Environmental sensitivity and mental health in Syrian refugee children
Published in Behavioural Sciences & Psychology

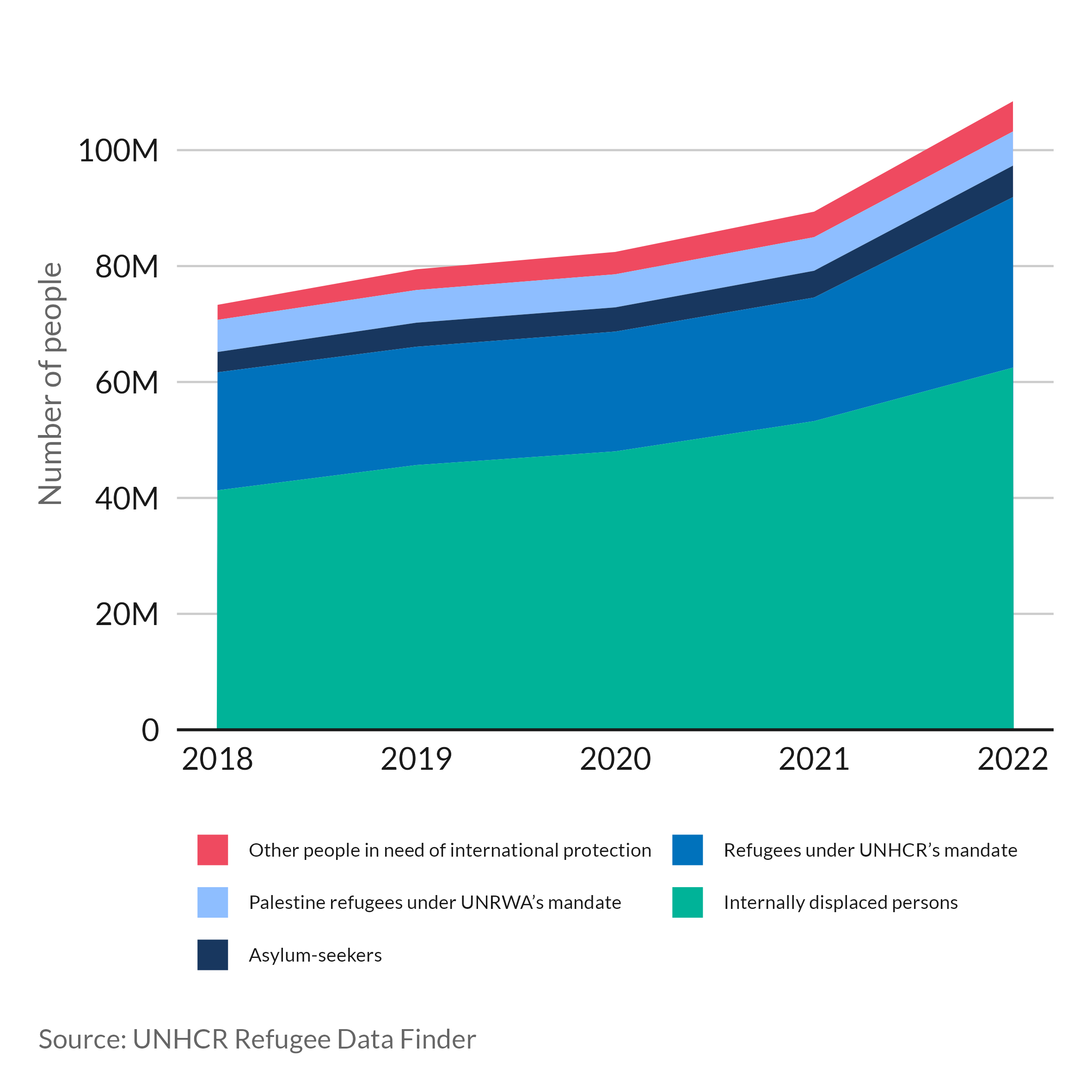
As a result of escalating armed conflict, the number of forcibly displaced people continues to rise worldwide (Figure 1), over 40% of whom are children under the age of 18. Experiences of war and displacement can cause substantial trauma, raising the risk for numerous mental illnesses which can severely disrupt early childhood development [1]. With the least access to mental healthcare [2], many refugee children are robbed of opportunities to reach their full potential in adulthood.
