Paving the way for precision treatment of psychiatric symptoms with functional connectivity neurofeedback
Published in Neuroscience, Protocols & Methods, and Biomedical Research
Different patients diagnosed with Major Depressive Disorder (MDD) report suffering from different subsets of symptoms, yet ultimately most are prescribed with homogenous first line treatment. For example, Person A might primarily suffer from repeated, uncontrollable, worrying and Person B might primarily suffer from a reduced ability to experience pleasure in their daily life and yet both are likely to be diagnosed as having MDD and prescribed serotonin reuptake inhibitors. Different subsets of symptoms are known to relate to different underlying neural perturbations and so it is logical that the same treatment will not work equally well when treating different types of depressive symptoms. It is therefore unsurprising that 30-50% of patients with MDD do not respond fully to their treatment. To improve response rates, treatment needs to become more precise and individual differences need to be better considered.
It was with the idea of 'precision psychiatry' in mind that we first conceived of our novel approach. We rationalized that if different types of symptoms arise from different underlying neural disturbances, then it would make sense to go straight to the root of the problem in each case. If we can bring these neural circuits back to the healthy states, then we expect to see a reduction in the associated symptoms. To test this, we used a technique called real-time fMRI neurofeedback, a kind of brain-machine interface that allows people to observe and learn to change their own brain activity in real time.
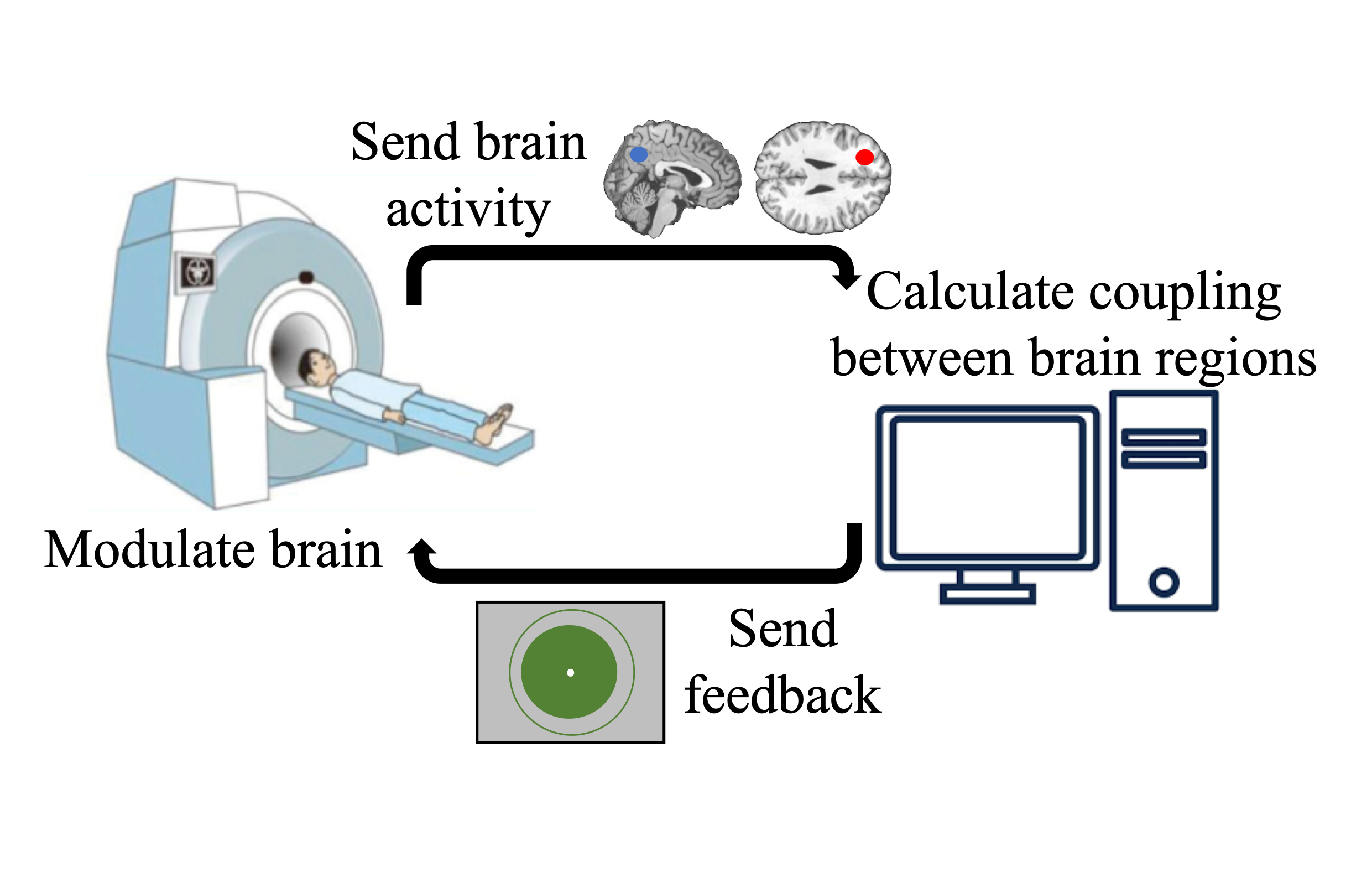
For our first target, we chose rumination. Think of rumination as a mental hamster wheel — you know you should stop worrying, but negative thoughts just keep going round and round in your head, like Person A from the example above. Research suggests that this arises partly from disturbances to coupling between a brain region involved in internal self-referential thinking (the posterior cingulate cortex) and a brain region involved in external goal-directed behavior (the dorsolateral prefrontal cortex). Our goal was to use real-time fMRI neurofeedback to train people to bring this coupling back toward a healthier balance.
To do this, we turned brain training into something resembling a video game. While lying in an MRI scanner, participants watched a green circle on a screen and were simply told: "use your brain to somehow make the green circle bigger." Participants came up with surprisingly creative strategies to modulate this neural coupling: some did mental arithmetic, others played word-association games, and some even imagined tiny people running around the edge of the green circle. Crucially, brain scans were being sent to a computer, on which a program was set to change the size of the displayed green circle in real-time dependent on how healthy-like the coupling between two target brain regions was. This feedback allowed the participants to learn to change brain region coupling with experience.
