The liver-lung axis in pulmonary vascular disease due to liver disease
Published in Cell & Molecular Biology
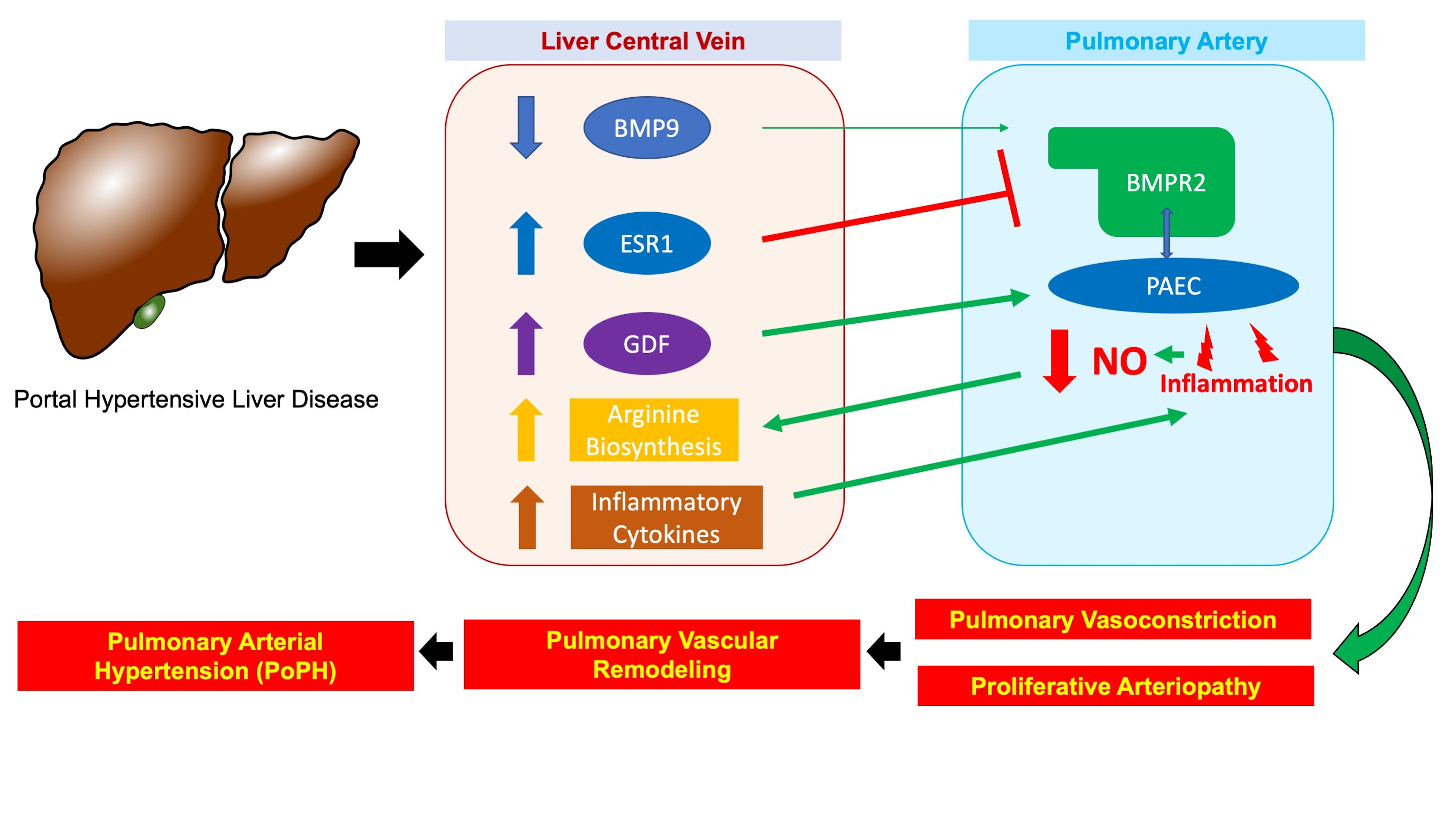
Portopulmonary Hypertension (PoPH) is a type of pulmonary vascular disease that occurs in the setting of chronic liver disease with portal hypertension. PoPH patients suffer from considerable morbidity and mortality, with a 5-year survival below 40%, even with treatment, and the presence of PoPH can severely limit treatment options for chronic liver disease. Despite the clinical scope of the problem, very little is known about the mechanisms linking portal hypertensive liver disease to pulmonary vascular remodeling in PoPH (the so-called "liver-lung" axis of disease). Although dysregulated angiogenesis and inflammation have been implicated, and a number of circulating mediators (including estrogen metabolites and members of the bone morphogenic protein family) have shown promise as clinically useful biomarkers, the precise molecular mechanisms that comprise the “liver-lung” axis of disease remain undefined. Taking advantage of the increased availability, flexibility, and affordability of next-generation sequencing technology, we sought to address this gap in knowledge by applying single nuclear RNA sequencing (snRNAseq) to human PoPH liver tissue for the first time and reporting our findings. Our ultimate goal was to describe the transcriptional and biological characteristics unique to PoPH that may form the basis of the elusive “liver-lung” axis.
