A mixed methods study of using Wasta in healthcare services in Palestine: predictors, consequences and proposed solutions
Published in Business & Management
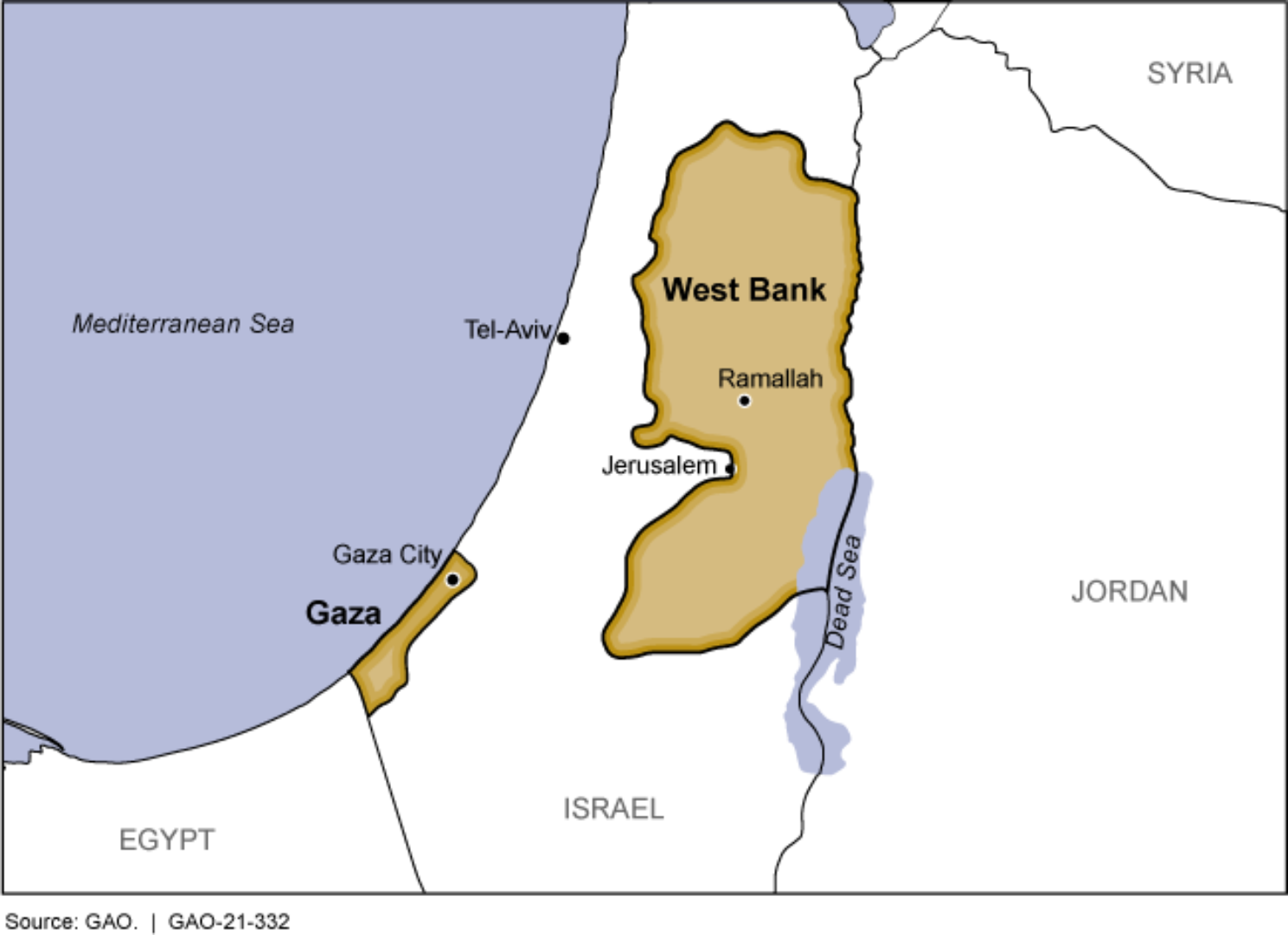
This unique study conducted in 2021-22 in the occupied Palestinian territories and Gaza examined the use of wasta. Examining the use of wasta in healthcare in Palestine, we employed qualitative (ten health professionals and eighteen patients from Gaza and the West Bank) and quantitative research methods, surveying more than 700 individuals. Where the official processes to reach a goal are corrupt, bureaucratic, or inefficient persons often turn to using wasta to overcome barriers.
Participants included refugees living in camps, urban, and rural dwellers from the age of 18. Approximately one-third (34%) stated they used wasta to get a health service in the last year, 39.3% from Gaza and 31.6% from the West Bank. Wasta is reportedly also used within healthcare institutions by some employees to gain unfair advantages over others. Our interviews also highlighted social and organizational-level predictors and consequences of wasta. The potential predictors include scarcity of resources (material, human, and financial), cultural factors, and inefficient administration. The consequences of wasta include inequities in healthcare, decreased healthcare professionals’ motivation and morale, and lower service quality.
This study considerably enriched the conceptual definition of wasta use in healthcare settings by elucidating the multifaceted mechanisms through which it manifests, its predictors, and its consequences. Wasta can be employed by utilizing social connections, political affiliations, family ties, and economic means. This study confirmed previous research about the role of organizational, social, and economic factors in causing wasta.
The utilization of wasta in healthcare leads to outcomes such as disparities, reduced staff motivation, and compromised service quality. Through wasta and social connections, some patients may gain unfair advantages over others. Our interviews revealed that when staff are promoted and rewarded through wasta or social connections rather than for hard work, dedication, or performance, inequities become manifest. These unfair practices cast a negative shadow on the institution and its services by eroding the morale and motivation of its personnel.
