Beyond the scales. What MRI reveals when weight changes
Published in General & Internal Medicine

Today, many people live with overweight or obesity — long‑term health conditions that often require ongoing care, support, and management. Losing 10% of your body weight is a real milestone, and the number on the scales can feel reassuring. But inside the body, the story is far more complex, and far more fascinating than a single measurement can show.
Weight changes reflect changes in both fat and muscle and fat does not simply disappear evenly. It shrinks faster in some areas, lingers in muscle tissue, and it behaves very differently in the liver compared with under the skin. These details matters more than ever as a new generation of weight-loss medications, including the GLP-1 receptor agonists like Wegovy, and Mounjaro, transform obesity treatment. Yet despite these advances, most clinicians and clinical trial researchers still largely rely on body weight alone to judge whether a treatment is working.
To understand the real health impact of these new treatments, researchers and clinicians first need a clear picture of how fat and muscle change naturally, without any drugs. Our study provides that baseline, a reference point captured in adults before GLP-1 therapies transformed the field. By showing what healthy, untreated weight change looks like inside the body, this work can help improve how future clinical trials are designed and interpreted.
Why body weight alone isn't enough
Two people can have the same body weight yet store fat in completely different ways. One may have harmful fat packed around the organs or inside the liver, while another stores most of their fat under the skin, where it poses far less risk. When someone loses weight, the changes happening inside their body are far more nuanced than the number on the scales. Fat is stored in several places, around the organs (visceral fat, or VAT), under the skin (subcutaneous fat, or SAT), and even inside the liver and muscle.
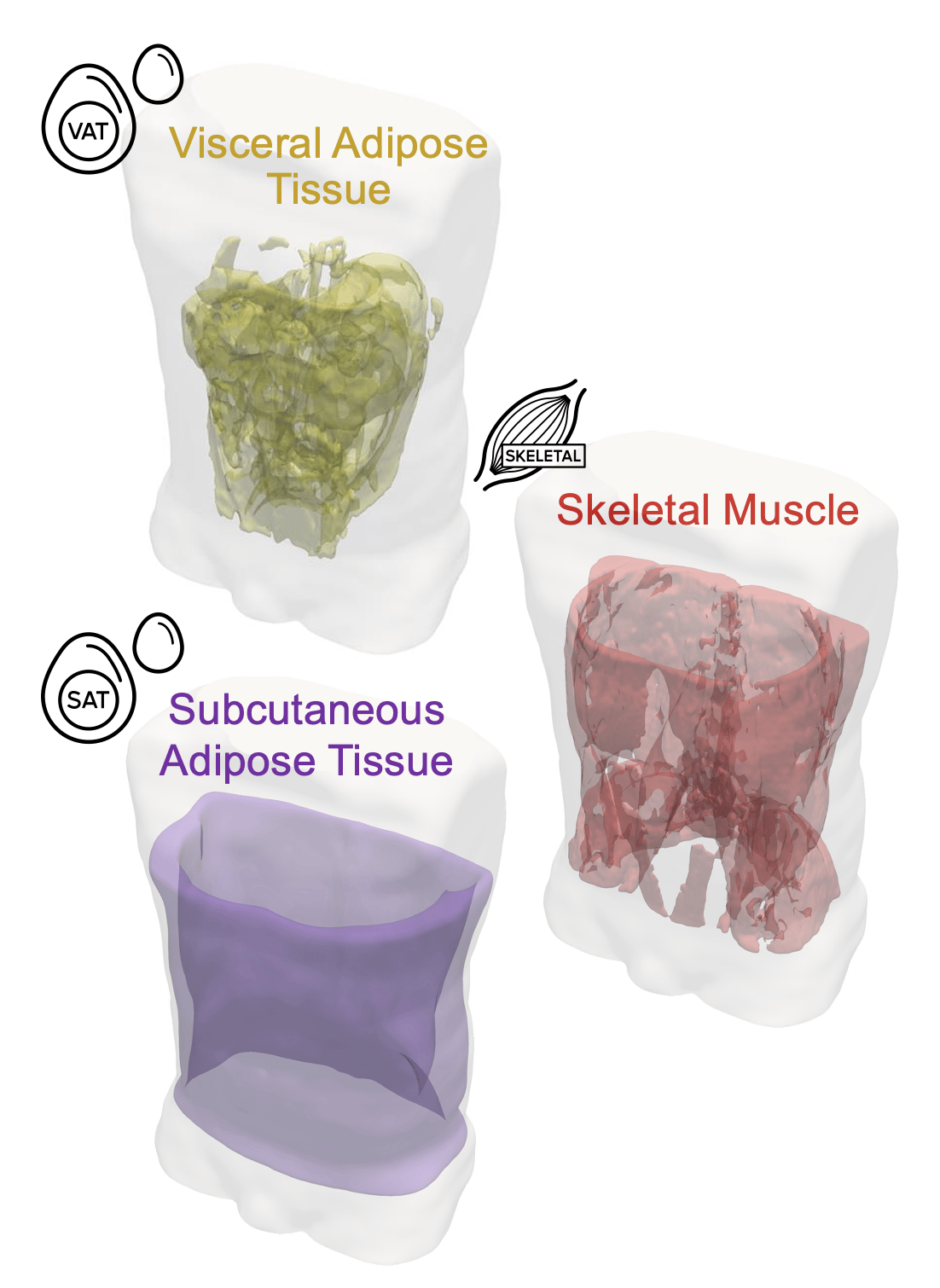
Each of these fat depots behaves differently during weight gain and weight loss and each carries different health implications for long‑term health.
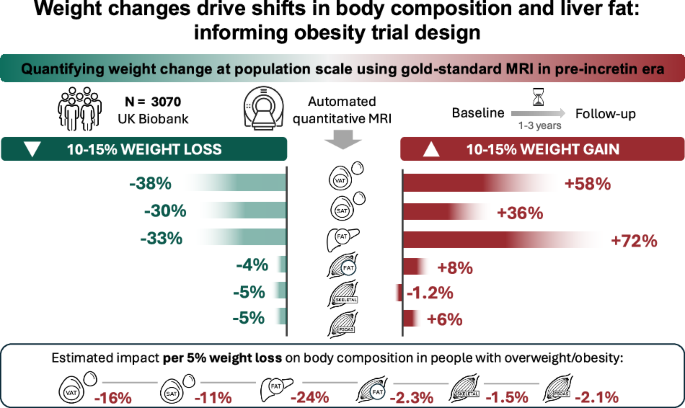
To understand these patterns, we used quantitative MRI, the gold standard for measuring body composition safely and precisely, without radiation, contrast agents or invasive procedures. We analysed MRI scans from around 3,000 adults in the UK Biobank, each scanned twice roughly 2.5 years apart, all before GLP-1 therapies became more widely prescribed. This gave us a real-world window into what happens to the body during natural weight gain and weight loss, without the influence of modern weight-loss drugs.
Visceral and liver fat – big changes seen with MRI gold standard assessment
One of the most striking findings was how quickly the liver responds to weight change. Among people who gained 10–15% of their body weight, liver fat content rose by roughly 70% relative to where they started, meaning that someone who began with a liver fat of 5%, the clinical threshold for metabolic dysfunction‑associated liver disease, could end up closer to 8–9%. In contrast, people who lost the same amount of weight saw liver fat fall by about one-third. Visceral fat followed a similar pattern: a ~60% relative increase with substantial weight gain, and a ~40% relative decrease with substantial weight loss. Clearly, the changes were not mirror images. The body accumulated visceral and liver fat more readily than it lost it, an important consideration when predicting how an untreated group might change during a clinical trial.
