PGT-WGS (Preimplantation Genetic Testing with Whole Genome Sequencing) in Malaysia and Singapore
Published in Social Sciences, Genetics & Genomics, and General & Internal Medicine
Please refer to the following articles:
Ethical Challenges with Comprehensive, Integrated, and Universal Preimplantation Genetic Testing Platforms Utilizing Whole Genome Sequencing (PGT-WGS)
Should Malaysia Embrace Advanced IVF Genetic Testing With Whole Genome Sequencing Technology? (PGT-WGS/PGT-G)
.png)

Introduction
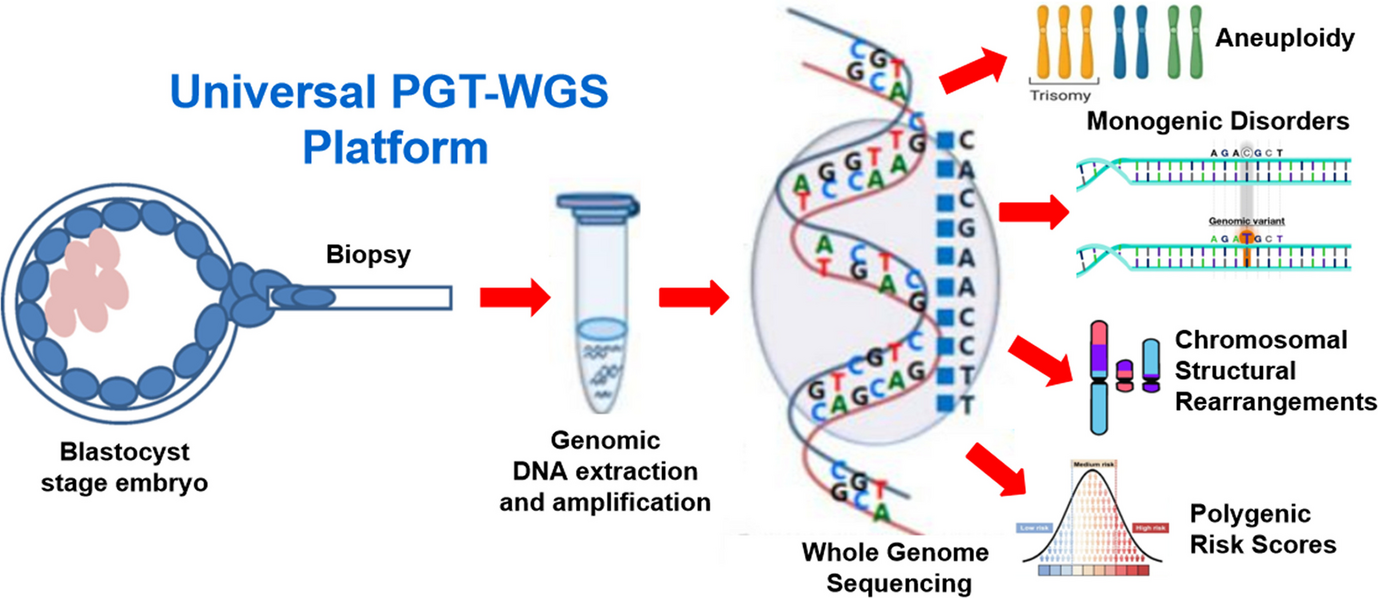
Recent advances in preimplantation genetic testing (PGT) and whole genome amplification technologies have resulted in the development of comprehensive platforms that integrate multiple types of PGT utilizing whole genome sequencing (PGT-WGS). These platforms combine PGT-A, PGT-M, PGT-SR, and PGT-P into a single universal genetic screening system for IVF embryos. Leveraging cutting-edge computing and artificial intelligence technologies, PGT-WGS allows simultaneous screening for aneuploidies, monogenic disorders, chromosomal structural rearrangements, and polygenic disease risks using a single trophectoderm biopsy from a blastocyst-stage embryo.
The popularization of Newborn Genomic Sequencing (NBSeq) for the early diagnosis and treatment of rare genetic disorders will likely promote extensive uptake of PGT-WGS among IVF patients because many prospective parents will rationalize that “prevention is better than cure.” Profit-driven fertility clinics can readily exploit various sociocultural drivers to aggressively market the PGT-WGS platform, often advocating for its extensive use regardless of whether appropriate medical indications, such as a family history of genetic disease, exist.
One primary method of exploitation involves leveraging the global trend of declining fertility rates and shrinking family sizes, which has fostered a culture of "child perfectionism" and "tiger parenting". Because parents are having fewer children, they are often willing to invest more time and money into each child and become increasingly fearful of "genetics going wrong", such as Down syndrome in older mothers. Fertility clinics play on these fears and the hopes of conceiving a "perfect child" to drive uptake.
