Behind the Paper: Intersecting Impacts of Ageing, Migration, and Socioeconomic Disparities on Health Equity – A Post-Pandemic Policy Review
Published in Social Sciences, Anatomy & Physiology, and Law, Politics & International Studies
The Story Behind the Paper
The Spark From Observation to Question
During the pandemic, we witnessed older adults in nursing homes devastated by COVID-19, migrant labourers losing their jobs and social protections, and low-income communities suffering high infection rates and poor access to care. These patterns felt connected. For example, an ageing migrant worker living precariously, lacking protection, and exposed to the virus illustrates overlapping vulnerabilities that erode health resilience.
In Ghana and many low- and middle-income countries, age-related care gaps, internal and external migration, and informal work intersect. We asked what the evidence reveals when ageing, migration, and socioeconomic inequality are examined together. How did the pandemic deepen these links, and what policy gaps emerged?
Conceptual Framing: Bringing Theory to Life
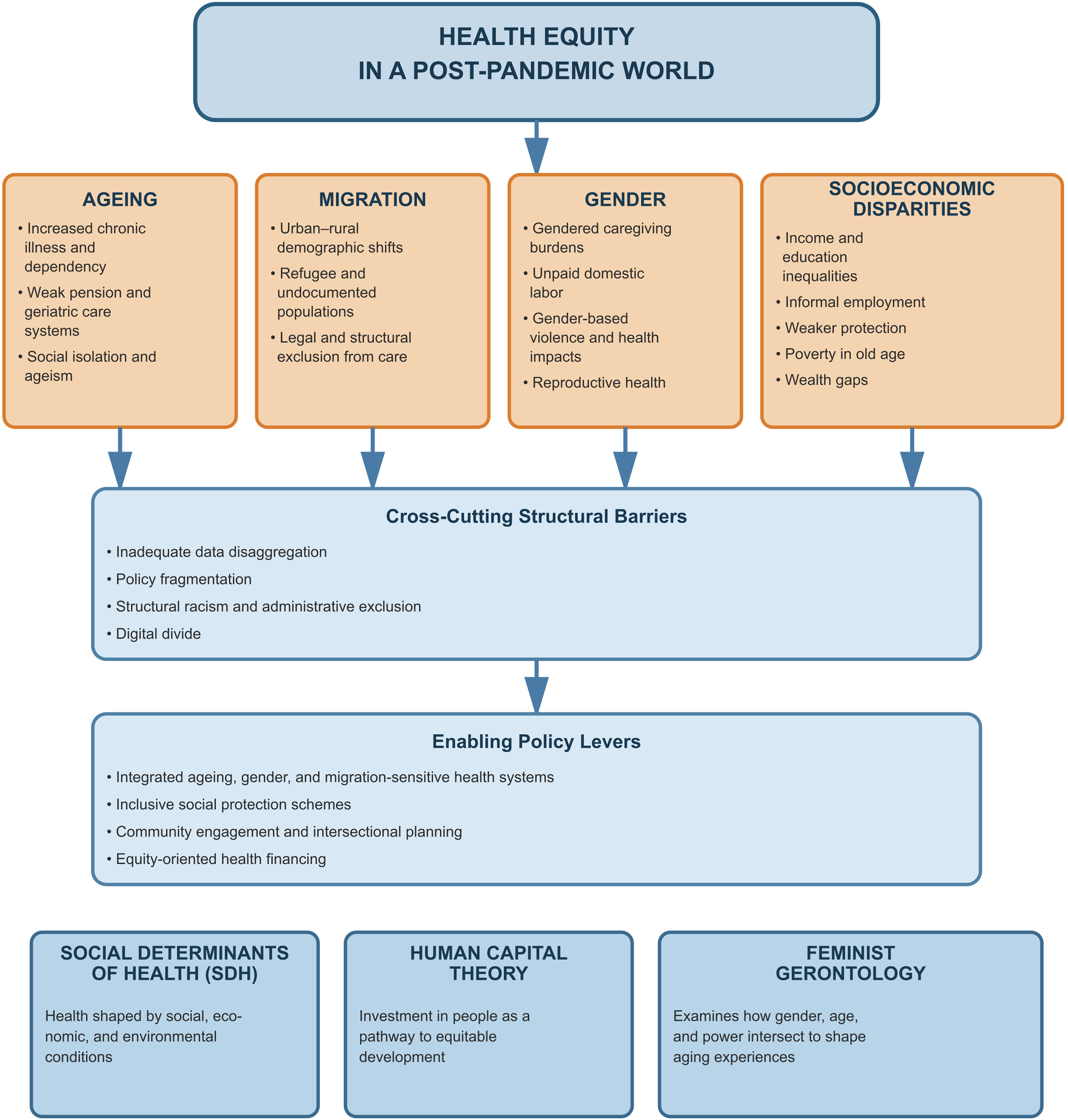
We grounded the study in three theoretical lenses
Social Determinants of Health (SDH) explains how living and working conditions, social protection, and public policy shape health outcomes.
