When Infection Triggers Stroke: Epstein–Barr Virus in a Young Adult with Acute Ischemic Stroke
Published in Neuroscience and Biomedical Research
Case Overview
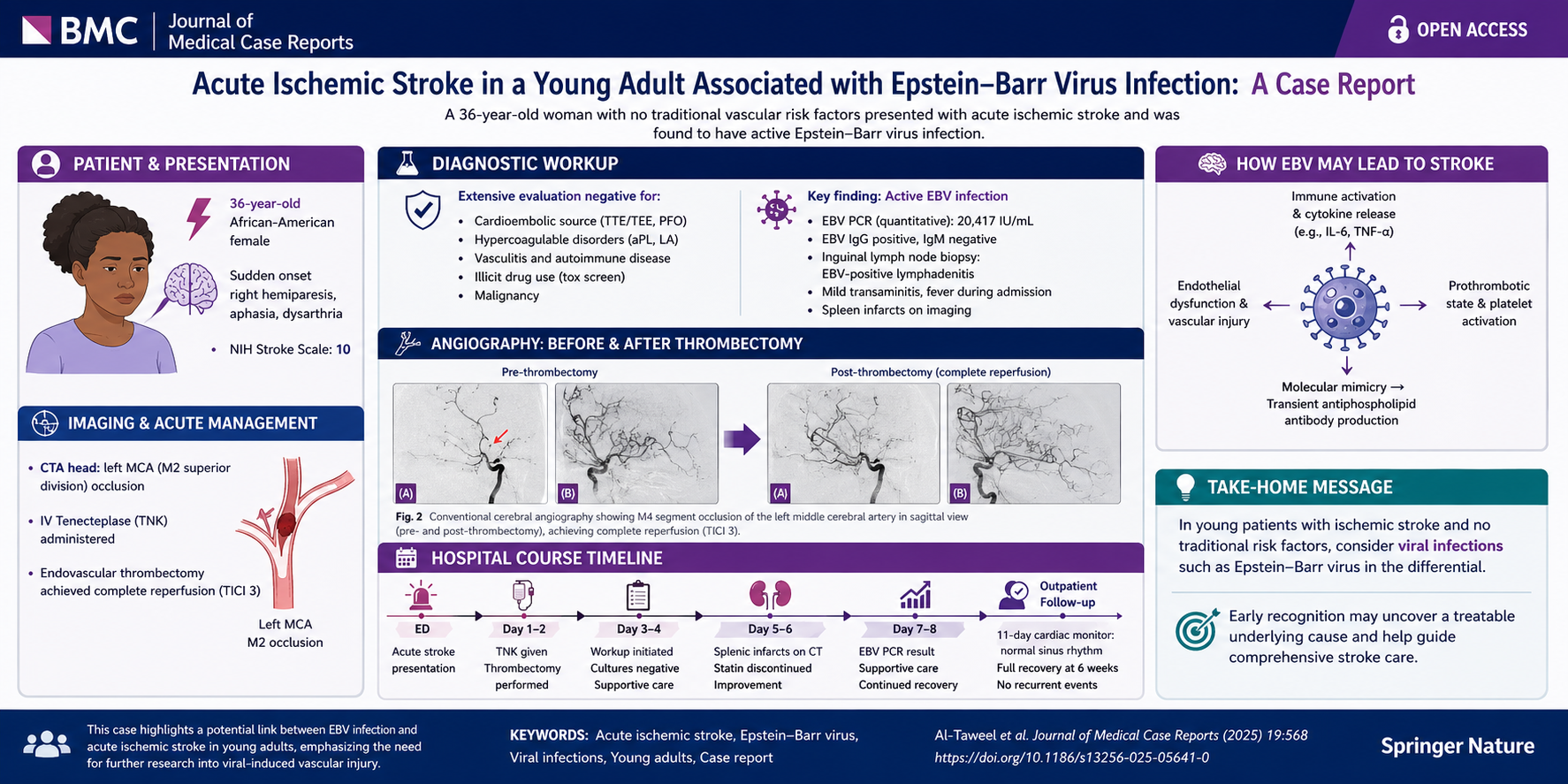
A 36-year-old woman presented with sudden right hemiparesis, aphasia, and dysarthria, with an NIH Stroke Scale score of 10. Imaging demonstrated a left middle cerebral artery (MCA) occlusion, and she underwent intravenous thrombolysis followed by successful endovascular thrombectomy, achieving complete reperfusion (as illustrated in the angiographic images on page 3).
Despite an extensive evaluation—including cardiac, hypercoagulable, and malignancy workups—no conventional etiology was identified. Notably, laboratory testing revealed markedly elevated EBV viral load (PCR >20,000 IU/mL) along with EBV-positive lymphadenitis on biopsy, suggesting active infection.
Additional findings—including splenic infarcts and transient lupus anticoagulant positivity—supported a systemic prothrombotic state. The patient ultimately made a full neurological recovery with standard stroke therapy and supportive care.
Why This Case Matters
This case underscores several important and evolving clinical insights:
Viral infections as stroke triggers: EBV may contribute to AIS through immune-mediated and prothrombotic mechanisms
Young stroke = broad differential: Absence of traditional risk factors should prompt expanded evaluation
Systemic clues matter: Lymphadenopathy, transaminitis, and inflammatory markers can signal an underlying infectious etiology
Mechanistic plausibility: Endothelial dysfunction, cytokine-mediated inflammation, and transient antiphospholipid antibody production may converge to promote thrombosis
The timeline figure on page 4 elegantly illustrates the sequence from acute stroke presentation through diagnostic clarification and recovery, emphasizing the temporal relationship between infection and cerebrovascular event.
Mechanistic Perspective
Although causality cannot be definitively established, several biologically plausible pathways link EBV to stroke:
Endothelial injury and vascular inflammation
Activation of coagulation cascade and platelet aggregation
Cytokine-driven proinflammatory state (e.g., IL-6, TNF-α)
Transient antiphospholipid antibody production via molecular mimicry
These mechanisms collectively support a temporary hypercoagulable state capable of precipitating arterial thrombosis.
Clinical Take-Home Message
In young patients with ischemic stroke and no clear etiology, particularly in the presence of systemic inflammatory or infectious features, viral causes such as EBV should be considered as part of the diagnostic workup.
Question
Which mechanism most plausibly links Epstein–Barr virus infection to ischemic stroke in this case?
A. Direct viral invasion of cerebral arteries causing vasculitis
B. Chronic atherosclerotic plaque rupture
C. Transient hypercoagulable state from immune activation
D. Cardioembolic source from atrial fibrillation
Correct Answer:
C. Transient hypercoagulable state from immune activation
Explanation:
EBV infection is thought to induce a prothrombotic milieu through immune activation, cytokine release, endothelial dysfunction, and transient antiphospholipid antibody production. These factors can promote thrombosis even in the absence of traditional vascular risk factors.
Final Thoughts
This case contributes to a growing body of literature suggesting that infection-associated stroke may be underrecognized, particularly in younger populations. While further research is needed, clinicians should remain vigilant—the trigger for stroke may lie outside the vasculature itself.
Journal of Medical Case Reports is the world’s first international, PubMed-listed, medical journal devoted to publishing case reports from all medical disciplines and will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports. The journal is open access, and strongly endorses the CARE guidelines for case reports, requiring authors to submit populated CARE checklists with submissions to improve transparency in reporting.
Follow the Topic
-
Journal of Medical Case Reports
This journal will consider any original case report that expands the field of general medical knowledge, and original research relating to case reports.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcement


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in