Understanding Australia’s Infectious Disease Trends Amid COVID-19: A Decade of Insights
Published in Microbiology and Public Health
Infectious diseases are constantly evolving, and understanding their trends is crucial to keeping communities healthy. Our study examines how notifiable diseases in Australia changed over the last decade, including during the COVID-19 pandemic. This study, which analysed data from the National Notifiable Disease Surveillance System from 2012 to 2022, sheds light on patterns of various diseases and the impact of the pandemic's public health measures.
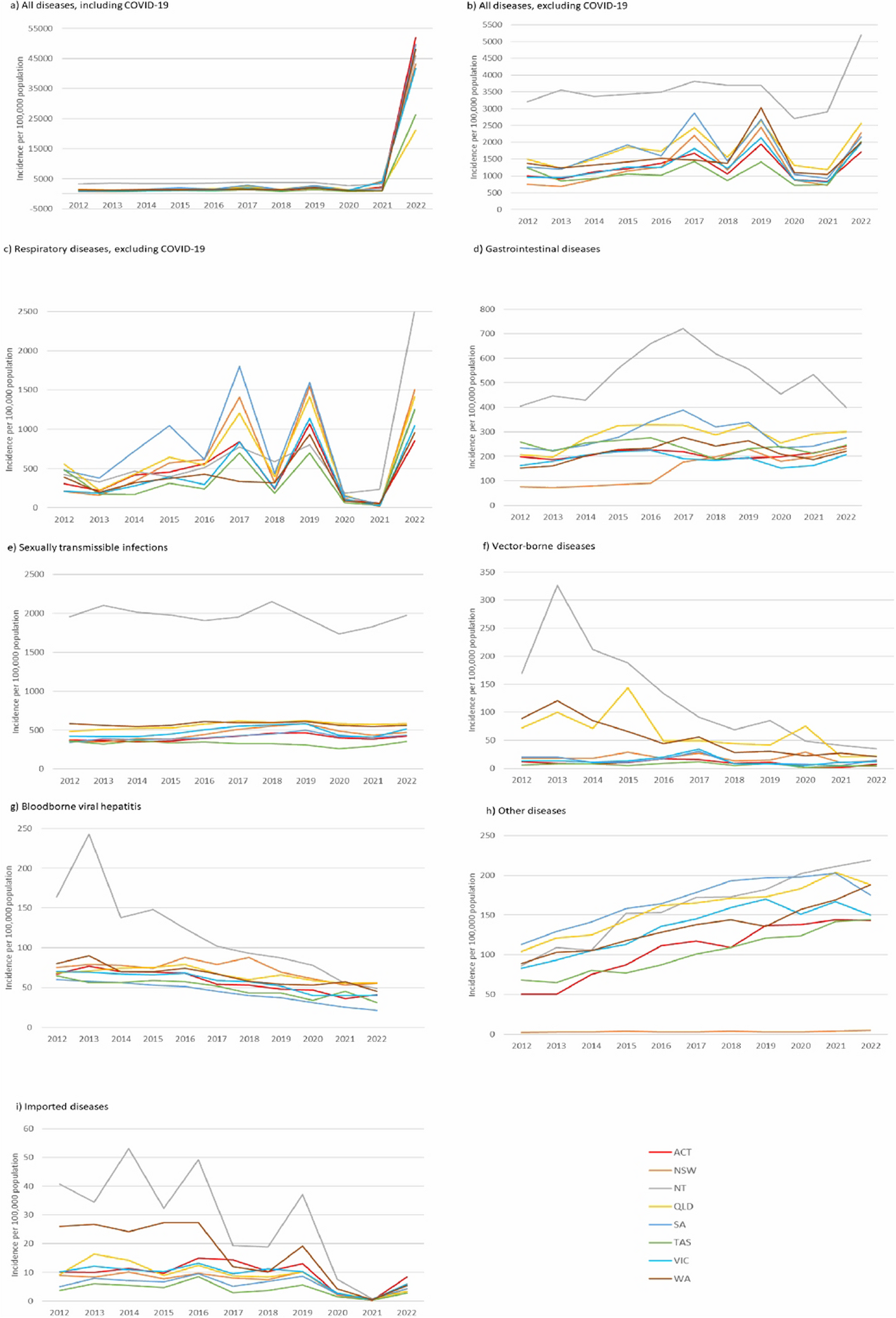
Our study found that prior to COVID-19, notifications for many infectious diseases were on the rise, especially respiratory and gastrointestinal infections. In contrast, diseases transmitted through blood or by vectors, such as viral hepatitis and vector-borne illnesses, showed a slight decline. We found an annual average increase of about 11% for all disease notifications from 2012 to 2019, with respiratory diseases leading this surge. These findings indicate shifts in healthcare engagement and public health policies, diagnostic technology, and possibly changing lifestyles.