We first applied snRNAseq to liver tissue samples from patients with PoPH (N=4) and non-PoPH cirrhosis (N=5) obtained at the time of transplantation.
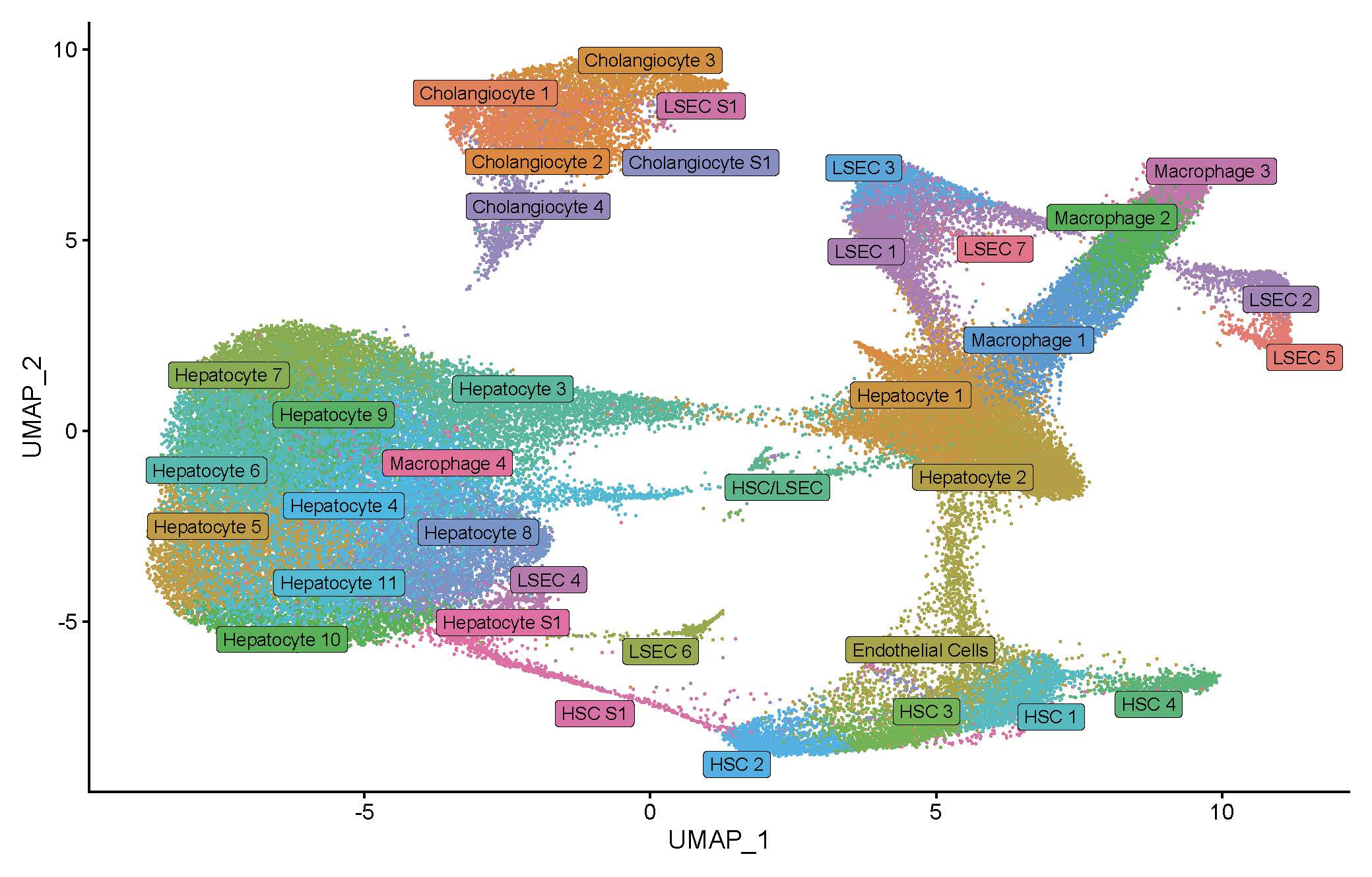
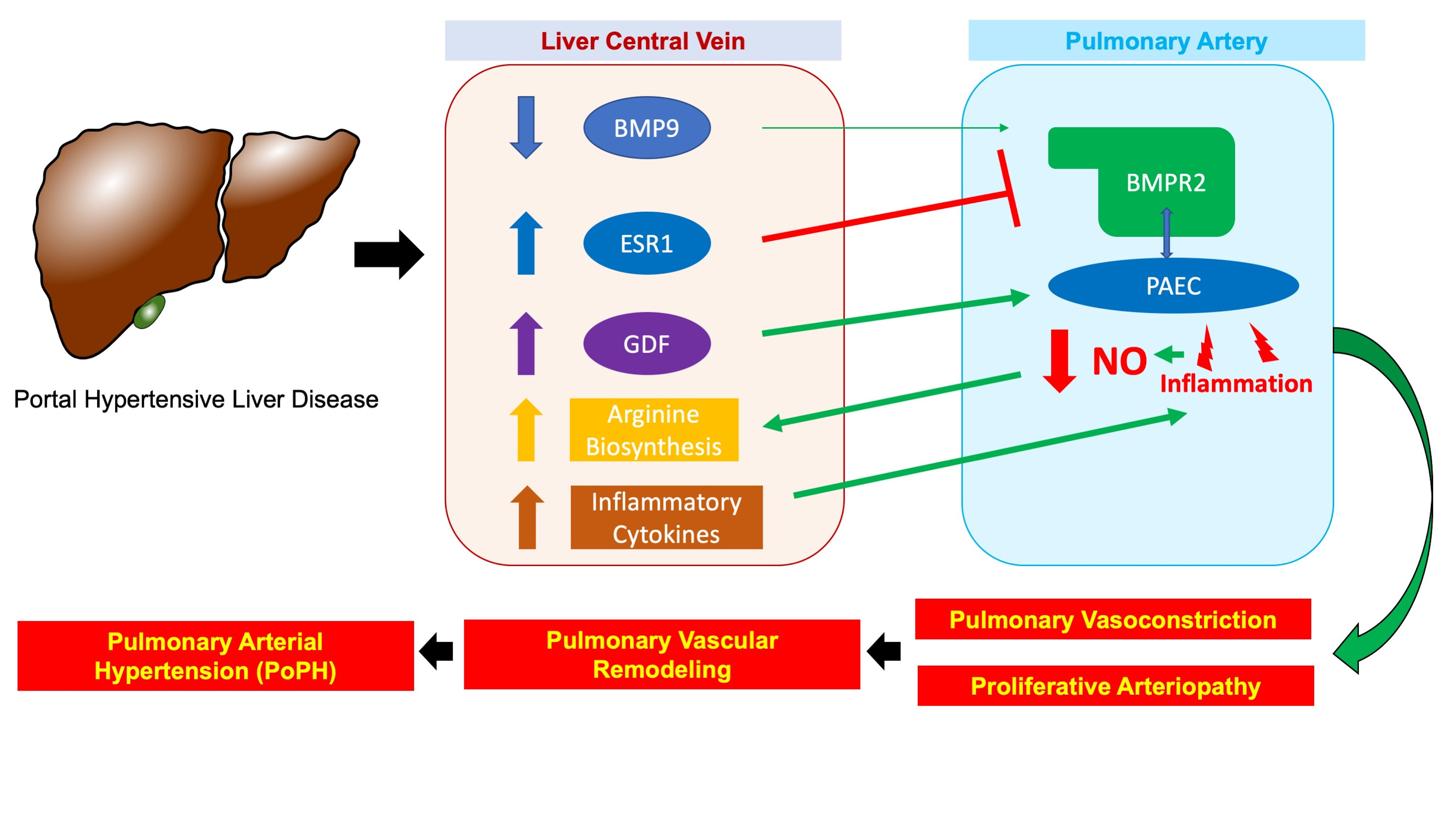
Compared to non-PoPH cirrhosis, nuclei from PoPH differentially expressed a number of genes, including those related to bone morphogenic protein type 2 (BMPR2) and estrogen signaling. Pathway analysis of PoPH differentially expressed genes indicated enrichment for pathways involved in fluid shear stress and estrogen signaling. PoPH nuclei also differentially expressed genes for inflammation and neutrophil chemoattraction. Focusing on the peri-central vein region of the liver, which is anatomically the closest avenue of communication between the hepatic and pulmonary circulation, we identified a unique signature for arginine biosynthesis and growth differentiation factor 15 (GDF15) pathway signaling in PoPH nuclei.