Human Capital Theory, which considers how investment or disinvestment in health and skills influences lifetime resilience.
Feminist Gerontology, which captures ageing as a gendered life course process and highlights the burdens borne by older women and ageing migrants.
Our premise is that ageing, migration, and socioeconomic disadvantage are not additive. They intersect to multiply risk. The pandemic was a global stress test of this reality.
Methodology Systematic Review of the Policy Terrain
Following PRISMA 2020 guidelines, we preregistered our protocol on the Open Science Framework (OSF) and reviewed studies, reports, and grey literature from 2020 to 2024 that linked ageing, migration, and socioeconomic factors to health equity. In total, 49 sources met inclusion standards.
Key Findings: Four Intersecting Themes
-
Demographic inequality and uneven exposure. Older adults, migrants, and low-income groups faced the greatest risk with limited protection.
-
Exclusionary health systems and digital divides. Health systems often lacked ageing and migrant-sensitive services, and unequal digital access worsened inequities.
-
Socioeconomic precarity, job losses, informal work, and weak social protection eroded human capital.
-
Fragmented policy responses. Post-pandemic strategies rarely integrated ageing, migration, and poverty, creating blind spots in design.
Comparative analysis showed these gaps were most severe in the Global South, where social protection and health infrastructure remain weak.
The Ghana Africa Lens and Why It Matters
Although global in scope, the review is deeply relevant to Ghana and similar contexts. Ageing, migration, and economic disparities intersect sharply across rural-urban divides and informal economies. Older migrants and rural elders often lack pensions, insurance, or digital access. Integrating these realities bridges global evidence with local policy relevance.
Policy Implications Beyond Health Care
Health equity cannot be achieved through clinical reforms alone. We recommend
-
Age and migrant-inclusive health system design
-
Comprehensive social protection coverage for informal and cross-border workers
-
Bridging the digital divide in healthcare access
-
Institutionalising intersectional policy design across ministries and agencies
Why the Timing Matters
Published in November 2025, this paper arrives as the world rebuilds from COVID-19. Without embedding ageing and migration into recovery strategies, cycles of cumulative disadvantage will persist. Our review aims to inform that global reckoning.
Personal Motivation and Ethical Imperative
For us as Ghanaian scholars, this study transcends academia and represents an ethical duty. Older adults, migrants, and low-income persons remain invisible in many policies. We sought to make their experiences visible and call for governance that upholds dignity and inclusion across Africa and the Global South.
Conclusion
This paper bridges divides between ageing and migration studies, health policy and social protection, and research and justice. We hope to advance a conversation where no older migrant is left behind and no low-income community is forgotten in future crises.
Follow the Topic
-
International Journal for Equity in Health
This journal presents evidence relevant to the search for, and attainment of, equity in health across and within countries and publishes research which improves the understanding of issues that influence the distribution of health and healthcare within populations.
Related Collections
With Collections, you can get published faster and increase your visibility.
Migration and its effects on maternal and child health and nutrition
International Journal for Equity in Health is hosting a cross-journal Collection in collaboration with the Journal of Health, Population and Nutrition.
This cross-journal Collection is seeking contributions showcasing research on the intersection of migration and maternal and child health and nutrition. Both forced and voluntary migration have become a global phenomenon with profound implications for mothers' and children’s health, nutrition, and overall well-being. This special edition will highlight diverse methodological approaches, including qualitative, quantitative, and mixed-methods studies, that contribute to a deeper understanding of health inequities among migrant populations and offer potential solutions to mitigate them.
This special issue aims to bridge gaps in the evidence base and promote research incorporating diverse disciplinary perspectives and methodological synergies. We welcome theoretical, review, and empirical contributions that enhance our understanding of the complex social, political, economic, and cultural determinants shaping the health of migrant women and children. In addition to the mentioned methodologies, several others can be incorporated to strengthen this research. Participatory and community-based methods, such as participatory action research (PAR), involve affected communities in all stages of the research process, ensuring relevance and applicability. Qualitative and ethnographic approaches, including in-depth interviews and focus groups, provide a deeper understanding of the cultural and social contexts influencing health. Longitudinal studies track health outcomes over time, offering insights into the long-term effects of migration. An intersectional approach considers how multiple identity factors intersect and affect health. Social network analysis explores the role of social connections in accessing healthcare and resources. Policy analysis methods assess how national and international policies impact migrant health, while big data and spatial analysis reveal trends across different regions and contexts. We encourage submissions that engage with affected communities, apply innovative methodological frameworks, and inform policy and practice.
