Very old patients need palliative care,not intensive care - an empirical and normative analysis
Published in Mechanical Engineering and Philosophy & Religion
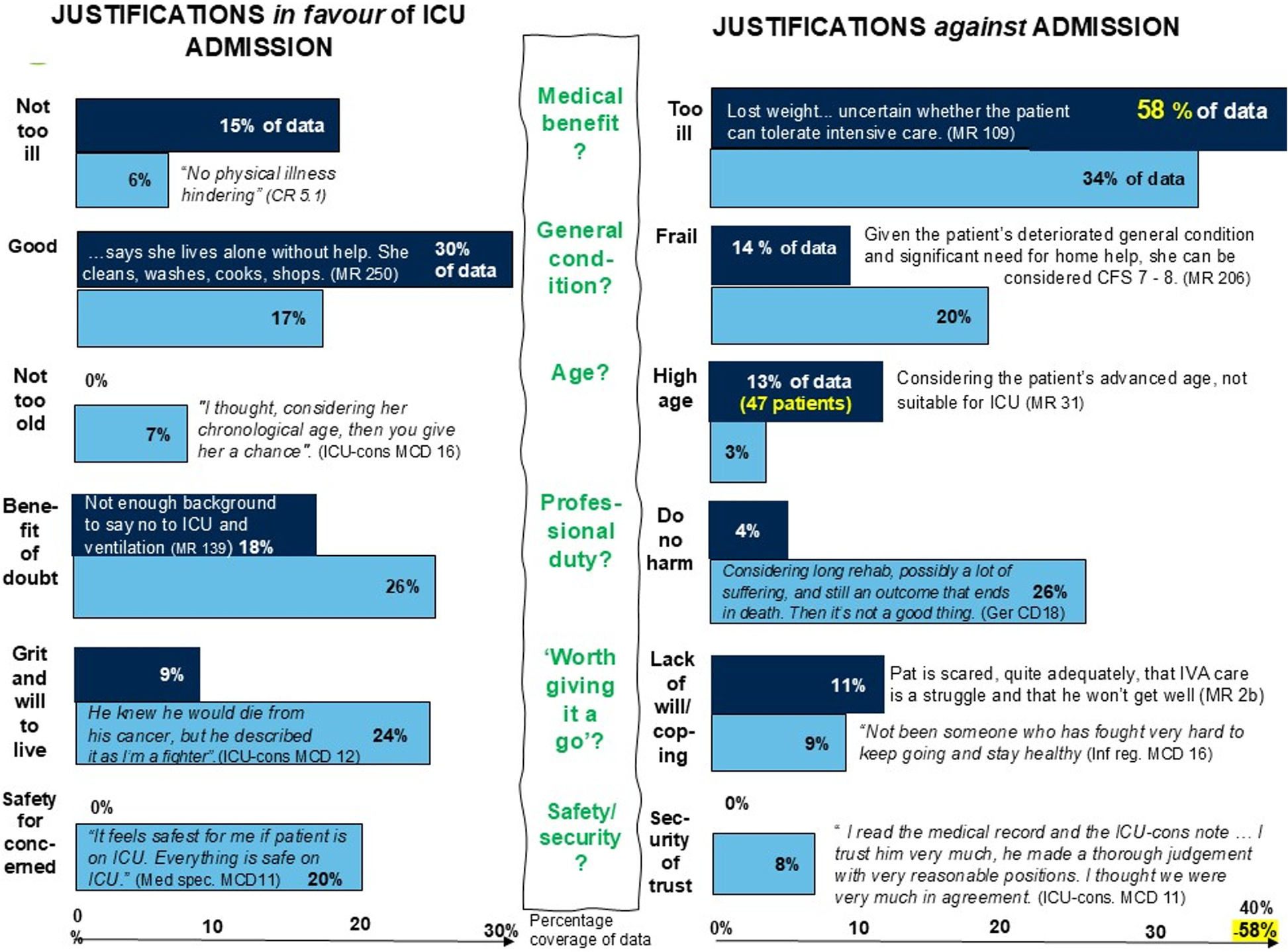
We found clear and consistent evidence – both quantitative and qualitative – that high chronological age is a key factor against ICU admission. Among all the variables we compared, only being 80 years or older clearly stood out as linked to not being admitted to intensive care.
Across every data source, high age kept reappearing as a justification for non-admission. In medical records, “considering age” was mentioned again and again. In the COVID Rounds, Moral Case Deliberations (structured reflections on ethically complex patient cases), and follow-up interviews, the phrase “very old” was used repeatedly when decisions were discussed.
