Why dementia prevention falls short when we ignore the exposome
Published in Social Sciences, Earth & Environment, and Neuroscience

From where you live to how your brain ages
Imagine two individuals of the same age. One lives in a country characterized by low air pollution, strong welfare systems, high democratic participation, accessible healthcare, and widespread green spaces. The other commutes long distances every day to access precarious work or healthcare, lives in a polluted and unequal environment, and has experienced climate-related displacement and lack of green spaces. We would not expect their brains to age in the same way. Yet most dementia research and prevention strategies implicitly assume that they do.
Research on aging and dementia has largely focused on individual-level risk factors (e.g., education, lifestyle, cardiovascular health) or on isolated macro-level exposures (e.g., specific air pollutants, socioeconomic inequality). This approach has been essential, but it implicitly treats exposures as operating independently. In reality, no one is exposed to just one factor. We live within layered, co-occurring environments shaped by interacting social, environmental, and political conditions. Inequality coexists with air pollution; limited healthcare access overlaps with political stability; climate-related events compound already fragile systems. These exposures cluster, interact, and accumulate over time.
A syndemic exposome
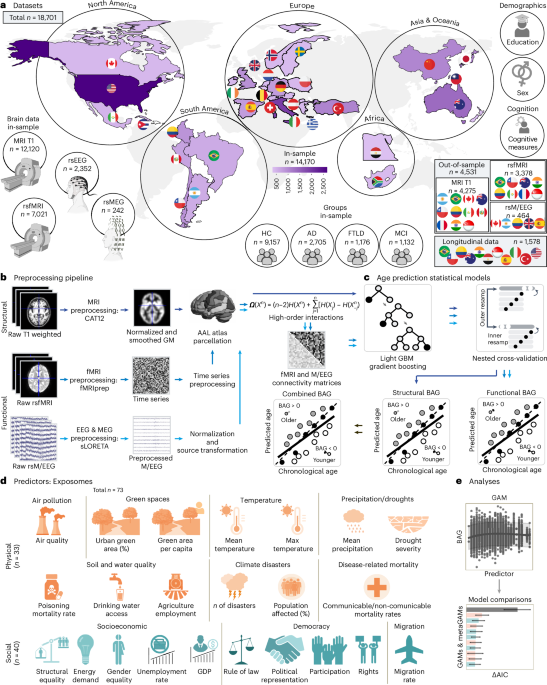
In our recent work, we asked what happens when we model these exposures as they actually occur: in combination. We analyzed 73 physical (environmental) and sociopolitical exposomal variables using brain clocks in 18,701 individuals across 34 countries, integrating them within a unified framework of brain aging. Participants spanned healthy aging, mild cognitive impairment, Alzheimer’s disease, and frontotemporal dementia.
One of the most compelling findings was that the combined exposome explained up to 15 times more variance in brain aging than individual factors alone. Cumulative exposure increased the likelihood of accelerated brain aging by 3 to 9 times, in some cases exceeding the effects associated with neurodegenerative diagnoses. Distinct domains also showed specific biological signatures: physical exposures were more strongly associated with structural brain aging, whereas sociopolitical exposures were more closely linked to functional brain changes.
But the most important insight was this: these effects were not simply additive. They were nonlinear and synergistic. Brain aging is not driven by isolated risks, but by interacting systems of exposure. Brain aging is a neurosyndemic process.
Why individual prevention may fall short
This perspective challenges how we think about prevention. Most current strategies focus on individual behaviors (e.g., exercise, diet, cognitive stimulation) or on treating disease once it is established. While important, these approaches overlook the structural conditions that shape risk in the first place. Dementia prevention frameworks often rely on decontextualized, individual-level models, ignoring the inequalities that constrain people’s ability to adopt healthy behaviors.
Our findings reinforce this point. When structural conditions persist, their biological effects accumulate through pathways such as stress regulation, immune activation, and cardiometabolic risk, ultimately accelerating brain aging.
Promoting physical activity, for example, has limited impact in environments without safe or accessible green spaces. Encouraging cognitive engagement without addressing educational inequality or healthcare access risks missing the root drivers of vulnerability. Brain health is also a social, environmental, and political issue, not only a biomedical one.
From exposome to policy. From global to local.
If brain aging is shaped by interacting exposures, then prevention must move beyond isolated actions and address the structural conditions that shape both risk and resilience. This means moving beyond fragmented interventions toward intersectoral strategies that address clusters of risk simultaneously: environmental regulation, social protection, healthcare access, urban planning, and institutional stability.
Our findings capture global patterns, but action takes place locally. The specific combinations of exposures that shape brain aging are likely to differ across regions, countries, cities and neighborhoods. The factors driving risk in one setting may not be the same in another. To translate this work into real-world impact, future research must identify context-specific exposome signatures. This will allow us to move from broad associations to targeted, actionable policies. In this sense, the exposome offers a bridge: from environments, to biological embedding, to policy action. What policies modify is not only context, but the biological brain trajectories shaped by that context.
Final thoughts
Addressing structural conditions does not replace individual-level prevention. However, by improving the environments in which people live, we expand the feasibility and impact of behavioral interventions, and potentially amplify their effects. Because when exposures interact, interventions must do the same.
Image created with AI assistance (ChatGPT, OpenAI), based on the author’s conceptual design.
Follow the Topic
-
Nature Medicine
This journal encompasses original research ranging from new concepts in human biology and disease pathogenesis to new therapeutic modalities and drug development, to all phases of clinical work, as well as innovative technologies aimed at improving human health.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Microbiome and energy metabolism
Publishing Model: Hybrid
Deadline: Dec 06, 2026
The expanding therapeutic landscape of GLP 1 receptor agonists
Publishing Model: Hybrid
Deadline: Jan 23, 2027


Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in