Teaching differently, eating differently: how collaborative learning transformed adolescent diet quality in Ogun State, Nigeria
Published in Healthcare & Nursing and Education
When I first started teaching nutrition to teenagers and adolescents in Ogun State, something troubled me: students could recite facts about balanced diets but weren't making healthier choices at the school canteen. They knew what to eat; that knowledge just wasn't reaching their plates. That gap between knowledge and behaviour had been nagging at me for years. When we finally designed a study to tackle it, we didn't just ask whether nutrition education worked — we asked whether the way we taught it made any difference at all.
The problem behind the problem
Nigeria's adolescents carry a dual burden: persistent micronutrient deficiencies on one hand, and rapidly rising rates of overweight, obesity, and diet-related noncommunicable diseases on the other. In Ogun State specifically, young people navigate between traditional dietary patterns and an expanding market for ultra-processed foods, sugar-sweetened beverages, and fast food. Schools represent one of the few settings where adolescents can be reached consistently and at scale — yet nutrition education in Nigerian secondary schools remains inconsistent, mostly embedded in broader health lessons, and delivered the way it has always been: a teacher at the front, a class of students passively listening. We wanted to test something different.
What we did
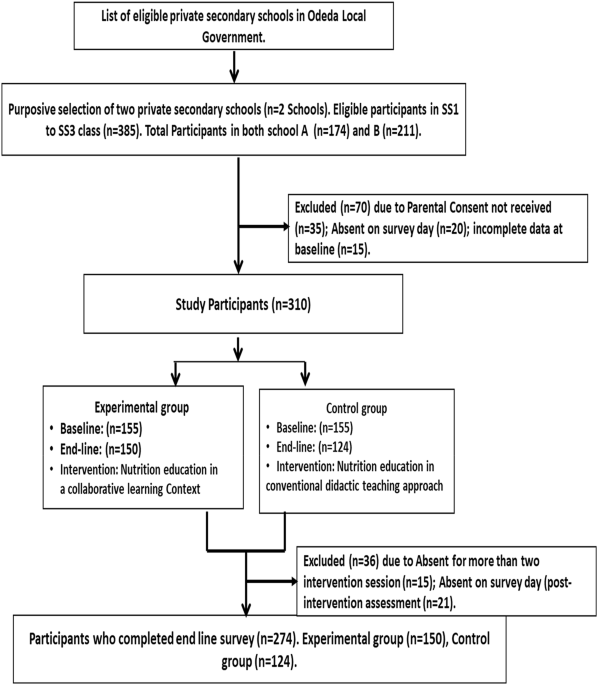
Between January and May 2024, we recruited 274 adolescents aged 13 to 19 from two private secondary schools in Odeda Local Government Area. Using a quasi-experimental design, we assigned one school to a collaborative learning–based nutrition education intervention and the other to conventional didactic teaching. Both groups received identical nutrition content — eight one-hour weekly sessions covering food groups, portion control, nutrient functions, beverage choices, and strategies for overcoming barriers to healthy eating — but the delivery differed entirely.
In the intervention group, students worked in small groups, took on rotating teaching roles, debated food choices, and solved real-life dietary dilemmas together through buzz group discussions, jigsaw learning, and role-play. In the control school, sessions looked like a standard classroom lesson: the teacher talked, the students listened. At the end of eight weeks, and again four weeks later, we assessed diet quality using the validated Diet Quality Questionnaire (DQQ) and measured nutrition knowledge with a validated instrument.

What we found
The results were striking. Across every major diet quality indicator, adolescents in the collaborative learning group outperformed their counterparts. The Global Dietary Recommendations (GDR) score — a composite measure of overall diet quality — rose by nearly five points in the intervention group compared to less than one point in controls. Their NCD-Protect score, measuring consumption of health-promoting foods like fruits, vegetables, pulses, and whole grains, jumped by nearly four points. Meanwhile, their NCD-Risk score fell by more than one point; in the control group, it barely moved. Improvements in nutrition knowledge followed the same pattern: intervention participants gained nearly 10 percentage points, while the control group scores changed by less than 2. After adjusting for baseline differences and sociodemographic factors through ANCOVA, the intervention effect remained large and statistically robust, with partial η² of 0.26 for GDR score and 0.13 for nutrition knowledge.
One finding gave us pause: processed meat consumption increased at the endline in the intervention group. This likely reflects the realities of the food environment — in peri-urban Ogun State, processed meat products are inexpensive and widely available. It is a reminder that school education alone cannot fully counteract food environment pull, and that future curricula should explicitly address processed meat risks.
Why this matters
Many school-based nutrition programmes improve knowledge without changing what adolescents actually eat. Our findings suggest that how nutrition is taught may be as important as what is taught. Collaborative learning — with its emphasis on peer interaction, shared problem-solving, and active engagement — appears to connect knowledge to behaviour in ways that passive instruction does not. The intervention is not expensive or complex. It uses existing classroom infrastructure, standard nutrition content, and facilitation skills that trained nutritionists and teachers can learn. Scaling it requires investment in teacher training and curriculum integration, not a wholesale reimagining of school health policy.