Another powerful justification across all data was about not harming the patient. This included avoiding unworthy suffering, not subjecting patients to what was described as torture when ICU care offered no benefit and recognising ventilator treatment as risky. For patients over 80, ICU care was often described as unacceptable; at 90, death was seen as a natural event. One ICU consultant put it poignantly:
“Ninety feels like, if you’ve had a good life and you’re spry and healthy ... if you die suddenly, then it’s expected. And better than dragging to the ICU and tormenting the person.”
Interestingly, few justifications were directly linked to the pandemic. The patterns we found mirror those from pre-COVID studies, suggesting that what we captured ordinary clinical decision-making, not crisis-specific thinking.
Normative discussion
When discussing chronological age as a factor, our findings align with two key ethical principles: non-maleficence and justice.
Non-maleficence implies here sparing patients from unnecessary suffering and loss of dignity. Distributive justice connects with the ICU prioritisation literature, which tends to exclude patients “with a fuller lifecycle.” In intensive care, defining what counts as a need becomes crucial.
According to Swedish legislation, healthcare needs are defined by both the severity of a condition and the potential benefit of treatment. For very old patients, with higher ICU mortality and poorer recovery rates, the potential benefit is often limited. From this perspective, ICU care may not truly meet very old patients’ needs.
Following the legal principle of Need and Solidarity, treatment should only be prioritised when there is potential for benefit. Our results therefore suggest that many very old patients are better served by palliative rather than intensive care.
A call for courage and clarity
We believe it is time for a national – and perhaps international – guiding policy on triage systems for very old patients in everyday care. Such a policy should be developed with courage and transparency, openly supporting a palliative approach for the very old.
Follow the Topic
-
BMC Medical Ethics
This journal is an open access journal publishing original peer-reviewed research articles in relation to the ethical aspects of biomedical research and clinical practice, including professional choices and conduct, medical technologies, healthcare systems and health policies.
Related Collections
With Collections, you can get published faster and increase your visibility.
Pediatric ethics
Pediatric ethics encompasses the complex moral considerations that arise in the healthcare of children, a population that requires special considerations due to their developmental, emotional, and social needs. As healthcare providers navigate the intricacies of medical decision-making for minors, ethical dilemmas frequently arise, particularly concerning parental authority, child autonomy, and the balance between beneficence and respect for the child's emerging independence.
The significance of research in pediatric ethics is underscored by the evolving landscape of child healthcare, where advances in medical technology and treatment options present new ethical challenges. Recent discussions have illuminated the importance of involving children in healthcare decisions appropriate to their maturity level, emphasizing the role of informed consent and assent. Continued exploration in pediatric ethics holds promise for developing more refined ethical guidelines that can adapt to the ever-changing healthcare environment. Future research may lead to improved frameworks for decision-making that incorporate the voices of children, parents, and healthcare providers alike, fostering collaborative approaches that respect the rights of minors while ensuring their well-being.
BMC Medical Ethics is calling for submissions to our Collection, Pediatric ethics. This Collection aims to explore these multifaceted ethical issues, promoting a deeper understanding of pediatric ethics in various clinical contexts. Key topics of interest for submission include, but are not limited to:
Ethical dilemmas in pediatrics
Parental authority vs. pediatric autonomy
Consent in children and adolescents
Ethics in neonatal care
End-of-life care for pediatric patients
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being and SDG 10: Reduced Inequalities.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jun 02, 2026
Medical ethics education
Medical ethics education has emerged as a critical component of healthcare training, equipping future healthcare professionals with the necessary tools to navigate the complex ethical dilemmas they will encounter in clinical practice. The integration of ethics into medical curricula serves to foster a deeper understanding of moral principles, patient rights, and the responsibilities of healthcare providers. As the healthcare landscape evolves, it is imperative to continuously assess and refine educational approaches to ensure that they effectively address emerging ethical challenges, including those related to technological advancements and diverse patient populations.
The significance of robust medical ethics education extends beyond individual practitioners; it influences the overall quality of care provided to patients and the integrity of healthcare systems. Recent advancements in this field have included the development of innovative pedagogical methods, such as simulation-based learning and interdisciplinary approaches, which promote active engagement and critical thinking among students. These developments not only enhance students' moral reasoning and decision-making skills but also contribute to a culture of professionalism and ethical competency within healthcare organizations.
BMC Medical Ethics is calling for submissions to our Collection, Medical ethics education. Key topics of interest for submission include, but are not limited to:
Empirical studies exploring ethical knowledge in healthcare professionals.
Strategies for enhancing moral competency in healthcare professionals.
Clinical ethics training approaches
Patient-centered ethics in practice
This Collection supports and amplifies research related to SDG 4: Quality Education.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Jun 02, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in