Proton boron capture therapy (PBCT) in glioblastoma model
Published in Cancer
Glioblastoma (GBM) patients usually receive a combination of aggressive therapeutic regimens using temozolomide, radiotherapy and surgery, whether applicable. This approach is often limited by hypoxia, radioresistance and chemoresistance, which ultimately lead to recurrences and reduced overall survival. Moreover treatments strongly reduce the quality of life and the need to improve cell-killing efficacy using ionizing radiation becomes undisputable1. The use of radiosensitizing agents, such as boron-containing molecules, offers the opportunity to increase proton-induced cell death and selectivity.
Key findings
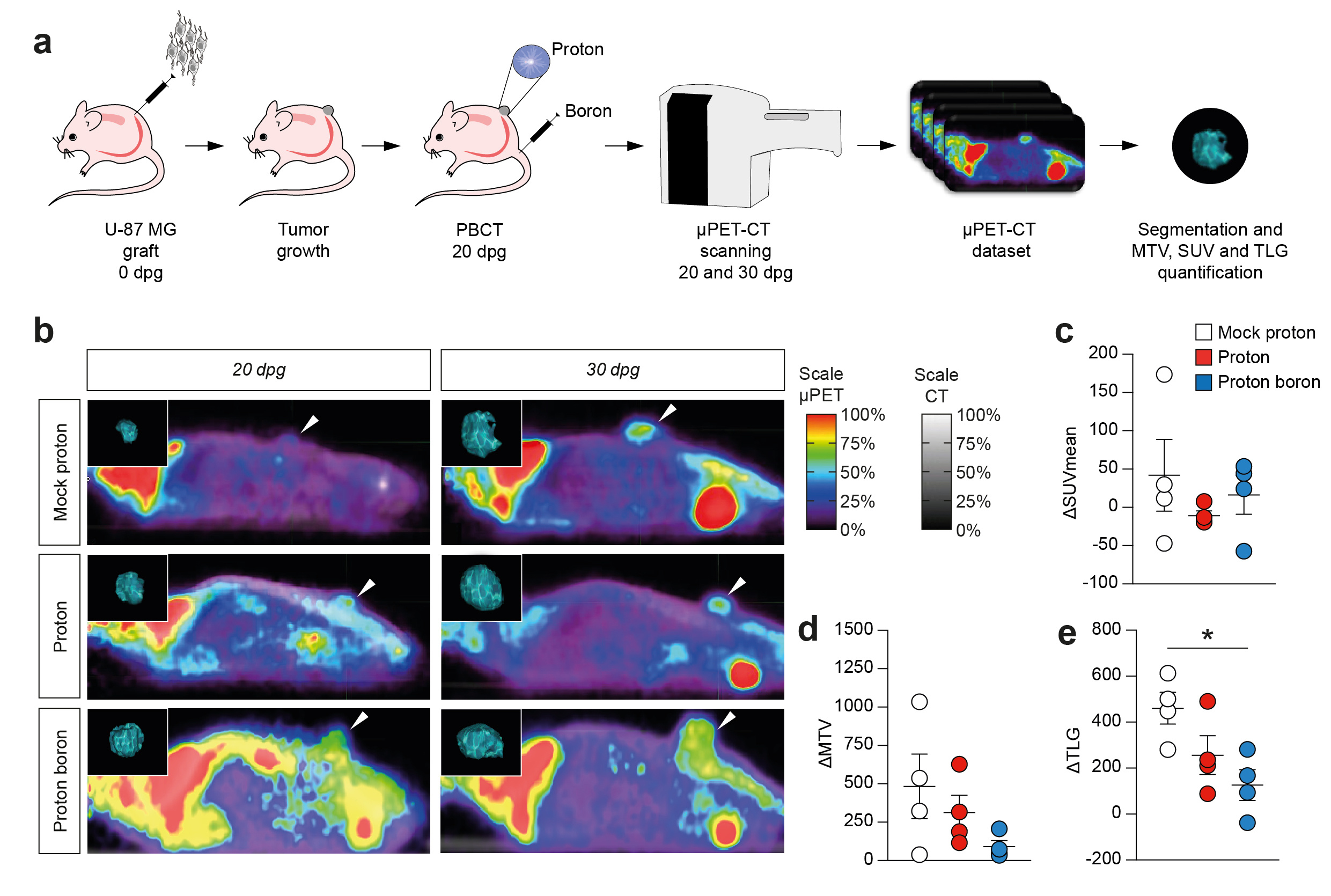
Here we explored the effect of Proton Boron Capture Therapy (PBCT) in a preclinical model GBM. We performed proton irradiation in a heterotopic model of GBM using sub-therapeutic dose of 10 Gy at 20 days post graft (dgp). Proton Boron Capture Therapy (PBCT) mice received a single i.p. injection of boronophenylalanine. Data showed a significant reduction of total lesion glycolysis, assessed using a μ positron emission tomography-computed tomography (μPET-CT) analysis in live imaging. We quantified a clinically scalable PET parameter (i.e. TLG), providing a simultaneous estimation of MTV and SUV for volumetric and metabolic information2. Results suggest a reduction of ΔTLG, indicating a better response in PBCT as compared to control and protons alone.
