Emerging maturation stage-associated markers predict AML subtype vulnerability to cardiac glycosides: a step towards their repurposing?
Published in Cancer
Acute myeloid leukemia (AML) is an aggressive blood cancer associated with a poor prognosis. In elderly adults, the non-eligibility for intensive treatments further reduces their chance of recovery. In children and young adults, AML is a rare form of leukemia presenting worse outcomes than any other type of cancer. Dramatically, the disparity in prognosis in the pediatric age has remained unchanged over the past twenty years. Recent combinational regimens, including improved formulations of chemotherapeutics and targeted therapies, are more tolerable and provide survival benefits. Despite these advances, treating AML is still challenging as about 50% of treated patients relapse within a year, impacting the 5-year overall survival rates.
Besides the age-associated limitations of intensive therapeutic regimens, AML therapy often fails due to the emergence of diversified clones of malignant myeloid blasts originating from different progenitor compartments participating in the hierarchical and multi-step process of hematopoiesis in the bone marrow. These clones acquire different mutations, play specific malignant roles, and exhibit distinct drug sensitivities [1]. Their profiling would be essential for upfront tracking and during therapy to promptly detect their outgrowth and ensure their therapeutic eradication.
The clinical use of venetoclax (VEN)-based regimens represents an example of a therapy that could benefit from markers improving patient stratification. Combining the selective inhibitor of the anti-apoptotic B-cell lymphoma-2 (BCL2) protein VEN with hypomethylating agents (HMAs), like azacytidine (AZA), is today the standard of care for AML patients unfit for intensive chemotherapy. While the treatment is tolerable and improves survival compared to single HMA treatment, it is not curative for most of the patients [2], and other combinations with alternative or additional agents are being investigated.
Recent studies indicate that the maturation state of AML blasts impacts therapy outcomes. Prospective and longitudinal studies have shown that myelomonocytic and monocytic blast differentiation confers resistance to VEN-based regimens [3-7]. Ex vivo drug sensitivity screenings on AML patient samples recapitulate the clinical response to therapy observed in the same patient subtypes and evoke the elaboration of more sophisticated predictive biomarkers integrating clinical features, gene expression, and cell state [6]. Other studies, however, question the predictive value of monitoring