Turning the tables on gammaherpesviruses to make vaccines.
Published in Bioengineering & Biotechnology, Microbiology, and Pharmacy & Pharmacology
Problem: human gammaherpesviruses cause numerous cancers.
Epstein-Barr virus (EBV) is a ubiquitous virus that infects almost all adults around the world. This virus lurks predominantly in B cells using an immunologically silent gene expression program known as latency. When the virus reawakens, new virus particles are produced and infect new cells to drive a proliferative process that bypasses normal checkpoints. EBV is the cause of numerous types of lymphomas, as well as epithelial cell-derived cancers. Recently, EBV infection was also linked to multiple sclerosis.
Kaposi sarcoma herpesvirus (KSHV) also lays low in B cells and, while infections may be less prevalent in high income countries, KSHV is endemic in some regions of the world such as sub-Saharan Africa. The HIV/AIDS epidemic led to the discovery that KSHV infection is common in men who have sex with men. Even in the modern era, with drugs that are effective at controlling HIV and restoring normal CD4 T cell levels, people living with HIV who are also infected with KSHV are at much higher risk of B cell lymphoma, the endothelial cell cancer Kaposi sarcoma, and an inflammatory cytokine syndrome.
A weakened immune system in an individual effectively removes the brakes on the latency program of these viruses, and the risk of virus-driven cancers skyrockets. While many vaccine approaches are in development, no licensed gammaherpesvirus vaccines for humans exist, and the field does not yet understand what vaccine-induced immune responses are needed to control latent versus lytic infections.
The study in brief.
Over the years, our groups have aimed to understand how gammaherpesviruses colonize their host and promote cancer. Since EBV and KSHV do not infect small animals, we use a closely related gammaherpesvirus that naturally infects rodents such as mice as a model pathogen system. The goals of our research are to identify how this mouse virus subverts the host checkpoints and defenses to replicate in some tissues and then find its way to cell types where it lies dormant as a latent infection.
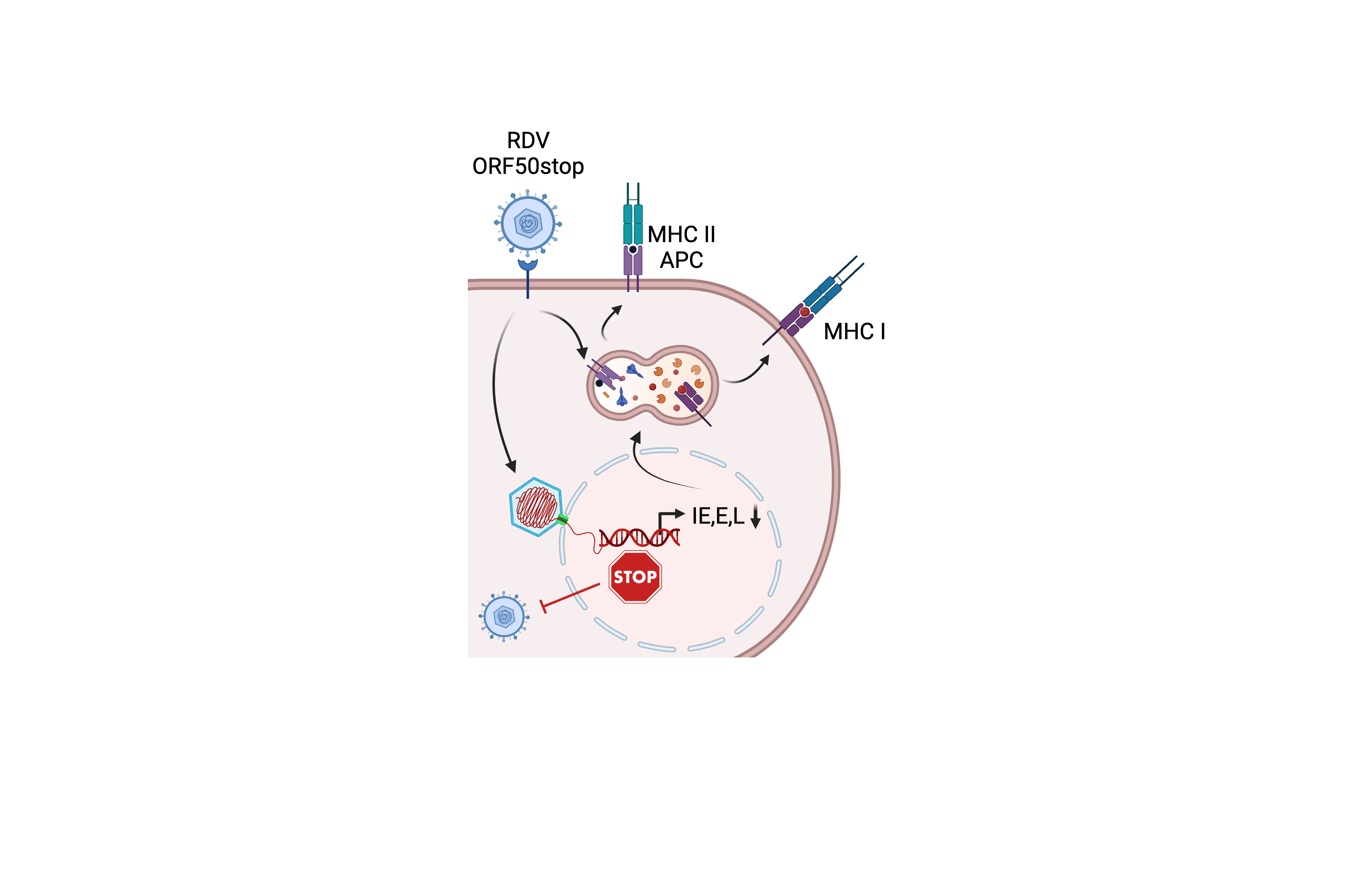
In this study, we turned the tables on the mouse gammaherpesvirus. We generated a mutant virus that could not produce an essential gene. This virus is structurally identical to wild-type virus but is unable to replicate. We asked whether multiple administrations of this replication-incompetent virus could generate neutralizing antibodies and virus-specific effector CD8 T cell responses; the answer was ->YES. Is the response long-lasting, -> YES. Does the vaccine protect against lytic replication of the wild-type challenge virus, -> YES. Does the vaccine protect against lytic disease in mice that cannot control lytic replication, -> YES. Next, we asked if this replication-defective vaccine protected better than a traditional heat-inactivated virus vaccine, -> YES.
