
Explore the Research
Adiposity, metabolites, and colorectal cancer risk: Mendelian randomization study
Obesity is viewed as a likely cause of colorectal cancer (CRC, also known as bowel cancer) [1], but still unclear is whether risk differs for men and women, and exactly how obesity biologically causes CRC. Using a sort of naturally occurring trial called Mendelian randomization [2], which uses genetic information to better understand causality of modifiable factors, we examined whether two different measures of obesity – namely body mass index (BMI) and waist-hip-ratio (WHR) were associated with CRC risk among men and women separately. We also investigated whether circulating metabolites, or small molecules in blood which capture metabolic processes, could explain these relationships [3]. These Mendelian randomization methods, when key assumptions are met, help to minimise issues of confounding and reverse causation which are common pitfalls of observational studies [2].

Obesity is viewed as an important risk factor for cancer by the World Cancer Research Fund (WCRF) https://www.wcrf-uk.org/uk/our-research/research-we-fund
As part of a collaboration between the International Agency for Research and Cancer (IARC) in France, the Fred Hutchinson Cancer Research Centre in the US, and the University of Bristol in the UK, we acquired summary statistics from three major consortia, including the Genetics of Epidemiology of Colorectal Cancer Consortium (GECCO), together describing the genotypes of over 100,000 individuals from 72 studies to better estimate the role of adiposity in CRC, separately by sex and anatomical sub-site (colon, proximal colon, distal colon and rectum). We used publicly available summary statistics describing the genetics of adiposity (BMI, WHR) and metabolites detected by targeted NMR spectroscopy. These metabolites included detailed lipid traits plus amino acids, fatty acids and inflammatory glycoproteins.
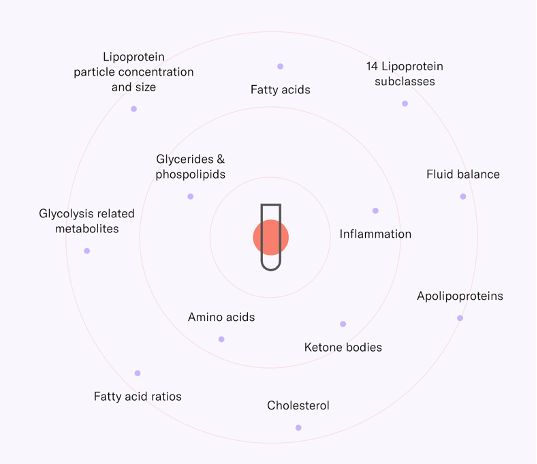
Metabolites detectable in blood using the Nightingale Health NMR panel https://nightingalehealth.com/research/blood-biomarker-analysis
Our results suggest that BMI and WHR associations do not differ substantially by CRC site, but do differ substantially by sex. Higher BMI is more strongly associated with CRC risk in men, whereas higher WHR is more strongly associated with CRC in women. This was surprising as BMI and WHR are highly correlated, and we hypothesise that this could be because women are more likely to store fat peripherally, meaning that WHR is better able to capture the extremes of adiposity in women.
A two-minute primer on Mendelian randomization
We explored potential mechanisms through which adiposity could influence CRC by examining metabolites as intermediate biomarkers. Despite examining over 100 metabolites from multiple biological subclasses, we did not identify any convincing metabolite-CRC associations which could explain the adipose-CRC relationship. Future studies using new and improved methodological techniques and exploring even more detailed metabolites, proteins, hormones, and inflammatory factors as potential mediators are needed to uncover the biological pathways between adiposity and CRC. This should be done among men and women separately given their markedly different risks from obesity. Understanding these pathways is more important than ever because of how common overweight and obesity are, and how difficult they are to reverse.
Read the paper here: https://rdcu.be/cclz2
References
- World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Expert Report. Diet, nutrition, physical activity and colorectal cancer. 2018.
- Davey Smith G, Ebrahim S. ‘Mendelian randomization’: can genetic epidemiology contribute to understanding environmental determinants of disease? Int J Epidemiol. 2003; 32(1): 1–22.
-
Bull CJ, Bell JA, Murphy N, et al. Adiposity, metabolites, and colorectal cancer risk: Mendelian randomization study. BMC Med. 2020; 18(1): 396.
