From Silence to Hope: How Women in Cameroon Rebuild Their Lives After Obstetric Fistula
Published in Biomedical Research and Behavioural Sciences & Psychology
In many communities, childbirth is expected to bring joy. But for some women, it becomes the start of long years of suffering. One of the most devastating childbirth injuries is obstetric fistula a condition that few people talk about, yet thousands of women live with every day.
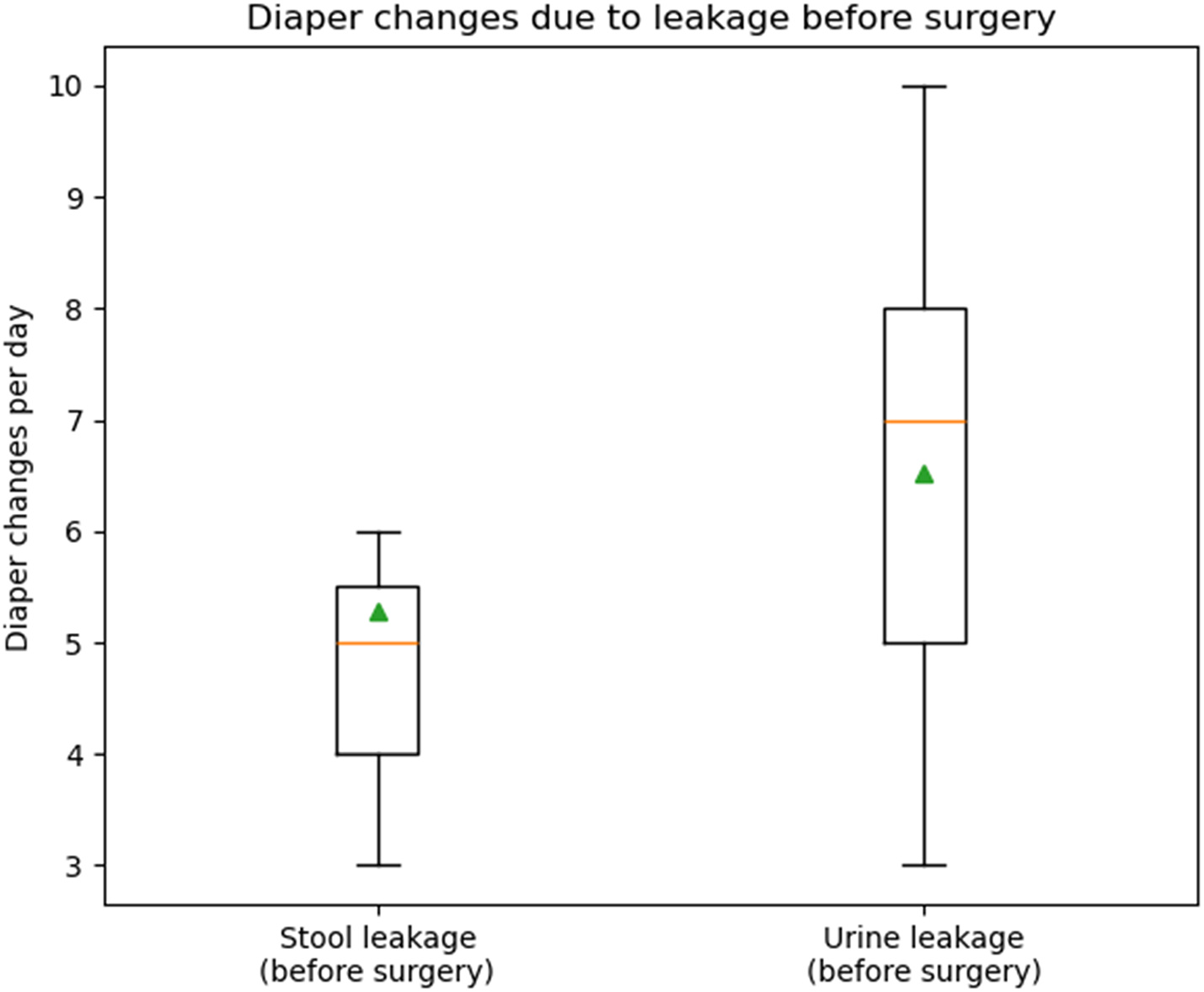
Obstetric fistula happens when a woman experiences prolonged and difficult labor without timely medical care. During this long labor, pressure from the baby blocks blood flow to tissues between the birth canal and the bladder or rectum. The damaged tissue then forms a hole, causing continuous leakage of urine or stool. Many women also lose their babies during such deliveries.
After this injury, life changes in painful ways. The constant leakage produces odor, infections, and skin sores. But even worse is the emotional and social suffering that follows. Women often feel ashamed and begin to isolate themselves. Some husbands leave them. Neighbors avoid them. Many women stop attending church, markets, or social events because they fear being mocked or rejected.
One woman described her experience simply: she stayed indoors most of the time because she feared people would laugh at her. Another explained that customers stopped coming to her small food business once people discovered her condition. Many women lost their ability to earn money and became dependent on relatives who were already struggling financially.
Yet behind these painful experiences lies a story of recovery and resilience.
In Northwest Cameroon, specialized programs now identify women living with fistula and bring them to hospitals where surgery can repair the injury. Mbingo Baptist Hospital is one such center where women receive treatment and follow-up care. Surgery often brings immediate relief. Women who have lived for years with constant leakage suddenly wake up dry after the operation.
For many, this moment feels like being given a new life.
Several women described how they could sleep peacefully again without fear of wetting the bed. Others spoke of walking freely or attending church without embarrassment. One woman joyfully expressed that she could now jump and dance again. Another said she felt like a human being again after years of humiliation.
