COVID-19 mRNA vaccine-induced memory T cells: strong preserved immune responses to Omicron
Published in Microbiology
Since the first report of coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection in December 2019, COVID-19 vaccines have been developed at an unprecedented pace and administered to large populations on a global scale. However, the pandemic continues due to the rapid decay of neutralizing antibodies (nAbs) and the emergence of variants, including the Omicron (B.1.1.529) variant. Substantial numbers of breakthrough infection cases have occurred following immunization with COVID-19 vaccines, raising doubts about the vaccines’ effectiveness. However, the current study revealed that COVID-19 mRNA vaccine-induced memory T cells exhibit strongly preserved responses to the Omicron variant1.
Viral infection or vaccination induces adaptive immunity that includes neutralizing antibodies and memory T cells. Neutralizing antibodies can directly block the process of viral entry to host cells. On the other hand, memory T cells, particularly CD8+ cytotoxic T cells, can selectively eliminate virus-infected cells and suppress further viral replication, contributing to recovery from the infection without progression to severe disease.
The Omicron variant, first reported in November 2021, exhibits over 30 mutations in the spike protein and infects host cells more efficiently than other variants. Therefore, it has rapidly replaced other variants and become the dominant SARS-CoV-2 strain worldwide. The Omicron variant frequently causes breakthrough infections among vaccinated individuals because this variant has the ability to extensively escape the neutralizing activities of vaccine-induced antibodies, although a third-dose booster vaccination increases neutralizing activities against the Omicron variant. To date, most studies of vaccine-induced immunity against the Omicron variant have focused on neutralizing antibodies, while relatively few studies have examined memory T cells, which also play a crucial role in anti-viral immunity.
Several SARS-CoV-2 variants show considerable evasion of the neutralizing activity of antibodies; however, it is more difficult for variants to completely escape T-cell responses because the spike protein has multiple T-cell epitopes, depending on each individual’s allotype of the human leukocyte antigen. When the Omicron variant was first reported, our laboratory conducted in silico analysis of the amino acid sequences of T-cell epitopes, which were previously identified from the ancestral SARS-CoV-2 strain, in the Omicron variant. We found that over 80% of T-cell epitopes in the spike protein, and over 95% in proteins other than the spike, were fully conserved in the Omicron variant2. This finding suggested that memory T cells elicited by COVID-19 vaccination or infection would be effective against the Omicron variant.
Based on those initial findings, we further investigated whether COVID-19 vaccine-induced memory T cells functionally respond to the Omicron spike1. For this study, we analyzed immune cells from the peripheral blood of healthcare workers who were immunized with two or three doses of the COVID-19 mRNA BNT162b2 vaccine, and from individuals who received two doses of the vaccine after recovery from prior SARS-CoV-2 infection. Vaccine-induced memory T-cell responses were examined by ex vivo stimulation with peptides from the ancestral or Omicron spike protein, and comparatively analyzed. The results showed that CD4+ and CD8+ memory T-cell responses against the ancestral SARS-CoV-2 versus the Omicron variant exhibit similar levels of effector functions. For example, the frequency of IFN-γ-producing CD4+ T cells against the Omicron spike was 80–88% of the frequency against the ancestral spike, and the frequency of TNF-producing CD4+ T cells against the Omicron spike was 86–94% of the frequency against the ancestral spike. Our data also confirmed that the memory T-cell response is stronger in individuals who are vaccinated after experiencing COVID-19 infection. We also investigated polyfunctional memory T cells, which play a key role in the anti-viral immune response due to their superior effector functions. The results indicated an effective polyfunctional memory T-cell response, without any significant difference in the responses against the ancestral SARS-CoV-2 versus the Omicron variant. Our current study demonstrated that memory T cells elicited by BNT162b2 mRNA vaccination substantially respond to the Omicron variant with preserved polyfunctionality. These findings suggest that memory T cells will exert effector functions against the Omicron variant during breakthrough infections among individuals immunized with COVID-19 vaccines. This study broadens our understanding of the mechanism of protection against severe disease even when breakthrough infections occur after vaccination.
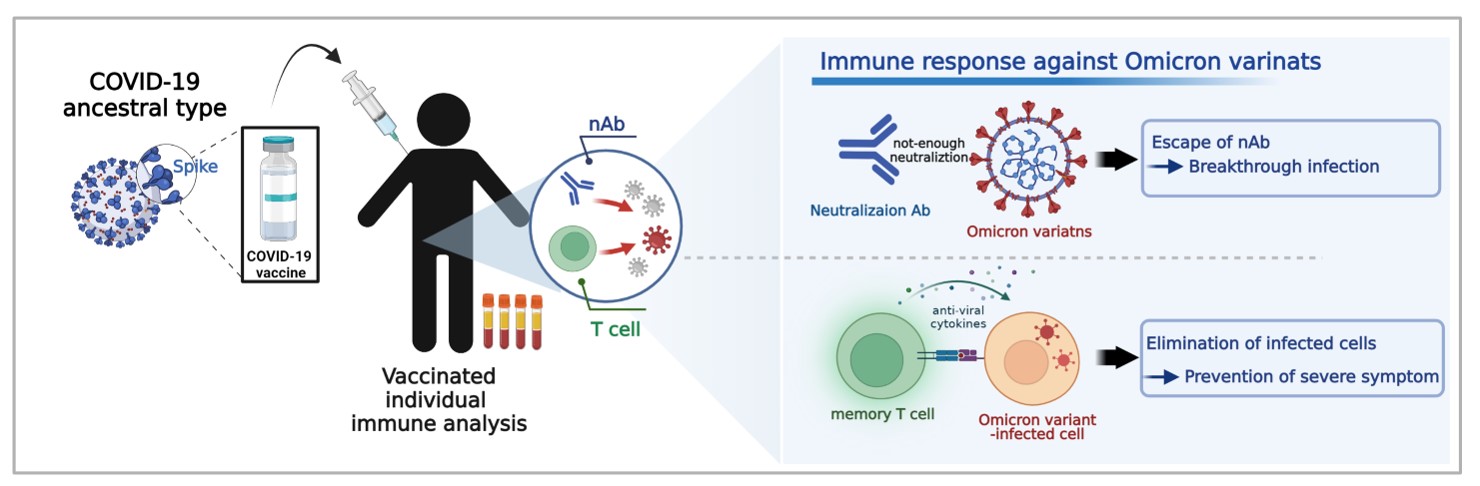
It is clear that Omicron breakthrough infections are common due to the insufficient neutralizing activities of antibodies. However, considering the role of vaccination-elicited memory T cells, patients can be expected to rapidly recover from breakthrough infections without progression to severe disease. For this reason, the research focused on neutralizing antibodies during the COVID-19 pandemic should now be extended to include memory T cells3. During endemic transition of COVID-19, it may be more important to make efforts to reduce the number of severe cases than to reduce new confirmed cases.
[References]
- Jung MK et al. BNT162b2-induced memory T cells respond to the Omicron variant with preserved polyfunctionality. doi: 10.1038/s41564-022-01123-x (2022).
- Choi SJ et al. T cell epitopes in SARS-CoV-2 proteins are substantially conserved in the Omicron variant. Cell Mol Immunol. 19:447-448 (2022).
- Noh, J. Y., Jeong, H. W., Kim, J. H. & Shin, E. C. T cell-oriented strategies for controlling the COVID-19 pandemic. Nat. Rev. Immunol. 21, 687–688 (2021).
Follow the Topic
-
Nature Microbiology
An online-only monthly journal interested in all aspects of microorganisms, be it their evolution, physiology and cell biology; their interactions with each other, with a host or with an environment; or their societal significance.




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in