Follow the Topic
-
BMC Medicine
This journal publishes outstanding and influential research in all areas of clinical practice, translational medicine, medical and health advances, public health, global health, policy, and general topics of interest to the biomedical and sociomedical professional communities.
Related Collections
With Collections, you can get published faster and increase your visibility.
Weight loss interventions and their health impacts
BMC Medicine is calling for submissions to our new Collection on weight loss interventions and their health impacts, emphasizing a variety of strategies, including dietary changes, physical activity, pharmacological treatments, and surgical options. We encourage submissions that explore the long-term effects of these interventions, adherence challenges, and strategies to address health inequities. The goal is to advance understanding and improve outcomes in weight management and overall health.
Weight loss interventions encompass a wide range of strategies aimed at reducing body weight and improving health outcomes. These interventions can include dietary changes, increased physical activity, pharmacological treatments, and surgical options such as bariatric surgery. As the global prevalence of obesity and related comorbidities continues to rise, understanding the efficacy and mechanisms of various weight loss interventions becomes increasingly crucial for public health. This Collection seeks to explore the diverse methodologies and outcomes associated with weight loss interventions, offering insights into their impacts on both individual and population health.
The significance of this research is underscored by the growing body of evidence linking obesity to numerous chronic health conditions, including diabetes, cardiovascular diseases, and certain types of cancer. Advances in pharmacological treatments, such as SGLT2 inhibitors and GLP-1 agonists, have emerged as promising options for weight management, demonstrating not only weight loss but also improved metabolic health. There are, however, challenges and limitations related to drug availability, healthcare delivery, and long-term treatment adherence with rapid weight gain when stopping treatment. Additionally, integrating behavioral strategies with nutritional and physical activity interventions has shown potential in enhancing adherence and long-term success. By further investigating these modalities, we can develop comprehensive approaches that address the multifactorial nature of obesity.
Continued research in this domain may yield innovative strategies that harness technology, such as mobile health applications and telehealth, to support weight loss interventions. As we deepen our understanding of the genetic, environmental, and behavioral factors influencing obesity, personalized interventions tailored to individual needs could emerge. This progress may lead to improved health outcomes, reduced health inequities, and ultimately a shift in the paradigm of obesity treatment and prevention.
We are looking for original manuscripts on topics including, but not limited to:
•Clinical trials investigating interventions for weight loss to promote health
•Real-world data on long-term effects and challenges of weight loss interventions
•Factors affecting long-term adherence to weight-loss or weight maintenance interventions
•Challenges and inequities in access to weight loss interventions
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being.
Publishing Model: Open Access
Deadline: May 07, 2026
Palliative care and medicine
BMC Medicine is calling for submissions to our new Collection, Palliative care and medicine, focused on the growing body of knowledge in end-of-life care. Palliative care is an essential component of healthcare that focuses on improving the quality of life for patients with serious, life-limiting illnesses. This specialized approach addresses not only physical symptoms but also psychological and social needs, emphasizing a holistic perspective on patient care. As the global population ages and the prevalence of chronic conditions rises, the demand for effective palliative care services is more critical than ever. This Collection aims to gather research that explores innovative practices, challenges, and advances in palliative care.
Advances in this field of palliative care have led to improved pain and symptom management techniques, enhanced communication strategies, and the integration of these initiatives into standard treatment protocols for various diseases. Additionally, there has been a growing recognition of the importance of advance care planning and bereavement support, which are crucial for ensuring that patients and their communities receive comprehensive care aligned with their values and preferences.
As research in palliative care continues to evolve, we may see the emergence of innovative models of care that integrate technology, such as telehealth solutions, to expand access and enhance patient engagement. Future studies may also focus on the development of personalized care plans that address the unique needs of diverse populations, ensuring that palliative care is equitable and inclusive. This ongoing exploration has the potential to transform the landscape of end-of-life care, ultimately improving the quality of life for patients and their communities.
Topics of interest include but are not limited to:
•Innovations in pain management in palliative care
•Advance care planning and its impact on quality of life
•Novel models for palliative and hospice care
•Bereavement support for families
•Addressing frailty in geriatric palliative care
•Palliative care in low-income and middle-income countries
•New technologies and big data for palliative care
•Access to palliative care medications
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
Publishing Model: Open Access
Deadline: May 07, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in