However, healing is not always perfect or immediate. Some women continue to experience minor leakage or discomfort months after surgery. Recovery also requires emotional support because many women carry deep psychological scars from years of isolation.
Health workers play an important role beyond performing surgery. Women repeatedly mentioned how respectful and compassionate treatment from nurses and doctors helped restore their confidence. Being treated with dignity even when they felt ashamed or smelled of urine helped them feel valued again.
But the journey does not end at the hospital. Returning home brings new challenges.
Some families welcome women warmly and support their recovery. Mothers, siblings, and sometimes husbands accompany them to hospital visits and help them reintegrate into community life. Such support gives women strength and motivation.
Sadly, not all women experience this acceptance. Many participants in the study reported that their husbands or in-laws abandoned them when they developed fistula. Some were blamed for bringing bad luck to the family. Even after successful surgery, stigma sometimes persists in certain communities. People may still remember their past condition and continue to avoid them.
At the same time, there are encouraging stories of community solidarity. Churches, women’s groups, and neighbors sometimes come together to help women seek treatment. Communities have donated blood, raised money, and provided emotional support. When communities understand that fistula is a medical condition and not a curse, acceptance improves.
Another critical part of recovery is economic independence. Before surgery, many women lost their livelihoods because of their condition. Farmers could no longer work in fields. Traders lost customers. Small businesses collapsed. Poverty worsened just when women needed money most.
To address this, recovery programs now include livelihood support. Women receive training in tailoring, hairdressing, poultry farming, farming, or small-scale trading. Some receive start-up materials or financial support to restart businesses. Others receive assistance to return to school.
This economic empowerment transforms lives.
Women begin earning income again and supporting their families. Confidence returns. Respect within communities grows. One participant proudly shared that people now complain when her shop is closed because they miss her services. Another woman explained that her small earnings help feed her family and restore her sense of importance.
Economic recovery also changes family relationships. Some husbands who once abandoned their wives try to reconnect after seeing their success. More importantly, women themselves gain independence and self-worth.
Something even more powerful happens for some survivors: they become leaders and advocates. Women who once hid in shame now speak publicly about fistula. They encourage others to seek treatment early and help reduce stigma in their communities.
One participant shared that she now holds a leadership role in a community organization and people listen to her opinions. Others educate women in meetings about childbirth risks and available treatment. These survivors move from being victims to becoming agents of change.
Their stories teach an important lesson: repairing obstetric fistula requires more than surgery. Women need emotional support, community acceptance, and economic opportunities to fully rebuild their lives. Recovery happens step by step restoring health, healing emotional wounds, regaining social acceptance, and rebuilding livelihoods.
The experiences of these women show that even after years of suffering, hope and healing are possible. With proper care and community support, women do not just return to normal life; many become stronger and more determined than before.
Their journeys remind us that medicine can repair the body, but compassion, dignity, and opportunity help restore the whole person.
https://link.springer.com/article/10.1007/s44337-026-00570-3
Follow the Topic
-
Discover Medicine

This is a fully open access, peer-reviewed journal that supports multidisciplinary research and policy developments across the fields of medical and clinical science.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Gut Microbiome and Human Well Being
The human gut microbiome plays a critical role in maintaining health and modulating disease processes. Its composition evolves across the lifespan under the influence of diet, lifestyle, aging, and environmental exposures. Disruption of gut microbial balance—known as dysbiosis—has been implicated in the pathogenesis of various chronic conditions, including autoimmune, metabolic, neurological, and inflammatory diseases.
This Collection welcomes submissions that explore the mechanistic, clinical, and translational aspects of gut microbiota in human health, with particular interest in:
The gut–brain, gut–heart, gut–cancer, and gut–joint axes
Gut dysbiosis and its immunological and metabolic consequences
Microbial metabolites and host-microbiome interactions
Microbiome-based diagnostics, therapeutic interventions, and biomarkers
We invite contributions including but not limited to:
Original research articles based on clinical, in vivo or in vitro studies
Reviews summarizing recent advances or proposing new frameworks
Perspective or opinion pieces that highlight emerging concepts or challenges
This Collection aims to enhance our understanding of the gut microbiome's contribution to health and disease and to inspire microbiome-based strategies for improving human well-being.
Keywords: Gut microbiome; Gut-organ-axis; chronic diseases; 16S rRNA; metagenomics
Publishing Model: Open Access
Deadline: Jul 01, 2026
Innovative Laboratory and Epidemiological Strategies to Reduce Mortality of Non-Communicable Chronic Diseases
Non-communicable chronic diseases (NCDs) and related conditions remain the leading causes of morbidity and mortality worldwide. These include two major categories: non-communicable chronic diseases—such as cardiovascular diseases, chronic respiratory diseases, and diabetes mellitus—and external causes, including accidents and violence. In parallel, advances in laboratory sciences and the growing field of precision medicine have opened new possibilities for early diagnosis, risk stratification, and personalized management. These approaches aim not only to identify individuals at greater risk of developing NCDs, but also to monitor disease progression and the emergence of complications or comorbidities. In this context, innovative laboratory methods and novel biomarkers are urgently needed to enhance disease detection and surveillance strategies. We therefore invite researchers to submit original articles, reviews, and case studies addressing the role of precision medicine in improving the surveillance and clinical management of chronic non-communicable diseases and their progression.
Keywords: Non-communicable chronic diseases; disease aggravation; biomarkers; laboratory methods; epidemiological aspects; individual risk classification; precision medicine; health promotion; surveillance; innovative laboratory approaches.
Publishing Model: Open Access
Deadline: Mar 23, 2026
Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in