From Urban Planning to Respiratory Health: Why Weighting Risk Factors Matters 🏙️➡️🫁⚖️
Published in Earth & Environment, Plant Science, and Public Health

Whenever I attended conferences and academic seminars, public health impacts were explained differently each time through urban, environmental, or socioeconomic dimensions. Each discipline offered its own lens, its own framework.
But one question kept returning: 🔁❓
If respiratory diseases are the result of multiple interacting configurations urban, environmental, and socioeconomic how much weight should be assigned to each ? And why do we still struggle to translate scientific evidence into clear territorial priorities ? ⚖️📊
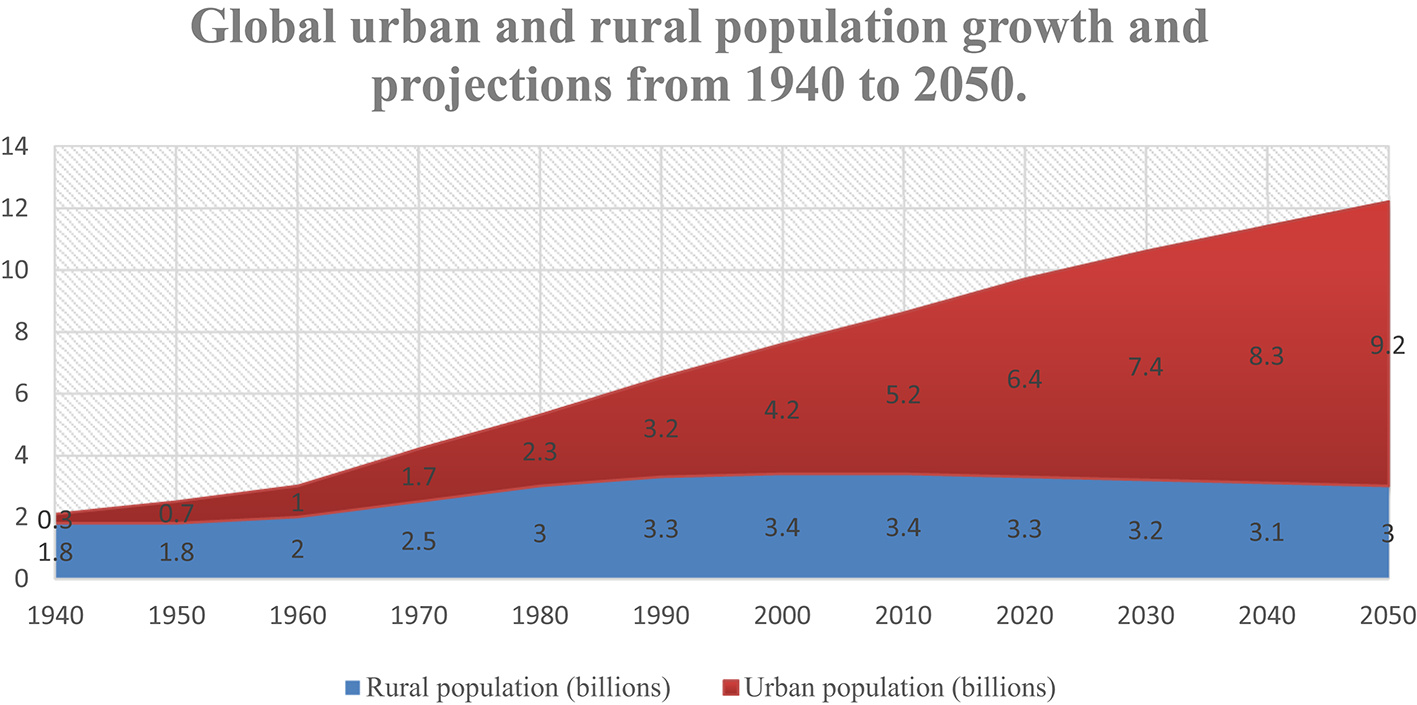
Cities are expanding rapidly. Pollution levels are rising. Climate change is reshaping exposure patterns. Social inequalities are deepening. And respiratory diseases from asthma and COPD to tuberculosis and COVID-19 continue to affect millions of people worldwide. We already know many individual risk factors: air pollution, housing overcrowding, traffic-related emissions, heat waves, lack of green spaces. The literature is abundant.