However, not all children are equally affected by war exposure and forced displacement. Children display remarkable differences in their ability to endure, and recover from, trauma, but identifying predictors of these differences has not been a straightforward task for researchers [3].
Environmental sensitivity: a new perspective
One possible, largely unexplored factor in how a child copes with trauma is their individual degree of environmental sensitivity [4]. Environmental sensitivity is a higher-order dimension of personality that is based on innate biological differences in people’s ability to detect and process sensory information. Research shows that while some individuals appear resilient to the influences of their environmental context, others are deeply attuned to sensory information, absorbing the quality of their surroundings for better and for worse [5]. These latter, highly sensitive persons appear at risk of mental illness under stressful environmental conditions, but they flourish and thrive when provided nurturance and support [6]. As a relatively new construct in psychology, however, there is much still to understand about the development and characteristics of environmental sensitivity.
As part of our larger efforts to explore the biological pathways of risk and resilience in refugee children (known as the BIOPATH study [7]), we recently looked at the relationship between mental health in Syrian refugee children and their self-reported environmental sensitivity (using the 12 item Highly Sensitive Child scale). Against the background of severe trauma wrought by war and forced displacement [8], and the harsh living conditions of informal refugee settlements (Figure 2), we suspected that highly sensitive refugee children would be at higher risk for mental illness.

Figure 2: Informal tented settlements are a common form of accommodation for many Syrian refugees, but these can be harsh environments for children to grow up in. Photo by Anmarrfaat, from Wikimedia Commons, licensed under CC BY-SA 4.0 DEED.
A multi-level cross-disciplinary investigation
To investigate, we analysed the BIOPATH dataset which comprises mental health and other psychological information on 1,591 Syrian refugee children, residing in informal tented settlements within Lebanon, at two time points spaced one year apart. Because children also supplied biological data in the form of both hair samples (for hormone analysis [9]) and DNA (for genotype, methylation, and telomere analysis [10]), we took this opportunity to explore whether there were biological markers (hormone concentrations and polygenic scores) that correlated with environmental sensitivity, and shared similar associations with mental health outcomes.
