Religiosity Weakens Gaming Disorder Risk
Published in General & Internal Medicine and Behavioural Sciences & Psychology

Study overview
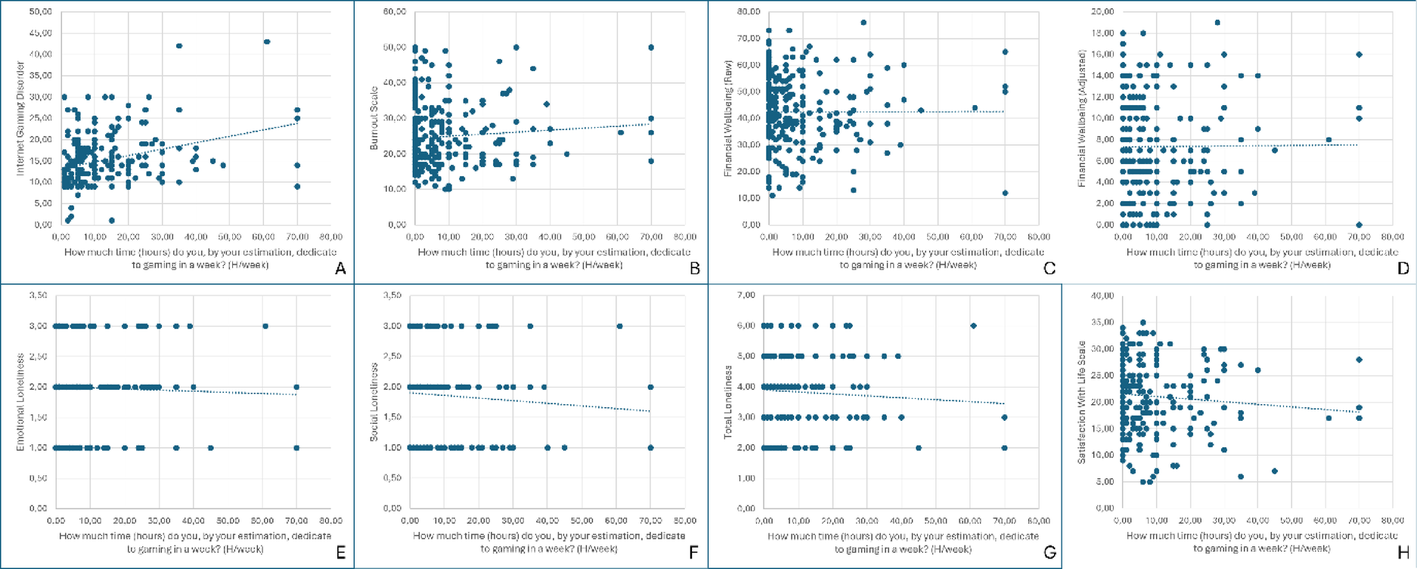
This work explores how weekly gaming duration relate to mental health outcomes in young university students in Georgia. We assessed gaming hours alongside IGD severity, burnout, loneliness, life satisfaction, financial wellbeing, and self-reported religiosity.
Although overall gaming time in our sample was modest (mean ≈ 8 hours/week), increased gaming hours were associated with higher IGD severity. Male students demonstrated significantly higher IGD scores than female students.
A protective role of religiosity
One of the central findings is that religiosity may act as a protective factor. Students with higher religiosity reported lower IGD severity, and religiosity moderated the relationship between gaming hours and IGD symptoms. This suggests that cultural and psychosocial resources could buffer some of the risks associated with problematic gaming behaviour.
Collaboration
The study was conducted in partnership with the RADAR Center at Ben-Gurion University of the Negev (Israel). Working with RADAR allowed us to integrate a broader cross-cultural perspective on digital behavior and mental health, and strengthened the methodological and analytical framework of the project. This collaboration highlights the importance of multidisciplinary and international teamwork in understanding emerging behavioral health challenges.
Why this matters
Most evidence on IGD originates from Western Europe, North America, and East Asia. Our data add insights from the Caucasus region, where cultural norms—including the role of faith communities—may shape coping strategies, socialization, and digital behavior. These findings offer valuable context for public health planning and student mental-health services.
Future directions
We anticipate that longitudinal and interventional research will clarify causal pathways (e.g., whether gaming intensity predicts burnout or vice-versa), and test whether community- or faith-based engagement can mitigate IGD-related harms in young adults.
We welcome discussion, replication efforts, and collaborative work—particularly comparisons across countries and cultures interested in youth mental health, digital behavior, and protective psychosocial factors.
Follow the Topic
-
Discover Mental Health
This is an international, open access journal that publishes research across the transdisciplinary field of mental health research.
