Clinico-imaging features of subjects at risk of Lewy body disease in NaT-PROBE baseline analysis
Published in Neuroscience
Lewy body disease (LBD) is a group of neurodegenerative disorders associated with intra-neuronal accumulation of alpha-synuclein, including Parkinson’s disease (PD) and dementia with Lewy bodies (DLB). Patients with LBD have a progressive motor and cognitive decline, and various medicines have been used in the treatment of LBD, but there is no therapy which suppresses the disease progression during the pre-manifest stage of LBD. Initially levodopa controls motor symptoms well, but motor complications, such as dyskinesia and wearing off, occur frequently as the disease progresses. Because > 50% of neurons in the substantia nigra are already lost at the clinical diagnosis of PD, earlier detection and treatment of individuals at greater risk of developing PD is important.
Prodromal symptoms, such as dysautonomia, hyposmia, and REM sleep behavior disorder (RBD), antecede the onset of motor or cognitive dysfunction in LBD by 10–20 years. In addition, dopamine transporter scintigraphy (DaT-SPECT) and 123I-meta-iodobenzylguanidine (MIBG) scintigraphy may help diagnosing patients with LBD at a very early stage. To date, many risk factors and prodromal markers of LBD have been reported, but little has been reported on the prevalence of prodromal symptoms in the Japanese general population and the appropriate method for identifying high-risk individuals before developing neurological symptoms do not manifest.