differentiated clones in real-world clinical practice, emphasizing instead the prominent role of the primitive stem-like leukemic cells in the therapy resistance [8]. Recent research has identified a new type of myeloid stem-like cell responsible for monocytic disease progression in patients treated with VEN-based regimens [9]. These findings highlight the need to track monocytic-like AML clones through more distinguishing markers.
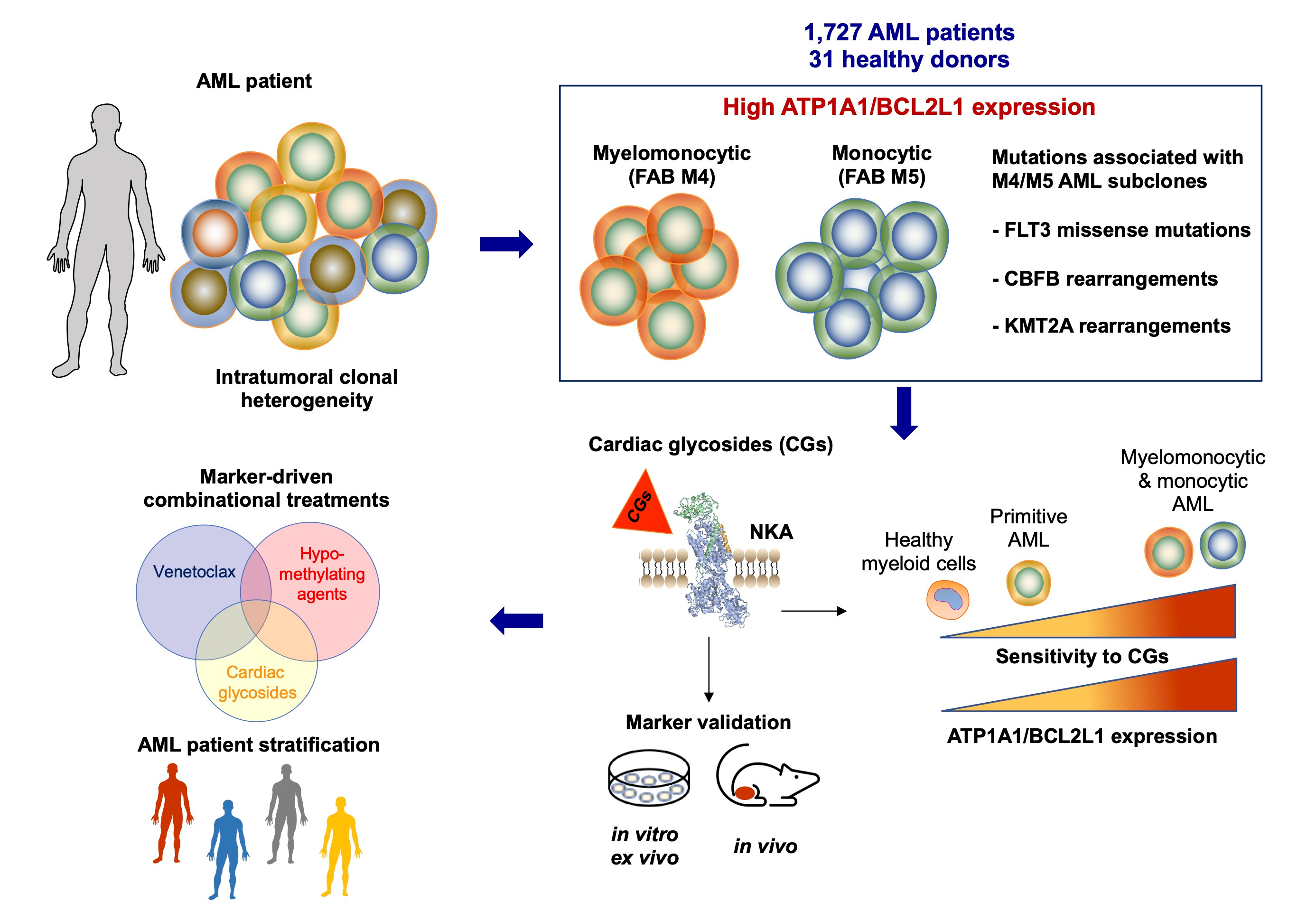
We explored potential treatments for increasing AML sensitivity to VEN [10, 11]. In our recent study, we focused on identifying new markers of AML maturation to target cell state-dependent vulnerability with new treatment options. We analyzed AML patient specimens from seven publicly available cohorts (including over 1,700 AML adult and pediatric patients) and focused on the expression of two groups of proteins. First, we considered the anti-apoptotic BCL2 family proteins, as their expression pattern changes with the myeloid differentiation stage. Next, we selected the alpha subunit isoforms of the sodium/potassium-ATPase (NKA), whose canonical function is to regulate cell homeostasis. Recent findings indicate a direct interaction between the subunit alpha 1 (ATP1A1) of the NKA and the monocytic marker CD14. This interaction modulates inflammatory pathways in macrophages [12]. Consistently, we found that, in both adult and pediatric cohorts, myelomonocytic and monocytic AML show higher levels of ATP1A1 while expressing lower levels of BCL2L1 (coding the pro-survival Bcl-xL protein). The combined ATP1A1/BCL2L1 ratio was even more strongly associated with the monocytic phenotype, as confirmed by the enriched expression of monocytic markers and the similarity with gene signatures of cell type or tissue-specific promonocytes, monocytes, and dendritic cells in the AML patient blasts showing ATP1A1/BCL2L1high phenotype. Furthermore, myelomonocytic/monocytic AML blasts express higher ATP1A1/BCL2L1 levels compared to myeloid cells from healthy donors and may represent a vulnerability of the diseased monocytes. We also found that patient blasts carrying alterations associated with the myelomonocytic and monocytic differentiation (e.g., FLT3 (Fms-related receptor kinase 3) missense driver mutations and the genetic rearrangements of CBFB (core-binding factor subunit) and KMT2A (lysine methyltransferase 2A)) also displayed ATP1A1/BCL2L1high phenotype. Notably, the ATP1A1/BCL2L1high phenotype distinguished the monocytic clone at the diagnosis of an AML patient, and the ratio expression level was even more exacerbated in the residual monocytic clone present at the relapse from the VEN+AZA regimen.
