Cost effectiveness of a novel SwaRSA Strategy to reduce acute exacerbations of COPD
Published in Neuroscience, Protocols & Methods, and General & Internal Medicine
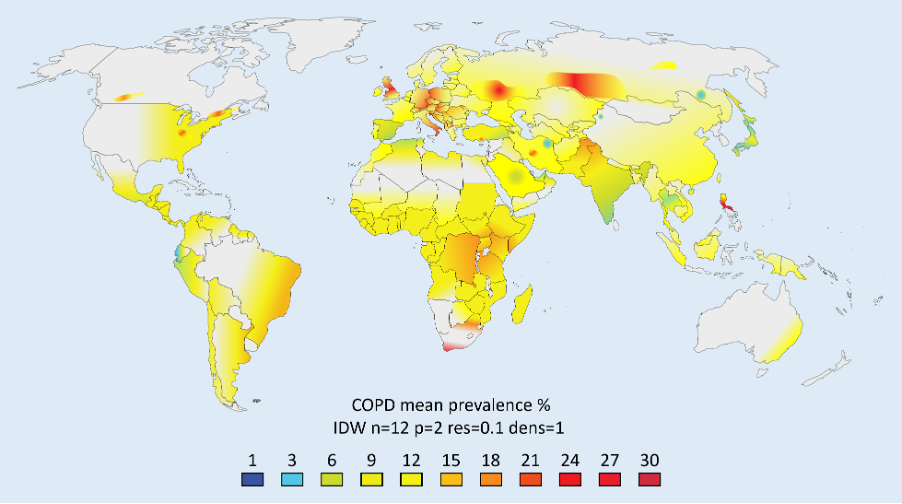
The paper discusses the significant economic burden of Chronic Obstructive Pulmonary Disease (COPD) and the potential cost savings from reducing COPD exacerbations. A decision analytic model that evaluates the cost-effectiveness of a Swallowing and Respiratory Sensation Assessment (SwaRSA) strategy, involving swallowing and respiratory sensation assessment tests and subsequent swallowing rehabilitation, is presented to reduce COPD exacerbations. The model suggests that self-assessment with the Eating Assessment Tool (EAT-10) and subsequent intervention is a highly cost-effective option compared to no-SwaRSA.
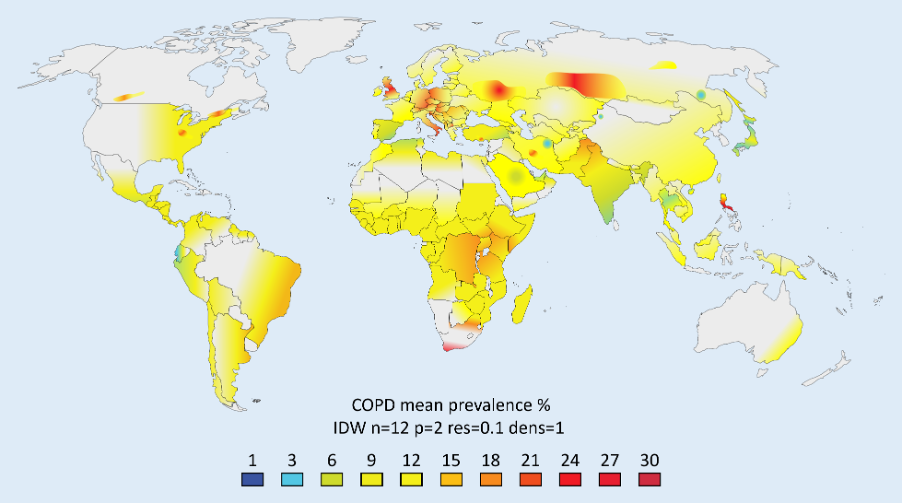
Key Points: Novel SwaRSA Decision Analytic Model; Epiu I. et al 2025 https://pubmed.ncbi.nlm.nih.gov/40200355/
Economic Burden of COPD
- COPD represents a considerable economic burden globally, with an estimated cost of US$ 2.1 trillion.
- Annual COPD costs in the USA are expected to increase to 40 billion USD per year.
- Australia spent about AUD$ 831.6 million in 2020-21 on the management of COPD, with over half of this cost for hospital care.
