E- Learning experience of the medical profession’s college students during COVID-19 pandemic in Saudi Arabia
Published in Education
E-learning is a broad concept that includes the delivery of educational programs through electronic systems using Internet for teacher/student interactions and dissemination of learning materials. It involves the implementation of advanced technologies for planning, designing, and delivering learning content, and for facilitating two-way communication between teachers and students.
The COVID-19 pandemic has led to the closure of educational institutions across the world. As a result, educational institutions shifted to online methods, commonly referred to as e-learning as possible replacement for traditional face-to-face teaching. By March 2020, more than 107 countries implemented a nationwide e-learning system. Similarly, the Ministry of Education in Saudi Arabia announced distance learning for public and private schools and universities as a preventive and precautionary measure to contain the spread of coronavirus.
It is well known that the success of an e-learning program depends largely on the learning tools and technical support available to users. E-learning standards for higher education in the Kingdom of Saudi Arabia were established in accordance with the most renowned international standards, which include technology, training and support, design, interaction, equity and accessibility, and assessment and evaluation. Each e-learning system established its basic foundation of computers, networks, communications and technical facilities, along with ICT specialists to continuously maintain and update the system, train users and provide technical support. Appropriate technological support and maintenance of available hardware and software were essential for the optimal use of technology by teachers and students. This study explored the e-learning experience of the students of the colleges of health sciences with regard to the technical preparedness, academic achievements, e-learning advantages and limitations.
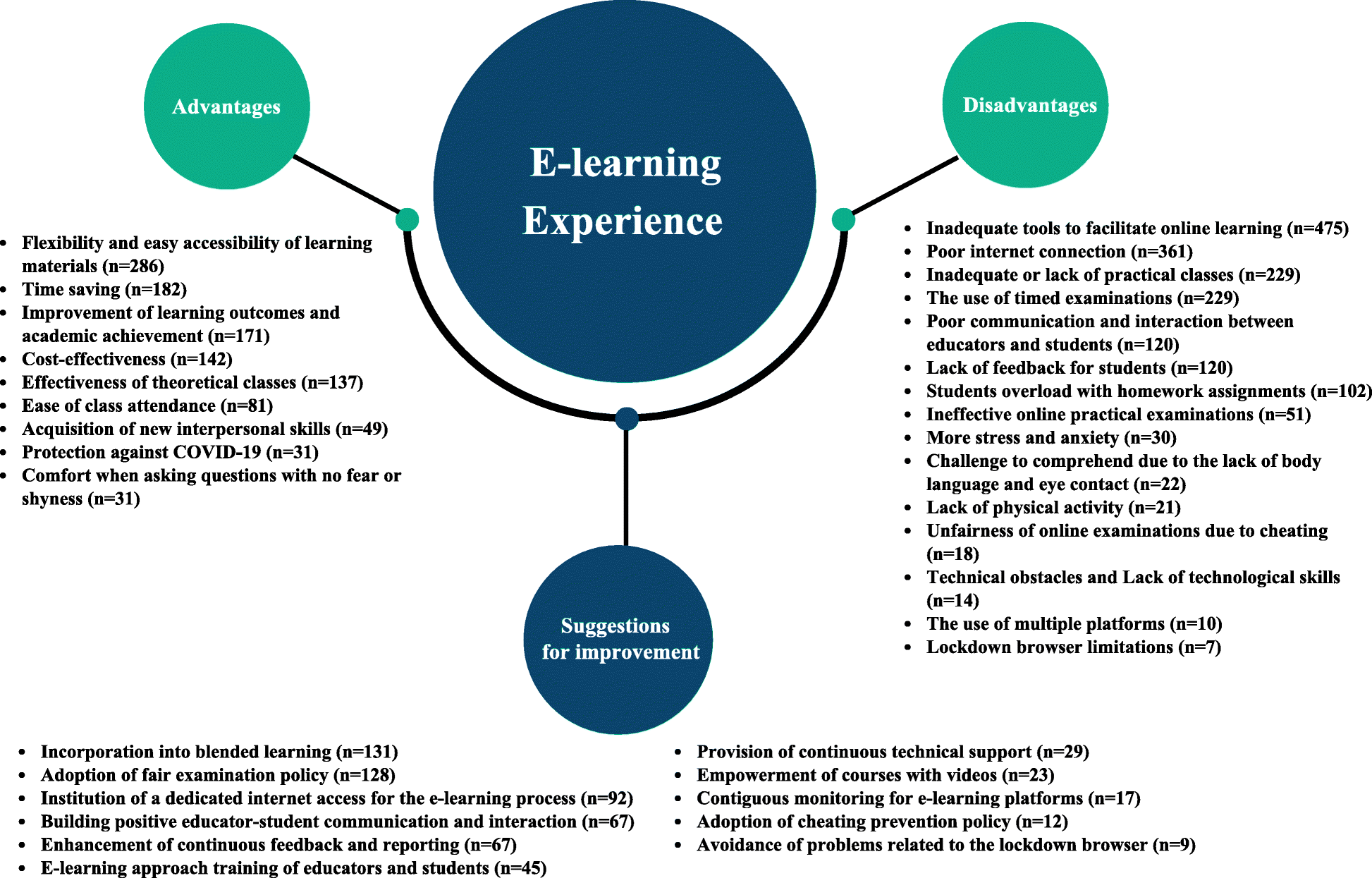
Out of 1288 respondents, 58.2% agreed that they had sufficient information about online learning. The advantages of e-learning were flexible access to learning materials, saving time, effort and money, acquiring and improving technical and self-learning skills, health safety, interacting without shyness and higher academic achievement. On the other hand, the disadvantages and challenges included inadequate tools to facilitate online learning, poor internet connection, lack of technology skills of teachers and students. In addition, there were insufficient or insufficient practical classes, lack of uniform clear policy for conducting online classes and examinations and distribution of marks, limited time for online examinations.
