Full-length MSP1 as a malaria vaccine: is there hope?
Successful immunisation studies in monkeys based on MSP1 involved the use of the full-length protein as a malaria vaccine. However, unsuccessful human trials only tested MSP1 subunits. We explore the potential of SumayaVac-1 to broadly stimulate immune mechanisms associated with protection.
Published in Microbiology
Unsuccessful clinical trials in humans have ruled out the once-promising malaria vaccine candidate antigen Plasmodium falciparum Merozoite Surface Protein 1 (MSP1). However, successful non-human primates immunization studies with parasites cultures-derived full-length MSP1 had rendered protection and clearance of blood infections from the monkeys. Difficulties at the time to recombinantly produce the whole full-length MSP1 protein as a vaccine construct, together with the high immunogenicity demonstrated against the C-terminal p42 fragment of MSP1 in immune-epidemiological studies, directed the interest of MSP1-based vaccines towards the design of subunit vaccines. The focus was quickly set on the GPI-anchored p19 subunit, the only remaining fragment of MSP1 attached to the merozoite surface at the onset of erythrocyte’s invasion and believed to play a crucial role in this important process.
Neutralizing antibodies inhibiting merozoite invasion have been considered key for immune protection. However, there is an increasing body of evidence suggesting a role of the innate immunity, via Fc-mediated effector mechanisms, in parasite clearance. These antibody functions have shown to highly correlate with protection in individuals from malaria endemic regions.
A previous publication by Blank & Fürle et al. demonstrated that SumayaVac-1, the first entire full-length MSP1-based malaria vaccine candidate expressed in E. coli, was safe, well-tolerated, and immunogenic in a first in human trial conducted in Heidelberg (Germany). SumayaVac-1 elicited high antibody titers in naïve volunteers that remained for more than six months after the last immunization over the level of semi-immune individuals from Africa.
In our recently published paper in npj Vaccines we describe that both, IgG and IgM antibodies elicited by SumayaVac-1 can activate, in a strain transcending manner, potent Fc-mediated effector mechanisms involved in the interaction with complement as well as with various immune cells, including monocytes, neutrophils, and NK cells, known to combat parasites. Notably, the N-terminal fragment p83, which contains highly conserved regions, emerged as a key target of functional immunoglobulins. Additionally, SumayaVac-1 elicited a recallable cellular cytotoxicity by IFN-γ producing CD8+ T cells, although at a low scale.
An ongoing clinical trial in Bagamoyo (Tanzania) will preliminarily evaluate the vaccine's proof of concept of efficacy through a control human malaria infection (CHMI). We will further determine if the quality feature of the SumayaVac-1 to elicit broadly functional antibodies at titers sufficient to stimulate several immune mechanisms can lead to a control in blood stage development of P. falciparum.
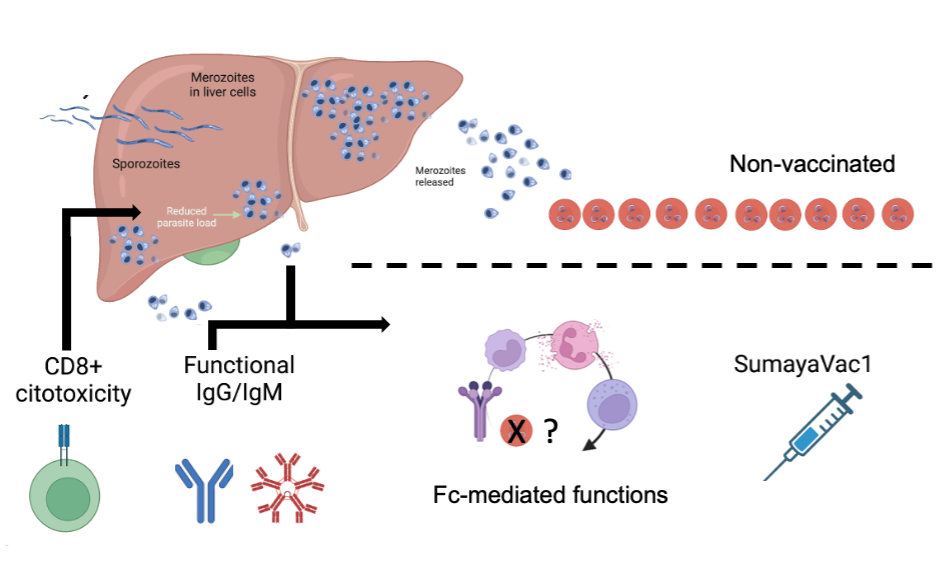
In the pursuit of malaria eradication, SumayaVac-1 may arise as a key contributor to other available tools to fight malaria by itself and/or by complementing other effective vaccines readily available, or soon in the market, targeting the liver stage, thereby extending protection against any potential parasite escaping the pre-erythrocytic immunological coverage.
Follow the Topic
Microbiology
Life Sciences > Biological Sciences > Microbiology
-
npj Vaccines
A multidisciplinary journal that is dedicated to publishing the finest and high-quality research and development on human and veterinary vaccines.
Related Collections
With Collections, you can get published faster and increase your visibility.
Therapeutic HPV vaccines
Therapeutic Human papillomavirus (HPV) vaccines are considered to be a promising approach to intercept the development of HPV-driven cancers in already HPV-infected people. This collection aims to gather the state of the art of therapeutic HPV vaccine research – from novel vaccine design concepts, to preclinical models, to results of clinical trials.
Publishing Model: Open Access
Deadline: Jun 30, 2026




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in