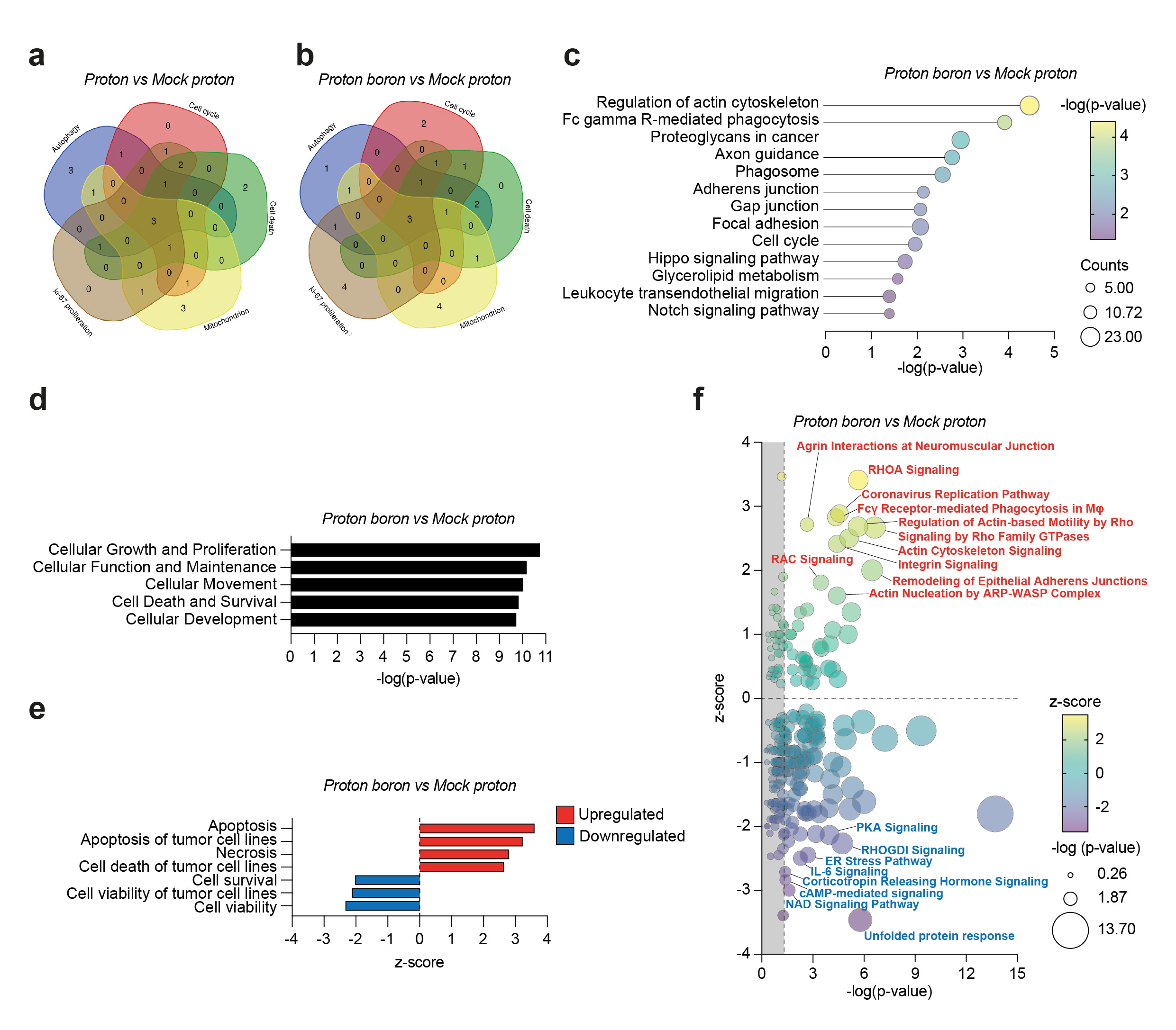
To identify detailed molecular pathways involved in PBCT-mediated effects, we performed an RNA-seq analysis on tumor biopsies, finding a significant alteration of pathways involved in cytoskeleton reorganization and cell-to-cell intercellular communication, such as adherens junction and gap junction, activated in PBCT group as compared to controls3. Notably our findings also support the hypothesis of PBCT effects on cell cycle deregulation, induction of cell death and anti-proliferative/pro-apoptotic signalling. It is worth noticing that we observed an involvement of Notch signalling, known to regulate cell fate via autophagy/apoptosis transition, RAC signalling, involved in autophagic response to chemo- and radio-resistance4,5.
Ex vivo analysis on biopsies showed that PBCT increases mitochondrial autophagy. Analysis of colocalization index between markers of autophagy and mitochondria showed a significant increase of colocalization index, suggesting that PBCT increase tumor autophagy and mitophagy.
Take-home message
In conclusion, we showed the effect of PBCT in an in vivo experimental model of GBM, highlighting potential exploitable targets to be targeted in combination to PBCT. The observation of the effects of sub-therapeutic radiation regiments using protons, characterized by limited RBE, in combination with a boron-releasing molecule, showed the molecular network of interaction that induce cell death in tumor cells. Our study supports PBCT approach for GBM and opens the opportunity to study selective deliver of boron-releasing molecules in order to increase cell-specific toxicity and reducing off-target effects of radiotherapy.
