When SIADH Meets PRES: A Rare Neuroendocrine Link Uncovered
Published in Neuroscience and Biomedical Research
Explore the Research
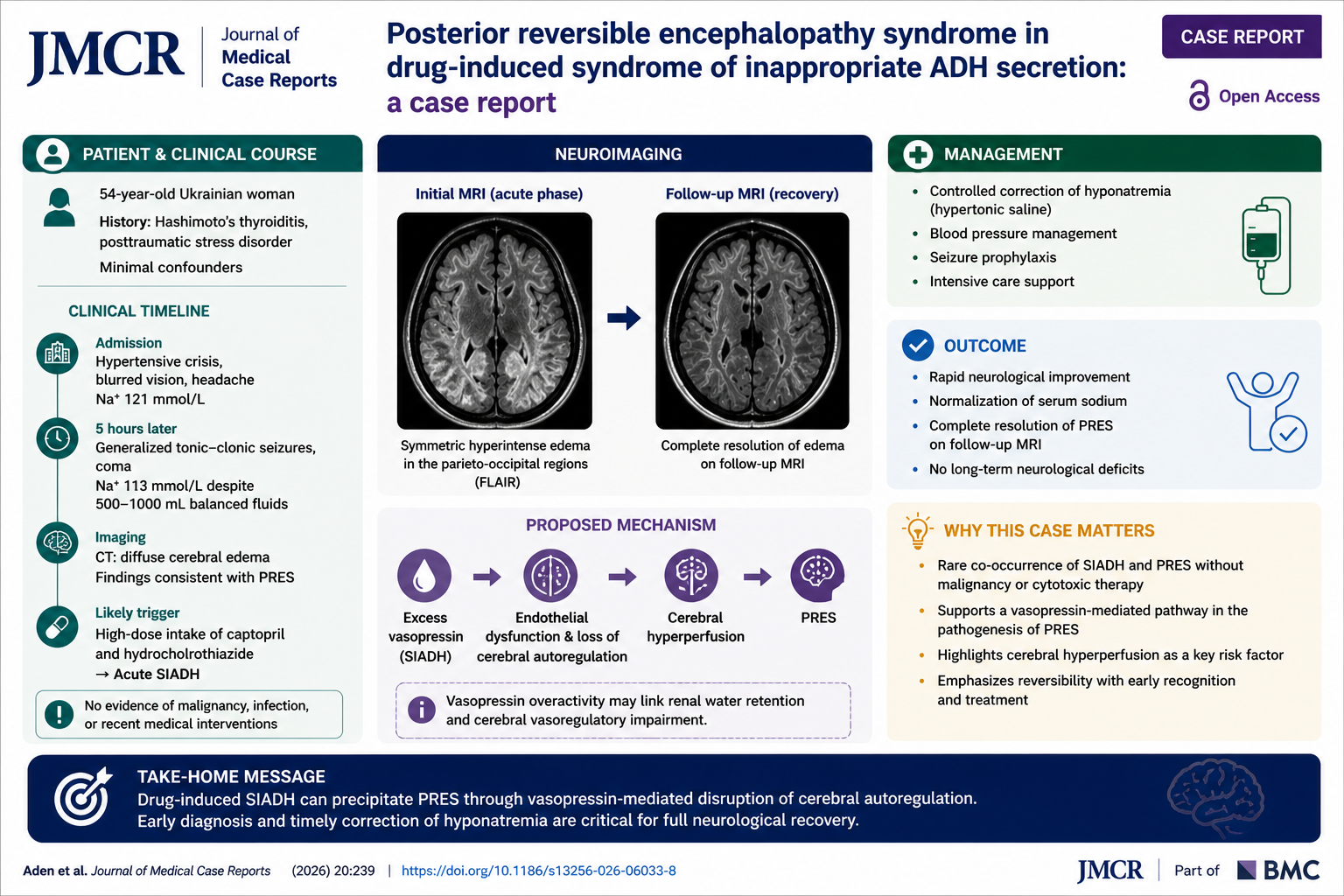
Posterior reversible encephalopathy syndrome in drug-induced syndrome of inappropriate ADH secretion: a case report
Case summary
In this case report from the Journal of Medical Case Reports, Aden and colleagues describe a 54-year-old woman who developed acute drug-induced SIADH followed by PRES.
The patient presented with hypertensive crisis, headache, and visual disturbances. Initial labs showed hyponatremia (Na⁺ 121 mmol/L), which rapidly worsened to 113 mmol/L within hours. This deterioration coincided with high-dose ingestion of captopril and hydrochlorothiazide—likely triggering SIADH.
Her clinical course escalated dramatically:
Generalized tonic–clonic seizures
Coma
Diffuse cerebral edema on CT imaging
Neurologic evaluation confirmed PRES, supported by visual symptoms, hypertension, and characteristic imaging findings.
Despite severe presentation, the patient improved with:
Controlled correction of hyponatremia using hypertonic saline
Blood pressure management
Supportive intensive care
Remarkably, she made a full neurological recovery within days, and follow-up MRI showed complete resolution of PRES, with no long-term deficits.
Why this case matters
This report is notable for several reasons:
Uncommon association: SIADH and PRES are rarely reported together in otherwise healthy individuals without malignancy or chemotherapy.
Mechanistic insight: The case supports a shared pathway involving vasopressin (AVP) overactivation, potentially affecting both renal water handling and cerebral vascular regulation.
Cerebral autoregulation: Findings reinforce the role of cerebral hyperperfusion and endothelial dysfunction in PRES pathogenesis.
Reversibility: Timely recognition and correction of the underlying trigger can lead to complete neurological recovery, even after severe presentation.
Clinical take-home message
Acute, drug-induced SIADH can precipitate PRES through vasopressin-mediated dysregulation of cerebral perfusion. Early recognition and prompt correction of hyponatremia are critical to achieving full neurological recovery.
Question:
Which mechanism most plausibly links SIADH to the development of PRES in this case?
A. Direct neuronal toxicity from hyponatremia
B. Autoimmune-mediated demyelination
C. Vasopressin-mediated dysregulation of cerebral blood flow
D. Primary intracranial infection
Correct answer:
C. Vasopressin-mediated dysregulation of cerebral blood flow
Explanation:
Excess vasopressin activity in SIADH may contribute to impaired cerebral autoregulation and endothelial dysfunction, promoting hyperperfusion and vasogenic edema—key features in PRES pathophysiology.
Journal of Medical Case Reports is the world’s first international, PubMed-listed, medical journal devoted to publishing case reports from all medical disciplines and will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports. The journal is open access, and strongly endorses the CARE guidelines for case reports, requiring authors to submit populated CARE checklists with submissions to improve transparency in reporting.
Follow the Topic
-
Journal of Medical Case Reports
This journal will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in