What are we learning from the UK's Meningitis B outbreak?
Published in Microbiology, General & Internal Medicine, and Public Health
Just over a week ago, a case of Meningitis B was confirmed at the University of Kent in the South East of England. Since then, a cluster of 29 infections have been identified amongst school and university students, with a University of Kent student and local sixth former sadly having died.
Concern amongst students, parents and the wider public has been palpable, but reassurance came on Monday with the news that the peak of the outbreak - believed to have stemmed from a Canterbury nightclub - looks to have passed.
How good is our understanding of Meningitis?
Clusters on this scale are rare, but individual cases of Meningitis B are not unusual in the UK, with around 400 reported per year.
Most people have heard of meningitis, know it can be serious or even fatal, and may even know someone who contracted meningitis as a baby or as a young adult. Beyond that, public understanding is pretty low.
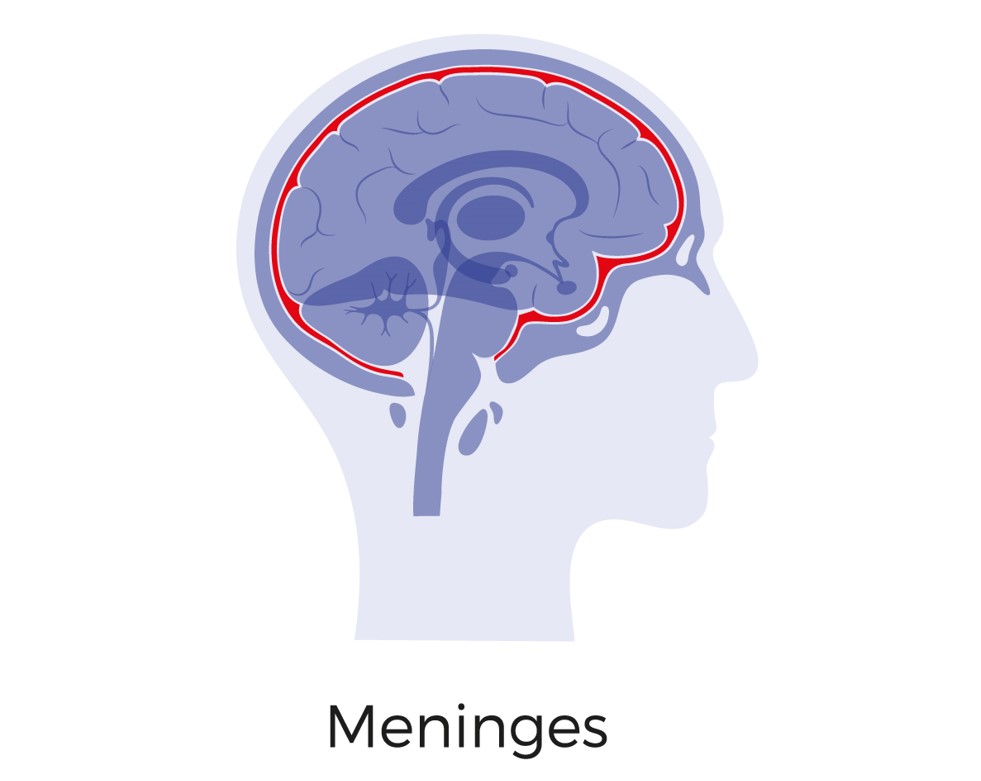
Meningitis is the inflammation of the meninges, protective layers that surround your brain and spinal cord. It can be caused by bacteria (as with the recent Meningococcal group B bacteria cases) or a virus.
Am I covered by a vaccine?
The past week has shown how confused so many of us are about whether we're vaccinated against meningitis.
In 1999, the Meningitis C vaccine was introduced for one year olds, tackling disease caused by Meningococcal group C bacteria. This led to UK cases of Meningitis C dropping from around 2500 per year to around 30-40 per year.
The vaccine programme expanded in 2015 to include the Meningitis ACWY booster for Year 9 students, covering three additional forms of bacterial meningitis. 'Catch up jabs' exist for people under the age of 25 who weren't previously vaccinated, so it's worth checking your record!
In the same year, the Meningitis B vaccine was introduced for newborn babies in the UK, the first country to roll this out. It's available privately for anyone too old to have been vaccinated as a baby, but isn't offered on the NHS if you weren't eligible as a baby.