Cardiac glycosides (CGs) are pharmacological agents against arrhythmia, which show potential for anti-cancer therapy [13]. However, their repurposing is challenging due to the lack of predictive markers. Although NKA is the known target, the correlation between CG sensitivity and NKA subunit expression is inconsistent. In our ex vivo analyses, we found that ATP1A1/BCL2L1 protein expression correlated significantly with CG sensitivity (investigated using the hemisynthetic cardenolide UNBS1450), particularly in myelomonocytic and monocytic AML (corresponding respectively to M4 and M5 AML subtypes of the French-American-British, FAB, classification). UNBS1450 was most effective against M4/M5 AML blasts, with CG binding causing on-target ionic perturbation and cell death, as proved through functional and chemical assays.
M4/M5 AML subtypes express high levels of the anti-apoptotic protein MCL1 (BCL2 family member), which is not targeted by VEN and leads to resistance. We previously identified CGs as inhibitors of MCL1 protein expression and showed that the CG AML-killing activity requires MCL1 downregulation [10, 14, 15]. Our recent study demonstrated that MCL1 modulation depends on the inhibition of protein synthesis induced by CG-induced NKA inhibition. Of note, the expression of MCL1 protein alone is not a predictor of CG sensitivity, but the MCL1/BL2L1 protein ratio is. This ratio is high in FAB M4/M5 AML subtypes. In resistant AML cell models that express high BCL2L1 levels, inhibiting or silencing BCL2L1 sensitizes AML blasts to CGs. We therefore established a mechanistic link between the two combined markers ATP1A1/BCL2L1 and MCL1/BCL2L1. Our murine models have validated CGs' translational potential and confirmed the importance of protein expression patterns as predictors of response.
Eventually, we explored combinational treatments benefiting from the inclusion of CGs. Previously, we documented strong VEN and UNBS1450 combination synergism in AML subtypes [10]. The drug resistance study from the Beat AML2 cohort confirms that VEN resistance is associated with the monocytic-like phenotype of AML blasts [16]. Using the same dataset, we validated a significant correlation between ATP1A1/BCL2L1high and MCL1/BCL2L1highphenotype and ex vivo VEN resistance, which suggests that these markers can be considered to stratify AML patients before VEN-based therapy. Additionally, combining HMAs (AZA or decitabine (DAC) with CGs (UNBS1450 and digitoxin) showed an effect ranging from additive to synergistic. These results encourage validating the efficacy of the triple combination VEN+HMAs+CGs on preclinical models in preparation for clinical trials.
In conclusion, our study characterized new AML blast markers associated with monocytic differentiation and could help distinguish AML subtypes resistant to VEN-based therapy but vulnerable to CGs (Figure 1). So far, the outcomes of the clinical trials involving CGs have been frustrating. Interestingly, most cancer types selected for these trials show ATP1A1/BCL2L1low phenotype, while AML is one of the top-expressing malignancies. ATP1A1/BCL2L1highphenotype may distinguish other blood-unrelated CG-sensitive malignancies and help repurpose CGs in therapy.
