When One Hand Acts on Its Own: A Stroke Presentation with Mixed Alien Hand Features
Published in Neuroscience and Biomedical Research
Explore the Research
Posterior alien hand syndrome in a patient with parieto-occipital infarction: a presentation mimicking anterior variant features—a case report
Case Summary
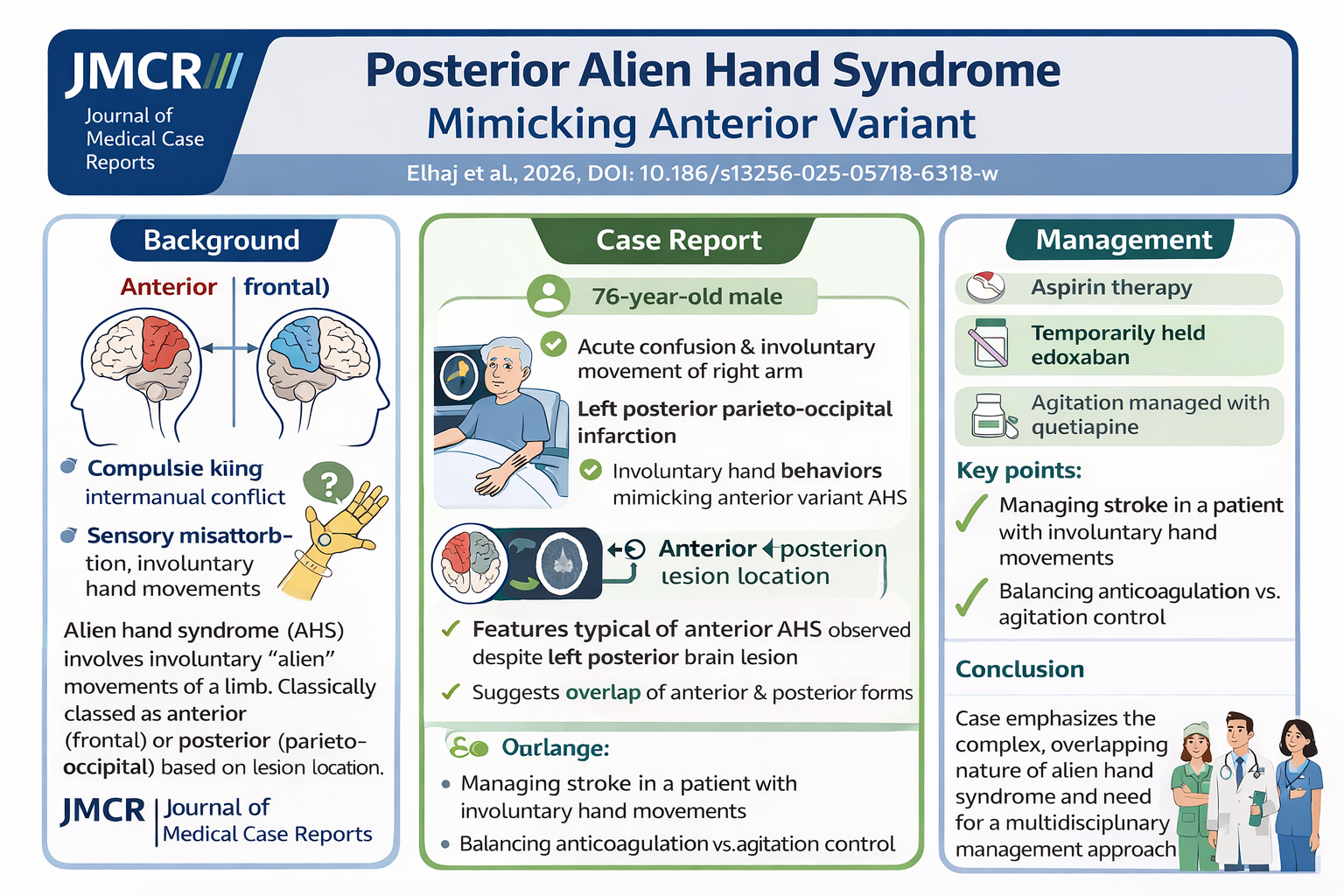
A 76-year-old man presented with acute confusion and involuntary movements of his right arm following a fall. Initial imaging was unrevealing, but rapid clinical progression prompted repeat imaging, which demonstrated a left posterior circulation infarction .
The patient developed classic features of alien hand syndrome—autonomous limb activity perceived as foreign—yet with a posterior lesion producing features typically associated with anterior variants. This diagnostic overlap is particularly instructive.
Management required careful balancing of competing priorities:
Acute stroke treatment with antiplatelet therapy
Temporary cessation and later reintroduction of anticoagulation
Symptom control of involuntary movements and agitation (quetiapine)
The case illustrates the complex interplay between neuroanatomy, behavior, and stroke management, especially in patients with competing thrombotic and hemorrhagic risks .
Why This Case Matters
This report challenges the traditional dichotomy of AHS into strictly anterior vs posterior forms. Instead, it supports a network-based model, where disconnection across distributed cortical and subcortical regions produces hybrid clinical phenotypes.
Key implications
AHS can evolve dynamically with lesion progression
Posterior lesions may produce “anterior-like” behavioral manifestations
Early imaging may be falsely reassuring—clinical evolution should drive repeat imaging
Clinical Pearl
Alien hand syndrome should be viewed as a network disconnection syndrome—not a strictly localization-bound entity.
Question
Which mechanism best explains alien hand syndrome?
A. Primary motor cortex hyperexcitability
B. Peripheral nerve hyperactivity
C. Disconnection between motor planning and execution networks
D. Basal ganglia dopamine deficiency
Correct Answer: C
Explanation:
Alien hand syndrome arises from disrupted integration between intention (frontal/parietal networks) and motor execution pathways, often due to lesions affecting interhemispheric or frontoparietal connectivity. This disconnection leads to goal-directed movements that are not perceived as self-generated.
Final Thoughts
This case reinforces a principle that remains as relevant today as ever: neurology is best understood through networks, not isolated lesions. As imaging advances, our clinical frameworks must evolve accordingly.
Journal of Medical Case Reports is the world’s first international, PubMed-listed, medical journal devoted to publishing case reports from all medical disciplines and will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports. The journal is open access, and strongly endorses the CARE guidelines for case reports, requiring authors to submit populated CARE checklists with submissions to improve transparency in reporting.
Follow the Topic
-
Journal of Medical Case Reports
This journal will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in