References
1Torrisi, F. et al. The Hallmarks of Glioblastoma: Heterogeneity, Intercellular Crosstalk and Molecular Signature of Invasiveness and Progression. Biomedicines 10, 806 (2022).
2Stefano, A. et al. Metabolic Response Assessment in Non-Small Cell Lung Cancer Patients after Platinum-Based Therapy: A Preliminary Analysis. Curr. Med. Imaging Rev. 11, 218–227 (2015).
3Jasinska-Konior, K. et al. Increased elasticity of melanoma cells after low-LET proton beam due to actin cytoskeleton rearrangements. Sci. Rep. 9, 7008 (2019).
4Vehlow, A. & Cordes, N. DDR1 (discoidin domain receptor tyrosine kinase 1) drives glioblastoma therapy resistance by modulating autophagy. Autophagy 15, 1487–1488 (2019).
5Mardanshahi, A., Gharibkandi, N. A., Vaseghi, S., Abedi, S. M. & Molavipordanjani, S. The PI3K/AKT/mTOR signaling pathway inhibitors enhance radiosensitivity in cancer cell lines. Mol. Biol. Rep. 48, 1–14 (2021).
Follow the Topic
-
Communications Biology
An open access journal from Nature Portfolio publishing high-quality research, reviews and commentary in all areas of the biological sciences, representing significant advances and bringing new biological insight to a specialized area of research.
Related Collections
With Collections, you can get published faster and increase your visibility.
From RNA Detection to Molecular Mechanisms
Publishing Model: Open Access
Deadline: May 05, 2026
Advances in neurodegenerative diseases
Publishing Model: Hybrid
Deadline: Jun 30, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in