Spousal Age Gaps and Women’s Contraceptive Use in Sub-Saharan Africa
Published in Social Sciences

What is a spousal age gap and why does it matter?
Spousal age gap refers the difference in age between a husband and wife. It is calculated by finding the difference between husband and wife’s age which means that higher the difference in terms of age between the husband and wife, the wider the gap between their ages.
Wider spousal age gaps between partners have been linked to a higher risk of intimate partner violence and of engaging in risky sexual behaviours, such as unprotected sex and having multiple concurrent partners. These risks are attributed to the power imbalance in relationships where women are much younger than their spouses.
Study background
In our study, we examined the relationship between spousal age difference and the likelihood of using contraception. The analysis used Demographic and Health Survey data from 29 sub-Saharan African countries. The surveys spanned a 24-year period from 1999 to 2022.
Key findings
Spousal age difference and contraceptive use
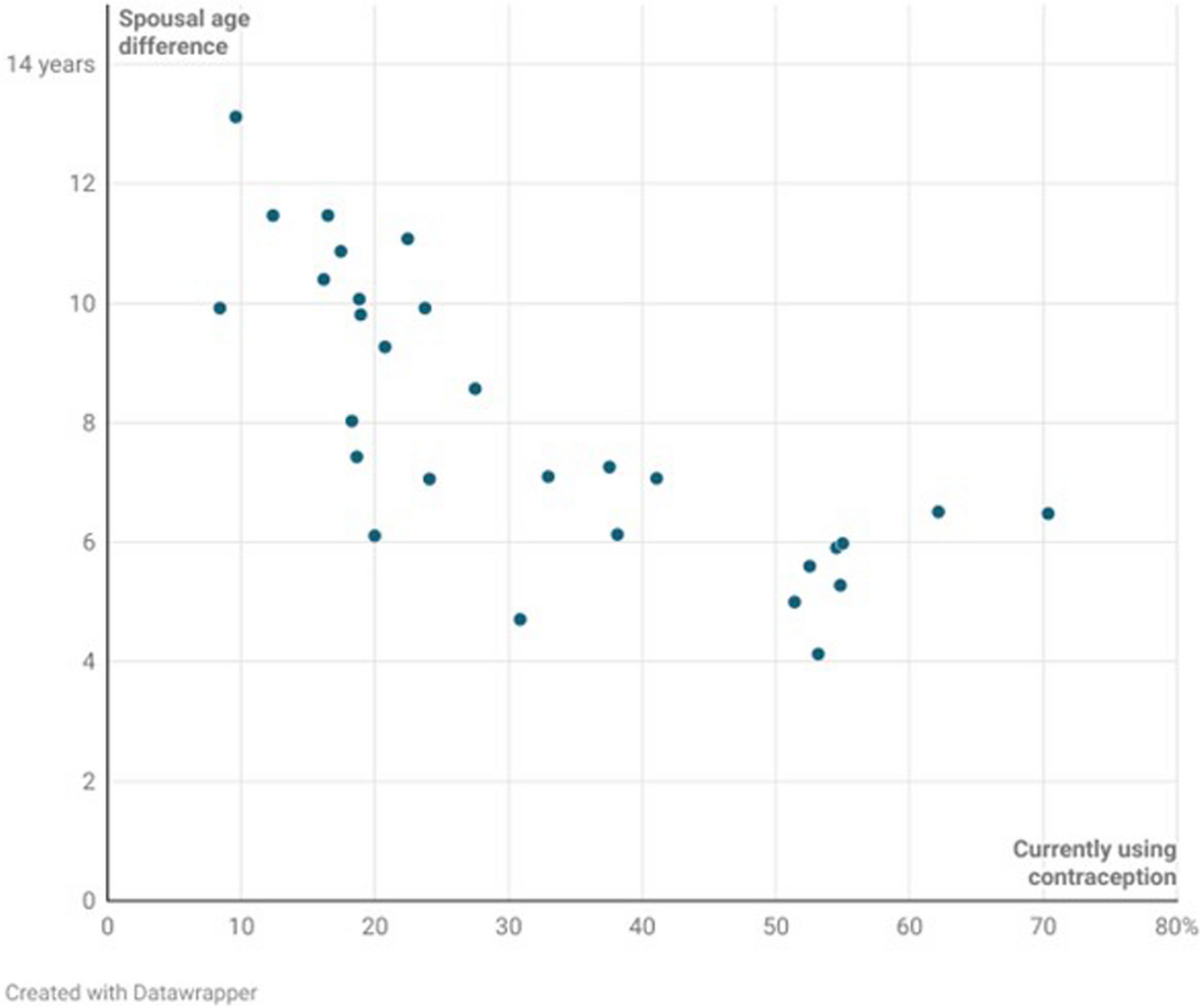
For women who do not use contraception, their husbands are, on average, about 9.1 years older than them. This age gap is about 2.5 years larger than the 6.7-year difference seen in women who do use contraception. This means that women with older husbands are less likely to use birth control than those with husbands whose husbands are closer in age. This might be because younger men are more likely to use contraceptives than older men.