Predictors and consequences of wasta in countries where official processes to reach a goal are corrupt, bureaucratic, or inefficient, individuals resort to wasta to overcome oppressive processes [1]. Patriarchy, tribalism, religious and political strife, inequities, discrimination, and lack of trust in public institutions are contextual vices within which wasta proliferates [2, 3].
The higher prevalence of wasta in refugee camps and in Gaza is probably because these communities have faced disadvantages for generations, enduring various difficulties and injustices. It is possible that their perception, based on personal experiences or hearsay, is that utilizing wasta can help improve their situation. In the camps, residents are bound by a common history of forced displacements and are living in crowded conditions. Political activism is stronger in camps.
Wasta results in inequalities by depriving women and those with lower social networks from accessing opportunities [4, 5]. Wasta encourages people to invest more in social networks rather than other more useful forms of social capital [6]. Wasta could decrease the utilization of healthcare services via a lack of trust in the system. Additionally, wasta may lower healthcare providers’ motivation, satisfaction, and morale. Our interviews highlighted social and organizational-level predictors and consequences of wasta. The consequences of wasta include inequities in healthcare, decreased healthcare professionals’ motivation and morale, and lower service quality.
It is essential to optimize processes for efficiency, alleviate financial strains, and implement accountability measures in the healthcare domains.
- Horak S, Afiouni F, Bian Y, Ledeneva A, Muratbekova-Touron M, Fey CF. Informal networks: Dark sides, bright sides, and unexplored dimensions. Manag Organ Rev. 2020;16:511–42.
- Hutchings K, Weir D. Guanxi and Wasta: A comparison. Thunderbird Int Bus Rev. 2006;48:141–56.
- Alsarhan F, Ali S, Weir D, Valax M. Impact of gender on use of wasta among human resources management practitioners. Thunderbird Int Bus Rev. 2021;63:131–43.
- Abalkhail JM, Allan B. “Wasta” and women’s careers in the Arab Gulf States. Gend Manag Int J. 2016;31:162–80.
- Banihani M. Empowering Jordanian women through entrepreneurship. J Res Mark Entrep. 2020;22:133–44.
- Baranik L, Gorman B, Wright N. Wasta and its relationship to employment status and income in the Arab Middle East. Curr Sociol. 2021;:00113921211024705.
Follow the Topic
-
BMC Health Services Research
An open access, peer-reviewed journal that considers articles on all aspects of health services research, focusing on digital health, governance, policy, system quality and safety, delivery and access, financing and economics, implementing reform, and the workforce.
Related Collections
With Collections, you can get published faster and increase your visibility.
Work-life integration among medical professionals
BMC Health Services Research is calling for submissions to our Collection on Work-life integration among medical professionals.
The concept of work-life integration has gained considerable attention in recent years, especially among professionals and pharmacists who face unique challenges in their demanding professions. These healthcare professionals often experience long work hours, high stress, and the emotional toll of patient care, which can adversely affect their personal lives and overall well-being. This Collection aims to explore the various dimensions of work-life integration within these fields, examining factors that contribute to or detract from achieving a healthy equilibrium between professional responsibilities and personal fulfilment.
Achieving work-life integration is crucial not only for the well-being of medical professionals but also for the quality of care provided to patients. Research indicates that when medical professionals experience burnout or dissatisfaction due to work-life imbalance, it can lead to decreased job performance and poorer patient outcomes. Advances in organizational strategies, such as flexible scheduling, mental health support, and initiatives promoting physical activity, have shown promise in enhancing work-life integration. Continued exploration of these topics can yield effective solutions that benefit both practitioners and the healthcare system.
Topics include but are not limited to:
Impact of work hours on burnout among medical professionals
Professional engagement during personal time and its impact on well-being
Strategies for improving work-life integration in healthcare
Role of physical activity in managing stress for pharmacists
Challenges faced by general practitioners in achieving work-life integration
Work-life integration initiatives in surgical practice
Organizational strategies for promoting sustainable work-life integration
Individual predictors of effective work-life integration
Effects of clinical workload on personal relationships and life satisfaction
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Aug 07, 2026
Patients' knowledge of the indications for their medications
BMC Health Services Research is calling for submissions to our Collection on Patients' knowledge of the indications for their medications.
Understanding the indications for prescribed medications is crucial for patient safety and effective healthcare delivery. Many patients lack adequate knowledge about their medications, which can lead to non-adherence, adverse drug reactions, and suboptimal health outcomes. This Collection invites research that examines the extent of patients' medication knowledge, the factors influencing their understanding, and the implications for healthcare practice. By exploring these aspects, we aim to illuminate the gaps in medication literacy and the importance of patient engagement in their treatment regimens.
Enhancing patients' knowledge of their medications is vital for fostering informed decision-making and promoting adherence to treatment plans. Recent advances in medication counseling, patient education programs, and digital health technologies have shown promise in improving medication awareness. These interventions not only empower patients but also support healthcare providers in delivering personalized care. By fostering a culture of medication literacy, healthcare systems can enhance patient outcomes and reduce the burden of medication-related issues.
Topics for submission:
Assessing medication literacy in diverse populations
Barriers and facilitators to understanding medication indications
Impact of patient education and other related interventions on medication adherence
Tools, interventions and strategies for enhancing patient medication knowledge
Understand how, why for whom and under what circumstances interventions to enhance medication knowledge work or not
This Collection supports and amplifies research related to SDG 3 (Good Health and Well-being).
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: Sep 30, 2026





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in