Turning our attention to validation of our snRNAseq data, we then applied immunohistochemistry to human liver tissue from PoPH (N=3), non-PoPH cirrhosis (N=5), and healthy (N=3) subjects. We observed relatively greater staining for the estrogen receptor (ESR1) protein, and relatively less staining for the BMPR2 protein, in the region surrounding the liver central veins of PoPH subjects as compared to non-PoPH cirrhosis subjects.
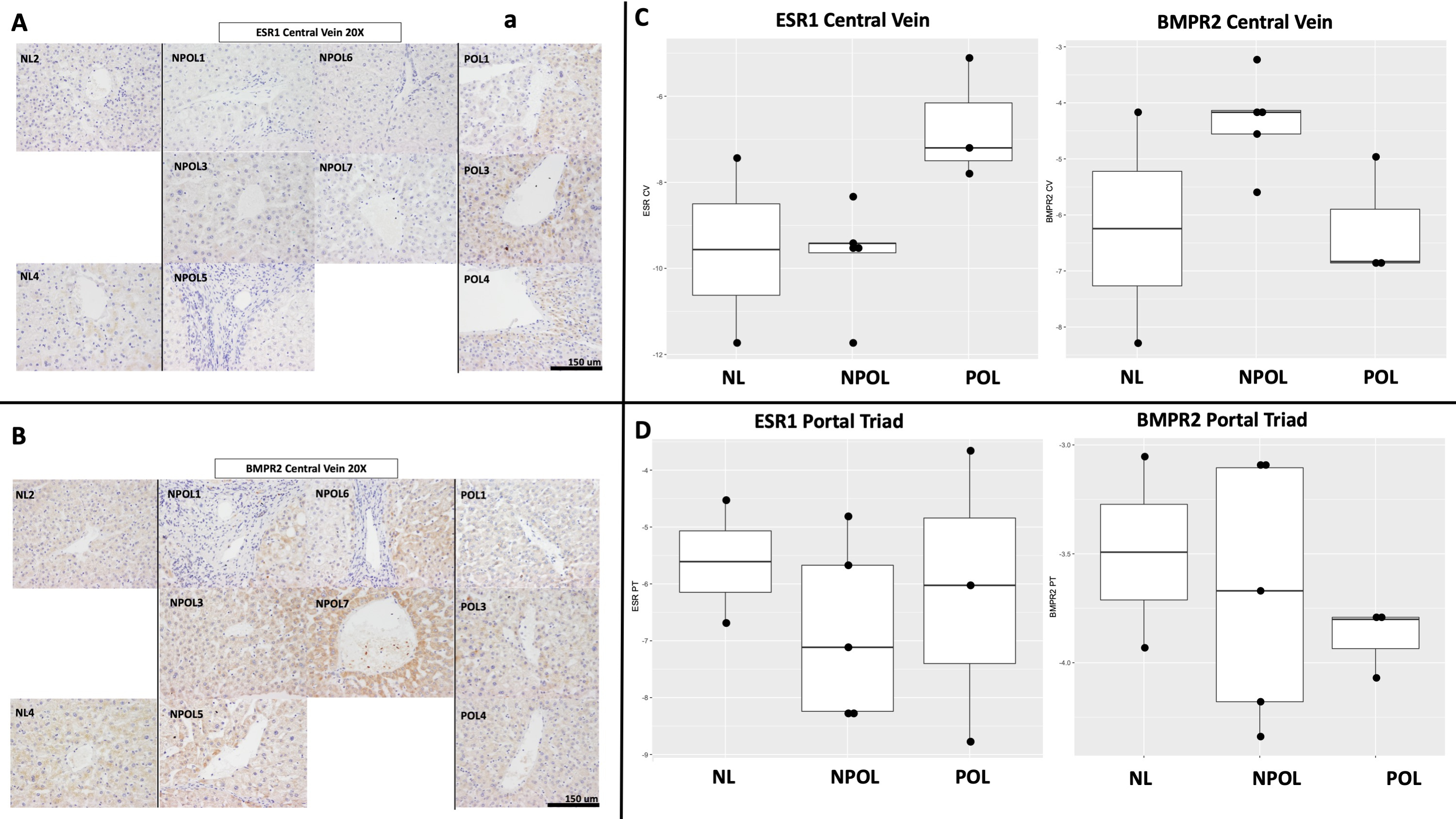
Increased protein expression of ESR1 (Panel A) and BMPR2 (Panel B) in PoPH relative to non-PoPH liver tissue, particularly in the region surrounding the central hepatic vein. This pattern corresponds with semi-quantitative immunohistochemistry increased for ESR1 and decreased for BMPR2 in PoPH versus non-PoPH cirrhosis liver tissue in the peri-central region (Panel C), a pattern not seen in the region of the liver surrounding the portal triad (Panel D).
