Effectiveness of a Nursing Rehabilitative Intervention for Elderly Victims of Spousal Emotional Abuse on Stress Level, Life Satisfaction, and Family Functioning
Published in Healthcare & Nursing
Emotional abuse among elderly couples represents a significant yet often underrecognized public health concern, with profound p sychological and social consequences. Older adults are particularly vulnerable due to increased dependency, social isolation, and reduced coping capacities. Exposure to spousal emotional abuse has been associated with elevated stress levels, diminished life satisfaction, and impaired family functioning, all of which negatively affect overall quality of life. Despite the seriousness of this issue, there is a lack of structured, evidence-based nursing interventions specifically designed to address the needs of this population.
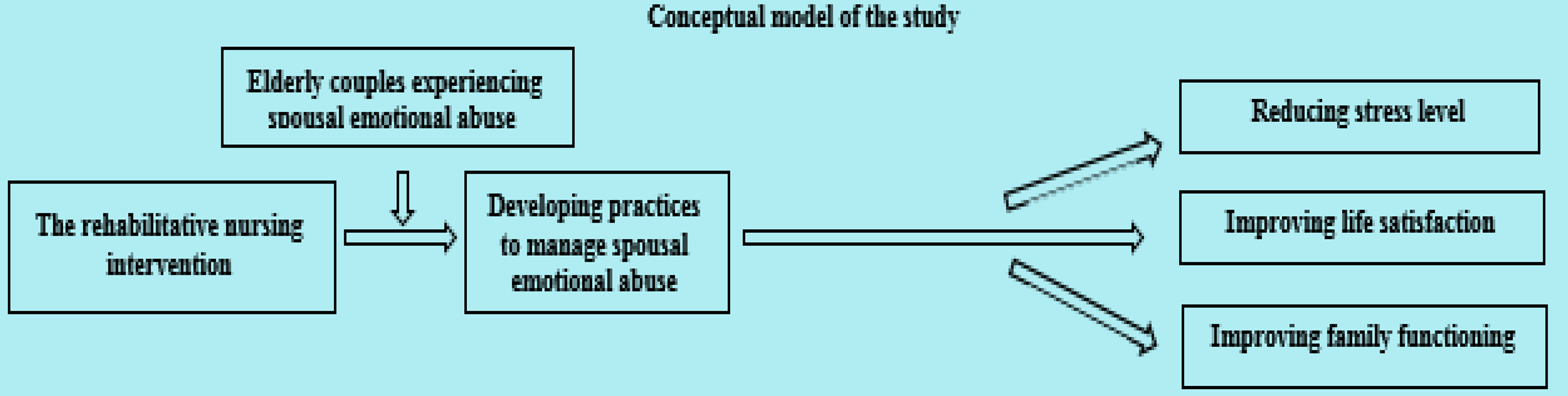
This study aimed to evaluate the effectiveness of a nursing rehabilitative intervention for elderly victims of spousal emotional abuse in reducing stress levels, enhancing life satisfaction, and improving family functioning. A quasi-experimental research design was utilized, involving a sample of elderly individuals exposed to emotional abuse within marital relationships. Participants were assessed before and after the implementation of the intervention using validated measurement tools for stress, life satisfaction, and family functioning.
The rehabilitative intervention included structured nursing sessions focusing on emotional support, education about abuse recognition, coping strategies, stress management techniques, and enhancement of interpersonal communication skills. The program was delivered over a specified period through individualized and group-based approaches.
The findings demonstrated a statistically significant reduction in stress levels, along with notable improvements in life satisfaction and family functioning among participants following the intervention. These results highlight the effectiveness of nursing-led rehabilitative programs in addressing the multifaceted consequences of emotional abuse in older adults.
In conclusion, the study underscores the critical role of nursing interventions in mitigating the negative impact of spousal emotional abuse among the elderly. Integrating such programs into routine geriatric and community health services may contribute to improving psychological well-being and strengthening family relationships. Further research is recommended to expand the evidence base and support the development of standardized intervention protocols.
Follow the Topic
-
BMC Nursing
This is an open access, peer-reviewed journal that considers articles on all aspects of evidence-based nursing care; nursing research methods; nursing service delivery, utilization, and evaluation; nursing administration and human resources.
Related Collections
With Collections, you can get published faster and increase your visibility.
