When Impulsivity Is Present but Hidden — A Neural Clue in Bipolar Vulnerability
Published in Neuroscience, General & Internal Medicine, and Behavioural Sciences & Psychology
Impulsivity is often viewed as a stable trait: you either have a lot of it, or you don't. In bipolar disorder, it's a core feature of mania and hypomania, fueling risky decisions, heightened goal pursuit, and thrill-seeking. Yet in the clinic, impulsivity doesn't always show up that way. During manic or hypomanic episodes, impulsivity is overt; patients often act with little forethought. When depression dominates, however, that same impulsivity can seem to vanish entirely, replaced by withdrawal, low energy, and inertia. This clinical mismatch prompted a deceptively simple question: Is impulsivity truly absent during depressive states, or is the neural vulnerability for impulsivity still present in the brain, just not expressed in behavior?
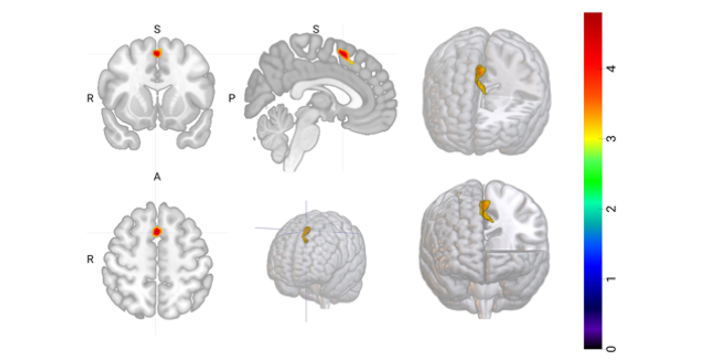
To investigate, we turned to functional MRI and a reward expectancy task. Participants anticipated potential monetary wins, a task phase that reliably engages motivational-approach neural circuits, allowing us to probe impulsivity-related neural signals in an anticipatory context, without requiring behavioral or self-reflective responses that might obscure underlying drives.
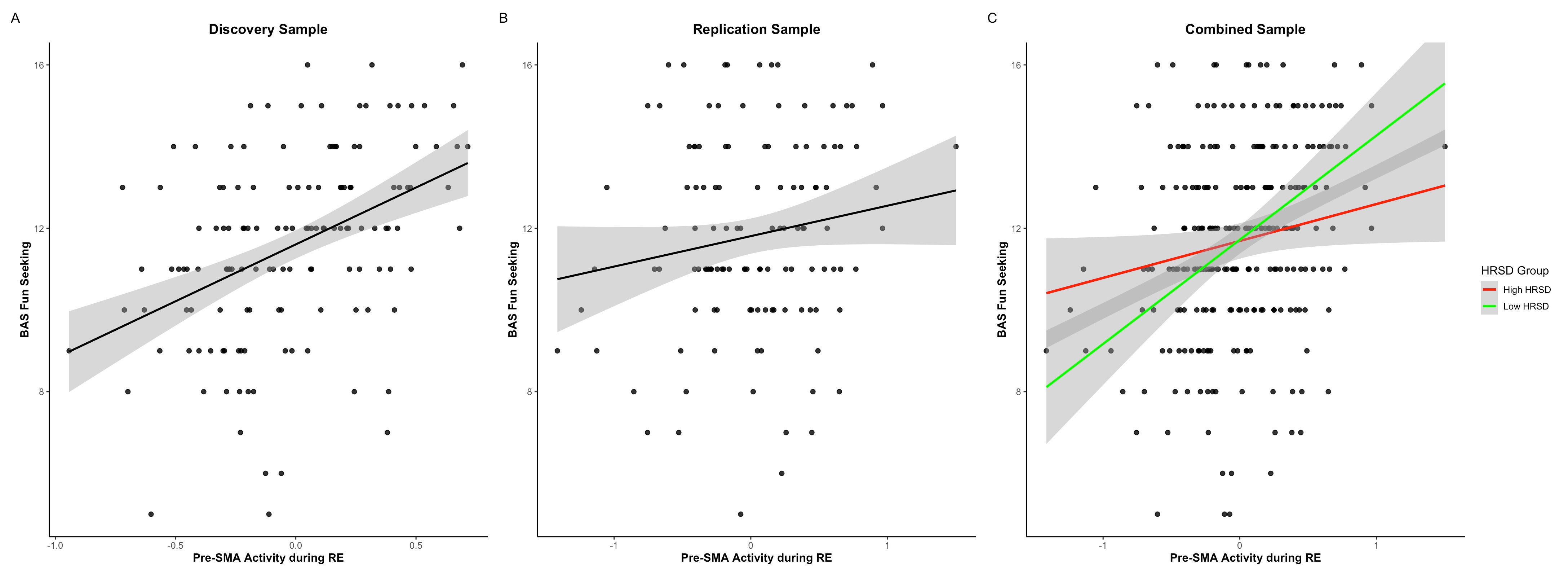
Across two independent samples of young adults, we consistently linked greater activity in the pre-supplementary motor area (pre-SMA) to higher BAS Fun Seeking, an impulsivity facet capturing the drive for excitement and novelty. The pre-SMA functionally sits at the crossroads of motivation and action initiation, helping translate internal urges into planned — or impulsive — behavior, which made it a prime candidate for capturing approach-related vulnerability in bipolar disorder. Replication was a top priority from the start. Despite differences in participant profiles, scanners, and symptom levels between cohorts, the core pattern remained robust, reinforcing our confidence that this reflects a meaningful signal rather than noise.