People do not all respond in the same way. Those with type 2 diabetes showed changes of a different magnitude in visceral and liver fat, while people taking blood pressure medications showed more muted changes in both directions. These differences matter when designing and interpreting trials.
Muscle behaves differently from fat
Skeletal muscle told a different story. Muscle volume did not increase when people gained weight, but it did shrink when they lost weight, and this happened even with modest weight loss of just 2-5%.
Fat inside the muscle behaved differently again, it increased readily with weight gain but was stubborn to reduce, only falling meaningfully with large weight loss of 10-15%. Together, these findings paint a challenging picture: gain weight and fat infiltrates the muscle; lose weight and muscle volume drops while the fat inside it barely moves. Even small amounts of fat in muscle are linked to reduced muscle function.
DXA lean mass does not tell you what exactly is happening to muscle
Many clinical trials use DXA (dual-energy X-ray absorptiometry) scans to measure “lean mass” as a proxy for muscle. But in our study, changes over time in DXA-derived lean mass only weakly reflected the true changes seen with muscle volume measured with MRI. DXA also cannot detect fat infiltrating muscle tissue. Given how differently muscle volume and muscle fat respond to changes in weight, relying on DXA alone may miss important effects of weight-loss drugs.

What comes next: trial design with an MRI reference dataset
A practical outcome of this work is the ability to design more informative clinical trials. Using our dataset, we created a "virtual placebo arm", a model of how body composition changes naturally with weight loss in people with overweight or obesity. This makes it possible to estimate how each fat and muscle depot typically changes for every 5% of weight lost, without any medication involved. The results reported give trial designers something concrete: a natural baseline to measure against, a way to calculate how many participants a study needs, and a reference for what the untreated group is likely to do. All derived from the era before GLP-1 therapies changed the picture.

This work has been published in the International Journal of Obesity. The data derive from the UK Biobank (access application 9914). Full author contributions, competing interests, and data availability statements are available in the published manuscript.
Image: Dr Luis Felipe Cardiel
Follow the Topic
-
International Journal of Obesity
This is a multi-disciplinary forum for research describing basic, clinical and applied studies in biochemistry, physiology, genetics and nutrition, molecular, metabolic, psychological and epidemiological aspects of obesity and related disorders.



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in