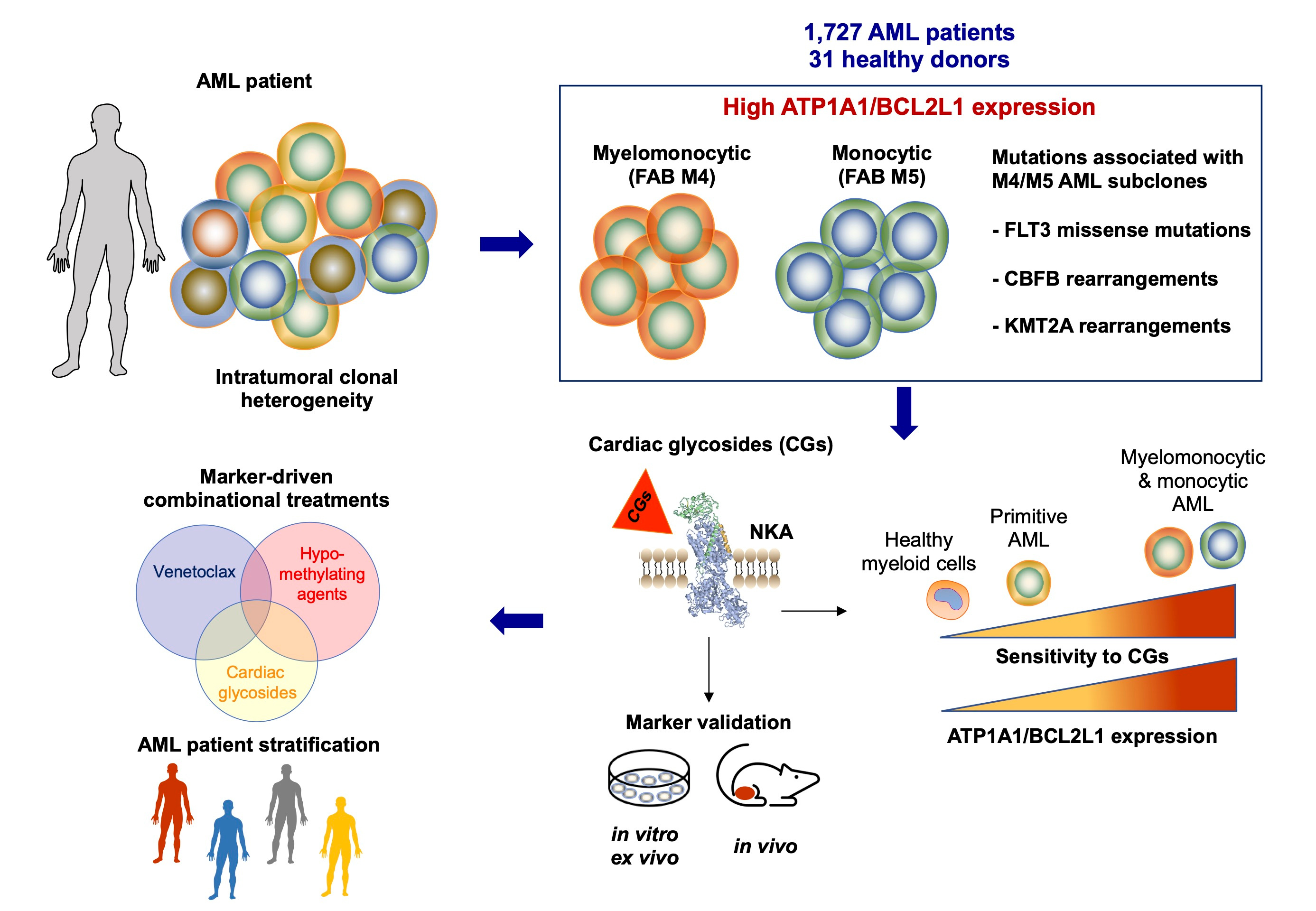
Figure 1. AML phenotypes associated with high ATP1A1/BCL2L1 expression levels are sensitive to cardiac glycosides alone or with approved treatments. The 3D NKA image is from FirstGlance, Jmol; https://www.bioinformatics.org/firstglance/fgij/fg.htm?mol=3kdp.
References
[1] van Galen P, Hovestadt V, Wadsworth Ii MH, Hughes TK, Griffin GK, Battaglia S, et al. Single-Cell RNA-Seq Reveals AML Hierarchies Relevant to Disease Progression and Immunity. Cell 2019 Mar 7; 176(6): 1265-1281 e1224.
[2] Pratz KW, Jonas BA, Pullarkat VA, Thirman MJ, Garcia JS, Fiedler W, et al. Long-Term Follow-up of the Phase 3 Viale-a Clinical Trial of Venetoclax Plus Azacitidine for Patients with Untreated Acute Myeloid Leukemia Ineligible for Intensive Chemotherapy. Blood 2022; 140(Supplement 1): 529-531.
[3] Pei S, Pollyea DA, Gustafson A, Stevens BM, Minhajuddin M, Fu R, et al. Monocytic Subclones Confer Resistance to Venetoclax-Based Therapy in Patients with Acute Myeloid Leukemia. Cancer Discov 2020 Apr; 10(4): 536-551.