However, our study also revealed some potential complications in the replication-defective virus vaccine strategy that reflect the sobering prowess of this family of viruses. Even though the vaccine virus was unable to replicate, it established latency - likely via direct infection of B cells. In future studies, we will knock-out genes required for viral latency to determine if a vaccine needs to be maintained long-term to provide durable protection.
Another potential shortcoming revealed by our study is that the replication-defective vaccine did not provide sterilizing immunity. The wild-type virus used in challenge experiments ultimately found its way to the lymphocyte reservoir. The ability of a herpesvirus to overcome such a strong vaccine-elicited immune defense suggests that therapeutic vaccines that boost or shape the immune response to control latency and prevent reactivation that drives lymphoproliferation and disease is a meritorious- and more feasible pursuit.
What challenges did we face?
How do you generate a broad immune response that blocks infection and controls replication? We banked on the antigenicity of the whole virion particle with the added spice of new viral gene expression in the cells to produce nascent viral proteins not present in the viral particle.
How do you make a stock of a virus that does not replicate? We produced the nonreplicating virus in a cell line expressing a ‘recoded’ version of the essential RTA protein, so the helper gene could not recombine with and repair the herpesvirus genome.
In the challenge experiment, was the virus that established latency the vaccine or the wild-type challenge? We used a PCR-based assay to detect all virus and then a different assay that amplified a molecular ‘scar’ in the vaccine virus to conclude that most of the breakthrough virus is wild-type.
Last, how do you show the vaccine protects against disease? The murine gammaherpesvirus that we use does not kill immune competent mice. However, IFNAR1-/- mice are unable to generate an interferon-driven antiviral response that is necessary to limit initial viral replication. These mice are more susceptible to the murine virus prior to viral recognition by the adaptive immune response. We vaccinated these mice with the replication-defective vaccine and protected these mice from a dose of wild-type virus that leads to severe illness and mortality.
Why is this research important?
EBV and KSHV are cancer-causing viruses. There is no vaccine and there is no drug that targets the ‘stealth’ latency program. We need to understand which components of the immune system are needed to block and control infection. This study using a closely related mouse gammaherpesvirus will promote further vaccine refinement to protect those at-risk from virus-driven cancers.
(figure created with BioRender.com)
Follow the Topic
-
npj Vaccines
A multidisciplinary journal that is dedicated to publishing the finest and high-quality research and development on human and veterinary vaccines.
Related Collections
With Collections, you can get published faster and increase your visibility.
Therapeutic HPV vaccines
Publishing Model: Open Access
Deadline: Jun 30, 2026
Lipid nanoparticle (LNP)-adjuvanted vaccines
Publishing Model: Open Access
Deadline: May 19, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in