Navigating the Future of Health Research: Evidence for the FP10 Debate
Published in Social Sciences and Public Health
As the European research community turns its attention toward the start of the 10th Framework Programme (FP10) in 2028, the debate over the direction of public funding has reached a critical juncture. With the European Commission proposing a nearly doubled budget of €175 billion and a restructured architecture that emphasizes “Competitiveness and Society,” policymakers are grappling with a fundamental question: how can research funding best address the complex health challenges of the 21st century while maintaining scientific excellence?
In this context, our recent study, “Evolution of public funding for collaborative health research towards higher-level patient-oriented research,” provides an empirical foundation for this discussion. By analyzing over 26,000 projects and their associated publications across European Framework Programmes and the U.S. National Institutes of Health (NIH), we offer a data-driven perspective on how public funding is evolving—and why this evolution matters for the future of health research.
Observable Shifts in Research Portfolios
One of the central findings of our study is that public funding for collaborative health research is undergoing a measurable and systematic reorientation. This is particularly visible in the European Union’s Framework Programmes.
Our analysis shows a pronounced shift in project-level priorities. While FP7 (2008–2014) maintained a significant focus on biomedical mechanisms, Horizon 2020 (2015–2021) and the early years of Horizon Europe have moved decisively toward higher-level research, including health systems, policy, and population-level approaches.
In Horizon 2020, for example, more than a third of collaborative health projects were classified in health management and policies, while only a small share focused on basic biomedical mechanisms. This transition reflects a deliberate effort to bring research closer to clinical application and societal implementation.
Importantly, these changes are not merely rhetorical. They are observable and measurable, based on large-scale analysis of both funded projects and their resulting scientific publications.
Understanding the Drivers of Change
This shift is best understood not as a short-term political adjustment, but as part of a broader evolution in how health challenges are conceptualized (see figure).
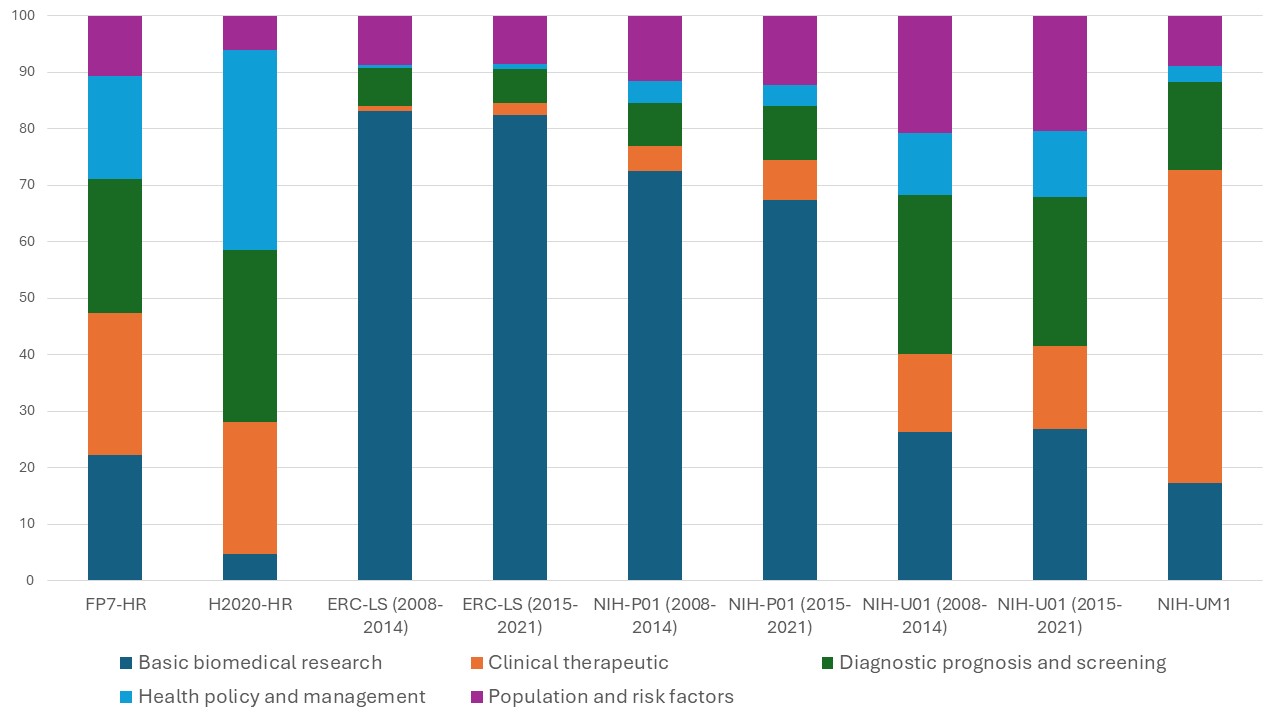
Figure. Distribution of health research orientations across major public funding programmes. The figure shows the percentage of funded projects classified by level of health research—from basic biomedical research to population and health systems research—across EU Framework Programmes, ERC, and NIH funding instruments. It highlights the shift toward higher-level, patient-oriented research in collaborative programmes, while basic research remains a central component across all funding schemes.