Yet something was missing.
What was lacking was a structured and transparent method to prioritize these factors to assign weight to each dimension and to validate findings through quantitative and econometric analysis, both for academic researchers and, especially, for policymakers who must decide where to intervene first.
It was precisely this gap that inspired the research titled “Environmental Urban and Socioeconomic Risk Factors for Respiratory Diseases: A Systematic Review with Quantitative Weighting Analysis.”
The Challenge of Fragmented Knowledge 🧩
We produce studies.
We accumulate data.
We publish analyses.
The literature in urban health is vast. Air pollution. Housing. Urban heat. Social inequalities. Daily mobility.
Each study adds a piece to the puzzle.
But the city is not a static puzzle.
It breathes. It moves. It amplifies.
Pollution circulates according to urban morphology.
Climate change alters the dispersion of particles and intensifies heat waves.
Social inequalities determine who lives near congested highways and who benefits from tree-lined parks.
Transport infrastructures shape, every single day, the air our lungs absorb.
Everything is interconnected.
And yet, our scientific syntheses remain fragmented. They isolate determinants as if the city could be understood by slicing it into separate compartments.
It was this fragmentation that deeply challenged me.
How Urban Form and Mobility Patterns Shape Respiratory Health Risks 🏙️🚦
This research demonstrates that urban form and mobility patterns are key determinants of population exposure to air pollution and heat-related health risks, directly influencing respiratory health outcomes.
Based on a systematic review of 43 studies published between 2014 and 2024, the analysis identified 211 occurrences of risk factors associated with respiratory diseases in urban settings. The study applied a rigorous, multi-layered methodological framework combining PRISMA-based literature selection, structured data extraction, Natural Language Processing (NLP), multi-criteria weighting, statistical normalization, and validation through ANOVA and OLS models.
By integrating environmental, urban, and socioeconomic dimensions, the research provides a structured and reproducible approach to understanding urban health dynamics.
A key finding is that specific urban configurations can either exacerbate or mitigate respiratory risks. In other words, city design is not neutral: spatial organization and mobility systems directly shape exposure patterns and vulnerability.
The study ultimately highlights that urban planning is not only an infrastructural discipline but a fundamental component of public health strategy.
Breathing is a territorial act. 🌍🫁
This study does not claim to establish definitive causal relationships. Instead, it offers a framework for thinking differently.
To think of the city as an active determinant of health.
To see prioritization as a strategic tool.
To understand research as a bridge between disciplines.
Health is not built solely in hospitals.
It is built in neighborhood density.
In air quality.
In planning decisions.
In public policies.
Breathing is a biological act.
But breathing is also a territorial act.
And if we want healthier cities, we must accept a simple truth:
📐What we plan today will determine who breathes freely tomorrow. 🌍🌱
Follow the Topic
-
Discover Public Health

This is an open access journal publishing research from all fields relevant to public health.
Related Collections
With Collections, you can get published faster and increase your visibility.
Antimicrobial Resistance: The New Challenge to Global Health in a Post-Pandemic World
Antimicrobial resistance (AMR) is a seriously ongoing threat to global health, occurring when bacteria, fungi, viruses, and parasites evolve to resist the drugs designed to kill or block them. The COVID-19 pandemic has both directly and indirectly exacerbated the problem of AMR, as the overuse of antibiotics has accelerated the development of resistance in many pathogens. COVID-19 may have subsided, but AMR continues to pose a significant risk to the effectiveness of global healthcare systems, threatening to reverse decades of progress in combating infectious diseases. The interplay between population health and AMR has become increasingly critical as healthcare practices have shifted in response to the pandemic. Understanding this relationship is essential for developing effective strategies to mitigate the impact of AMR on population health in a post-COVID context.