Person-centered care in nursing 2026
BMC Nursing is calling for submissions to its Collection, Person-centered care in nursing 2026. Person-centered care (PCC), often embraced as part of the culture change movement, describes a shift from staff-centric task-based and disease-centered care to a focus on the individual. This philosophy is characterized by health care professionals’ (such as nurses’) knowledge of the individual with various care needs and a close and trusting relationship between care professionals and recipients. Furthermore, this integrates a clinical perspective with a broader understanding that recognizes the unique experiences of each person with various care needs. Particular attention is required for populations such as older adults in long-term and home-care settings and individuals with complex, multi-morbid conditions, where coordinating person-centered, inter-professional care is critical. In recent years, PCC has gained traction as a “gold standard” in nursing and healthcare, fostering improved communication between individuals with various care needs and healthcare professionals, enhancing the quality of nursing, and promoting better health outcomes. The integration of the perspectives of individuals with various care needs and their loved ones into care planning and decision-making is vital for the successful implementation of PCC.
Advancements in technology (e.g., artificial intelligence) seems to provide promising contributions to the evolution of person-centered care, allowing for greater autonomy and empowerment of individuals with various care needs and involvement in their own care. Research has shown that when people with various care needs are actively engaged in their care, they are more satisfied with it. Moreover, the emphasis on gender and ethnic competence and health equity within PCC frameworks highlights the need for nurses to tailor care interventions to diverse populations, ensuring that all individuals receive equitable treatment that respects their unique backgrounds.
As research in PCC continues to evolve, new methodologies and frameworks are anticipated to further empower individuals with diverse care needs and their loved ones in their care. Future advancements may include innovative digital tools that enhance care communication, more comprehensive approaches to informed consent, and strategies to ensure that care delivery is equitable and gender- and culturally sensitive. Such developments will likely transform how nurses engage with individuals receiving care, ultimately leading to improved health outcomes and a more inclusive healthcare system.
We call for studies contributing to the investigation of topics relating to person-centered care, including but not limited to:
- Empowerment strategies through PCC for individuals with diverse care needs
- Development of innovative PCC interventions and their implementation
- Enhancing health equity through PCC
- Gender and cultural competence in PCC
- PCC approaches in aged-care and long-term residential facilities
- PCC models for dementia, frailty and multimorbidity
- Coordination of complex care across settings (acute, community, home)
- Technology-enabled PCC for older and complex-care populations (e.g., remote monitoring, AI-supported care planning)
- Innovative PCC outcomes
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer-review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jan 15, 2027
Nursing and midwifery
BMC Nursing is calling for submissions to its Collection, Nursing and Midwifery. Nursing and midwifery are critical components of healthcare systems worldwide, playing an essential role in promoting health, preventing disease, and providing care across diverse populations. This Collection aims to highlight the latest research and advancements in these fields, focusing on the practices, challenges, and innovations that shape the experiences of nurses and midwives. By fostering collaboration and knowledge sharing, we hope to elevate the discourse surrounding nursing and midwifery, ensuring that these professions continue to evolve and adapt to the changing landscape of healthcare.
Research in nursing and midwifery is vital for improving patient outcomes and enhancing the quality of care provided to people and families. Recent advances have included the integration of evidence-based practices, the development of specialized roles, and the incorporation of technology into patient care. These efforts have demonstrated significant improvements in areas such as prenatal and neonatal care, patient education, and the empowerment of people in childbirth. Understanding these advancements helps to inform future training and policy decisions that can further enhance the effectiveness of nursing and midwifery practices.
As this research continues to evolve, we may witness innovative approaches that further integrate nursing and midwifery into interdisciplinary healthcare teams. Future studies may uncover effective models for collaborative care, improved birth plans, and enhanced patient engagement strategies. Additionally, ongoing research could lead to the development of new educational frameworks that prepare nurses and midwives to meet the complex needs of patients in an increasingly diverse and globalized world.
Topics of interest include, but are not limited to:
- Innovations in prenatal care
- Best practices in neonatal care
- The contribution of midwives to reproductive health education
- The impact of telehealth on nursing and midwifery practices
- Cultural competency in nursing and midwifery
- Evidence-based interventions for postpartum care
- The role of nurses and midwives in addressing health disparities
- The integration of technology in patient care, education and empowerment
- Innovative midwifery service models
- Community and public health nursing and midwifery
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Feb 08, 2027




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in