Submissions may include, but are not limited to, the following areas:
Health disparities in migrant populations:
- Examining health inequities affecting migrant mothers and children.
- Identifying key determinants of health disparities in various migration contexts.
Nutritional challenges and interventions:
- Assessing the nutritional status of migrant mothers and children.
- Evaluating policies, interventions, and strategies aimed at addressing nutritional challenges among migrant populations.
Impact of migration policies:
- Analyzing how migration policies influence maternal and child health outcomes.
- Investigating the role of legal frameworks in shaping access to healthcare and nutrition for migrant populations.
Psychosocial well-being:
- Exploring the psychosocial effects of migration on maternal and child health.
- Assessing the role of social support systems in mitigating mental health challenges.
Community health and resilience:
- Investigating community-based approaches to improve the health and resilience of migrant populations.
- Understanding the role of cultural adaptation and integration in health outcomes.
Health systems and access to care:
- Examining how health systems address the needs of migrant mothers and children.
-Identifying innovative approaches to enhance healthcare accessibility and equity for migrant populations.
This Collection supports and amplifies research related to SDG 5, Gender Equality.
This collection is open for submissions from all authors on the condition that the manuscript falls within both the scope of the collection and the journal it is submitted to.
All submissions in this collection undergo the relevant journal’s standard peer review process. Similarly, all manuscripts authored by a Guest Editor(s) will be handled by the Editor-in-Chief of the relevant journal. As an open access publication, participating journals levy an article processing fee (International Journal for Equity in Health, Journal of Health, Population and Nutrition). We recognize that many key stakeholders may not have access to such resources and are committed to supporting participation in this issue wherever resources are a barrier. For more information about what support may be available, please visit OA funding and support, or email OAfundingpolicy@springernature.com or the Editor-in-Chief of the journal where the article is being submitted.
Publishing Model: Open Access
Deadline: Jul 31, 2026
Racism and Health
The ongoing advancement of our understanding of how racism impacts health - both directly and structurally - is crucial for addressing the deep-rooted health inequities that persist globally. Structural racism shapes health outcomes among racialized populations, contributing to inequities in healthcare access and quality, and impacting social, political, or environmental determinants of health. Existing research also connects direct and visible manifestations of racism, such as major and everyday discrimination, to negative health outcomes. At the same time, racism does not operate in isolation. A growing body of research shows how it intersects with other systems of oppression—such as classism and patriarchy—and with broader social determinants of health, producing compounded and context-specific inequities. An intersectional lens is therefore essential to understand how overlapping structures of power and exclusion shape health and healthcare experiences. These insights are essential in conducting rigorous and thorough health research, guiding anti-racist health policy, and ultimately, ensuring equitable health for all.
Looking forward, research holds the potential to develop new methodologies and indices and unveil complexities in how racism manifests within healthcare systems and societal structures. By deepening our collective understanding, we can develop more effective interventions that target the root causes of health inequities.
We invite researchers to contribute to this special Collection on Racism and Health, focusing on advancing our understanding and addressing health inequities. Topics of interest include but are not limited to:
- Racism as a structural determinant of health
- Racism as a direct determinant of health
- Racialized health outcomes in different populations
- Intersectionality and inequities in health, healthcare access and quality
- Nexuses between social, political, and environmental determinants of health and systemic discrimination
- Anti-racist health policy frameworks and systems
- Impact of racism on mental health
- Health inequities in reproductive, maternal, and child health
- Obstetric and reproductive violence
- Community-based interventions for equitable health
- Decolonizing health research and global health epistemologies
We strongly encourage contributions from racialized scholars and authors with lived experience or expertise in addressing systemic discrimination in health research.
This Collection supports and amplifies research related to SDG 3, Good Health and Well-Being and SDG 10, Reduced Inequalities.
All submissions in this collection undergo the journal’s standard peer review process. Similarly, all manuscripts authored by a Guest Editor(s) will be handled by the Editor-in-Chief. As an open access publication, this journal levies an article processing fee (details here). We recognize that many key stakeholders may not have access to such resources and are committed to supporting participation in this issue wherever resources are a barrier. For more information about what support may be available, please visit OA funding and support, or email OAfundingpolicy@springernature.com or the Editor-in-Chief.
Publishing Model: Open Access
Deadline: Aug 14, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in
Thank you, Yuanxin, for engaging with my post and for the work you do in building scholarly connections across the Springer Nature Research Communities. I truly appreciate the visibility this platform gives to early career researchers and the spirit of collaboration it fosters across disciplines.
Thank you for your contribution and I'm glad you like the Communities. Here is the Welcome course which can help you discover how to make the most of the Communities: https://communities.springernature.com/courses/1964