Potential for Cost Savings
- A significant portion of the COPD management cost could be avoided by reducing exacerbations.
Cost-Effectiveness of SwaRSA Strategy
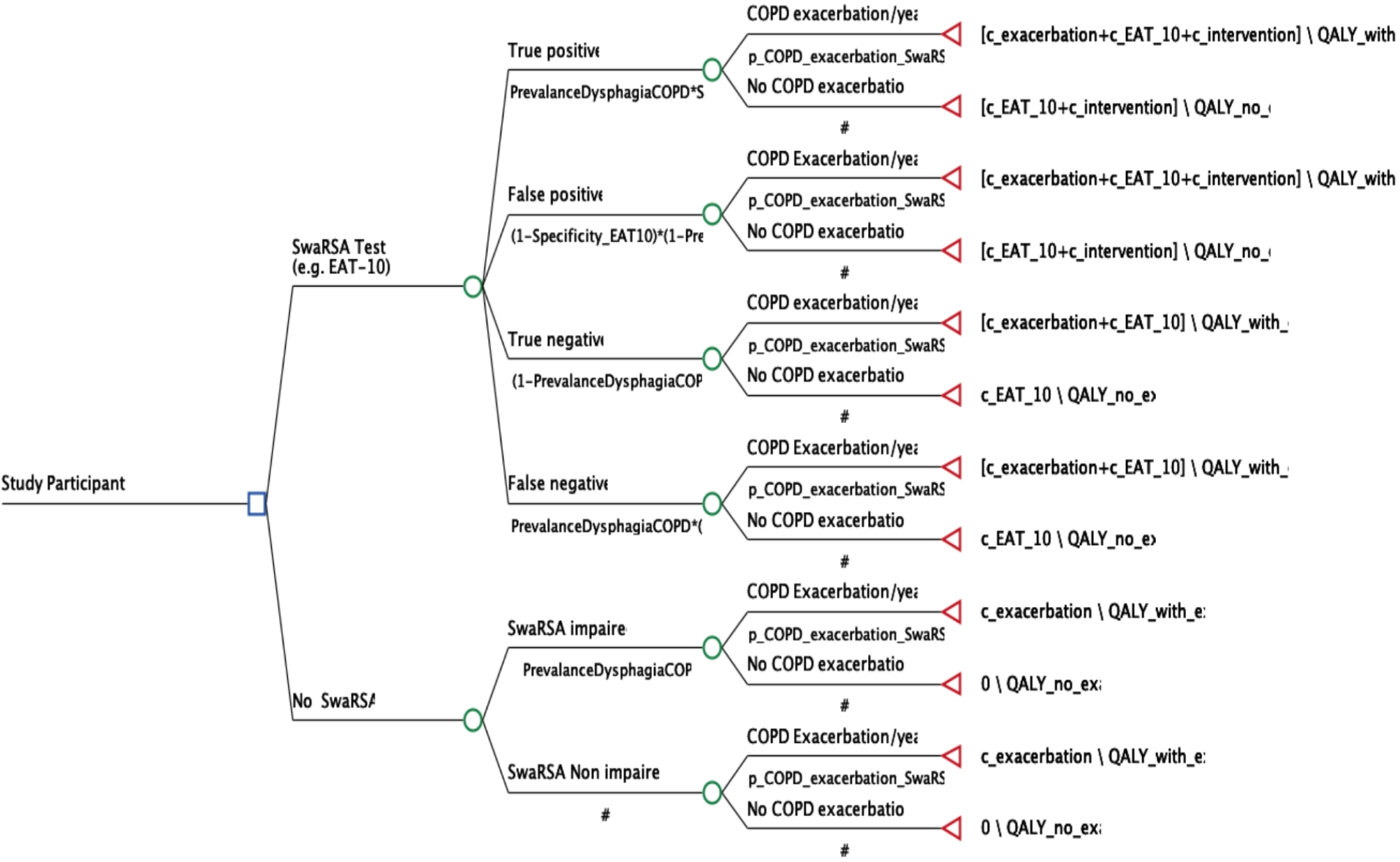
- The decision analytic model assessed the cost-effectiveness of a Swallowing and Respiratory Sensation Assessment (SwaRSA) strategy, which involved swallowing and respiratory sensation assessment tests and subsequent swallowing rehabilitation.