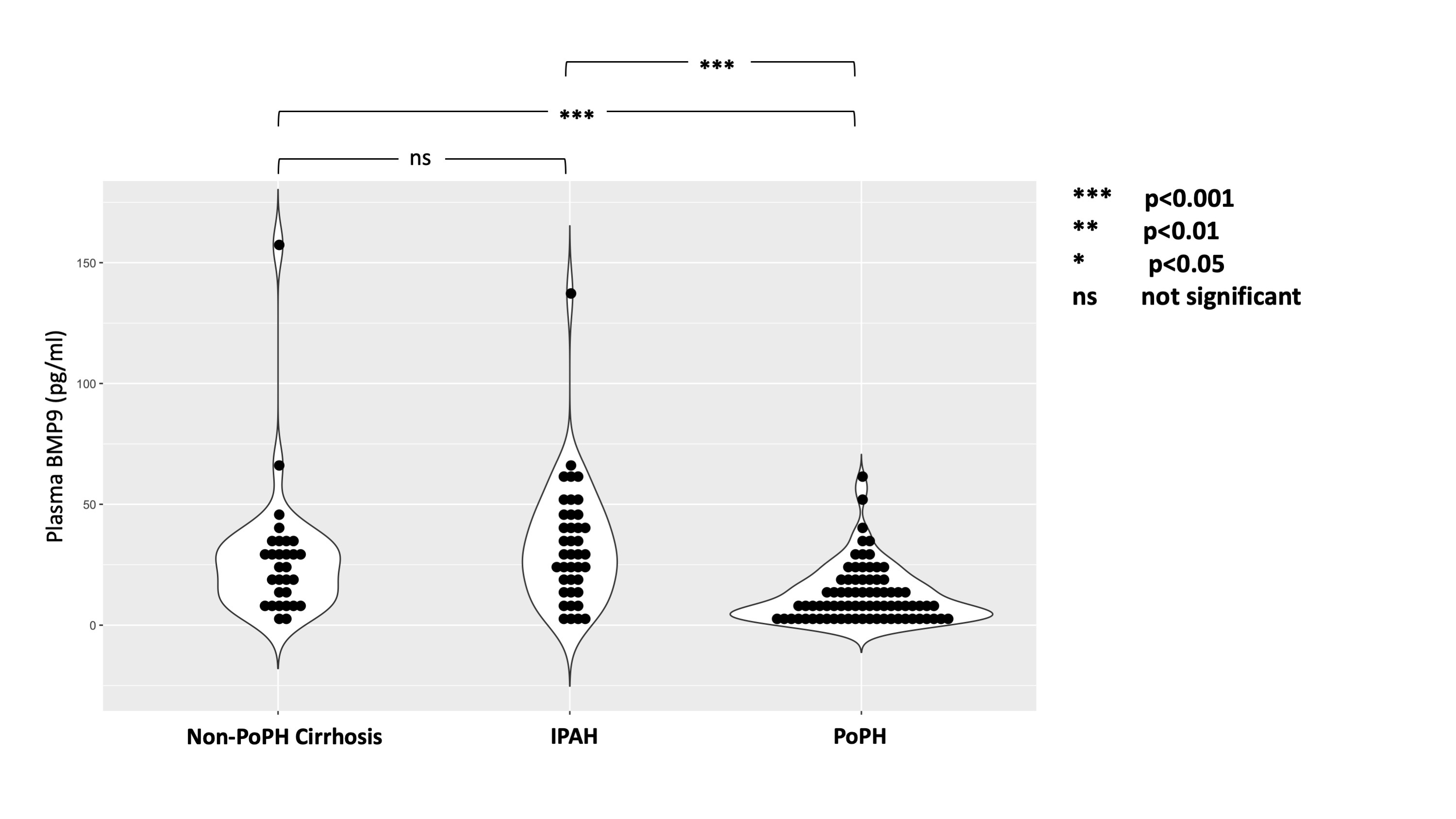
Circulating biomarker analyses from two large, independent cohorts of PoPH and non-PoPH cirrhosis subjects indicated that plasma levels of bone morphogenic protein type 9 (BMP9) were significantly lower in PoPH as compared to non-PoPH cirrhosis.
This work represents the first look into the unique transcriptional characteristics present in the PoPH liver as compared to the non-PoPH cirrhosis liver. First and foremost, our results provide a rich resource that we hope future investigators will build upon when investigating the “liver-lung” axis of disease that drives pulmonary vascular disease due to liver disease. Regarding the liver-lung axis, this work generates as many questions as it answers: Are these mechanisms (diminished circulating