Because vaccines were introduced at different times, and as a result of various waves of vaccine scepticism since the 1990s, we're a patchily-protected population. Unsurprisingly, lots of people are confused about what they received growing up.
How have the public reacted to a new disease outbreak?
Despite some confusion about what Meningitis is and who's protected from it, there's reassurance to be gained from the knowledge that it's a well-studied and relatively well-understood disease.
Naturally, there have been a lot of questions. Why are young people most affected? Are you at risk if you're not a student? Are immunosuppressed people more likely to contract it? How is it spread?
Overwhelmingly, the students most at risk of contracting and spreading disease have been willing to act fast to protect themselves and others around them, like James Thompson, who got up at 4am to receive his MenB vaccine on Friday.
As of Sunday, the Department of Health and Social Care reported more than 8,000 vaccinations and 12,000 courses of antibiotics have been provided to students and sixth formers in Canterbury, close contacts of patients, and anyone who had recently visited the nightclub where the cluster was believed to have originated.
While Kent expands emergency vaccine coverage to Year 11 pupils, other parts of the country have struggled balancing supply and demand. One pharmacy in York has only been able to get hold of four extra doses in the last week.
Meanwhile, routine vaccinations for babies and teenagers continue across the country as normal.
How does this compare to the Covid-19 pandemic response?
It's tempting to draw parallels between this outbreak and the early days of coronavirus in March 2020. For students and medical responders, having a pandemic so fresh in memory may even be helpful.
This time, the media response feels less frantic and more factual, but this is understandable when we have a better grasp of how a disease is spread (via much closer contact than covid), and an existing method for testing which means case numbers are a lot less speculative and misrepresented than we'd seen during the pandemic:

It's been a deeply worrying week for students, especially those whose friends, flatmates and coursemates have been hospitalised. Even with an infection as potentially serious as Meningitis - all confirmed cases from this outbreak have resulted in hospitalisation - there's reassurance to be found in the fact that the response to an outbreak of a known disease will always be faster than the response to an emerging one.
There's some deep-seated irony in the timing of the outbreak, in the middle of the release of the outcomes of the Covid inquiry, which examines the UK's governmental and societal response to Covid-19, and the burden the pandemic had on healthcare systems, patients and healthcare workers.
The main findings of the inquiry so far? The NHS "teetered on the brink of collapse" throughout, and only survived thanks to superhuman efforts of healthcare workers, while politicians were reluctant to recognise the severity of the situation. The problem with the Covid inquiry, Isabel Hardman points out in the Spectator, is that it isn’t able to examine the wider context for the strain on the healthcare system.
Even though this Meningitis outbreak hasn't pushed the system back to those same limits, it still feels optimistic to assume things have substantially improved since then.
What can we learn this time around, then?
Familiarity with a disease in name doesn't mean we could spot it in practice. While we haven't seen misinformation whip around at the speed it did during the Covid-19 pandemic, the last week has shown that so many people are unfamiliar with which diseases they're vaccinated against, and would struggle to spot a real case of Meningitis in themselves, friends or family.
The charity Meningitis Now do vital work raising awareness of the infection and encouraging vaccine uptake. They also encourage everyone to understand what symptoms can look like - the classic 'meningitis rash' doesn't appear for everyone.

Research never stops on established diseases like Meningitis, even once effective vaccines are in place. We've made the latest Springer Nature journal articles on Meningitis available together here.
New clinical trials focused on Meningitis are regularly made public through ISRCTN, the UK's clinical study registry. Previously, these have included investigating a new vaccine with fewer side effects, when to vaccinate premature babies, and whether vaccination reduces the percentage of teenagers who carry Meningitis B bacteria in their throats without symptoms.
We'll only know this cluster has been fully contained once the 10-day incubation window has passed for contacts of all patients. For now though, it looks like Canterbury is through the worst. In the meantime, perhaps today is the day to check your vaccine record and learn the symptoms of Meningitis.
Follow the Topic
-
ISRCTN: The UK’s Clinical Study Registry
A primary clinical trial registry recognised by WHO and ICMJE that accepts studies involving human subjects or populations with outcome measures assessing effects on human health and well-being, including studies in healthcare, social care, education, workplace safety and economic development.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in