Genetic contribution to disease-course severity and progression in the SUPER-Finland study, a cohort of 10 403 individuals with psychotic disorders
Published in Genetics & Genomics, General & Internal Medicine, and Behavioural Sciences & Psychology
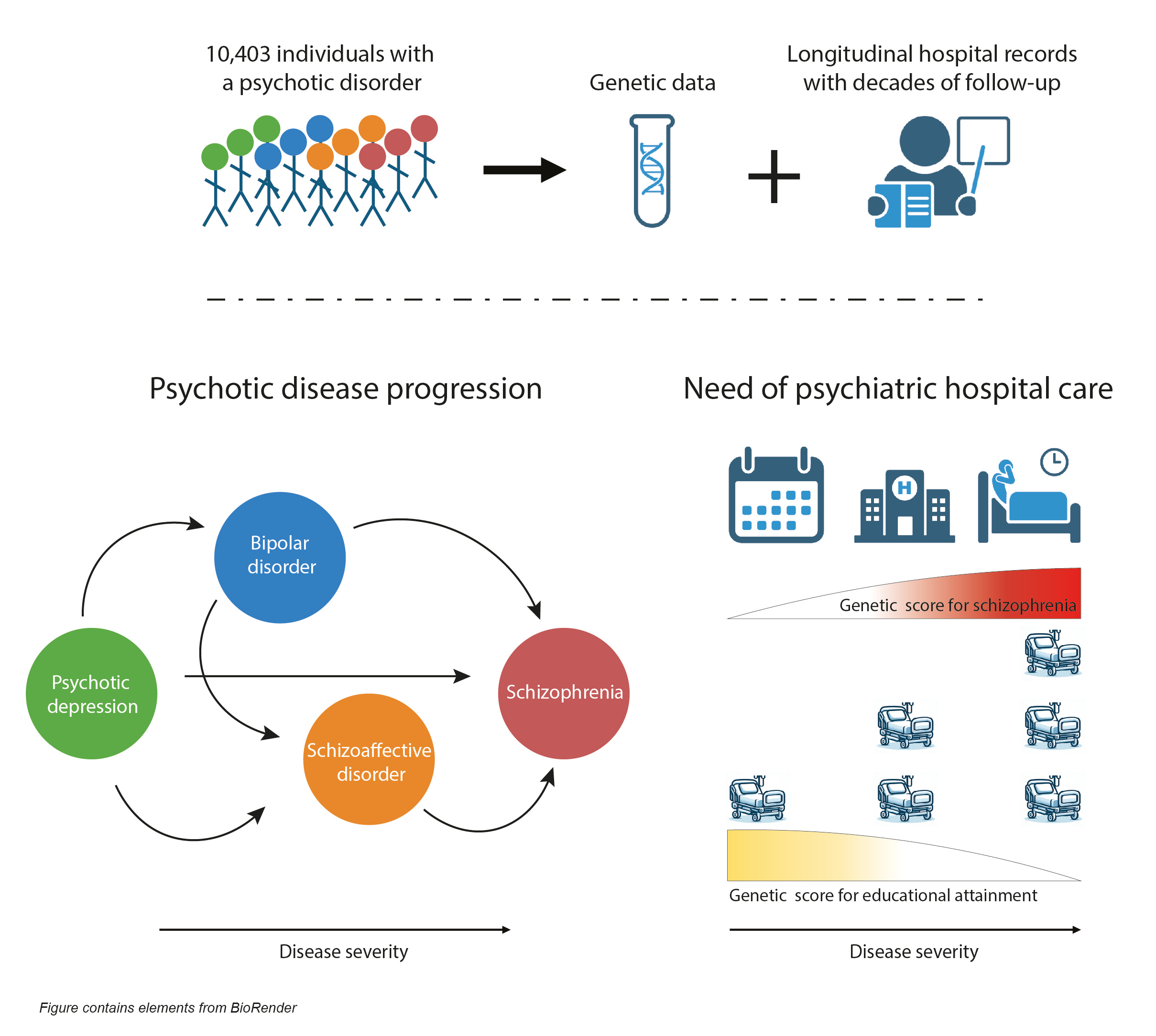
Genetics influences the risk of acquiring a psychotic disorder, but little is known how genetic factors contribute to the disease course. To study psychotic disease-course development, we combined longitudinal information from the Finnish medical health care records with genetic data from over 10,000 individuals with a psychotic disorder. We followed the individuals’ disease-courses and transitions from the first initial diagnosis to different disease trajectories. Further, using an innovative approach, we estimated the longitudinal hospitalization burden for each study participant from nation-wide, full-coverage medial record data collected from 1969 and onwards. We hypothesized that a more severe manifestation of illness would result in more frequent hospitalization and longer time spent at hospital care. We tracked the individual’s past disease-course severity at different time points, and in relation to disease onset, by calculating the yearly need for in-hospital care due to a psychiatric diagnosis. We then assessed the genetic contribution to psychotic disease development and need for psychiatric hospital care.
The data revealed that individuals who were initially diagnosed with a milder psychotic disorder (psychotic depression, bipolar disorder, or schizoaffective disorder), but later developed schizophrenia had a higher genetic loading for schizophrenia and a higher hospital burden than those who remained in the initial diagnoses. We show that the individuals, who later progressed to schizophrenia, had the same need for hospital care as other individuals with schizophrenia already from the start of first psychotic illness – despite receiving their schizophrenia diagnosis almost 6 years later. This indicated that a subset of the people, initially diagnosed with milder psychotic disorders, were in a trajectory to a more severe outcome already from the start of first illness. Interestingly, an initial diagnosis of milder psychotic disorder preceding schizophrenia was more common among women than men, potentially explaining in part why women often are found to have a later onset of schizophrenia compared to men.
We also studied the genetic contribution to disease severity associated with schizophrenia. We found that individuals with a high genetic liability for schizophrenia had a more severe psychiatric disease trajectory, with more frequent and longer hospital visits than schizophrenia diagnosed individuals with a low genetic loading. The genetic make-up associated with a low educational attainment also impacted the psychotic disease-course, but independently from the genetic loading associated with schizophrenia, suggesting two separate underlying mechanisms. The genetic profile for low educational attainment resulted in a distinctly increased need for psychiatric hospital care. While study participants with a high genetic liability for schizophrenia had long individual hospital visits, the participants with a low genetic loading for educational attainment had short and more frequent visits – a hospitalization profile often known as a “revolving door” phenomenon. This revolving door pattern was strongly associated with substance use, which acted as a mediator of the observed genetic effect. A low genetic score for educational attainment had a very strong impact on the risk of having been diagnosed with a substance use disorder, while the genetic score for schizophrenia were uncorrelated with substance use disorder. Importantly, we found that having been diagnosed with a substance use disorder was not just a marker for a poor outcome, but that the diagnosis for substance use disorder preceded an increase in psychiatric hospitalizations even when it was given years after the initial psychotic disorder diagnosis – making it an attractive target for prevention. We also validated these results in a non-psychiatric population in the large Finnish biobank study FinnGen.
Follow the Topic
-
Molecular Psychiatry
This journal publishes work aimed at elucidating biological mechanisms underlying psychiatric disorders and their treatment, with emphasis on studies at the interface of pre-clinical and clinical research.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in