From an Unprecedented Mass Trauma to New Insights into PTSD Risk
Published in Behavioural Sciences & Psychology
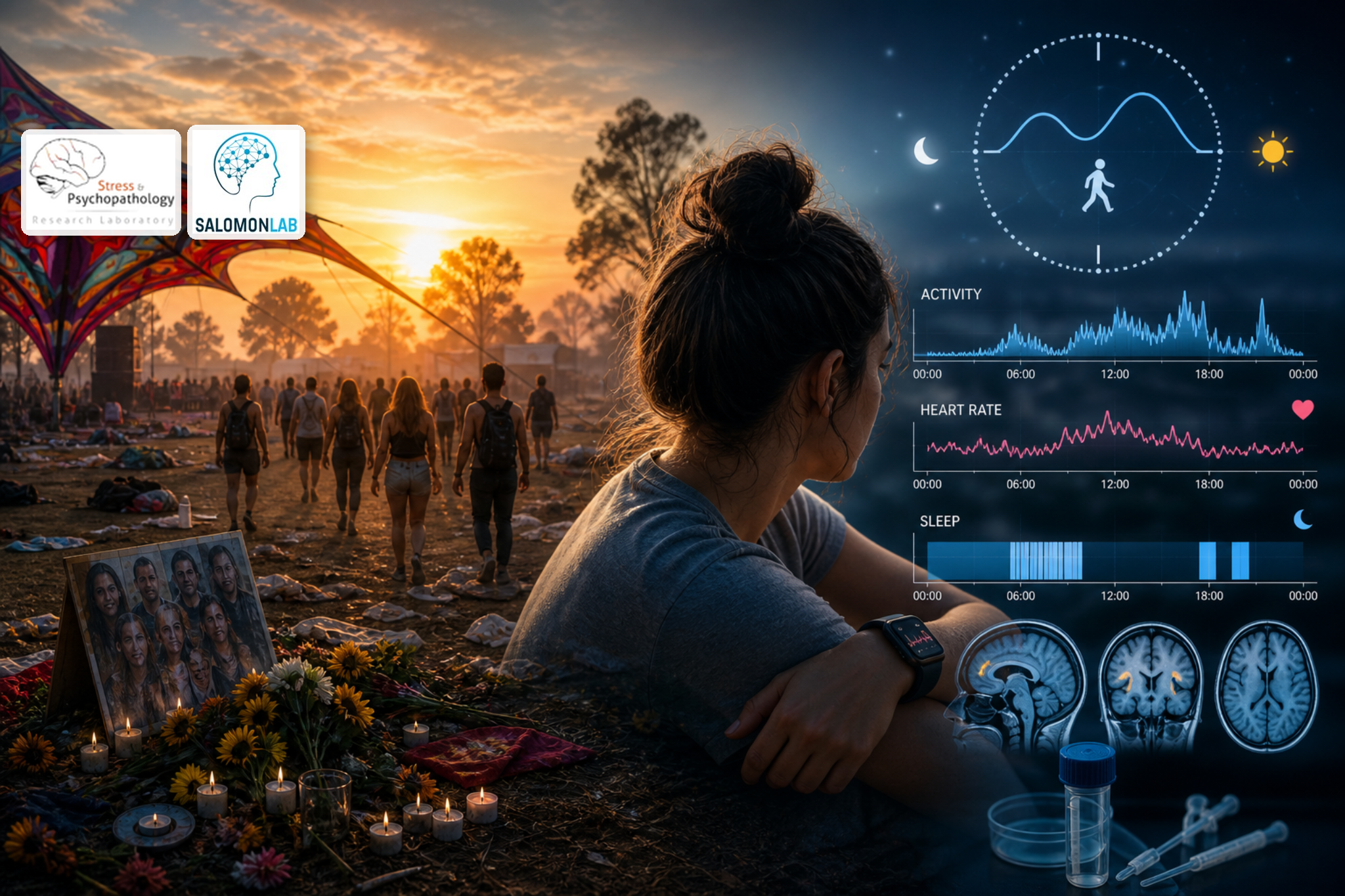
On October 7, 2023, the Supernova music festival became the site of an unprecedented civilian mass-trauma event. Thousands of young people had gathered overnight to dance, celebrate, and welcome the sunrise. At sunrise, the festival was attacked by Hamas-led terrorists, killing more than 360 festival attendees. Hence, within minutes, a setting of music, movement, and social connection was transformed into one of prolonged life-threatening danger, loss, and survival. For many festival survivors, the trauma did not end when they escaped the festival grounds. It continued in the weeks and months that followed, in sleep, in the body, in daily routines, and in the struggle to return to life.
Our research began in this urgent aftermath. Together with the non-profit-organization SafeHeart, clinicians, volunteers, and survivors themselves, we were confronted with a question that was both scientific and deeply practical: how can we understand who is recovering, who remains at risk, and what forms of support are needed? The Nova cohort was therefore built not as a single study, but as a broad longitudinal effort to follow survivors over time using multiple complementary tools including clinical assessments, wearable sensors, brain imaging, interoception tasks, ecological momentary assessments, clinical interviews, and biological sampling. The aim was to capture trauma recovery as it unfolds over time in real life, across psychological, physiological, behavioral, and neural domains.
The paper now accepted in Translational Psychiatry focuses on one specific part of this larger project: the daily rhythms of the body. Trauma is often studied through symptoms, memories, and emotions. Yet trauma also affects the basic systems that organize everyday life, such as when we sleep, how regularly we move, and how the heart activity changes across the day. We asked whether disruptions in these circadian rhythms during the aftermath of trauma could help predict later PTSD risk.
What we found was that the stability of these rhythms mattered. Survivors showed reduced circadian stability compared with matched comparison participants, including less stable sleep–wake rhythms and greater day-to-day variability in heart-rate peak timing. Most importantly, survivors whose sleep–wake rhythms were less stable during the months after the attack were more likely to show clinically significant PTSD symptoms later on. This association remained meaningful even after accounting for initial PTSD symptom severity.
For us, this finding shifts the emphasis from average levels to temporal organization. It was not only how much people slept, or what their average heart rate was, but how stable their daily rhythms remained over time. This suggests that wearable sensors may help identify patterns of post-trauma vulnerability in real-world settings, long before clinical deterioration becomes entrenched. These tools are not a replacement for clinical assessment, but they may offer a scalable way to monitor recovery and guide early support.
Follow the Topic
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in