The motivation for launching this Collection arises from the urgent need to address the rising tide of AMR as healthcare systems grapple with the long-term effects of the pandemic. Increased antibiotic use during COVID-19 treatment, changes in healthcare access, and disruptions in public health interventions have all contributed to an environment where AMR can thrive. Moreover, the pandemic has highlighted the importance of a multidisciplinary approach to tackling AMR, involving epidemiology, policymaking, and community health initiatives. This Collection aims to provide a platform for researchers and practitioners to share insights and findings that can inform future strategies to combat AMR while considering the broader implications for population health.
This Collection aims to highlight the multifaceted nature of AMR in a post-pandemic environment. We solicit articles that investigate the particular issues provided by the pandemic in terms of AMR development and containment, examine the impact of AMR on many sectors of healthcare, and propose novel strategies to minimize resistance propagation. Submissions may include original research, policy assessments, program evaluations, and comments on the following major areas:
• Epidemiology and trends of AMR post-pandemic
• Impact of COVID-19 on antibiotic usage
• Surveillance strategies for AMR
• AMR and stewardship
• Prevention and control measures to limit AMR spread
• Policies and programs to promote antibiotic stewardship
• Economic and social implications of AMR
• Global collaboration and initiatives to tackle AMR
By addressing these critical issues, this Collection aims to provide a comprehensive understanding of the emerging challenges in antimicrobial resistance in a post-pandemic world and to promote effective strategies to preserve the power of our current antimicrobials.
Keywords: antimicrobial resistance; COVID-19; antibiotics; global health; infectious diseases; public health; policy; prevention
This Collection supports and amplifies research related to SDG 3.
Publishing Model: Open Access
Deadline: Jun 30, 2026
From Public Health Policy to Community Practice: Navigating Systemic Challenges in the Health System
Health is shaped by a wide range of interconnected factors, making it a complex and adaptive state that emerges from the interplay of biological, social, emotional, and meaning-making (semiotic) dimensions. As such, improving public health cannot be accomplished through isolated interventions targeting single structural issues or individual diseases. However, medicine and public health research and policies are too often considered through a reductionist, positivist and normative perspective, as epitomised by the influential “disease control” paradigm. This approach limits health to the absence of disease and intends to address the latter by specific “high-impact” or “cost-effective” interventions, neglecting the root causes of ill-health and the complex interplay between individual interventions and (health) systems. This collection invites contributions that demonstrate how systems and complexity thinking can inform and transform public health policy and practice.
The interplay between public health policy and community practice is essential in shaping health outcomes and addressing systemic challenges within health systems. Despite the formulation of comprehensive public health policies, translating these policies into effective community-level interventions often faces numerous obstacles, including resource limitations, bureaucratic inertia, and varying local contexts. Understanding the dynamics between policy intent and on-the-ground implementation is crucial for fostering health equity and improving population health. The ability to navigate these complexities is vital for public health professionals, policymakers, and community practitioners alike. We are particularly interested in articles that showcase practical applications of systems approaches to address real-world public health challenges. We especially encourage submissions from authors in low- and middle-income countries (LMICs), highlighting efforts to strengthen healthcare systems in their specific contexts.
The purpose of this Collection is to explore the systemic challenges in public health and the strategies employed to overcome them in community settings. We invite contributions that examine case studies, innovative frameworks, and collaborative approaches that enhance policy implementation and address local health needs.
Keywords: public health, health policy, community health, health economics, social determinants of health, political determinants of health, commercial determinants of health, health system, systems thinking, complexity science
This Collection supports and amplifies research related to SDG 3.
Publishing Model: Open Access
Deadline: May 31, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in