BMP9, increased signaling of GDF15, enriched arginine biosynthesis, differential expression of BMPR2 and ESR1 in liver cells surrounding the central hepatic vein, a pro-inflammatory cytokine environment) part of the liver-lung axis of disease? Do they operate through circulating mediators enhance proliferative arteriopathy and remodeling at the level of the pulmonary vasculature? Is there cross-talk, or is this a unidirectional flow of biological information?
To answer these questions, the focus of our current work, we plan to examine the biological and transcriptional characteristics of pulmonary vascular cells, construct a liver-lung interactome of cellular communication, and validate candidate circulating PoPH pathogenic factors in a large, well-phenotyped biorepository. These are not easy steps to take, and there is good reason the liver-lung axis of disease in PoPH has remained mostly undefined for the past 70 years, but our hope is that this work will enhance screening and diagnosis in chronic liver disease, accelerate the development of novel therapeutics, and improve clinical outcomes in this high-risk population.
Follow the Topic
-
Communications Biology
An open access journal from Nature Portfolio publishing high-quality research, reviews and commentary in all areas of the biological sciences, representing significant advances and bringing new biological insight to a specialized area of research.
Related Collections
With Collections, you can get published faster and increase your visibility.
Mechanistic insights into human host and microbiome interactions
Publishing Model: Open Access
Deadline: May 31, 2026
Advances in neurodegenerative diseases
Publishing Model: Hybrid
Deadline: Jun 30, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in