Making the Most of Brain Dock: Translating a Uniquely Japanese Screening Tradition into Evidence for Primary Stroke Prevention
Published in Healthcare & Nursing, Neuroscience, and General & Internal Medicine
The Challenge Behind the Data
https://doi.org/10.1038/s41440-026-02639-z
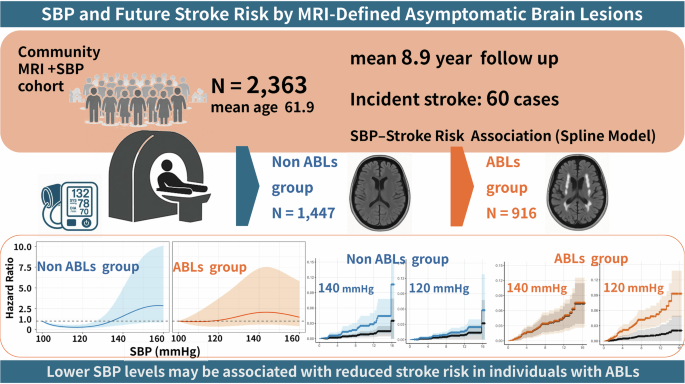
"Systolic blood pressure and future stroke risk by asymptomatic brain lesions in a community MRI cohort: a retrospective study - Hypertension Research"
At Shimane University, we have built one of Japan's largest Brain Dock cohorts over more than three decades, accumulating data from more than 10,000 participants. Yet this very scale has long concealed a methodological paradox. Because individuals who voluntarily undergo self-funded preventive screening tend to be health-conscious and proactive about their wellbeing, the incidence of stroke within our cohort is, by consequence, comparatively low. For years, this fortunate biological reality came at an analytic cost: traditional threshold-based statistical approaches lacked the power to detect meaningful associations, and the evidence needed to translate imaging findings into structured clinical guidance remained frustratingly out of reach.
A New Analytic Path
Our study, now published in Hypertension Research, represents our attempt to overcome this limitation. Rather than imposing arbitrary blood pressure cut-offs, we employed restricted cubic spline (RCS) modelling to characterise the smooth, continuous relationship between systolic blood pressure (SBP) and stroke hazard across its full observed range. This approach, combined with formal statistical interaction testing between SBP and asymptomatic brain lesion (ABL) status, multiple imputation with chained equations to handle missing covariate data, and bootstrap-based internal validation to assess model optimism, allowed us to extract interpretable signal from a dataset where events were rare but follow-up was long and imaging characterisation was meticulous.
What the Findings Reveal
Across a mean follow-up of nearly nine years in 2,363 neurologically healthy adults, stroke risk increased progressively with rising SBP regardless of ABL status. Crucially, however, among individuals with MRI-detected ABLs — encompassing white matter hyperintensities, silent brain infarctions, and cerebral microbleeds — the risk trajectory suggested an elevated vulnerability to blood pressure even at comparatively lower SBP levels. Cumulative hazard analyses across representative SBP categories of 120, 130, and 140 mmHg illustrated that, whereas risk differences across strata were modest among ABL-negative participants, a more discernible separation emerged among those with ABLs.
We wish to be transparent about the boundaries of these observations. The interaction between SBP and ABL status did not achieve conventional statistical significance, and confidence intervals were wide, particularly at the upper extremes of the SBP range. These findings are explicitly exploratory and hypothesis-generating. They should not be interpreted as evidence for specific revised clinical targets, nor should the spline-based inflection patterns be read as definitive thresholds. What they do offer, however, is a carefully reasoned foundation for future hypothesis-driven investigation.
Toward Precision Prevention
The broader significance of this work lies in its conceptual contribution to what might be called precision cerebrovascular prevention. Current international guidelines — including the 2025 AHA/ACC recommendations — provide clear SBP targets for most adults but offer no specific guidance for individuals in whom MRI has incidentally revealed silent cerebrovascular disease. Our findings suggest that this may be a clinically meaningful distinction worth investigating further. ABLs, though clinically silent, may reflect a state of heightened microvascular fragility and impaired cerebrovascular autoregulation that renders the brain more susceptible to the cumulative consequences of even modestly elevated blood pressure. If confirmed in larger prospective cohorts and interventional studies, this paradigm could position MRI-detected cerebrovascular markers as actionable imaging biomarkers within a personalised hypertension management framework — an approach conceptually aligned with precision medicine strategies already established in diabetes and chronic kidney disease.
A Reflection on the Journey
There is something fitting about the fact that this evidence has emerged from Brain Dock — a programme conceived in Japan, built on the belief that early detection serves prevention, and sustained by the quiet commitment of tens of thousands of individuals who chose to invest in their own health before symptoms demanded it. The road from data to evidence has been long, and the limitations of this study are real. But we hope this work — born of three decades of institutional dedication, refined through contemporary statistical methodology, and grounded in the trust of our community participants — takes a meaningful step toward establishing what Brain Dock can genuinely offer: not merely the identification of risk, but the beginning of a rational, imaging-guided framework for acting on it.
Key points for readers:
-
Study population: 2,363 neurologically healthy adults from the Shimane Brain Dock cohort (mean follow-up 8.9 years)
-
Core method: Cox proportional hazards models with restricted cubic splines, stratified by ABL status, with formal interaction testing and bootstrap internal validation
-
Main finding: Stroke risk increased progressively with SBP in both groups; ABL-positive individuals showed a trend toward risk elevation at comparatively lower SBP levels
-
Clinical implication: MRI-detected ABLs may serve as imaging biomarkers for refining individualised blood pressure management strategies for primary stroke prevention
Follow the Topic
-
Hypertension Research
Hypertension Research is the official journal of the Japanese Society of Hypertension, publishing high-quality original research articles, reviews, correspondence and editorials on all aspects of hypertension and related cardiovascular diseases.




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in