Profit-driven fertility clinics can also exploit specific sociocultural vulnerabilities and stigmas, such as those in East Asian Confucian societies, where congenital disabilities are often viewed with low tolerance and seen as a source of social shame. In these contexts, PGT-WGS is marketed as a "wonder technology" for preventing disabilities and avoiding the social stigma associated with birth defects. Furthermore, clinics may exploit the religious beliefs and consciences of patients who oppose abortion by framing PGT-WGS as an "ideal preventive measure" that eliminates the need for future pregnancy terminations.
Another aggressive marketing tactic is "guilt-tripping," in which clinics pressure prospective parents to believe they are failing to give their offspring the "best start in life" if they do not use the technology. This can lead to the non-judicious application of IVF and invasive testing in healthy, fertile couples who have no medical necessity for such procedures.
To maintain their customer base, fertility clinics and genetic testing companies often present a simplistic "good" versus "bad" view of genes. This approach hides the "intricate paradox of choices" and the high volume of conflicting or confusing information that full genomic data actually provides, such as the fact that many "bad" genes actually confer survival advantages or that "best genetics" may not align with the best embryo for a successful pregnancy.
Finally, fertility clinics can exploit the rising popularity of Newborn Genomic Sequencing (NBSeq) by using the intuitive rationale that "prevention is better than cure". They convince patients that preventing a rare disorder through PGT-WGS is a superior alternative to diagnosing and treating it after birth, despite the high cost and invasive nature of the procedure.
Moreover, with the advent of Polygenic Embryo Screening (PES) or PGT-P, there is a dire risk of PGT-WGS shifting from medical diagnosis to a fashionable cosmetic procedure used for enhancing socially desirable traits like high IQ, athletic prowess, and specific physical features.
Deficiencies and limitations of the PGT-WGS platform
The PGT-WGS platform faces several technical, clinical, and psychosocial deficiencies and limitations that challenge its widespread and non-judicious application.
Technical and Clinical Limitations
- Risks of Embryo Damage: The trophectoderm biopsy required for PGT-WGS is a highly invasive procedure that can inadvertently damage embryos, particularly those of lower quality from older women. While some studies suggest no negative effects, these often focus on high-quality embryos and ignore the possibility of human error in busy laboratories
- Inaccurate Representation: A biopsy of the trophectoderm (which becomes the placenta) may not accurately represent the inner cell mass, which actually develops into the fetus
- Misdiagnosis of Mosaicism: Many human embryos exhibit mosaicism (a mix of normal and abnormal cells), and PGT-WGS may lead to the erroneous rejection of these embryos. Evidence suggests mosaic embryos can "self-correct," and discarding them can significantly lower IVF success rates, especially for older women with few embryos
- Lack of Proven Benefit for PGT-A: Large-scale randomized clinical trials have repeatedly shown that the PGT-A component of the platform does not improve overall IVF success rates and may even lead to a lower cumulative live birth rate compared to conventional IVF.
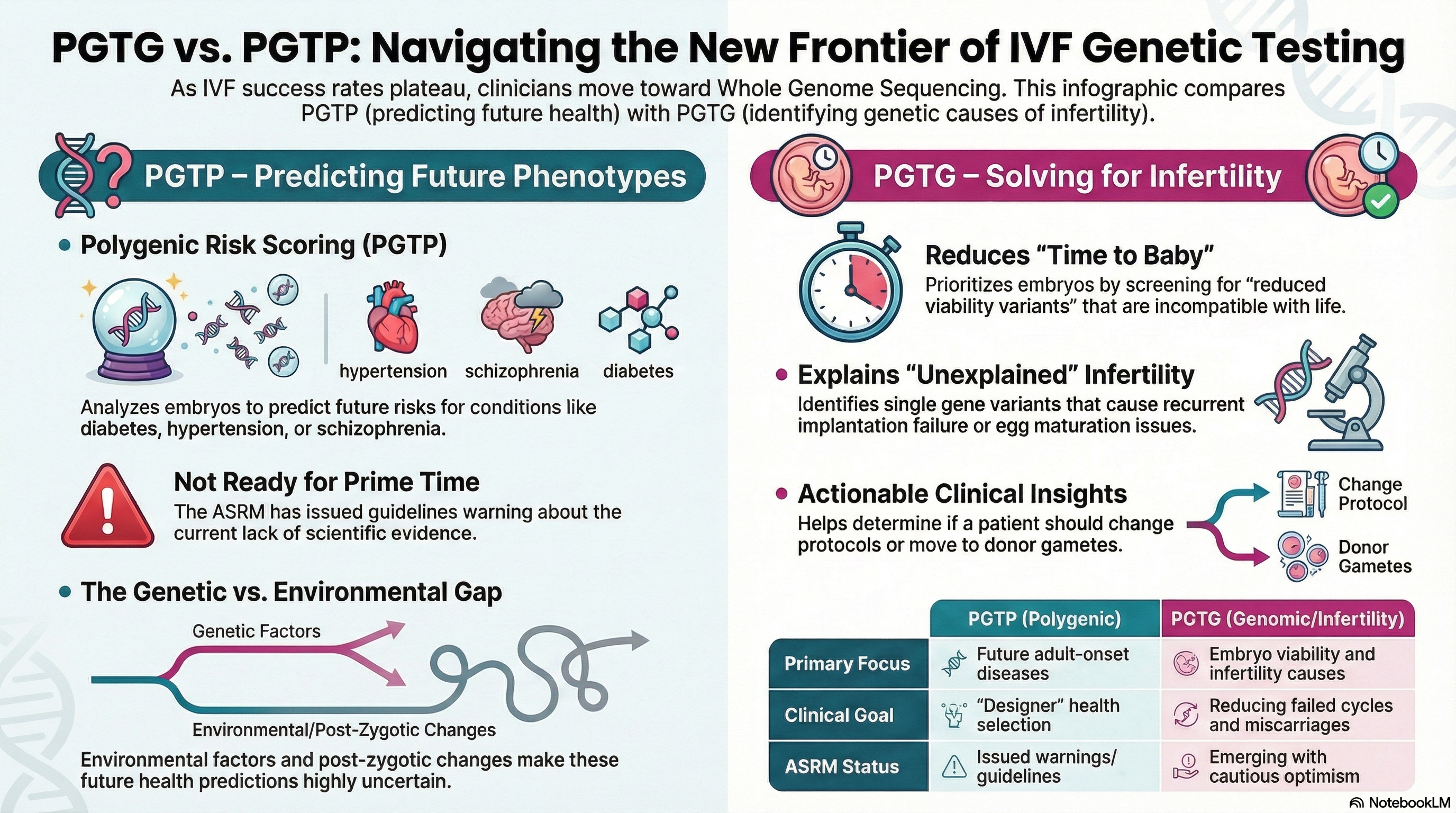
- Ineffectiveness of Polygenic Embryo Screening (PES): The PES component is limited by the low genetic diversity of embryos from a single pair of parents, leading to only modest predicted gains, such as a mere 2.5 cm increase in height or 2.5 IQ points.