A one-year increase in the spousal age difference between spouses is linked to a 1.1 per cent decrease in the chances of using contraception, a statistically significant likelihood. A comparison of this relationship across marriage cohorts reveals that the relationship between spousal age difference and contraceptive use has largely remained unchanged over time.
Cross-national differences
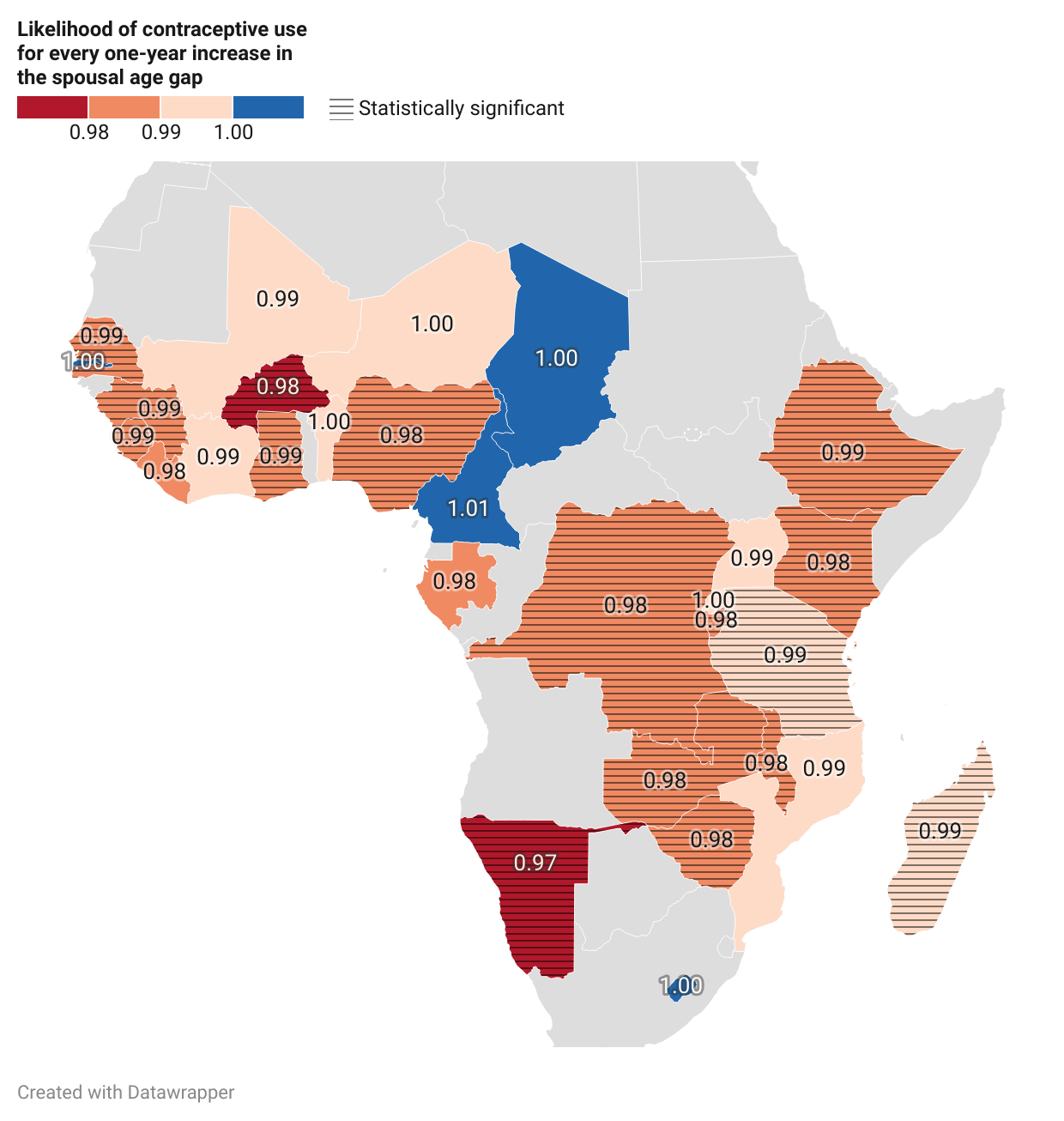
The results show that the link between the age difference of spouses and contraceptive use varies from country to country. This means that having a big age gap between spouses does not always negatively affect contraceptive use.
Implications
This study confirms that relationships with large age gaps can have negative effects. One reason is that in these marriages, the older spouse often has more power, which affects contraceptive use. However, when women have better education and more say in healthcare decisions, the impact of age differences on contraceptive use is lessened. This suggests that empowering women can help reduce the negative effects of larger spousal age differences on their health.
