Therefore, to address questions about prioritization and feasibility while also engaging a wider interest-holder group, we conducted a U.S. national survey of chiropractors. We included practitioners in different geographic regions and practice environments to understand if certain setting features substantially changed how practitioners prioritized individual measures.
Two main findings came from this effort. The first was that despite differences in geography and practice characteristics, respondents ranked the importance and feasibility of measures with a high level of agreement. The second was that most of the highest ranked measures were directly related to safety. These findings are consistent with the idea that safe care is a fundamental component of quality. Without safety, the effectiveness of care greatly suffers and the value of other components of quality (equity, efficiency, patient-centeredness, and timeliness) is markedly reduced.
Where do we go from here?
Developing quality measures is a meaningless effort if they aren’t used. We encourage health organizations offering chiropractic services to begin piloting current measures. Implementation will be more successful if carefully planned, focusing first on the policies and infrastructure needed to support clinical processes and outcomes. What is learned from piloting a few measures can inform and enable broader use over time while also providing data on real-world feasibility and utility.
Measure development is an ongoing process. Currently, a critical element is missing – patient perspectives. Patient experience measures assess what patients experience during care, offering data to understand the effectiveness of policies and processes intended to support quality. These measures differ from satisfaction, which can be high even with poor quality care. Our team is developing patient experience measures as a next step.
Quality measures are not developed, validated, or implemented quickly. Once developed, they require continual review to support ongoing validity, alignment with advancing scientific evidence, and feasibility. The work requires a sustained long-term effort, reflecting a commitment to help ensure patients remain the primary focus and principal beneficiaries of care.


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in