The real revelation, however, was how current mood modulated this link. As current depressive symptom severity increased, the association between pre-SMA hyperactivity and Fun Seeking weakened significantly. Importantly, this was not due to reduced pre-SMA activity itself — the neural signal stayed robust. Instead, its translation into Fun Seeking was dampened, masked by affective state. Together, our results point to impulsivity as a latent neural drive that persists across mood states in bipolar vulnerability, but whose behavioral expression is gated by current affective state.
Clinically, this is critical for bipolar disorder. Relying on behavioral observation or self-report alone risks underestimating vulnerability during depression, when impulsivity hides rather than disappears. A stable neural marker like pre-SMA hyperactivity during reward anticipation could provide a more trait-like index of mania/hypomania risk, potentially aiding earlier detection, monitoring across episodes, or guiding intervention. Targeted neuromodulation of the pre-SMA has already shown promise in reducing impulsivity in related disorders, and these findings suggest it may be a relevant target in bipolar vulnerability as well.
Looking ahead, we are eager to test whether this marker predicts mood episode onset or transitions from externalizing disorders to bipolar disorder, as well as how it interacts with other markers from our prior work, including left ventrolateral prefrontal cortical activity during reward anticipation, which we have previously linked to mania/hypomania risk as well. The broader point, however, may be this: a patient who appears inert during depression may still carry the underlying neural risk for high impulsivity. Recognizing that distinction, and finding ways to detect it, may be what matters most for precision-guided early intervention in bipolar disorder.
Follow the Topic
-
Molecular Psychiatry

This journal publishes work aimed at elucidating biological mechanisms underlying psychiatric disorders and their treatment, with emphasis on studies at the interface of pre-clinical and clinical research.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement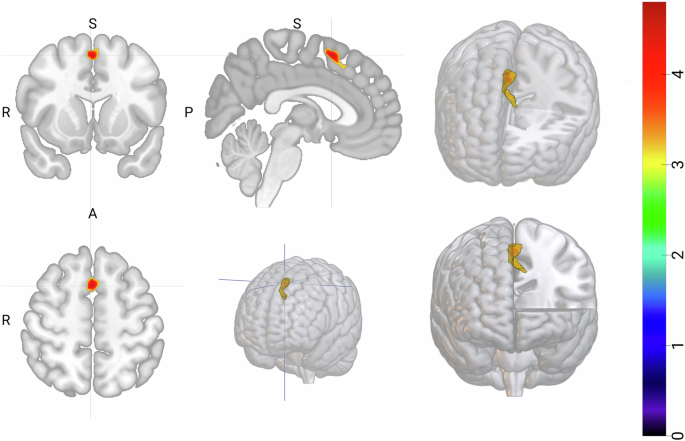


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in