Ever shifting strains
Published in Microbiology
The bacteria Streptococcus agalactiae is more commonly known as Group B Streptococcus or GBS. The Streptococcus groupings were developed by Rebecca Lancefield in the 1930s. They are somewhat redundant now due to other methods of categorising bacteria, but Group A Strep and Group B Strep are still commonly used (Group A strep or GAS is Streptococcus pyogenes, which causes a range of diseases, the most well known of which is scarlet fever).
Anyway back to GBS, which is mostly harmless – until it isn’t. It can colonise people without causing an infection. It mainly lives in the gastro-intestinal (GI) and genito-urinary (GU) tracts. Unfortunately, it can have major and severe impacts during pregnancy. It is the leading cause of neonatal infection, having severe consequences for the newborn baby. It passes from the mother, who has some level of immune protection, to the baby (who doesn’t) during, or shortly after, birth. Whilst antibiotics can reduce the burden of disease, they are not completely effective and alternative preventative approaches are needed. One of which is vaccination, but one of the challenges is that the mechanism by which women are protected against disease is not well understood. More work is needed to understand the interplay between the immune system and the colonising bacteria.
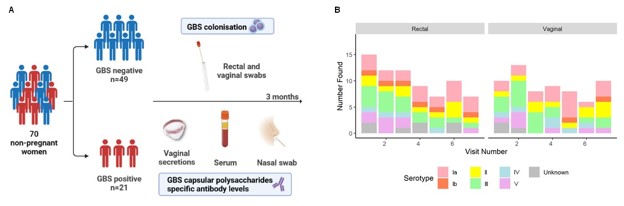
In our latest study, Group B Streptococcus (GBS) colonisation is dynamic over time, whilst GBS capsular polysaccharides-specific antibody remains stable we worked with Professor Kirsty le Doare and her group at St George’s University in London to look at the interplay of GBS colonisation and the immune response. Women were recruited and had samples taken from their GI-GU tracts every 2 weeks for 12 weeks. We then measured whether GBS was present, which strain of GBS it was and whether colonisation led to an increase in the amount of antibody the women made.
We observed that colonisation with GBS was dynamic – there were volunteers that were colonised initially that subsequently cleared the colonisation, there were others that acquired bacterial colonisation, there were some that were never colonised and others that had multiple different strains. However, whilst the bacterial colonisation was variable, the levels of antibody were fairly constant implying that acquisition of bacteria may not be directly affecting whether the women make more antibody – or that they have previously been exposed to the same strains and therefore don’t make new responses. Alternatively, there may be something special about the guts that mean that bacteria that live there (but are not necessarily causing disease) don’t trigger the immune response.
This study was performed during the COVID lockdowns which significantly disrupted the collection of samples. However, thanks to innovations by the study leads – such as home sampling, it was possible to continue. These kinds of approaches may mean larger studies can be performed as they are less intensive on the researchers and participants.
This study demonstrated the complex interplay between host and bacteria. Further investigation is needed to understand how best to utilise a vaccine to protect against this devastating disease.





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in