In our previous study using questionnaires on prodromal symptoms, we found that approximately 8% of health checkup examinees with ≥ 50 years old had ≥ 2 prodromal symptoms (dysautonomia, hyposmia, and RBD), and defined them as high-risk subjects (Fig. 1, Hattori et al. J Neurol 267(5):1516-1526, 2020 modified). Here we analyzed neurological and imaging indices, including DaT-SPECT and MIBG scintigraphy, in the 69 high-risk individuals with prodromal symptoms as well as 32 low-risk individuals without prodromal symptoms, to clarify the manifest LBD-related changes at possible prodromal subjects and to verify the plausibility of our screening methods using questionnaires.

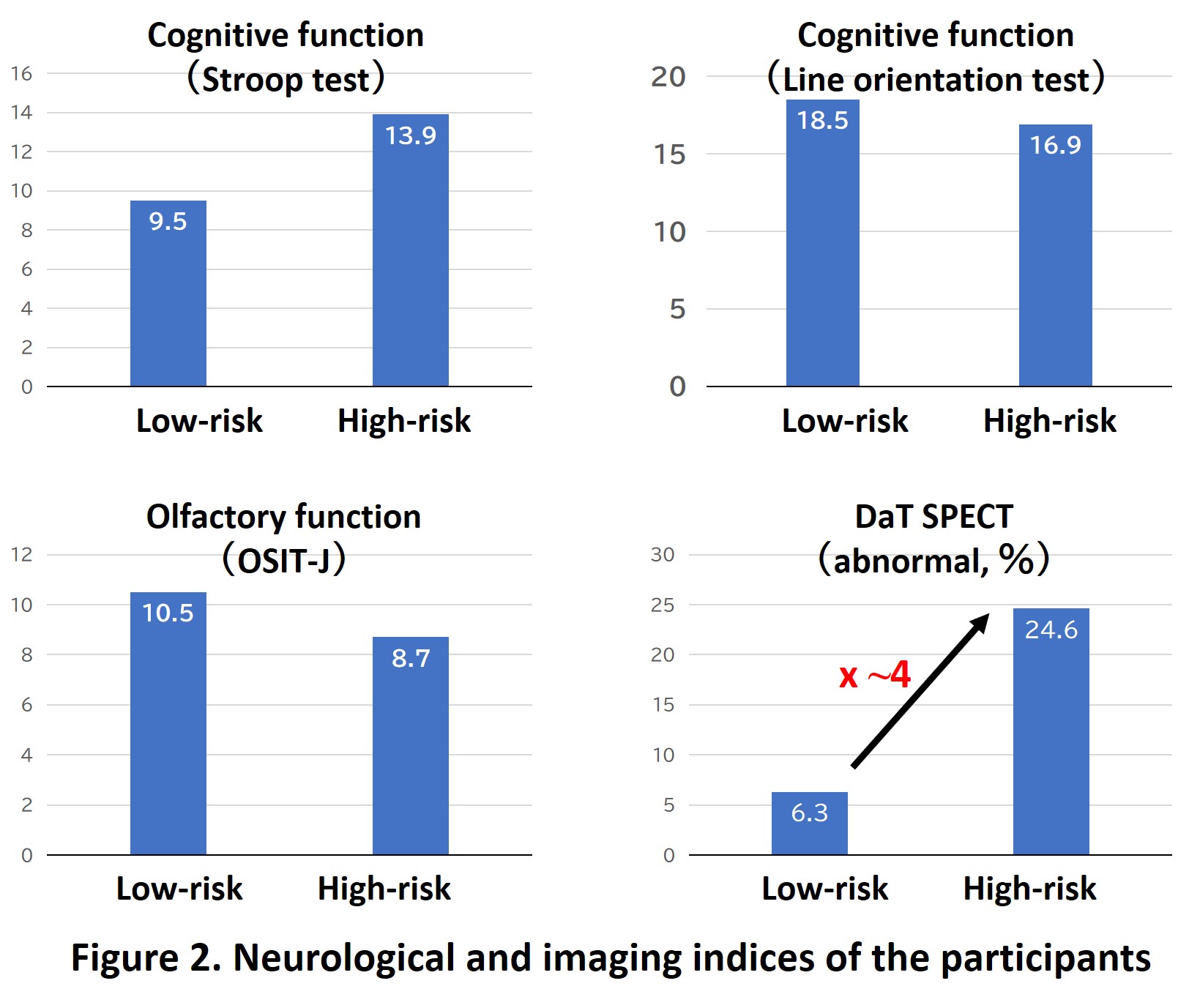
The present study revealed that high-risk subjects with two or more prodromal symptoms had significantly worse scores on Stroop test, line orientation test, and the Odor Stick Identification Test for Japanese (OSIT-J) compared to low-risk subjects without prodromal symptoms. The prevalence of abnormalities on DaT-SPECT was higher in the high-risk group than in the low-risk group (24.6% vs. 6.3%, p = 0.030), indicating that dopamine neurodegeneration occurs even at the prodromal stage (Fig. 2).
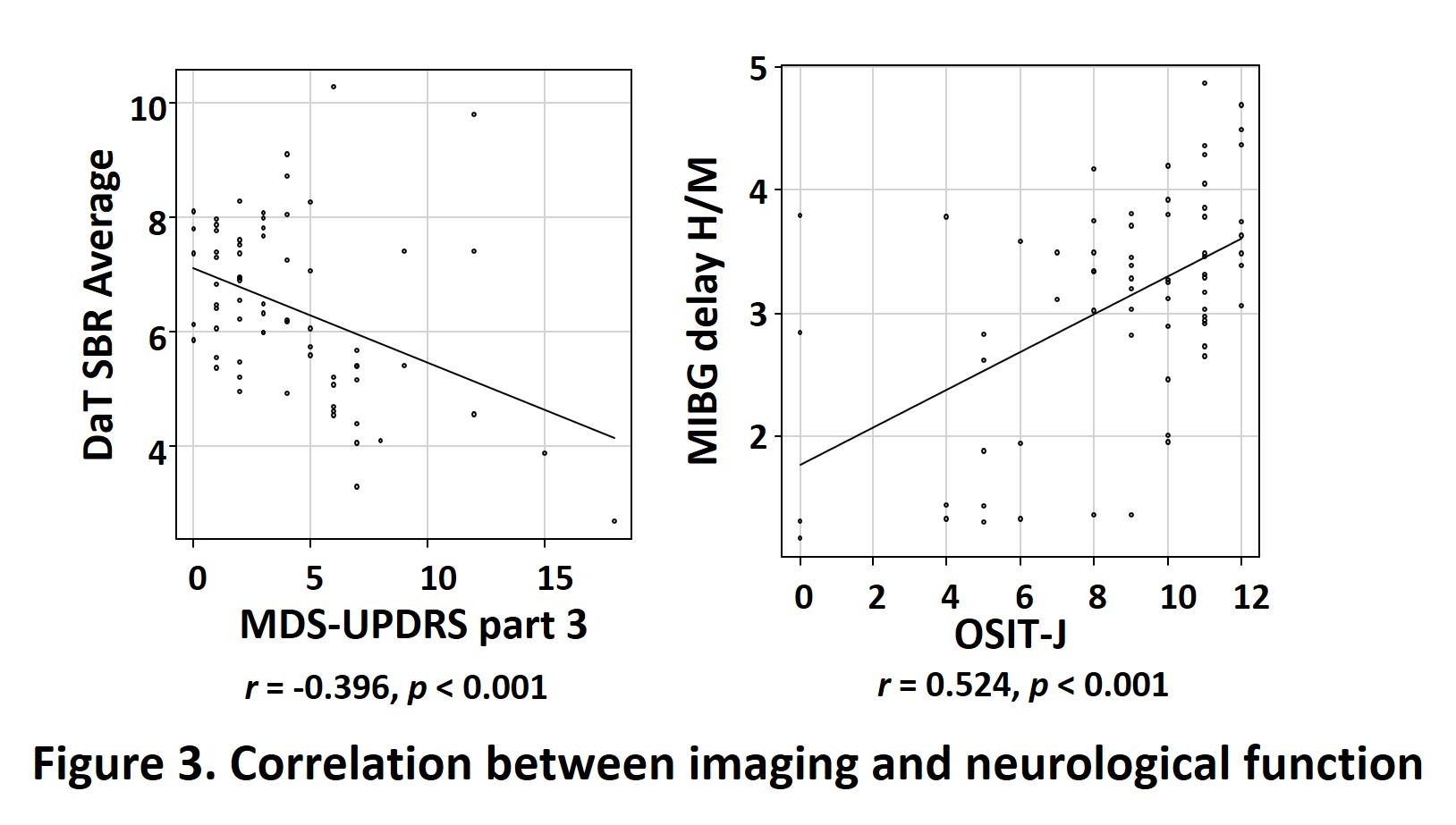
A decreased uptake on DaT-SPECT was associated with motor impairment, and MIBG scintigraphy defects were associated with hyposmia (Fig. 3). In addition, high-risk subjects who showed abnormalities in both DaT-SPECT and MIBG scintigraphy were approximately 10 years older than other groups, and had more severe motor impairment, cognitive decline, and olfactory dysfunction, suggesting that LBD-related pathological changes developed more extensively in such subjects and possibly closer to the onset of LBD than in other groups.
The clinical course of PD is diverse, especially in the early stages of the disease, with some patients having predominantly motor deficits and less prominent non-motor symptoms, and others having predominantly non-motor symptoms and less prominent motor deficits. Since neurodegeneration is mild at the prodromal stage compared with patients with LBD, there are many cases in which only one of DaT-SPECT and MIBG scintigraphy show abnormalities. We found that the simultaneous evaluation of DaT-SPECT and MIBG scintigraphy may capture a wide range of individuals with prodromal LBD. Although it has been difficult to identify high-risk subjects without neurological symptoms in daily medical practice, our results indicate that a combination of a simple questionnaire survey and imaging tests, such as DaT-SPECT and MIBG scintigraphy, was feasible for assessing the risk of Lewy body disease in a healthy population.