The proportion of those who reported receiving adequate guidance, technical support, and having satisfactory equipment and internet access for online learning were 48.1%, 42%, and 35.4%, respectively. Of all the participants, 40.8% agreed that they had a good understanding of the learning outcomes of their courses. Only 30.0% agreed that the quality of online learning was similar to traditional classes, and 56.1% agreed that online learning was not suitable for learning health sciences. The study found that a relatively high proportion of respondents, 58.2%, agreed that they had sufficient information about the e-learning platform. However, less than 50% of the total participants agreed that they had received adequate guidance and technical support during the e-learning process. Personal equipment and internet access were rated as satisfactory for the learning process by 35.5% in the current study, compared to 44.1% who rated them as unsatisfactory. Most of the respondents to the study agreed that easily accessible online learning materials for all courses were provided in a timely manner during the study period. It was stated that the success of the online education program was due to the provision of adequate levels of educational guidance and technical support.
Most students disagreed with the effectiveness of virtual practicals as a substitute for real laboratory training. It was recommended that a mixed learning strategy that includes face-to-face laboratory training was more appropriate. Virtual labs and video labs were the best choice when students were not physically on campus. It was stated that online learning and laboratory practice in biological sciences were often more effective than traditional teaching.
A significant proportion of participants in the current study considered e-learning to be a stressful experience. Anxiety and stress related to the pandemic were listed among the concerns. Most of the students in this study stated that they would not want to attend more e-learning classes if given the option. Stress was more often associated with e-learning than with traditional learning. Increased concerns about academic performance had previously been identified as stressors contributing to increased levels of stress, anxiety, and depressive thoughts among students due to the COVID-19 pandemic situation.
Several suggestions were mentioned to improve the e-learning process. These included the use of mixed learning strategies that include face-to-face practical/clinical teaching. Other suggestions included technical training of staff and students, greater use of visual learning materials, more time for multiple-attempt exams, having an exam policy during internet disconnection, using an effective system that detects and prevents cheating, and encouraging active interaction between the instructor and students. The cumulative data of this study and international evidence from the pandemic years show that more scientific evidence is still needed to clearly compare online and traditional teaching.