Related Collections
With Collections, you can get published faster and increase your visibility.
Child and Adolescent Mental Health: Challenges and Innovations
Child and adolescent mental health is an urgent global concern, with increasing prevalence of anxiety, depression, behavioral problems, neurodevelopmental disorders, and self-harm. Rapid social changes, academic pressures, digital and social media influences, and the lingering psychological impacts of the COVID-19 pandemic have intensified vulnerabilities in this age group. Persistent gaps remain in early detection, equitable access to care, interdisciplinary collaboration, and the safe integration of evidence-based innovations into clinical and community settings.
This Collection aims to provide a comprehensive platform for emerging research, critical reviews, and practice-based insights that advance understanding of mental health challenges among children and adolescents—while highlighting transformative innovations. We especially welcome studies on digital health and artificial intelligence (AI), including AI-assisted screening, machine learning–driven predictive models, tele-mental health, virtual reality therapies, and mobile applications designed for youth and families.
Recognizing that digital and AI-driven approaches carry unique risks for young populations, this Collection places strong and explicit emphasis on addressing the ethical, access, and data-privacy challenges embedded in these technologies. We actively encourage submissions that explore:
• Ethical safeguards and governance models for responsible AI use in youth mental health, including algorithmic transparency, bias mitigation, informed consent, and child-safeguarding principles;
• Data-privacy and security frameworks that protect sensitive behavioral, emotional, and biometric data collected through digital platforms;
• Equitable access challenges, including digital divides, disparities in device/internet availability, structural inequities, and cultural or linguistic barriers that limit benefit from digital innovations;
• Evaluation of risks, such as data misuse, surveillance, stigmatization, or unintended harms resulting from automated decision-making;
• Policy, regulatory, and implementation guidelines that ensure digital and AI tools are safe, trustworthy, and centered on the rights and well-being of children and adolescents.
By elevating these critical concerns, the Collection seeks to promote innovations that are not only technologically advanced but also ethically responsible, privacy-protective, culturally sensitive, and accessible across diverse global contexts.
In addition to digital innovations, the Collection welcomes scholarship on school-based programs, family-centered care, trauma-informed interventions, and community-level strategies. Bringing together perspectives from nursing, psychiatry, psychology, public health, data science, social sciences, and education, this Collection aims to stimulate global dialogue, strengthen evidence-based practice, and support the development of safe, scalable, and person-centered mental health solutions. Ultimately, the goal is to enhance resilience, reduce stigma, expand equitable access to quality care, and shape the future of child and adolescent mental health worldwide.
Keywords:
• Child mental health
• adolescent mental health
• Pediatric psychiatry
• cytogenetics
• neurodevelopmental Disorders
• Behavioral disorders
• Anxiety and depression
• Self-harm and suicide prevention
• Early identification and prevention
• Community-based mental health care
• Mental health nursing
• Artificial intelligence in mental health
• Tele-mental health
• mHealth applications
• Virtual reality–based interventions
• Ethical AI in youth mental health
Publishing Model: Open Access
Deadline: Aug 31, 2026
Mental Health and Psychological Well-Being of Healthcare Professionals
Healthcare professionals operate in complex, high-pressure environments where heavy workloads, role conflicts, emotional labor, ethical challenges, and adverse occupational experiences—including workplace violence, harassment, racisme, discrimination, inadequate recognition and reward, and feeling undervalued—place substantial strain on mental health and psychological well-being. These conditions are associated with burnout, moral injury, psychological distress, trauma-related symptoms, low job satisfaction, increased intention to leave, workforce attrition, and long-term mental health consequences. This Collection focuses on mental health outcomes; structural and organizational determinants; inequities and intersectional vulnerabilities; and rigorously evaluated individual-, organizational-, and system-level interventions that promote well-being, resilience, equity, and workforce sustainability among healthcare professionals across roles, settings, and global regions. The Collection particularly welcomes studies that address structural determinants, intersectional inequities, and the implementation of evidence-based interventions in real-world healthcare systems.
Keywords: Healthcare professionals; Mental health; Psychological well-being; Occupational stress; Burnout; Moral injury; Workplace violence; Harassment; Racism; Discrimination; Organizational culture; Structural inequities; Job satisfaction; Intention to leave; Workforce attrition; Resilience; Interventions; Healthcare work environment
Publishing Model: Open Access
Deadline: Nov 09, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in
This is very interesting and relevant paper in this decades. Gaming disorder significantly increases in the few recent years. Findings of this article may provide valuable information to prevent the risk of gaming disorder.
Thank you, the international cooperation is moving forward with gathering multicultural data and analysis. More papers to come.