Patient-derived xenograft models confirm the early seeding and recapitulate the evolution of Richter transformation
Published in Cancer and Protocols & Methods

The problem
Somatic changes in genes that suppress tumors, regulators on cell cycle and support cell growth (i.e., mutations or alterations of TP53, NOTCH1, MYC and CDKN2A/B) are commonly found in RT cells [1]. However, RT research requires models that replicate the biology observed in patients to achieve a thorough understanding of the disease. In addition, new development and testing of new treatments is necessary considering the dismal prognosis of patients with RT with current therapeutic options.
The patient-derived xenograft (PDX) system is widely used for solid tumors because it reproduces the development of tumors through repeated growth in mice. PDX models also reflect the diversity between patients. However, engrafting these tumors in mice has been a major challenge when it comes from hematological malignancies. Few PDXs have been created so far, which all come from RT original samples [2]. This creates an opportunity to generate new PDXs and assess novel therapeutic strategies based on the specific mutational profiles of the tumors.
The research
We generated two new PDXs, one of which was, for the first time, originated from a CLL sample and developed to a RT mimicking the evolution observed in the patient. This PDX model thus confirms the evolutionary framework of RT characterized by an early seeding of transformed cells. PDX models were created by injecting peripheral blood mononuclear cells into immunodeficient mice with autologous T cells to aid in tumor engraftment. Genomic and morphological studies on several passages confirmed that the two PDXs were RT clonally related to the original sample (Fig.1 [yellow]).
We tracked the subclonal evolution of the PDXs by whole-genome sequencing and RNA sequencing and compared them with the evolutionary trajectories observed in the patients. This analysis revealed a genomic progression in PDX similar to the parental samples. We also discovered here that the RT is clonally heterogeneous, that this heterogeneity in the pool of RT cells may be acquired also early during the evolution of CLL (i.e., years before their final manifestant), and that these distinct subclones compete along disease evolution (Fig.1 [blue]). Furthermore, the transcriptomic analysis found that RT cells have high levels of genes involved in energy production through oxidative phosphorylation (OXPHOS) and a downregulation of genes involved in the B-cell receptor pathway, which confers resistance to Bruton’s tyrosine kinase (BTK) inhibitors such as ibrutinib. Interestingly, one PDX was resistant to the BTK inhibitor even though the sample used to generate the PDX was never exposed to the drug (Fig.1 [red]), which suggests that this phenomena is intrinsic of (at least) some RT cells.
Previous studies have suggested that targeting OXPHOS in different types of tumors could be an effective treatment approach in different cancers [3], including in RT. Our experiments with the PDX models support this hypothesis. We found that OXPHOS inhibition through the use of IACS-010759 (a compound that inhibits complex I of the mitochondrial electron transport chain) reduced the growth of RT-PDX cells (Fig.1 [green]). Finally, we also discovered that when combining this OXPHOS inhibitor with an apoptotic drug, venetoclax, which blocks BCL2 protein and lead cells to apoptosis, we could overcome initial resistance to venetoclax, similarly to previous studies on acute myeloid leukemia [4].
The impact
Our PDX models confirmed that RT subclones are present early in the CLL phase of the disease and enables the study of this evolutionary process. While creating PDX models is difficult with low success rates, established models can still be an effective tool in assessing RT biology. The observed OXPHOShigh-BCRlow axis may contribute to the low response of RT patients to BTK inhibitors. In addition, we propose addressing OXPHOS using venetoclax to provide a new treatment option for RT patients with limited therapies and dismal prognosis.
This study also raises questions about the potential role of the tumor environment as we used mice with compromised immune system. However, these models might help to investigate new immunotherapies, such as immune checkpoints and CAR-T therapies, using patient's own T cells.
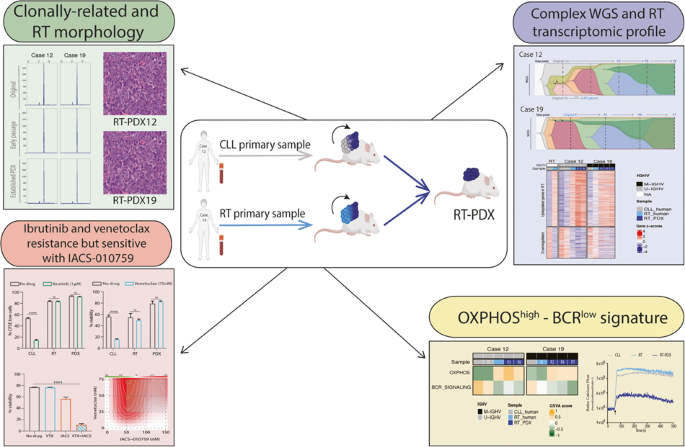
![Summary Figure 1. Two new PDX have been established, one of them came from an initial CLL sample which confirmed the idea of early seeding from RT cells. [yellow] Morphological and clonality studies were carried out to establish that both PDXs are RT and come from the original clone. [blue] Genomic and transcriptomic characterization confirmed the evolution to RT. [red] In vitro studies confirmed the OXPHOShigh-BCRlow axis. [green] The new in vivo model was used to test new therapeutic strategies.](https://images.zapnito.com/cdn-cgi/image/metadata=copyright,fit=scale-down,format=auto,quality=95/https://images.zapnito.com/uploads/HzainxsbQWKRy6GbYNjd_picture1.png)
Figure 1. Two new PDX have been established, one of them came from an initial CLL sample which confirmed the idea of early seeding from RT cells. [yellow] Morphological and clonality studies were carried out to establish that both PDXs are RT and come from the original clone. [blue] Genomic and transcriptomic characterization confirmed the evolution to RT. [red] In vitro studies confirmed the OXPHOShigh-BCRlow axis. [green] The new in vivo model was used to test new therapeutic strategies.
References
- Nadeu F, Royo R, Massoni-Badosa R, Playa-Albinyana H, Garcia-Torre B, Duran-Ferrer M, et al. Detection of early seeding of Richter transformation in chronic lymphocytic leukemia. Nat Med. 2022;28:1662–71.
- Vaisitti T, Braggio E, Allan JN, Arruga F, Serra S, Zamò A, et al. Novel Richter Syndrome Xenograft Models to Study Genetic Architecture, Biology, and Therapy Responses. Cancer Res. 2018;78:3413–20.
- Molina JR, Sun Y, Protopopova M, Gera S, Bandi M, Bristow C, et al. An inhibitor of oxidative phosphorylation exploits cancer vulnerability. Nat Med. 2018;24:1036–46.
- Bosc C, Saland E, Bousard A, Gadaud N, Sabatier M, Cognet G, et al. Mitochondrial inhibitors circumvent adaptive resistance to venetoclax and cytarabine combination therapy in acute myeloid leukemia. Nat Cancer. 2021;2:1204–23.
Follow the Topic
-
Leukemia
This journal publishes high quality, peer reviewed research that covers all aspects of the research and treatment of leukemia and allied diseases. Topics of interest include oncogenes, growth factors, stem cells, leukemia genomics, cell cycle, signal transduction and molecular targets for therapy.



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in