Using Bayesian multivariate linear mixed models, we discovered that self-reported highly sensitive children scored consistently higher on measures of anxiety, depression, and post-traumatic stress disorder (PTSD). To ensure that our measure of sensitivity was not biased by existing mental illness, we generated cross-lagged panel models to explore our data across both waves (Figure 3). Self-reported sensitivity at wave 1 was not significantly correlated with mental health outcomes at wave 2, or vice versa, suggesting that children reported their sensitivity and mental health as separate aspects, not allowing one to influence the other.
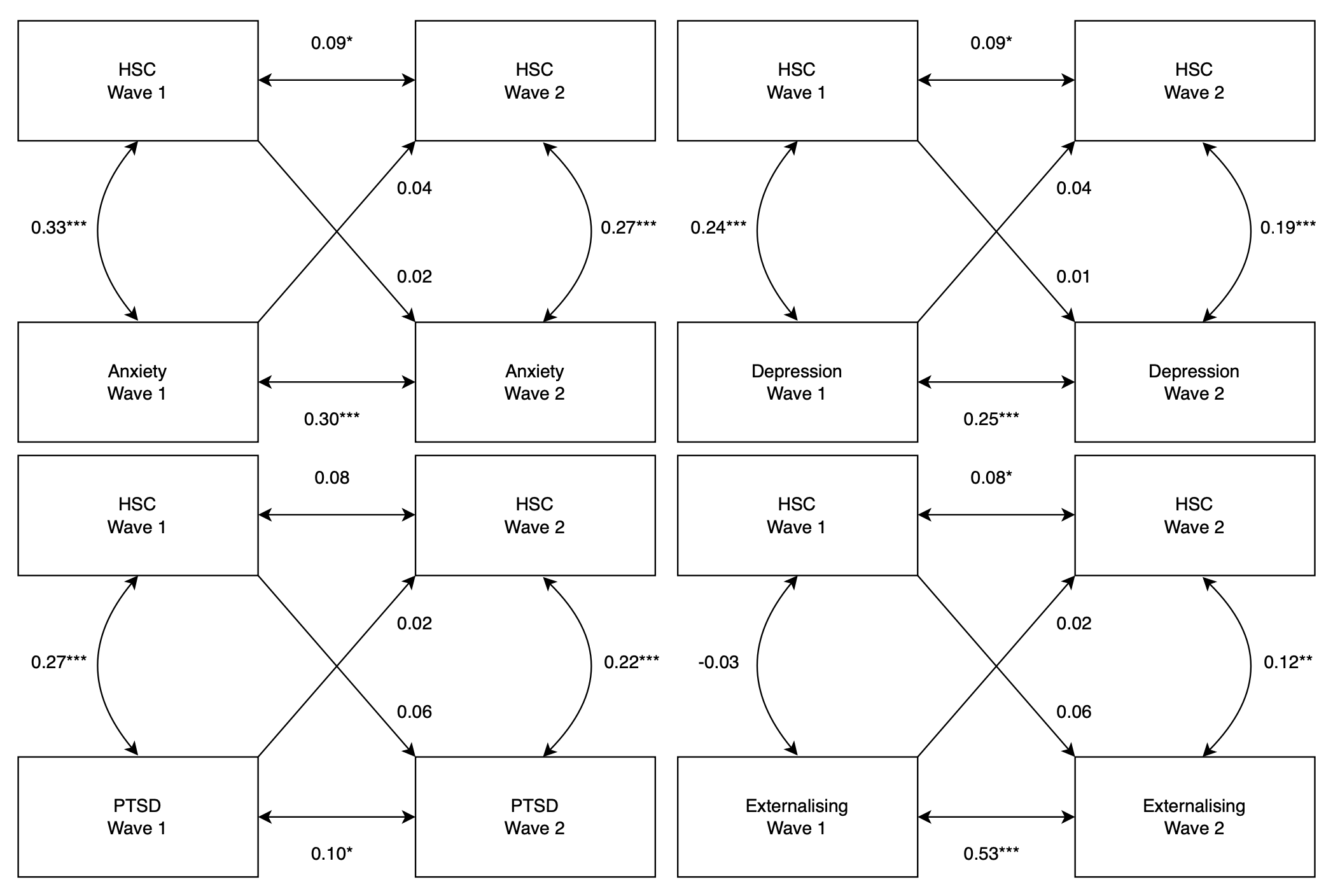
Figure 3: Cross-lagged panel models revealed no strong correlations between self-reported sensitivity, using the Highly Sensitive Child (HSC) scale and mental health outcomes such as anxiety, depression, post-traumatic stress disorder (PTSD) and externalising behaviour.
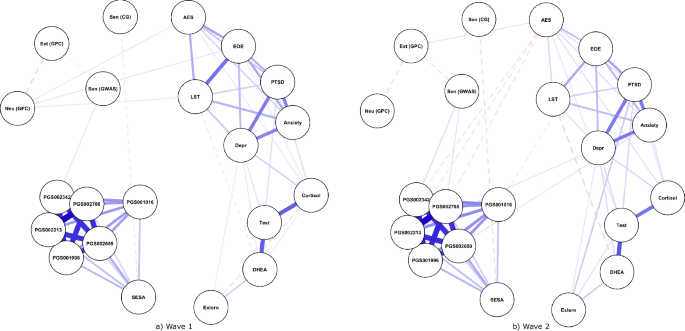
Because self-report data are prone to many issues in psychological research, we hoped to find a biological marker correlating sufficiently well with self-report sensitivity that might serve as a more objective indicator of sensitivity in future. We examined concentrations of hair cortisol, dehydroepiandrosterone (DHEA), and testosterone, as well as a selection of different polygenic scores (weighted sums of genetic variants) for personality traits such as neuroticism, extraversion, and general sensitivity to stress and socioemotional influences. However, none of these biological metrics seemed to track well with environmental sensitivity.
Similarly, our selection of biological markers did not appear to be good indicators of mental health outcomes. One possible exception was the concentration of hair DHEA [11], which was significantly associated with anxiety and depression (but not PTSD). Although we found limited evidence for a relationship between our specific selection of biological markers and refugee sensitivity or mental health, there remain other markers and contexts which need to be investigated in future research.
Significance and implications
Our study is significant for a number of reasons. We have provided one of the first examinations of environmental sensitivity and its relation to mental health in refugee children. In addition to self-reported sensitivity, we also simultaneously explored numerous possible biological markers of sensitivity, which has rarely been done within the same cohort of participants. Ours is also amongst a small selection of studies that combines psychological, physiological, and genetic data together to more comprehensively understand refugee children. Lastly, our research helps bring attention to two comparatively understudied population groups, namely refugees hosted in developing countries, and people of Middle Eastern genetic ancestry.
