 SpringerLink
SpringerLink
Femoral neck version in the spinopelvic and lower limb 3D alignment: a full-body EOS® study in 400 healthy subjects - European Spine Journal
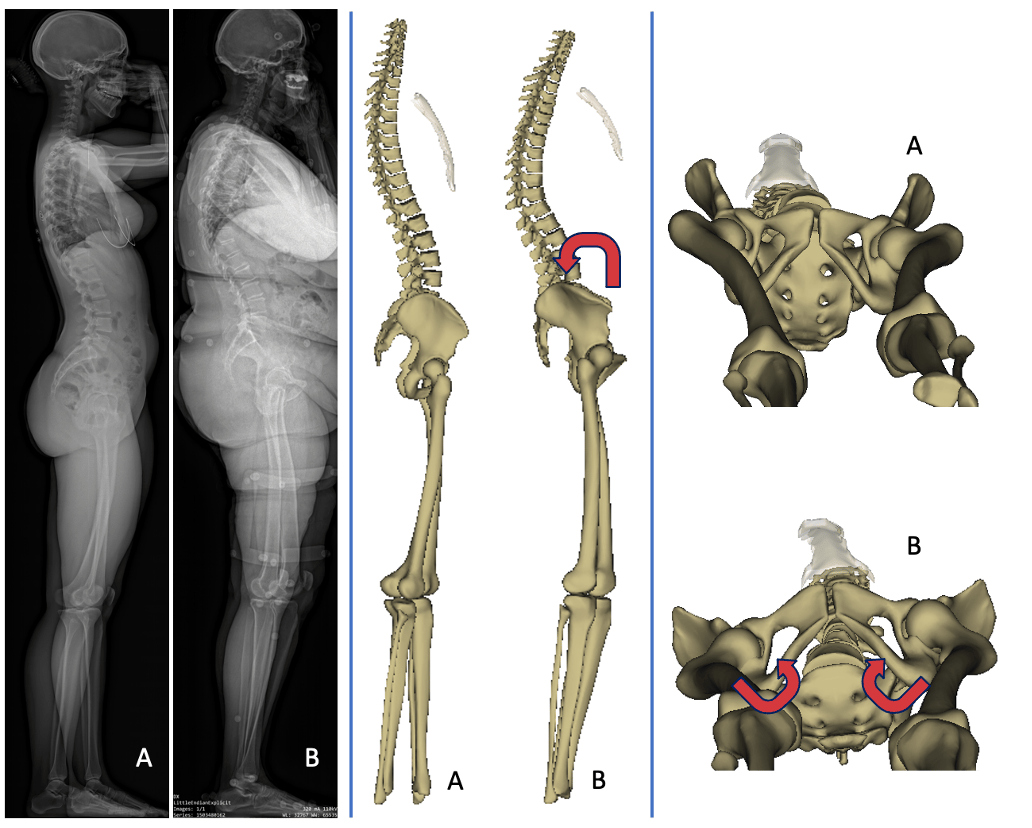
Background The goal of this study was to better understand the variation of femoral neck version according to spinopelvic and lower limb 3D alignment using biplanar X-rays in standing position. Methods This multicentric study retrospectively included healthy subjects from previous studies who had free-standing position biplanar radiographs. Subjects were excluded if they presented spinal or any musculo-skeletal deformity, and reported pain in the spine, hip or knee. Age, sex, and the following 3D-reconstructed parameters were collected: spinal curvatures, pelvic parameters, sagittal vertical axis (SVA), T1 pelvic angle (TPA), spino-sacral angle (SSA), femoral torsion angle (FTA), sacro-femoral angle (SFA), knee flexion angle (KA), ankle angle (AA), pelvic shift (PS) and ankle distance. Femoral neck version angle (FVA) was calculated between horizontal plane projection of the bi-coxo-femoral axis and the line passing through the femoral neck barycenter and femoral head center. Analysis according to age subsets was performed. Results A total of 400 subjects were included (219 females); mean age was 29 ± 18 years (range: 4–83). Subjects with high pelvic tilt values presented significantly higher FVA than average and low-PT individuals, respectively, 7.8 ± 7.1°, 2 ± 9° and 2.1 ± 9.5° (p < 0.001). These subjects also presented lower lumbar lordosis values and higher acetabulum anteversion in the horizontal plane than the two other groups. SVA correlation with FVA was weaker (r = 0.1, p = 0.03) than SSA and TPA (r = − 0.3 and r = 0.3, respectively, p < 0.001). A strong correlation was found with femoral torsion (r = 0.5, p < 0.001). SFA (r = − 0.3, p < 0.001), pelvic shift (r = 0.2, p < 0.001) and ankle distance (r = 0.3, p < 0.001) were also significantly correlated. Multivariate analysis confirmed significant association of age, pelvic tilt, lumbar lordosis, pelvic shift, ankle distance and femoral torsion with FVA. Conclusion Patients with lower lumbar lordosis present pelvic retroversion which induces a higher femoral neck version. This finding may help positioning implants in total hip replacement procedures. Higher pelvic shift, age, male gender and increased femoral torsion were also correlated with higher FVA. Level of evidence II (Diagnostic: individual cross-sectional studies with consistently applied reference standard and blinding).



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in