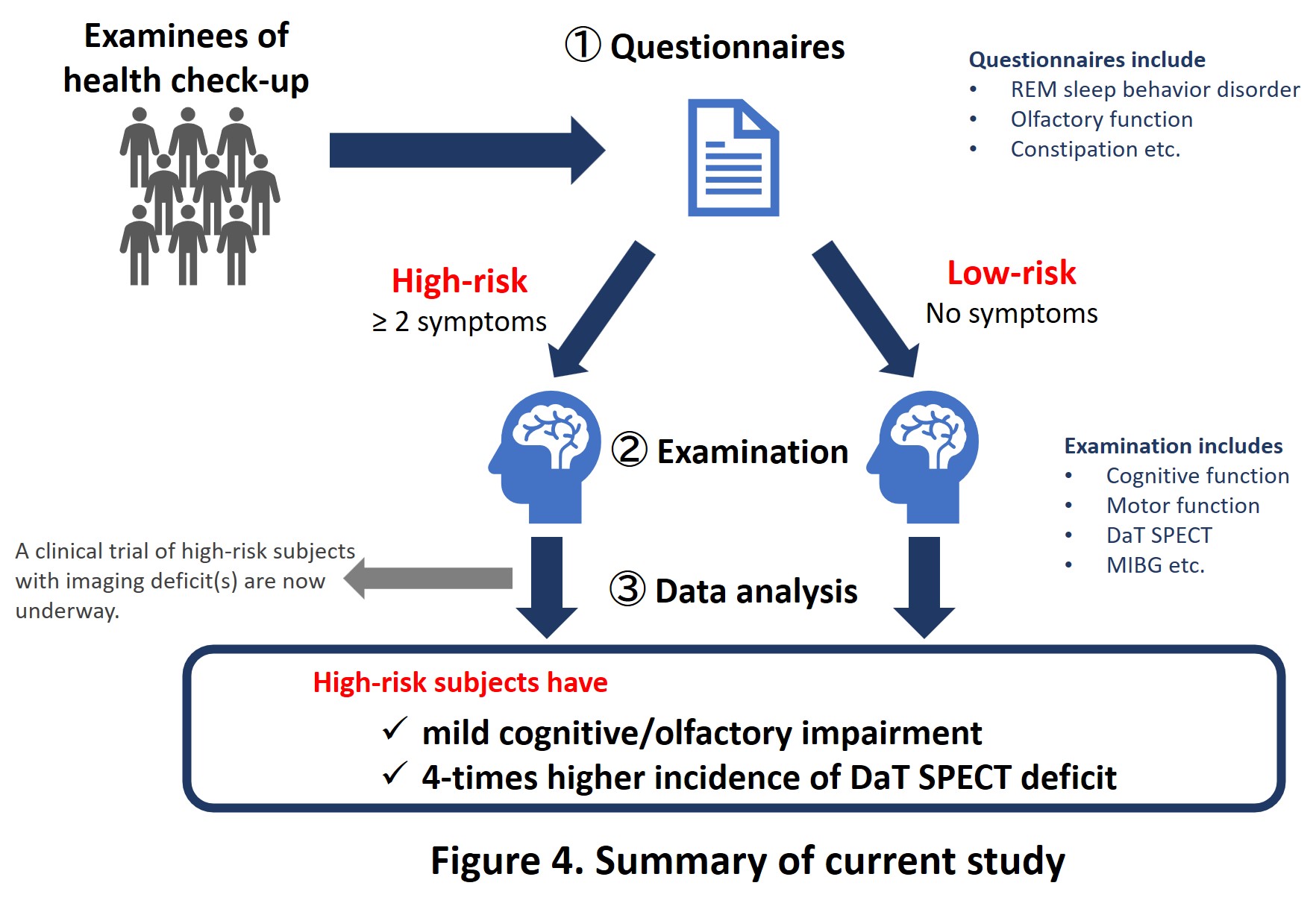
In summary, our study revealed that high-risk subjects with two or more prodromal symptoms had mild cognitive decline and hyposmia compared to low-risk subjects, and the prevalence of abnormalities on DaT-SPECT was higher in the high-risk group. We are currently conducting a clinical study titled “Study on efficacy and safety of zonisamide in at-risk subjects of Lewy body disease” in patients with prodromal LBD detected in this study (Fig. 4). Zonisamide, which was selected as the study drug, is widely used in daily medical practice as a previously approved drug for PD and DLB, and has been reported to show neuroprotective effects in basic studies using rats, mice, and cells. We expect that zonisamide would delay the onset of LBD by administering it very early to patients with prodromal LBD.
Follow the Topic
-
npj Parkinson's Disease

This journal publishes original basic science, translational and clinical research related to Parkinson's disease, including anatomy, etiology, genetics, cellular and molecular physiology, neurophysiology, epidemiology and therapeutic development and treatments.
Your space to connect: The Psychedelics Hub
A new Communities’ space to connect, collaborate, and explore research on Psychotherapy, Clinical Psychology, and Neuroscience!
Continue reading announcementRelated Collections
With Collections, you can get published faster and increase your visibility.
Cognition - preclinical models, and preclinical unmet need
Publishing Model: Open Access
Deadline: Jul 27, 2026
Environmental risk factors for Parkinson’s disease
Publishing Model: Open Access
Deadline: May 13, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in