“A tumor-associated heparan sulfate-related glycosaminoglycan promotes the generation of functional regulatory T cells”.
Published in Immunology
Oscar Palomares1 and José Luis Subiza2
1Department of Biochemistry and Molecular Biology, School of Chemistry, Complutense University, Madrid, Spain 2Inmunotek, Alcalá de Henares, Madrid, Spain
Nowadays, it is well-accepted the essential role of the immune system in both tumor rejection and tumor progression1. Effective host antitumor responses are challenged by a plethora of different tumor escape mechanisms2-4. In this regard, compelling experimental evidence demonstrated that functional regulatory T cells (Tregs), which constitute a heterogeneous group of T cells with potent suppressive capacity, are abnormally expanded in cancer and greatly increased within the tumor tissues, thus playing a key role in tumor development and progression and posing a major barrier to anti-cancer immunity3, 5.
The mechanisms by which Tregs are fueled in hosts bearing malignant tumors and the contribution of the tumor microenvironment (TME) to these processes are not yet fully understood1-3, 6. Dendritic cells (DCs) are professional antigen-presenting cells that are crucial in the orchestration of proper immune responses by linking innate and adaptive immunity7. The ability of mature DCs infiltrating tumors to promote highly suppressive Tregs is strongly influenced by exogenous signals encountered in the TME7. However, how DCs integrate these signals and the functional resulting outcomes remains elusive.
Malignant transformation is accompanied by changes in tumor cell surface glycoconjugates8, including the aberrant or incomplete glycosylation of heavily glycosylated structures such as mucins and proteoglycans9. These structures are often overexpressed and shed from tumor cells, having a strong influence on tumor progression by modulating cell adhesion, neo-angiogenesis and metastases10. In addition, tumor-associated carbohydrates may inhibit anti-cancer immunity through different mechanisms11, including the activation of highly suppressive Tregs. Whether tumor-derived carbohydrate structures encountered by DCs might condition their capacity to polarize functional Tregs, the underlying molecular mechanisms and the potential clinical implications in tumor development, progression and anti-cancer treatments remain incompletely understood.
Murine Ehrlich's tumor (ET) cells, originally derived from a spontaneous mammary carcinoma, lack of H-2 antigens and can grow either in ascitic or solid form in almost any mouse strain across different antigenic backgrounds, thus representing a suitable model to uncover potential novel tumor escape mechanisms 12. Ca10 is a highly glycosylated ET cell surface macromolecule defined by the binding of monoclonal antibody (mAb) A1013,14. This antibody specifically recognizes a carbohydrate epitope on the Ca10 macromolecule. Ca10 is spontaneously released from ET cells and can be detected in the serum of ET-bearing mice14. Although A10 also reacts with glycan moieties located in some human cancer mucins15, the structural features of the carbohydrate moiety contained in Ca10 and its potential functional implications in cancer remains largely unknown.
In this study, we reveal that Ca10 derived from ET cells is mainly composed of heparan sulfate-related structures that promotes the generation of tolerogenic human DCs, which are able to produce highly suppressive FOXP3+ Tregs by mechanisms partially depending on PD-L1, IL-10, IDO, mTOR pathway and glycolysis. In vivo, we observed positive correlations between the serum level of Ca10, the tumor size and the generation of splenic Tregs in mice bearing solid ET. Remarkably, the administration of Ca10 to tumor-free mice also increased the frequency of splenic Tregs, which was fully impaired by the mAb A10. It is worthy to highlighting that in this study we also provide evidence supporting the presence of a circulating human counterpart and show, for the first time, that serum levels of Ca10H are increased in patients suffering from different cancer types compared to healthy individuals. Of note, in prostate cancer patients, these levels are higher in those with bone metastases.
In summary, in this work we demonstrated the involvement of a tumor-associated heparan sulfate structure in the induction of tolerogenic responses in cancer, which might well play an important role in the mechanisms of tumor escape and progression. The discovery of this novel structural-functional relationship might well pave the way for the identification of potential novel tumor biomarkers and for the improvement or development of alternative therapeutic strategies in cancer.
References
- Glasner A, Plitas G. Tumor resident regulatory T cells. Semin Immunol 2021; 52:101476.
- Watson MJ, Vignali PDA, Mullett SJ, Overacre-Delgoffe AE, Peralta RM, Grebinoski S, et al. Metabolic support of tumour-infiltrating regulatory T cells by lactic acid. Nature 2021; 591:645-51.