- Three individual testing strategies within the SwaRSA approach were found to be cost-effective, with incremental cost-effectiveness ratios per QALY ranging from $27,000 to $37,000 AUD.
- The EAT-10 and the tongue strength were the two dominant options on the cost-effectiveness frontier.
- The model results were robust to variations in one-way and probabilistic sensitivity analyses, and the self-assessment with the EAT-10 and subsequent intervention was highly cost-effective relative to no-SwaRSA.
Here are the key implications of the findings for healthcare policy regarding COPD management:
-
The high economic burden of COPD, estimated at over $2 trillion globally and $40 billion annually in the US, highlights the need for more effective and cost-efficient management strategies.
-
Novel finding that a significant portion of COPD costs could be avoided by reducing exacerbations suggests that interventions targeting exacerbation prevention should be a priority for policymakers.
-
The high prevalence of swallowing difficulties (dysphagia) among COPD patients, affecting up to 56% of hospitalized patients, suggests that screening and management of swallowing disorders should be integrated into standard COPD care.
-
This cost-effectiveness analysis of the SwaRSA strategy, which includes swallowing and respiratory sensation assessment tests followed by swallowing rehabilitation, provides strong evidence that such an approach can be a highly cost-effective way to reduce COPD exacerbations and associated costs.
-
Further research may be needed to validate these findings in different healthcare settings and populations, but the current evidence suggests that integrating swallowing assessment and rehabilitation into COPD management should be a priority for healthcare policy
Follow the Topic
-
BMC Pulmonary Medicine
This journal is an open access, peer-reviewed journal that considers articles on all aspects of the prevention, diagnosis and management of pulmonary and associated disorders, as well as related molecular genetics, pathophysiology, and epidemiology.
🔍 Ask the Editor – Clinical medicine, Respiratory physiology, and Cardiology
I’m excited to connect with a global network of specialists through the Research Communities – how will you get involved?
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Social and economic factors in pulmonary disease and disorders
BMC Pulmonary Medicine is calling for submissions to our Collection on social and economic factors in pulmonary disease and disorders. Pulmonary diseases and disorders are increasingly recognized as not only medical conditions but also as complex issues deeply intertwined with social and economic factors. Conditions such as asthma, chronic obstructive pulmonary disease (COPD), and lung cancer disproportionately affect specific demographics, particularly those in low-income communities and vulnerable populations. Infectious diseases affecting the lungs are also a challenge for those living in cramped or overcrowded areas. This Collection aims to illuminate how socioeconomic status, environmental exposures, and other social determinants impact the prevalence, management, and outcomes of pulmonary diseases, fostering a more holistic understanding of these conditions.
Addressing the intersection of pulmonary diseases and socioeconomic factors is crucial for developing effective public health interventions and policies. Recent advancements in research have highlighted the critical role that exposure to environmental pollution, access to healthcare, and health literacy play in exacerbating lung disorders in marginalized groups. By identifying and understanding these interrelations, researchers and healthcare professionals can better advocate for equity in healthcare access and improve treatment outcomes for affected populations. With a focus on social determinants, there is potential to develop tailored interventions that not only target the diseases themselves but also the underlying social and economic factors that contribute to their prevalence. We invite submissions on a range of topics that include, but are not limited to:
- Social determinants of pulmonary health
- Biological mechanisms linking social factors and environmental exposure to lung disease
- Longitudinal or causal approaches to associating social factors and environmental exposure to lung disease
- Impact of environmental pollution on lung disease
- Pulmonary diseases and disorders in low-income communities
- Lines of work in resource-limited settings that contribute to pulmonary disease
- Health disparities in refugee and migrant populations
- Socioeconomic factors influencing treatment adherence
- Diagnosis and treatment options in resource-limited settings
This Collection supports and amplifies research related to SDG 1: No Poverty, SDG 3: Good Health and Well-being, SDG 8: Decent Work and Economic Growth, and SDG 11: Sustainable Cities and Communities.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Feb 10, 2027



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in