In summary, children highly sensitive to environmental input are at higher risk for larger burdens of mental illness within the refugee context. As a simple 12-item measure, assessing environmental sensitivity through the Highly Sensitive Child scale may provide clinicians and health professionals with a convenient indication of the temperament of young patients, and how receptive they are to both trauma and intervention. Additional basic research will be needed to determine if sensitivity levels can be inferred from biological markers, while future clinical research may reveal specific treatment guidelines for high- and low-sensitive children, aligning with wider medical efforts to personalise the care of individuals [12].
References
- Murray, J. S. (2019). War and conflict: addressing the psychosocial needs of child refugees. Journal of Early Childhood Teacher Education, 40(1), 3–18. https://doi.org/10.1080/10901027.2019.1569184
- McGorry, P. D., & Mei, C. (2018). Early intervention in youth mental health: Progress and future directions. Evidence-Based Mental Health, 21(4), 182–184. https://doi.org/10.1136/ebmental-2018-300060
- Mesman, E., Vreeker, A., & Hillegers, M. (2021). Resilience and mental health in children and adolescents: An update of the recent literature and future directions. Current Opinion in Psychiatry, 34(6), 586–592. https://doi.org/10.1097/YCO.0000000000000741
- Pluess, M. (2015). Individual Differences in Environmental Sensitivity. Child Development Perspectives, 9(3), 138–143. https://doi.org/10.1111/cdep.12120
- Belsky, J., & Bakermans-Kranenburg, M. J. (2007). For Better and For Worse Differential Susceptibility to Environmental Influences. Current Directions in Psychological Science, 16(6), 300–304.
- Pluess, M., & Boniwell, I. (2015). Sensory-Processing Sensitivity predicts treatment response to a school-based depression prevention program: Evidence of Vantage Sensitivity. Personality and Individual Differences, 82, 40–45. https://doi.org/10.1016/j.paid.2015.03.011
- McEwen, F. S., Popham, C., Moghames, P., Smeeth, D., Villiers, B. de, Saab, D., Karam, G., Fayyad, J., Karam, E., & Pluess, M. (2022). Cohort profile: biological pathways of risk and resilience in Syrian refugee children (BIOPATH). Social Psychiatry and Psychiatric Epidemiology, 57(4), 873–883. https://doi.org/10.1007/s00127-022-02228-8
- McEwen, F. S., Biazoli, C. E., Popham, C. M., Moghames, P., Saab, D., Fayyad, J., Karam, E., Bosqui, T., & Pluess, M. (2023). Prevalence and predictors of mental health problems in refugee children living in informal settlements in Lebanon. Nature Mental Health, 1(2), 135–144. https://doi.org/10.1038/s44220-023-00017-z
- Smeeth, D., McEwen, F. S., Popham, C. M., Karam, E. G., Fayyad, J., Saab, D., Rieder, M. J., Elzagallaai, A. A., Uum, S. van, & Pluess, M. (2023). War exposure, post-traumatic stress symptoms and hair cortisol concentrations in Syrian refugee children. Molecular Psychiatry, 28(2), 647–656. https://doi.org/10.1038/s41380-022-01859-2
- Smeeth, D., May, A. K., Karam, E. G., Rieder, M. J., Elzagallaai, A. A., Uum, S. van, & Pluess, M. (2023). Risk and resilience in Syrian refugee children: A multisystem analysis. Development and Psychopathology, 35(5), 2275–2287. https://doi.org/10.1017/S0954579423000433
- Dutheil, F., de Saint Vincent, S., Pereira, B., Schmidt, J., Moustafa, F., Charkhabi, M., Bouillon-Minois, J.-B., & Clinchamps, M. (2021). DHEA as a Biomarker of Stress: A Systematic Review and Meta-Analysis. Frontiers in Psychiatry, 12(July), 1–14. https://doi.org/10.3389/fpsyt.2021.688367
- Belsky, J., & IJzendoorn, M. H. van. (2015). What works for whom? Genetic moderation of intervention efficacy. Development and Psychopathology, 27(1), 1–6. https://doi.org/10.1017/S0954579414001254
Follow the Topic
-
Molecular Psychiatry
This journal publishes work aimed at elucidating biological mechanisms underlying psychiatric disorders and their treatment, with emphasis on studies at the interface of pre-clinical and clinical research.


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in