Epigenetic immunomodulation to improve the efficacy of cancer immunotherapy: a long-standing path
Published in Cancer
The story behind
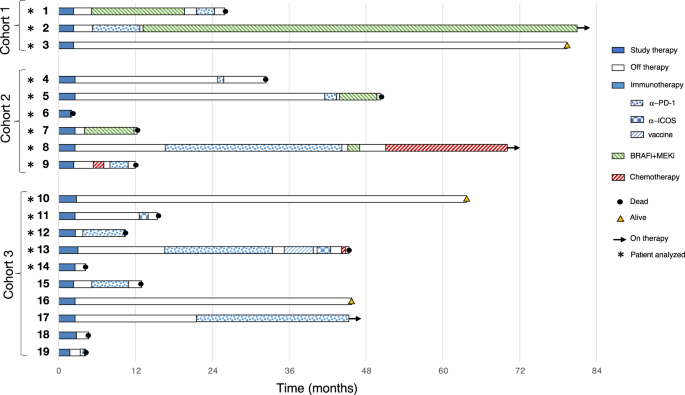
Therapeutic targeting of immune check-point(s) inhibitors (ICI) has dramatically changed the prognosis of cancer patients in multiple tumor types. However, a significant proportion of patients still fails to respond to ICI therapy due to primary or secondary resistance to treatment. Thus, identifying new combination/sequencing therapeutic approaches to improve the efficacy of ICI, as well as other immunotherapeutic agents is mandatory. Along this line were our very initial observations generated over two decades ago, demonstrating the role of DNA hypomethylating agents (DHA) to upregulate HLA class I antigens (1) and tumor recognition by antigen-restricted cytotoxic T lymphocytes (2). These findings allowed us to firstly contribute to the notion that DHA may represent ideal partner agents to improve the efficacy of cancer immunotherapy (3). Since then, a bulk of pre-clinical in vitro and in vivo evidence further supported this hypothesis, clearly identifying DHA as the best-in-class agents due to their strong immunomodulatory activity (4-8). Though conceptually highly promising, the idea that combination of DHA with immunotherapies could improve the clinical outcome in cancer patients required a significant amount of time to move to the clinic. Indeed, the first clinical proof ever generated confirming the feasibility, clinical, and immunomodulatory potential of such combination, derived from the Italian Network for Tumor Biotherapy (NIBIT) Foundation phase Ib clinical NIBIT-M4 trial, based on the association of the anti-CTLA-4 ipilimumab, with the DHA guadecitabine, in advanced melanoma patients. This very initial study was made possible also thanks to the tight and long-standing collaboration we had established with colleagues at Astex Pharmaceuticals who provided the DHA guadecitabine for the study. Indeed, the results of the NIBIT-M4 study showed significant tumor immunomodulatory effects and evidence of clinical activity for this combination (9). An undoubtful support to the NIBIT-M4 study, and to its further clinical and multi-omics integrated analyses published in Nature Communications (10) has derived from the work of the EPigenetic Immune-oncology Consortium AIRC (EPICA) consortium established in 2017, within the 7-year grant Fondazione AIRC under 5 per Mille 2018 (see below). Indeed, main goals of the EPICA program are to characterize epigenetically-regulated mechanism(s) contributing to cancer progression and metastatization and to resistance to ICB therapy, and to develop innovative therapeutic combinations of epigenetic drugs with ICI. Based on the initial results of the NIBIT-M4 study (9), we now aimed to report its long-term follow-up, together with an integrated multi-omics analysis of pre-defined exploratory endpoints. The novel key messages of the paper published in Nature Communications (10) are: i, guadecitabine combined with ipilimumab in metastatic melanoma patients leads to an intriguing 28.9% 5-year overall survival, to a median duration of response of 20.6 months, and to a prolonged treatment free interval, that well compare with ipilimumab administered as single agent (11); ii, re-expression of immunomodulatory endogenous retroviruses and other repetitive elements, and a mechanistic signature of guadecitabine associate with response to therapy (Figure 1); iii, integration of a genetic immunoediting index with an adaptive immunity signature classifies patients into four subsets and discriminates 5-year overall survival and progression free survival.