However, the results vary across countries when it comes to the relationship between the age difference of spouses and contraceptive use. In countries where a larger age gap does have a negative association, there are differences in location, how common contraceptive use is, and the average age difference between spouses. This highlights a need for further research to understand how cultural beliefs, gender roles, and broader social factors might affect the relationship between spousal age gaps and contraceptive use.
References
Bajunirwe F, Semakula D, Izudi J. Risk of HIV infection among adolescent girls and young women in age-disparate relationships in sub-Saharan Africa. AIDS. 2020 Aug 1;34(10):1539-48.
Jewkes RK, Dunkle K, Nduna M, Shai N. Intimate partner violence, relationship power inequity, and incidence of HIV infection in young women in South Africa: a cohort study. The lancet. 2010 Jul 3;376(9734):41-8.
Stein CR, Kaufman JS, Ford CA, Feldblum PJ, Leone PA, Miller WC. Partner age difference and prevalence of chlamydial infection among young adult women. Sexually Transmitted Diseases. 2008 May 1:447-52.
Follow the Topic
-
Contraception and Reproductive Medicine
This journal is designed to promote the advancement of contraceptive technology and general reproductive medicine particularly in the areas of education, effectiveness, safety, research interest, improved or new technologies, non-contraceptive benefits, and long-term health.
Related Collections
With Collections, you can get published faster and increase your visibility.
Breaking Barriers: Users’ Perceptions, Preferences, and Access to Long‑Acting Reversible Contraception (LARC)
Long-Acting Reversible Contraception (LARC) is increasingly recognized as a vital component of reproductive health, yet the experiences of those who use or desire to use LARCs remained shaped by a range of challenges. This Collection seeks to explore the nuanced barriers and biases that affect the uptake, continued use, and discontinuation of LARC methods, including intrauterine devices (IUDs) and implants. Understanding these dynamics is crucial for enhancing the reproductive autonomy of individuals across diverse populations, particularly in the context of structural inequities that may disproportionately affect marginalized groups.
The relevance of this research extends beyond individual choice; it impacts public health, community well-being, and the advancement of reproductive rights. Recent developments have underscored the importance of person-centered care in improving user experiences with LARC and in addressing provider-related factors that can inhibit informed decision-making, both for initiating and discontinuing methods. As healthcare systems evolve, there is a pressing need to evaluate how these factors intersect and influence LARC accessibility, especially as new contraceptive options and educational resources become available.
Continued exploration in this field may yield innovative strategies to dismantle barriers to accessing LARC initiation or discontinuation, fostering improved provider‑patient communication and ultimately enhancing user satisfaction and increasing alignment with user preferences. Future research could lead to the creation of targeted interventions that not only educate potential users about LARC options but also empower them to navigate existing healthcare structures confidently.
In this Collection, we invite submissions covering a range of topics, including but not limited to:
- Understanding structural inequities in LARC access
- Understanding structural inequities in LARC removal
- Understanding the impact of the reduction in official development assistance (ODA) on LARC service provision
- Provider biases and their impact on contraceptive choice
- Enhancing reproductive autonomy through understanding user preferences around LARC methods
- Person-centered care approaches in contraceptive counseling
- LARC manufacturing, supply-side bottlenecks and market-shaping constraints
This Collection supports and amplifies research related to SDG 3, Good Health and Well-Being.
All submissions in this Collection undergo the journal’s standard peer review process. Similarly, all manuscripts authored by a Guest Editor(s) will be handled by the Editor-in-Chief. As an open access publication, this journal levies an article processing fee. We recognize that many key stakeholders may not have access to such resources and are committed to supporting participation in this issue wherever resources are a barrier. For more information about what support may be available, please visit OA funding and support, or email OAfundingpolicy@springernature.com or the Editor-in-Chief.
Publishing Model: Open Access
Deadline: Dec 16, 2026
Reviews of Contraception in Healthcare
In this collection, we welcome reviews covering a range of topics related to contraception in health care including:
• Contraceptive failure: Global Perspectives.
• Access and information regarding contraception in rural areas
• Contraceptive methods in adolescence.
• Contraception in young women.
• Contraceptive use during the menopausal transition.
• Contraceptive methods, demands and future development.
• Contraception Selection, Effectiveness, and Adverse Effects.
• Long-Acting Reversible Contraception.
• Safety and Efficacy of Intrauterine devices.
• Hormonal and natural contraceptives: on efficacy and risks of different methods for an informed choice.
• Emergency contraception.
• Postpartum contraception.
• Contraceptive use among women with medical conditions: Factors that influence method choice.
• Contraceptive options for women living with HIV.
• Contraceptive Strategies in Women with Heart Failure or With Cardiac Transplantation.
• Male contraceptive advances.
• Quality of contraceptive services.
This Collection supports and amplifies research related to SDG 3, Good Health and Well-Being.
Publishing Model: Open Access
Deadline: Jul 24, 2026


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in