Follow the Topic
-
BMC Medical Education
This is an open access journal publishing original peer-reviewed research articles in relation to the education and training of healthcare professionals. It welcomes studies on students and professionals across all levels of education; education delivery aspects; and other education-related topics.
Related Collections
With Collections, you can get published faster and increase your visibility.
Transnational medical education programs
BMC Medical Education is calling for submissions to our Collection on Transnational medical education programs. As medical education expands beyond national boundaries, new opportunities and challenges are emerging in how curricula are delivered, quality is assured, and learners are supported across diverse cultural and institutional contexts. These cross-border educational partnerships are reshaping the way we define standards, prepare future health professionals, and foster global health equity.
This Collection invites research that critically examines the structure, outcomes, and implications of educational initiatives that operate across borders. Whether through institutional partnerships, dual-degree programs, offshore campuses, or digital learning platforms serving international student populations, transnational initiatives demand thoughtful attention to pedagogical alignment, accreditation, faculty development, and learner experience. We welcome insights that address the complexity of delivering medical education in settings where geographic, regulatory, and cultural contexts differ.
We encourage submissions on topics such as:
• Curriculum design and adaptation across cultural and regulatory contexts
• Accreditation and quality assurance in cross-border medical education
• Faculty development and support in international teaching environments
• Student experiences, identity formation, and transitions between institutions
• Governance models and institutional partnerships in global medical education
• Ethical considerations and power dynamics in transnational collaborations
• Role of digital platforms and technology-enhanced education in delivering cross-border education
This Collection aims to showcase diverse voices and evidence-based approaches that inform the development and sustainability of cross-national medical education programs. By fostering open dialogue and rigorous inquiry, we seek to support inclusive, high-quality education that prepares graduates to meet health needs across a global landscape.
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-being, SDG 4: Quality Education, and SDG 17: Partnerships for the Goals.
Publishing Model: Open Access
Deadline: Jun 23, 2026
Lifelong learning and patient safety
BMC Medical Education is calling for submissions to our Collection, Lifelong learning and patient safety. As healthcare delivery becomes increasingly complex, shaped by biomedical advances, digital transformation, demographic shifts, and changing patient expectations, so does the potential for errors and adverse events. This phenomenon makes it essential to equip all healthcare professionals with training and tools to prioritize patient safety across different clinical environments.
Patient safety is a global health priority, with the World Health Organization identifying unsafe care as one of the leading causes of avoidable morbidity and mortality worldwide. While traditional models of competence, validated at a single point in time through licensure or certification, can be valuable, addressing this challenge requires a workforce that is continuously learning, adaptive, and equipped to respond to evolving patient safety threats. Lifelong learning in healthcare plays a pivotal role in fostering patient safety by making sure that healthcare professionals remain competent and adaptive to the best practices in the medical field. Outdated knowledge or skills in the medical field can directly jeopardize patient outcomes. Therefore, continuous professional development allows clinicians to update their professional competencies, reducing the risk of errors and adverse events.
This Collection invites research that examines how patient safety, which should be a professional expectation and ethical imperative at all stages of one’s career trajectory, can be enhanced through innovation in health professions education and training. Topics of interest include, but are not limited to:
• Tools and strategies for integrating patient safety into medical and nursing curricula
• Lifelong learning and continuing professional development (CPD) for patient safety and competence
• Simulation for teamwork, inclusion, and communication in diverse healthcare teams to enhance patient safety
• Interprofessional and collaborative safety culture
• Infection prevention and medication safety practices
• Learning from errors, near-misses, and real-time decision-making in clinical teams
• Strategies and policies for enhancing lifelong learning for patient safety
All manuscripts submitted to this journal, including those submitted to collections and special issues, are assessed in line with our editorial policies and the journal’s peer review process. Reviewers and editors are required to declare competing interests and can be excluded from the peer review process if a competing interest exists.
This Collection supports and amplifies research related to SDG 3: Good Health and Well-Being and SDG 4: Quality Education.
Publishing Model: Open Access
Deadline: Aug 18, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in