Behind the Paper: Survey of lived experiences and challenges in hepatitis B management and treatment
Published in Microbiology, General & Internal Medicine, and Public Health
Over 250 million people are living with hepatitis B worldwide and approximately 20 to 30 percent of those infected will develop life-threatening complications, including cirrhosis and liver cancer. Globally, the majority of individuals remain undiagnosed, and out of care. Individuals who are aware of their infection, particularly within low and middle income countries, face significant health disparities (including costs for testing, management and treatment, access to a knowledgeable health care provider, stigma and discrimination) that limit the ability to following to the standard guideline recommendations for treatment and management.
What inspired this study?
To gain a better understanding of the values and preferences from people with hepatitis B regarding their care, our team conducted a survey to better understand diagnostics, treatment and management preferences and barriers to accessing care for hepatitis B. This study reports on survey findings and provides insight into the current lived experiences of people with hepatitis B and suggestions for improving care service delivery and management. The survey results can be used to inform key updates and considerations to hepatitis B clinical management and treatment recommendations within future hepatitis B guideline development.
Why is it important?
Despite significant mortality, only approximately 10% of people with hepatitis B are diagnosed and therefore there is a major diagnostic and care gap for those with hepatitis B worldwide. Disparities and limited clinical management including treatment, particularly in low and middle-income countries (LMIC), is a significant challenge for those diagnosed with hepatitis B. There is limited literature about patient values and preferences related to testing, management and treatment of hepatitis B. Our intent is to fill that gap and call attention to the need for more research in this space.
What makes this study unique?
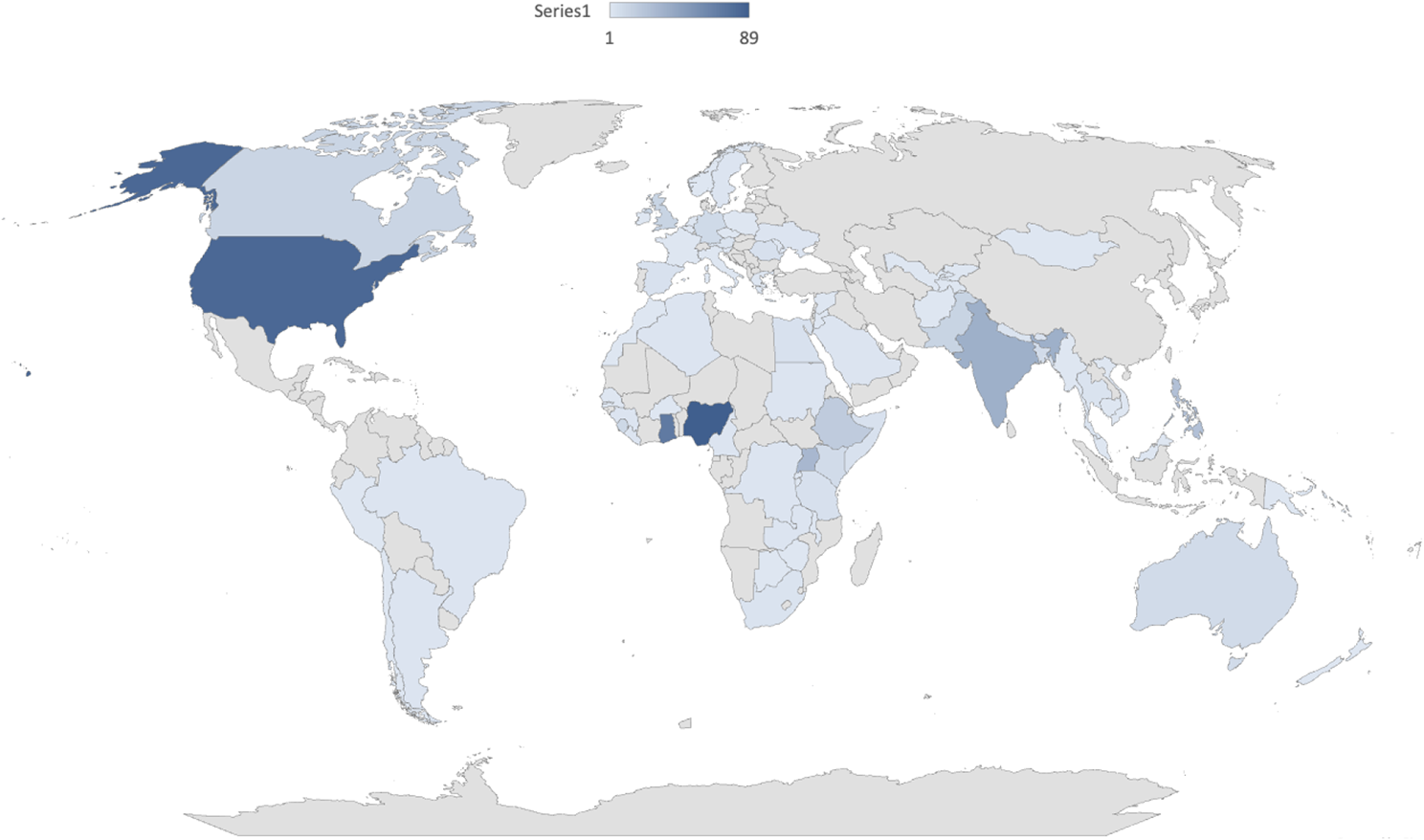
This study was unique in that it was a global survey examining lived experiences and treatment preferences for those with hepatitis B. It is one of the first that examines treatment values and preferences.
