Expanding the Spectrum of Autoimmune Encephalitis — A Rare Anti-Recoverin Case
Published in Neuroscience and Biomedical Research
Clinical Presentation and Diagnostic Features
The report describes a 33-year-old woman presenting with a subacute syndrome characterized by temporal lobe seizures, progressive cognitive dysfunction, and insomnia. Neuroimaging demonstrated bilateral hippocampal and thalamic signal abnormalities, while EEG confirmed bilateral temporal epileptiform activity.
Importantly, both serum and cerebrospinal fluid were strongly positive for anti-recoverin antibodies—classically associated with cancer-associated retinopathy but rarely implicated in central nervous system autoimmunity.
After excluding malignancy and alternative etiologies, the patient fulfilled criteria for definite autoimmune limbic encephalitis
Therapeutic Course and Outcome
The patient was treated with high-dose corticosteroids and intravenous immunoglobulin, alongside antiseizure therapy. Over a two-year follow-up period, she demonstrated sustained clinical and radiologic improvement, with partial persistence of antibody titers.
Broader Implications
This case offers several important contributions to the literature:
- It expands the phenotypic spectrum of anti-recoverin–associated disease beyond retinopathy
- It reinforces the need to consider intracellular neuronal antibodies in atypical or seronegative AE presentations
- It highlights the potential reversibility of rare autoimmune syndromes with timely immunotherapy
- It underscores the enduring value of carefully documented case reports in identifying novel or underrecognized disease associations
Knowledge Check
Which statement best reflects the clinical significance of anti-recoverin antibodies in this context?
A. They are exclusively associated with retinal disease
B. They are common markers of anti-NMDA receptor encephalitis
C. They may rarely be associated with autoimmune encephalitis, even in the absence of malignancy
D. They are surface antibodies directly targeting synaptic receptors
Correct answer: C
Closing Perspective
As the landscape of autoimmune neurology continues to expand, recognition of rare antibody-mediated syndromes remains essential. This case exemplifies how individual observations—carefully reported—can meaningfully shape clinical understanding and patient care.
Journal of Medical Case Reports is the world’s first international, PubMed-listed, medical journal devoted to publishing case reports from all medical disciplines and will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports.
Follow the Topic
-
Journal of Medical Case Reports
This journal will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement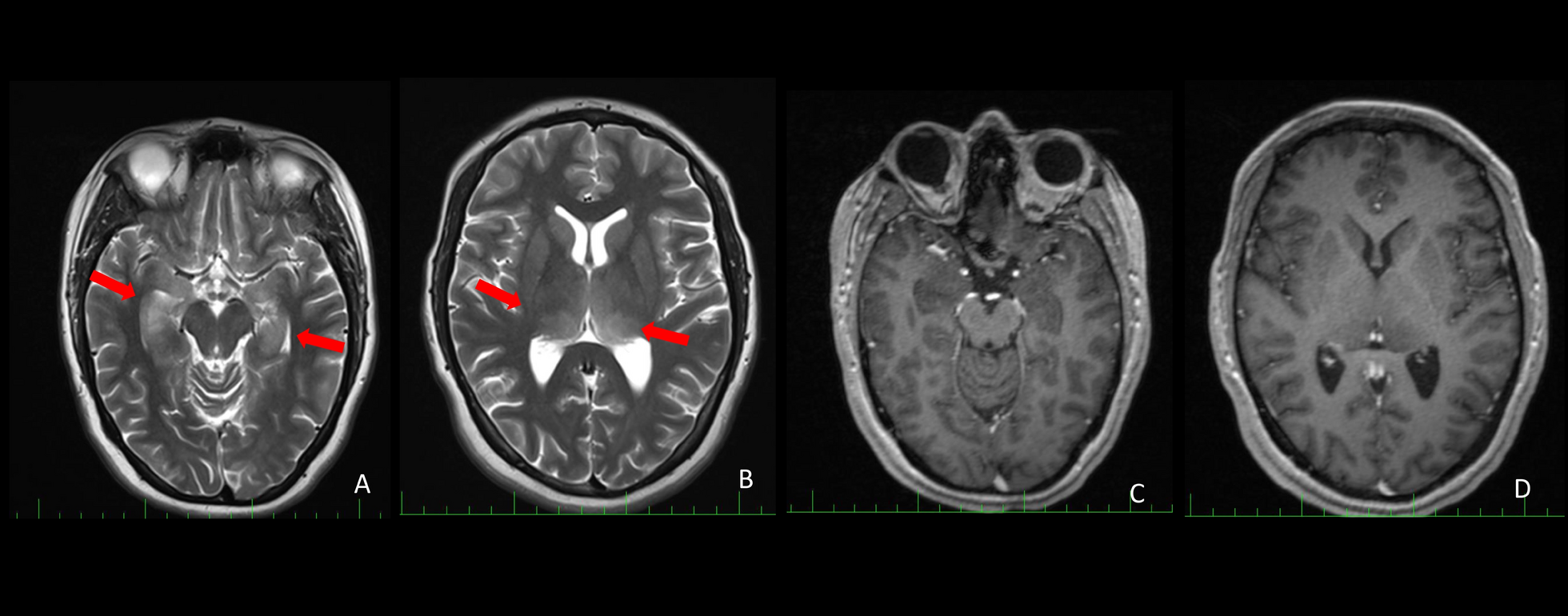



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in