Understanding the knowledge gap in dental stem cell therapy
Published in Bioengineering & Biotechnology, Biomedical Research, and General & Internal Medicine

Dental stem cell therapy is often discussed as a potential direction in regenerative dentistry. Yet for me, this study was never only about stem cells, education, or professional attitudes. It was also about a practical question: how prepared are practicing dentists to understand, evaluate, and potentially adopt emerging regenerative approaches in real clinical settings?
This question became the starting point for our recently published article in BMC Medical Education. As a dentist and researcher working in regenerative dentistry and dental stem cells, I was interested not only in the scientific promise of dental stem cell therapy, but also in the educational gap that may shape how such therapies are understood by practicing clinicians.
In contexts where access to specialized training, institutional support, and regulatory guidance may be limited, understanding professional knowledge gaps becomes especially important. Scientific progress alone is not enough if clinicians do not have the educational tools needed to interpret and apply emerging therapies responsibly.
The study focused on Palestinian dentists and explored their knowledge, attitudes, perceived barriers, and willingness to adopt dental stem cell therapy. Using a cross-sectional, web-based survey, we assessed factual knowledge, adoption attitudes, ethical concerns, perceived obstacles, and interest in future education and training.
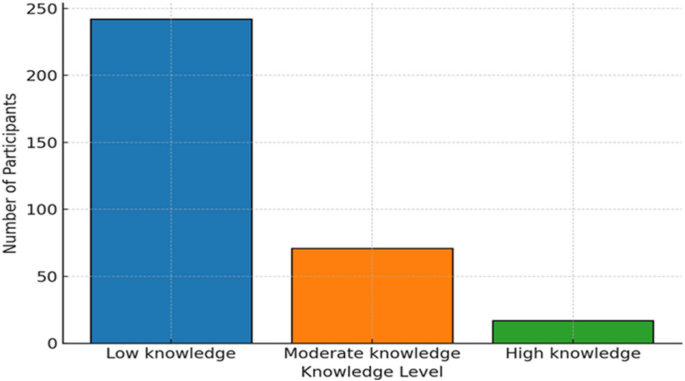
One of the clearest findings was that knowledge remained limited among many respondents, even though willingness to adopt dental stem cell therapy was relatively high. This contrast felt important to us. It suggested that there is genuine interest and openness toward innovation, but interest alone is not enough for safe and responsible implementation. Clinicians also need structured education, clear professional guidance, and access to evidence-based training.
The most commonly reported barrier was lack of knowledge, followed by cost and ethical concerns. These findings suggest that the challenge is not only scientific or technical. It is also educational, regulatory, and practical. For dental stem cell therapy to move responsibly toward clinical contexts, dentists need more than awareness; they need a clear understanding of indications, limitations, safety considerations, regulatory boundaries, and ethical responsibilities.
At the same time, we were careful not to overinterpret the findings. This was a cross-sectional survey, not a measure of clinical competence or actual adoption behavior. Recruitment was conducted through closed professional online groups, which may have reached dentists who were more digitally connected or more education-oriented. Therefore, the results should be interpreted as a context-specific snapshot of knowledge, attitudes, and perceived barriers among the surveyed Palestinian dentists, rather than as a definitive national assessment.
For me, the value of this work lies in highlighting a practical gap between scientific progress and professional readiness. Dental stem cell therapy may hold promise, but responsible translation requires education before implementation. Undergraduate curricula, continuing education programs, and clearer regulatory guidance may all play important roles in preparing dentists to engage with regenerative therapies in a safe and evidence-informed way.
I hope this study contributes to discussions around dental education, regenerative dentistry, and the responsible adoption of emerging therapies, especially in settings where access to specialized training and regulatory guidance may still be limited. Identifying educational gaps is not a small matter; it is one step toward supporting future healthcare education and preparedness.
Published article:
Zahedah R, Jaber M, Dinç B. Exploring the knowledge gap in dental stem cell therapy: educational challenges and adoption attitudes among Palestinian dentists. BMC Medical Education. 2026;26:535. https://doi.org/10.1186/s12909-026-08880-x
Follow the Topic
-
BMC Medical Education
This is an open access journal publishing original peer-reviewed research articles in relation to the education and training of healthcare professionals. It welcomes studies on students and professionals across all levels of education; education delivery aspects; and other education-related topics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Transnational medical education programs
BMC Medical Education is calling for submissions to our Collection on Transnational medical education programs. As medical education expands beyond national boundaries, new opportunities and challenges are emerging in how curricula are delivered, quality is assured, and learners are supported across diverse cultural and institutional contexts. These cross-border educational partnerships are reshaping the way we define standards, prepare future health professionals, and foster global health equity.
This Collection invites research that critically examines the structure, outcomes, and implications of educational initiatives that operate across borders. Whether through institutional partnerships, dual-degree programs, offshore campuses, or digital learning platforms serving international student populations, transnational initiatives demand thoughtful attention to pedagogical alignment, accreditation, faculty development, and learner experience. We welcome insights that address the complexity of delivering medical education in settings where geographic, regulatory, and cultural contexts differ.
We encourage submissions on topics such as:
• Curriculum design and adaptation across cultural and regulatory contexts
• Accreditation and quality assurance in cross-border medical education
• Faculty development and support in international teaching environments
• Student experiences, identity formation, and transitions between institutions
• Governance models and institutional partnerships in global medical education
• Ethical considerations and power dynamics in transnational collaborations
• Role of digital platforms and technology-enhanced education in delivering cross-border education
This Collection aims to showcase diverse voices and evidence-based approaches that inform the development and sustainability of cross-national medical education programs. By fostering open dialogue and rigorous inquiry, we seek to support inclusive, high-quality education that prepares graduates to meet health needs across a global landscape.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being, SDG 4: Quality Education, and SDG 17: Partnerships for the Goals.
Publishing Model: Open Access
Deadline: Jun 23, 2026
Lifelong learning and patient safety
BMC Medical Education is calling for submissions to our Collection, Lifelong learning and patient safety. As healthcare delivery becomes increasingly complex, shaped by biomedical advances, digital transformation, demographic shifts, and changing patient expectations, so does the potential for errors and adverse events. This phenomenon makes it essential to equip all healthcare professionals with training and tools to prioritize patient safety across different clinical environments.
Patient safety is a global health priority, with the World Health Organization identifying unsafe care as one of the leading causes of avoidable morbidity and mortality worldwide. While traditional models of competence, validated at a single point in time through licensure or certification, can be valuable, addressing this challenge requires a workforce that is continuously learning, adaptive, and equipped to respond to evolving patient safety threats. Lifelong learning in healthcare plays a pivotal role in fostering patient safety by making sure that healthcare professionals remain competent and adaptive to the best practices in the medical field. Outdated knowledge or skills in the medical field can directly jeopardize patient outcomes. Therefore, continuous professional development allows clinicians to update their professional competencies, reducing the risk of errors and adverse events.
This Collection invites research that examines how patient safety, which should be a professional expectation and ethical imperative at all stages of one’s career trajectory, can be enhanced through innovation in health professions education and training. Topics of interest include, but are not limited to:
• Tools and strategies for integrating patient safety into medical and nursing curricula
• Lifelong learning and continuing professional development (CPD) for patient safety and competence
• Simulation for teamwork, inclusion, and communication in diverse healthcare teams to enhance patient safety
• Interprofessional and collaborative safety culture
• Infection prevention and medication safety practices
• Learning from errors, near-misses, and real-time decision-making in clinical teams
• Strategies and policies for enhancing lifelong learning for patient safety
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-Being and SDG 4: Quality Education.
Publishing Model: Open Access
Deadline: Aug 18, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in