- Wing JB, Tanaka A, Sakaguchi S. Human FOXP3(+) Regulatory T Cell Heterogeneity and Function in Autoimmunity and Cancer. Immunity 2019; 50:302-16.
- Zhang H, Tomar VS, Li J, Basavaraja R, Yan F, Gui J, et al. Protection of Regulatory T Cells from Fragility and Inactivation in the Tumor Microenvironment. Cancer Immunol Res 2022; 10:1490-505.
- Gonzalez-Navajas JM, Fan DD, Yang S, Yang FM, Lozano-Ruiz B, Shen L, et al. The Impact of Tregs on the Anticancer Immunity and the Efficacy of Immune Checkpoint Inhibitor Therapies. Front Immunol 2021; 12:625783.
- Palomares O, Akdis M, Martin-Fontecha M, Akdis CA. Mechanisms of immune regulation in allergic diseases: the role of regulatory T and B cells. Immunol Rev 2017; 278:219-36.
- Wculek SK, Cueto FJ, Mujal AM, Melero I, Krummel MF, Sancho D. Dendritic cells in cancer immunology and immunotherapy. Nat Rev Immunol 2020; 20:7-24.
- Silva MC, Fernandes A, Oliveira M, Resende C, Correia A, de-Freitas-Junior JC, et al. Glycans as Immune Checkpoints: Removal of Branched N-glycans Enhances Immune Recognition Preventing Cancer Progression. Cancer Immunol Res 2020; 8:1407-25.
- Houvast RD, Vankemmelbeke M, Durrant LG, Wuhrer M, Baart VM, Kuppen PJK, et al. Targeting Glycans and Heavily Glycosylated Proteins for Tumor Imaging. Cancers (Basel) 2020; 12.
- Ahrens TD, Bang-Christensen SR, Jørgensen AM, Løppke C, Spliid CB, Sand NT, et al. The Role of Proteoglycans in Cancer Metastasis and Circulating Tumor Cell Analysis. Front Cell Dev Biol 2020; 8:749.
- RodrÍguez E, Schetters STT, van Kooyk Y. The tumour glyco-code as a novel immune checkpoint for immunotherapy. Nat Rev Immunol 2018; 18:204-11.
- Chen L, Watkins JF. Evidence against the presence of H2 histocompatibility antigens in Ehrlich ascites tumour cells. Nature 1970; 225:734-5.
- Gil J, Alvarez R, Viñuela JE, Ruiz de Morales JG, Bustos A, De la Concha EG, et al. Inhibition of in vivo tumor growth by a monoclonal IgM antibody recognizing tumor cell surface carbohydrates. Cancer Res 1990; 50:7301-6.
- Viñuela JE, Rodriguez R, Gil J, Coll J, De la Concha EG, Subiza JL. Antigen shedding vs. development of natural suppressor cells as mechanism of tumor escape in mice bearing Ehrlich tumor. Int J Cancer 1991; 47:86-91.
- Medina M, Velez D, Asenjo JA, Egea G, Real FX, Gil J, et al. Human colon adenocarcinomas express a MUC1-associated novel carbohydrate epitope on core mucin glycans defined by a monoclonal antibody (A10) raised against murine Ehrlich tumor cells. Cancer Res 1999; 59:1061-70.
Follow the Topic
-
Cellular & Molecular Immunology
A monthly journal from the Chinese Society of Immunology and the University of Science and Technology of China, covering both basic immunology research and clinical applications.
Ask the Editor - Immunology, Pathogenesis, Inflammation and Innate Immunity
Got a question for the editor about the complement system in health and disease? Ask it here!
Continue reading announcement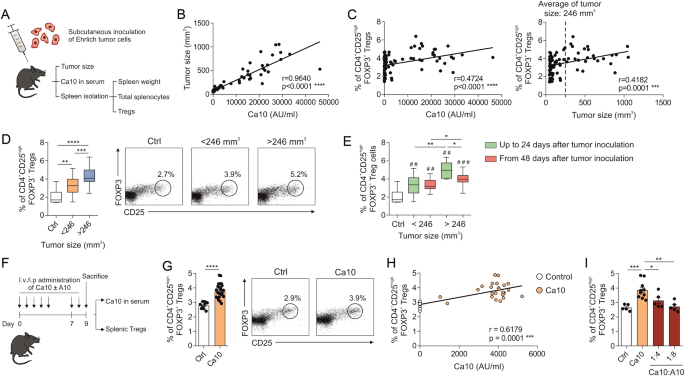



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in