The first author, Jessica Taylor, getting ready to run a pilot subject in our brain training neurofeedback task.
We ran 69 participants across multiple sessions to understand not just whether this approach works, but how to make it work best. For example, we tested whether brain training on consecutive days is more effective than spreading sessions out over weeks, or whether stronger reward incentives improve performance. Indeed, participants who trained on consecutive days and had the highest earning potential showed the greatest improvements, with coupling between the two targeted brain regions becoming more healthy-like with training for these participants. Beyond the training task itself, the healthier brain patterns carried over into periods when participants were simply resting — suggesting a genuine shift in participants brain activity rather than a performance effect. Furthermore, the results extended beyond the smaller targeted brain regions to the greater brain networks to which these belong. Most importantly, the greater the improvement in targeted brain activity over the course of training, the greater the reduction in depressive and rumination symptoms. Notably, the same was not found for anxiety symptoms, which supports the precision of this approach: we targeted rumination, and rumination is what changed.
Overall, our results are promising for a new type of brain-based, symptom-specific intervention. Though this work took multiple years and lots of hard work from many collaborators at all levels, the findings indicate the possibility of precision neuromodulation in psychiatric disorders. The dream is that one day patients will be able to walk into a clinic, have their brains scanned, and then be prescribed a portable EEG headset for neurofeedback targeted at their own specific symptoms — something they could use from the comfort of their own homes.
Follow the Topic
-
Translational Psychiatry
This journal focuses on papers that directly study psychiatric disorders and bring new discovery into clinical practice.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
From mechanism to intervention: translational psychiatry of childhood maltreatment
Publishing Model: Open Access
Deadline: Jun 30, 2026
Moving towards mechanism, causality and novel therapeutic interventions in translational psychiatry: focus on the microbiome-gut-brain axis
Publishing Model: Open Access
Deadline: Nov 15, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in