Exploring the Relationship Between Blood Glucose and the Menstrual Cycle
Published in Healthcare & Nursing, Bioengineering & Biotechnology, and General & Internal Medicine
Summary
In this study, we examined the relationship between blood glucose levels and the menstrual cycle using continuous glucose monitoring and daily hormone testing. The results demonstrated that glucose levels fluctuate throughout the menstrual cycle, with an increase in the luteal phase and a decrease in the late-follicular phase. The study suggests that blood glucose could be a significant factor in understanding menstrual health and warrants further investigation.
Context
Blood glucose levels can vary due to various factors, including body composition, diet, and exercise. Understanding these fluctuations is important for maintaining a healthy lifestyle as they can reveal or mask indicators of health problems like diabetes and vascular diseases. People who menstruate are particularly vulnerable to these issues due to hormonal imbalances, especially during life events such as pregnancy and menopause. Although the exact mechanisms are unclear, changes in estrogen levels throughout the menstrual cycle are believed to be involved. Therefore, studying glucose levels in non-diabetic menstruating individuals can further our understanding of glucose variation in relation to hormonal levels and management in pathological conditions.
Designing the Study
Previous studies had incongruent findings, potentially due to limited blood draws and reliance on self-reported menstrual cycles. To address these limitations, we conducted a study utilizing continuous glucose monitoring and daily hormone testing for more accurate and reliable data collection. The study involved 49 participants who wore a Dexcom G6 continuous glucose monitor and a Fitbit Sense smartwatch for an average of 79.3 ± 21.2 days. They also provided daily self-reports on their menstrual cycle characteristics and underwent daily hormone tests to determine their menstrual cycle phase.
Study Results
Our findings indicate that glucose levels peaked during the luteal phase, which follows ovulation, and reached a minimum during the late-follicular phase, which follows menstruation. These biphasic patterns remained consistent even after accounting for participant characteristics like age, BMI, and weight, and self-reported menstrual experiences like food cravings, bloating, and fatigue. We also discovered several other associations, such as lower glucose levels being linked to higher daily estrogen levels, increased step count, reduced fatigue, and vice versa. Moreover, higher levels of food cravings were positively associated with elevated median glucose levels.
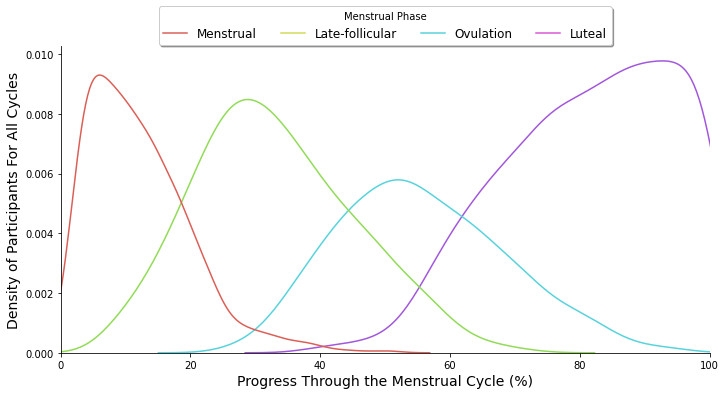
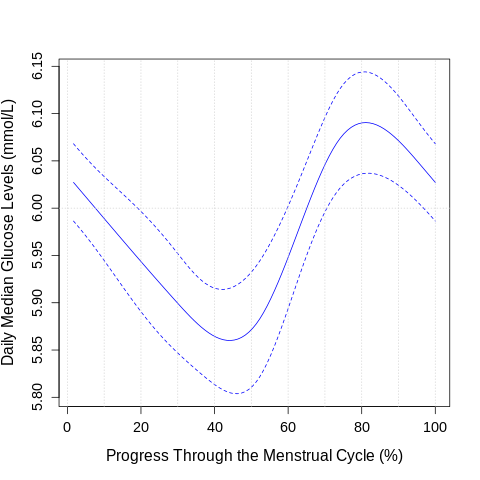
Implications for Menstrual Health
Our study holds significant implications for menstrual health in several ways. First, understanding the connection between blood glucose levels and the menstrual cycle enables individuals to interpret their glucose data more effectively. Moreover, the observed biphasic pattern suggests that blood glucose could potentially be used as an indicator for menstrual phase prediction. By integrating blood glucose monitoring and hormone tracking into wearable devices, we could enhance monitoring capabilities and facilitate trend identification.
Continuing the Research
To ensure a more representative sample, future research should focus on expanding the demographic variation of participants. Additionally, incorporating clinical tests to determine menstrual cycle phases and including objective measures like sleep trackers would strengthen and complement the findings. Furthermore, efforts towards developing user-friendly visualizations and applications that integrate data from multiple devices would enhance our understanding of various physiological trends during the menstrual cycle.
Follow the Topic
-
npj Digital Medicine

An online open-access journal dedicated to publishing research in all aspects of digital medicine, including the clinical application and implementation of digital and mobile technologies, virtual healthcare, and novel applications of artificial intelligence and informatics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Evaluating the Real-World Clinical Performance of AI
Publishing Model: Open Access
Deadline: Jun 03, 2026
Impact of Agentic AI on Care Delivery
Publishing Model: Open Access
Deadline: Jul 12, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in