With the onset of COVID-19 in 2020, Australia implemented some of the world's most stringent public health measures, including lockdowns, international travel restrictions, and social distancing mandates. The effects on other diseases were profound. Respiratory infections, such as the flu, dropped significantly due to reduced social interactions, masking, and sanitation protocols. However, by 2022, as restrictions eased, these infections rebounded significantly.
Interestingly, while COVID-19 measures decreased respiratory infections and imported diseases, we noted that some infections continued to rise, such as certain gastrointestinal diseases and STIs. This suggests that while some infections are closely tied to social behaviour and public movement, others are less influenced by these factors or might be indirectly affected by changes in healthcare access and behaviours during lockdowns.
Using pre-pandemic trends, we also estimated that over 200,000 cases of various infections were likely averted during the pandemic. We estimated that 65,000 fewer gastrointestinal infections and 121,000 fewer sexually transmitted infections were notified. These “averted cases” provide valuable insights, showing the influence of public health measures on infectious disease dynamics. While the declines in respiratory and imported infections were expected due to restricted travel and physical interactions, the reduction in other diseases highlights how closely healthcare access and behaviours are intertwined with transmission.
Why These Findings Matter
The study’s insights are significant for several reasons:
-
Public Health Preparedness: Knowing how diseases respond to interventions helps us prepare for future pandemics. Public health policies can be adapted to mitigate the risks of other infections when similar measures are necessary.
-
Healthcare Planning: These trends inform healthcare resource allocation and support the development of targeted vaccination, diagnostic, and treatment programs.
This study provides a foundation for ongoing research. Future surveillance is essential to monitor whether these trends persist or shift again as communities adjust to a post-pandemic world. By understanding these trends, public health officials, researchers, and policymakers can make informed decisions that protect communities and create resilient health systems.
Follow the Topic
-
BMC Global and Public Health
An open access, transparent peer review journal publishing outstanding and influential research and opinion of broad interest to all professional communities involved in global and public health research, policy-making, implementation and delivery worldwide.
Related Collections
With Collections, you can get published faster and increase your visibility.
Climate change and human health: Unpacking connections, advancing solutions
BMC Global and Public Health is calling for submissions to our Collection on the intersection of climate change and global and public health. This Collection seeks to unpack the profound impacts of climate change on population health, health equity, and health systems – and the solutions needed to protect health, reduce inequities, and enhance health system resilience.
We welcome papers covering diverse geographies and populations (especially marginalized groups), climate hazards and risks (both direct and indirect), diseases and health outcomes (including physical and mental health), and health system areas. Submitted papers may fall under the following sub-themes:
1. Climate and Health Pathways and Mechanisms
How climate change affects population health, health equity, and health systems – with a focus on the pathways and mechanisms, the wide range of upstream drivers (ex. ecosystem change) and downstream determinants (ex. social conditions) involved, and existing and emerging solutions to address them
2. Climate Justice and Health Equity
How climate change worsens existing health inequities and impacts marginalized communities – and the range of solutions – from the community to the policy level – required to achieve climate justice and health equity
3. Data for Climate and Health: Challenges and Innovations
What data gaps and challenges are faced in climate and health research and action – and the emerging methodological, technological, and governance innovations for overcoming them to inform policies and societal responses
4. Interventions for Climate Change and Health
What are the emerging interventions – ex. clinical, technological, community-based, institutional – for climate-health problems – at micro, meso, and macro levels – and evidence of effectiveness, lessons learned from their implementation, and prospects for sustainability and scale up
This Collection supports and amplifies research related to SDG 3: Good Health and Well-Being and SDG 13: Climate Action.
We encourage work from local, regional, national, and global partnerships and collaboration among multidisciplinary scientists using multiple methodologies. We ask that authors be careful to use non-stigmatizing/preferred language in their manuscripts as outlined in relevant language guidelines for their respective fields.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer-review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Aug 13, 2026
Food security, nutrition, and dietary trends
BMC Global and Public Health is calling for submissions to our Collection on food security, nutrition, and dietary trends. These are interconnected elements that profoundly impact global health and well-being. As the world grapples with rapid population growth, climate change, and economic disparities, the challenges surrounding food access, quality, and sustainability have intensified. This Collection aims to gather diverse research that examines these complex relationships, focusing on how dietary patterns, food availability, and nutritional status influence overall health outcomes. By exploring the multifaceted nature of food systems, this Collection seeks to showcase pathways to achieve improved food security and nutritional health worldwide.
The goal of this Collection is to build a comprehensive body of knowledge that informs policy and practice. We encourage submissions that investigate:
Impact of dietary patterns on health outcomes
Addressing food insecurity through policy
Role of ultra-processed foods in nutrition
Personalized nutrition and dietary therapy
Nutritional supplements for malnutrition
This Collection supports and amplifies research related to SDG 2: Zero Hunger and SDG 3: Good Health and Well-Being.
We encourage work from local, regional, national, and global partnerships and collaboration among multidisciplinary scientists using multiple methodologies. We ask that authors be careful to use non-stigmatizing/preferred language in their manuscripts as outlined in relevant language guidelines for their respective fields.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer-review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: May 28, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in