[4] White BS, Khan SA, Mason MJ, Ammad-Ud-Din M, Potdar S, Malani D, et al. Bayesian multi-source regression and monocyte-associated gene expression predict BCL-2 inhibitor resistance in acute myeloid leukemia. NPJ Precis Oncol 2021 Jul 23; 5(1): 71.
[5] Kurtz SE, Eide CA, Kaempf A, Long N, Bottomly D, Nikolova O, et al. Associating drug sensitivity with differentiation status identifies effective combinations for acute myeloid leukemia. Blood Adv 2022 May 24; 6(10): 3062-3067.
[6] Eide CA, Kurtz SE, Kaempf A, Long N, Joshi SK, Nechiporuk T, et al. Clinical Correlates of Venetoclax-based Combination Sensitivities to Augment Acute Myeloid Leukemia Therapy. Blood Cancer Discov 2023 Sep 12.
[7] Kuusanmaki H, Leppa AM, Polonen P, Kontro M, Dufva O, Deb D, et al. Phenotype-based drug screening reveals association between venetoclax response and differentiation stage in acute myeloid leukemia. Haematologica2020 Mar; 105(3): 708-720.
[8] Waclawiczek A, Leppa AM, Renders S, Stumpf K, Reyneri C, Betz B, et al. Combinatorial BCL2 Family Expression in Acute Myeloid Leukemia Stem Cells Predicts Clinical Response to Azacitidine/Venetoclax. Cancer Discov 2023 Jun 2; 13(6): 1408-1427.
[9] Pei S, Shelton IT, Gillen AE, Stevens BM, Gasparetto M, Wang Y, et al. A novel type of monocytic leukemia stem cell revealed by the clinical use of venetoclax-based therapy. Cancer Discov 2023 Jun 26.
[10] Cerella C, Gaigneaux A, Mazumder A, Lee JY, Saland E, Radogna F, et al. Bcl-2 protein family expression pattern determines synergistic pro-apoptotic effects of BH3 mimetics with hemisynthetic cardiac glycoside UNBS1450 in acute myeloid leukemia. Leukemia 2017 Mar; 31(3): 755-759.
[11] Florean C, Kim KR, Schnekenburger M, Kim HJ, Moriou C, Debitus C, et al. Synergistic AML Cell Death Induction by Marine Cytotoxin (+)-1(R), 6(S), 1'(R), 6'(S), 11(R), 17(S)-Fistularin-3 and Bcl-2 Inhibitor Venetoclax. Mar Drugs 2018 Dec 19; 16(12).
[12] Zhang J, Chang J, Beg MA, Huang W, Zhao Y, Dai W, et al. Na/K-ATPase suppresses LPS-induced pro-inflammatory signaling through Lyn. iScience 2022 Sep 16; 25(9): 104963.
[13] Diederich M, Muller F, Cerella C. Cardiac glycosides: From molecular targets to immunogenic cell death. Biochem Pharmacol 2017 Feb 1; 125: 1-11.
[14] Juncker T, Cerella C, Teiten MH, Morceau F, Schumacher M, Ghelfi J, et al. UNBS1450, a steroid cardiac glycoside inducing apoptotic cell death in human leukemia cells. Biochem Pharmacol 2011 Jan 1; 81(1): 13-23.
[15] Cerella C, Muller F, Gaigneaux A, Radogna F, Viry E, Chateauvieux S, et al. Early downregulation of Mcl-1 regulates apoptosis triggered by cardiac glycoside UNBS1450. Cell Death Dis 2015 Jun 11; 6: e1782.
[16] Bottomly D, Long N, Schultz AR, Kurtz SE, Tognon CE, Johnson K, et al. Integrative analysis of drug response and clinical outcome in acute myeloid leukemia. Cancer Cell 2022 Aug 8; 40(8): 850-864 e859.
Follow the Topic
-
Leukemia
This journal publishes high quality, peer reviewed research that covers all aspects of the research and treatment of leukemia and allied diseases. Topics of interest include oncogenes, growth factors, stem cells, leukemia genomics, cell cycle, signal transduction and molecular targets for therapy.






Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in