Did this study show anything unexpected?
Almost all individuals responding to the survey expressed the desire to be involved in care and treatment decisions around their hepatitis B management. This encourages the need for more shared decision-making models of care delivery including peer support for people with hepatitis B and strengthened relationships between providers and their patients. Additionally, having a knowledgeable health care worker and one that could empathize with those with hepatitis B was a challenge for many, particularly those in low- and middle-income countries. This emphasizes the low knowledge and awareness among health care providers and the need for enhanced hepatitis B specific training of providers. Access to affordable testing and treatment was a major barrier of care for people with hepatitis B due to the high out-of-pocket expenses required for hepatitis B management.
What is the wider significance of the study findings?
Takeaways from this study involve addressing access to management and care challenges reported within this survey so guidelines and recommendations can be applicable to those directly impacted by hepatitis B. Another significant finding is the need for expansion of health care worker training to ensure accurate and appropriate management for hepatitis B occurs within health care settings. The third major point is that shared decision making is a key aspect of care delivery and should be integrated within hepatitis B service delivery. And finally, survey findings demonstrate the social and psychological consequences associated with a hepatitis B diagnosis like stigma and discrimination. The stigma and discrimination associated with hepatitis B have also been linked to poor knowledge of hepatitis B among both providers and the general public and misconceptions around hepatitis B transmission. Education surrounding hepatitis B among both the general population and providers is essential to reduce these negative consequences of hepatitis B that impact those diagnosed.
Peer support: Downs LO, Kabagambe K, Williams S, et al. Peer support for people living with hepatitis B virus—A foundation for treatment expansion. J Viral Hepat. 2024; 00: 1-10. doi:10.1111/jvh.13952
Freeland, C., Qureshi, A., Wallace, J. et al. Hepatitis B discrimination: global responses requiring global data. BMC Public Health 24, 1575 (2024). https://doi.org/10.1186/s12889-024-18918-8
Freeland, C., Mendola, L., Cheng, V. et al. The unvirtuous cycle of discrimination affecting people with hepatitis B: a multi-country qualitative assessment of key-informant perspectives. Int J Equity Health 21, 77 (2022). https://doi.org/10.1186/s12939-022-01677-6
Follow the Topic
-
BMC Public Health
An open access, peer-reviewed journal that considers articles on the epidemiology of disease and the understanding of all aspects of public health.
Related Collections
With Collections, you can get published faster and increase your visibility.
Monitoring, preventing, and managing type 2 diabetes
BMC Public Health is calling for submissions to our Collection on Monitoring, preventing, and managing diabetes at the population level. With rates of type 2 diabetes rising globally, especially in low- and middle-income countries and underserved communities, prevention strategies are critical. As the disease progresses people with diabetes are at increased risk of complications such as cardiovascular and kidney diseases, neuropathy and visual loss.
This Collection seeks submissions that explore population-level approaches to monitoring rates of diabetes, preventing or delaying the development of type 2 diabetes, and system-wide efforts to improve the management of the disease and reduce rates of complications, with a focus on improving health outcomes and reducing healthcare burdens.
Submissions are encouraged on primary prevention initiatives and culturally adapted, community-level interventions to reduce the risk of diabetes. Research aimed at improving systems for monitoring rates of diabetes and its complications through routinely-collected health data, or for improving management by enhancing patient engagement with healthcare systems or better identifying those in need, are encouraged. Research on diabetes education and support systems is also welcomed, with a focus on empowering individuals to adopt and sustain healthier lifestyles and avoid known causes of diabetes.
Additional topics of interest include (but are not limited to):
Access to healthcare and diabetes management
The impact of food insecurity on diabetes outcomes
Community-based interventions for low-income populations
Interventions to reduce exposure to environmental causes of diabetes
Financial barriers to diabetes medication and treatment
Housing instability, employment status and type 2 diabetes
Health literacy, poverty, and diabetes management
Policies to reduce poverty-related health disparities in diabetes
This Collection supports and amplifies research related to SDG 3: Good Health & Well-Being.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jul 16, 2026
Male reproductive health
BMC Public Health invites submissions to our new Collection, "Male reproductive health”. Male reproductive health is an essential yet often overlooked aspect of public health that encompasses various factors affecting men's fertility and overall well-being. Issues such as declining sperm counts, poor sperm quality, the impact of environmental exposures and the effects of lifestyle and dietary factors on reproductive outcomes are gaining increasing attention.
This Collection seeks to examine the multifaceted influences on male reproductive health, considering environmental, infectious and sociocultural dimensions that affect male reproductive parameters and contribute to fertility challenges. Continued research in this area could help identify causative factors and contribute to advances in public health policies, ultimately benefiting future generations.
Key topics of interest include, but are not limited to:
Environmental pollution and reproductive health
Sperm count trends and implications for fertility
The role of occupational exposures in male fertility
The effects of infectious diseases on sperm parameters
Impact of diet and lifestyle factors on sperm quality and fertility
Psychological factors influencing reproductive health
Interventions for improving male reproductive health
This Collection supports and amplifies research related to Sustainable Development Goal 3- Good Health and Well-Being.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jun 29, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in
Great story and well-conducted study