Information Overload and Decision-Making Challenges
- Unnecessary Anxiety and Distress: The vast amount of genomic data can subject patients to information overload, causing confusion and anxiety. For instance, ill-informed patients may be distressed to find that most healthy embryos are carriers for at least one recessive monogenic disorder, even though such embryos can result in healthy children.
- The Paradox of Choice: Patients face confounding dilemmas when forced to choose between embryos with conflicting risk profiles (e.g., lower risk for one disease but higher for another). This is exacerbated by pleiotropy, where a genotype for a "positive" trait might simultaneously increase the risk of a "negative" one, such as the link between high intelligence and autism or bipolar disorder.
- Genetic vs. Morphological Quality: Choosing an embryo with "better" genetics over one with superior morphological quality can detract from the primary goal of achieving a successful pregnancy, as the lower-quality embryo may have a reduced chance of implantation.
Cost-Effectiveness and Ethical Concerns
- Questionable Value: Given that genetic disorders and de novo mutations are relatively rare, and most non-viable embryos fail to implant naturally, the high cost of universal PGT-WGS is often not warranted.
- Better and Cheaper Alternatives: Cheaper and equally effective alternatives exist, such as Non-Invasive Prenatal Testing (NIPT) during pregnancy or preconception carrier screening of the parents.
- Social and Genetic Risks: Widespread use could encourage eugenics, social discrimination, and a reduction in human genetic diversity, potentially eliminating genes that might provide survival advantages in future environments (e.g., genes related to energy metabolism during famine).
- Impact on Parent-Child Relationships: The use of "specially genetically optimized" embryos may lead to unrealistic parental expectations and "nurtured genetics," potentially causing children to feel like "laboratory animals" rather than being loved unconditionally.
Conclusion
While this technology platform provides the opportunity to select the “best and healthiest” IVF embryo based on the optimal genetic profile, it also raises profound ethical issues. Due to commercial interests, profit-driven private fertility clinics will likely advocate for extensive, indiscriminate, and non-judicious use of universal PGT-WGS in the future, regardless of appropriate medical indications, such as family history of genetic diseases, recurrent miscarriages, or repeated IVF failures. This concern is amplified by findings from large randomized clinical trials, which have repeatedly demonstrated that the broad application of PGT-A does not significantly improve IVF success rates, which can be extrapolated to PGT-WGS in the future. There are also concerns about the lack of evidence for the usefulness and effectiveness of the PGT-P component of PGT-WGS. Moreover, the identification of recessive monogenic disease gene loci in a significant number of IVF embryos via PGT-WGS may cause unnecessary confusion and distress to some ill-informed patients. Hence, the ethical implications of the potential widespread, indiscriminate, and non-judicious use of universal PGT-WGS will be examined, focusing on its possible harms and the need for balanced and comprehensive patient counseling.
Follow the Topic
-
Asian Bioethics Review
This is an international academic journal, based in Asia, providing a forum to express and exchange original ideas on all aspects of bioethics, especially those relevant to the region.

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in