Many of today’s major health issues—such as antimicrobial resistance, mental health, and chronic diseases—are increasingly recognized as complex, multi-level phenomena. Addressing them requires not only biological insight, but also an understanding of social, environmental, and economic determinants.
In response, funding agencies have expanded their portfolios to support interdisciplinary, collaborative, and more societally oriented research. In the European context, call-based funding mechanisms have proven particularly effective in aligning research efforts with emerging public health priorities.
The Myth of Displacement: Strategic vs. Basic Research
A recurring concern in policy debates is that the rise of strategic, mission-oriented funding may come at the expense of basic science. Our findings provide a clear and important clarification: this is not what we observe in practice.
While project descriptions in collaborative programmes have shifted toward applied and societal goals, publication outputs show a more stable pattern. Basic biomedical research remains a central component, even within programmes explicitly designed to support health systems and policy-oriented work.
This indicates that research conducted in problem-oriented contexts continues to generate fundamental scientific knowledge. Rather than replacing basic research, strategic funding appears to embed it within broader, more application-oriented research trajectories.
From a policy perspective, this suggests that the research system functions as an integrated ecosystem, where applied and fundamental research are mutually reinforcing.
Complementarity as a Design Principle
A key implication of our study is that the strength of research systems lies in the complementarity of their funding instruments.
Investigator-driven funding schemes—such as the European Research Council (ERC) or NIH programmes—are highly effective at supporting frontier research and deep specialization. In contrast, collaborative and policy-driven programmes are essential for addressing complex, system-level challenges that require coordination across disciplines and sectors.
These are not competing models. They are structurally distinct but mutually reinforcing components of a well-functioning research ecosystem.
The policy implication is straightforward: achieving both scientific excellence and societal impact does not require trade-offs, but rather the careful design of diversified and coordinated funding portfolios.
Opportunities for FP10
For those involved in shaping FP10, these findings offer a useful perspective on how to position health research within the proposed “Competitiveness and Society” pillar.
Integrating health into a broader framework can support the continued transition toward systems-oriented and population-level research, particularly by facilitating connections with areas such as digital technologies, environmental change, and social innovation.
At the same time, maintaining the visibility of health as a priority will depend on implementation choices, including:
- Clearly defined thematic priorities
- Strong coordination mechanisms
- Sustained support for research communities
FP10 also provides an opportunity to further develop integrative approaches such as One Health, and to leverage emerging technologies—including artificial intelligence—in addressing complex health challenges.
Broader Relevance: Lessons Beyond Europe
Although this study focuses in part on European funding, its insights are also relevant in other contexts, particularly the United States.
The NIH model, with its strong emphasis on investigator-driven research, illustrates a different pathway: one based on stability and incremental adaptation, complemented by targeted strategic initiatives.
Comparing these systems highlights how institutional design shapes the ways in which research portfolios evolve. The European model enables more direct steering through funding calls, while the NIH model supports gradual integration of new priorities within a stable research base.
Understanding these differences can help policymakers and scholars on both sides of the Atlantic better navigate the challenges of aligning research systems with societal needs.
Conclusion: Evidence for a More Responsive Research System
Our study contributes to the FP10 debate by grounding it in empirical evidence rather than assumptions. It shows that the shift toward patient-oriented and systems-level research is not only real, but already underway.
At the same time, it demonstrates that this evolution does not come at the expense of foundational science. Instead, it reflects the emergence of a more differentiated and interconnected research ecosystem.
For policymakers and research scholars, the key takeaway is clear: the goal is not to choose between excellence and impact, but to optimize the relationship between them.
By supporting a diverse set of funding instruments—each fulfilling complementary roles—public research systems can continue to advance both the frontiers of knowledge and the solutions needed to address the most pressing health challenges of our time.
David Fajardo-Ortiz, Bart Thijs, Wolfgang Glänzel, Karin R. Sipido; Evolution of public funding for collaborative health research towards higher-level patient-oriented research. Quantitative Science Studies 2026; doi: https://doi.org/10.1162/QSS.a.472

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in