The team behind
The results reported in the paper (10) were generated thanks to the multi-faceted professionals belonging to the EPICA consortium led by Michele Maio, and to the collaboration with well-renewed scientists outside the consortium. This multi-professional integration was deemed crucial to unravel the complex questions spanning from the laboratory to the clinic and vice versa, that we wanted to address in the NIBIT-M4 study. Indeed, among other professionals belonging to the EPICA consortium, medical oncologists (Anna Maria Di Giacomo and Michele Maio), computational biologists (Michele Ceccarelli and Teresa Maria Rosaria Noviello), immunobiologists (Andrea Anichini, Roberta Mortarini, and Alessia Covre) had worked hardly to integrate their very diverse professional expertise. Not being enough to fully achieve the goal, the work also required a thorough analysis of the tumor microenvironment (Wolf-Hervé Fridman and Catherine Sautes-Fridman) that was performed outside the EPICA consortium.
The future behind
Being a phase Ib study, the relative contribution of ipilimumab and guadecitabine to its results could not be fully dissected in the NIBIT-M4 trial. However, its comprehensive findings have paved the way to the ongoing NIBIT-ML1 study, a randomized, multicenter, phase II trial (NCT04250246), sponsored by the NIBIT Foundation within the EPICA consortium. The NIBIT-ML1 study will further address the clinical and immunobiologic contribution of the oral DHA decitabine/cedazuridine (ASTX727) to ICI therapy with ipilimumab and nivolumab, in PD-1/-L1-resistant melanoma and non-small cell lung cancer patients.
References
- Coral S et al. Prolonged upregulation of the expression of HLA class I antigens and costimulatory molecules on melanoma cells treated with 5-aza-2'-deoxycytidine (5-AZA-CdR). J Immunother. 1999 Jan;22(1):16-24.doi: 10.1097/00002371-199901000-00003.
- E Fonsatti E et al. Functional up-regulation of human leukocyte antigen class I antigens expression by 5-aza-2'-deoxycytidine in cutaneous melanoma: immunotherapeutic implications. Clin Cancer Res. 2007 Jun 1;13(11):3333-8. doi: 10.1158/1078-0432.CCR-06-3091.
- Maio M et al. Molecular Pathways: At the Crossroads of Cancer Epigenetics and Immunotherapy. Clin Cancer Res. 2015 Sep 15;21(18):4040-7. https://doi: 10.1158/1078-0432.CCR-14-2914.
- Sigalotti L et al. Epigenetic Drugs as Pleiotropic Agents in Cancer Treatment: Biomolecular Aspects and Clinical Applications. J. Cell. Physiol. 212: 330–344, 2007.
- Lofiego et al. Epigenetic Immune Remodeling of Mesothelioma Cells: A New Strategy to Improve the Efficacy of Immunotherapy. Epigenomes 2021, 5, 27. https://doi.org/10.3390/ epigenomes5040027
- Covre A et al. Epigenetics meets immune checkpoints. Semin Oncol. 2015 Jun;42(3):506-13. https:// doi: 10.1053/j.seminoncol.2015.02.003.
- Covre A et al. Antitumor activity of epigenetic immunomodulation combined with CTLA-4 blockade in syngeneic mouse models. OncoImmunology, 4:8, e1019978, DOI: 10.1080/2162402X.2015.1019978
- Anichini A et al. Landscape of immune-related signatures induced by targeting of different epigenetic regulators in melanoma: implications for immunotherapy. J Exp Clin Cancer Res. 2022 Nov 17;41(1):325. https://doi: 10.1186/s13046-022-02529-5.
- Di Giacomo AM et al. Guadecitabine Plus Ipilimumab in Unresectable Melanoma: The NIBIT-M4 Clinical Trial. Clin Cancer Res. 2019 Dec 15;25(24):7351-7362. https://doi: 10.1158/1078-0432.CCR-19-1335.
- Noviello, T.M.R., et al. Guadecitabine plus ipilimumab in unresectable melanoma: five-year follow-up and integrated multi-omic analysis in the phase 1b NIBIT-M4 trial. Nat Commun 14, 5914 (2023). https://doi.org/10.1038/s41467-023-40994-4
- Larkin J et al. N Engl J Med 2019; 381:1535-1546. DOI: 10.1056/NEJMoa1910836
Follow the Topic
-
Nature Communications
An open access, multidisciplinary journal dedicated to publishing high-quality research in all areas of the biological, health, physical, chemical and Earth sciences.
Related Collections
With Collections, you can get published faster and increase your visibility.
Women's Health
Publishing Model: Hybrid
Deadline: Ongoing
Biosensing
Publishing Model: Hybrid
Deadline: Jun 30, 2026





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in