What comes next
This was a short-term study in two private schools. We do not yet know whether improvements persist over months or years, how the intervention performs in public schools or rural settings, or how effects vary across socioeconomic groups beyond what our design could capture. Cluster-randomised trials with longer follow-up, multiple schools, and mixed school types are needed. Incorporating anthropometric outcomes alongside diet quality could also provide a fuller picture of impact.
Adolescents are among the most nutritionally vulnerable populations in the world, and among the most underserved in targeted programmes. Getting nutrition education right for them — not just in content but in method — could matter enormously for chronic disease trajectories across a generation.
Follow the Topic
-
Discover Public Health
This is an open access journal publishing research from all fields relevant to public health.
Related Collections
With Collections, you can get published faster and increase your visibility.
Antimicrobial Resistance: The New Challenge to Global Health in a Post-Pandemic World
Antimicrobial resistance (AMR) is a seriously ongoing threat to global health, occurring when bacteria, fungi, viruses, and parasites evolve to resist the drugs designed to kill or block them. The COVID-19 pandemic has both directly and indirectly exacerbated the problem of AMR, as the overuse of antibiotics has accelerated the development of resistance in many pathogens. COVID-19 may have subsided, but AMR continues to pose a significant risk to the effectiveness of global healthcare systems, threatening to reverse decades of progress in combating infectious diseases. The interplay between population health and AMR has become increasingly critical as healthcare practices have shifted in response to the pandemic. Understanding this relationship is essential for developing effective strategies to mitigate the impact of AMR on population health in a post-COVID context.
The motivation for launching this Collection arises from the urgent need to address the rising tide of AMR as healthcare systems grapple with the long-term effects of the pandemic. Increased antibiotic use during COVID-19 treatment, changes in healthcare access, and disruptions in public health interventions have all contributed to an environment where AMR can thrive. Moreover, the pandemic has highlighted the importance of a multidisciplinary approach to tackling AMR, involving epidemiology, policymaking, and community health initiatives. This Collection aims to provide a platform for researchers and practitioners to share insights and findings that can inform future strategies to combat AMR while considering the broader implications for population health.
This Collection aims to highlight the multifaceted nature of AMR in a post-pandemic environment. We solicit articles that investigate the particular issues provided by the pandemic in terms of AMR development and containment, examine the impact of AMR on many sectors of healthcare, and propose novel strategies to minimize resistance propagation. Submissions may include original research, policy assessments, program evaluations, and comments on the following major areas:
• Epidemiology and trends of AMR post-pandemic
• Impact of COVID-19 on antibiotic usage
• Surveillance strategies for AMR
• AMR and stewardship
• Prevention and control measures to limit AMR spread
• Policies and programs to promote antibiotic stewardship
• Economic and social implications of AMR
• Global collaboration and initiatives to tackle AMR
By addressing these critical issues, this Collection aims to provide a comprehensive understanding of the emerging challenges in antimicrobial resistance in a post-pandemic world and to promote effective strategies to preserve the power of our current antimicrobials.
Keywords: antimicrobial resistance; COVID-19; antibiotics; global health; infectious diseases; public health; policy; prevention
This Collection supports and amplifies research related to SDG 3.
Publishing Model: Open Access
Deadline: Jun 30, 2026
Digital Frontiers in Public Health: Data-driven Solutions and Technologies for Efficiency, Effectiveness, and Equity
In recent years, the landscape of public health has been transformed by unprecedented access to high-quality data, advances in data storage and processing, and a growing willingness to share information across jurisdictions. The global response to the COVID-19 pandemic exemplified how coordinated data use and technological innovation can accelerate decision-making, enhance surveillance, and save lives. These developments mark a new era in which the application of modern data analytics in evidence-driven public health practices is not only possible but essential.
Building on this momentum, contemporary innovations are contributing to significant improvements in the three Es of public health: efficiency, effectiveness, and equity. Improved efficiency enables resources to be allocated and managed in a manner that generates the maximum attainable outputs; enhanced effectiveness ensures that public health policies, interventions, and practices achieve the expected health outcomes; and strengthened equity promotes fair access to healthcare and public health services across all populations. Together, these dimensions reflect the evolving priorities and capabilities of modern public health systems.
This Collection, “Digital Frontiers in Public Health: Data-driven Solutions and Technologies for Efficiency, Effectiveness, and Equity,” invites contributions that explore these themes through empirical studies, methodological advancements, case studies, and policy analyses. We seek manuscripts that highlight innovative data applications, cross-sector collaborations, digital health initiatives, and strategies that enhance equity through technology and data integration, as well as collaborative public health practices.
Topics of interest include, but are not limited to:
- Applications of novel data linkage and analytics methods in public health
- The role of participation and co-creation in addressing public health issues
- Digital and technological innovations in public health
- Complete or partial assessments of triple Es in public health
- Economic evaluations of public health interventions
By showcasing diverse approaches from around the world, this Collection aims to provide a comprehensive overview of how data-driven innovations are reshaping public health practice today, and in the future. Researchers, practitioners, and policymakers are encouraged to share their insights and experiences to contribute to this critical dialogue on the future of public health.
This Collection supports and amplifies research related to SDG 3.
Keywords: digital applications; data sharing; data infrastructure; economic evaluations; health equity; public health; policy analysis; health informatics
Publishing Model: Open Access
Deadline: Sep 30, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in