Getting People Vaccinated: The impact of social conformity
Published in Healthcare & Nursing
People’s reluctance to be vaccinated has been one of the largest public policy stumbling blocks in the current Covid-19 pandemic. Yet Covid-19 vaccine hesitancy is merely the latest in a long line of visceral aversions towards novel technologies - from eating genetically-modified foods to drinking recycled water.
Specific to vaccines, past research has demonstrated this effect for vaccines for HPV and the influenza A (H1N1) virus. In the current pandemic, hesitancy has been mapped across the world - in a survey of 13,426 people across 19 countries, only 47% reported that they “completely agree” with getting a Covid-19 vaccine.
An interesting question arises about Covid-19 vaccines using the relatively newer mRNA technology – these are more effective than vaccines produced using conventional technology, but how much does the novelty of its technology affect vaccine hesitancy? Second, what if anything, can reduce this hesitancy?
Answering these questions will help governments manage mass vaccination programmes better, not just in the current pandemic, but for future mass outbreaks.
Our study has two main goals. The first is to determine the extent of increased hesitancy toward novel mRNA vaccines. We anticipate people will be more hesitant due to the novelty of the mRNA vaccine technology, which we call a “novelty penalty.” This term was first coined by psychologists to refer to people’s preference for familiar experiences over novel ones.
Our second is to investigate forces that may reduce vaccine hesitancy. Would a person’s willingness to get vaccinated increase dramatically if the person found out that many members of the community had already been vaccinated? What level of vaccination would be required to trigger this dramatic increase? Such bandwagon effects, if proven, will provide governments with a powerful policy instrument against the pandemic.
We surveyed 35,180 adults in nine of the most populated countries in the Americas (Brazil, Mexico, and the United States of America), Asia (China, India, and Indonesia) and Europe (Germany, Russia, and the United Kingdom. We asked about people’s confidence in vaccines in general (based on four questions used in the Wellcome Global Monitor study28), and their willingness to receive a Covid-19 vaccine if it were provided for free.
First, our study shows that the overall proportion of people indicating they are “very likely” to get vaccinated is around 50%, well below the 84% to 90% level needed for herd immunity. However, our study was conducted at the start of vaccination programs when people were still cautious about vaccines. Now that the programs have proven highly successful, especially in developed countries, we expect a significant increase in the proportion of people “very likely” to get vaccinated.
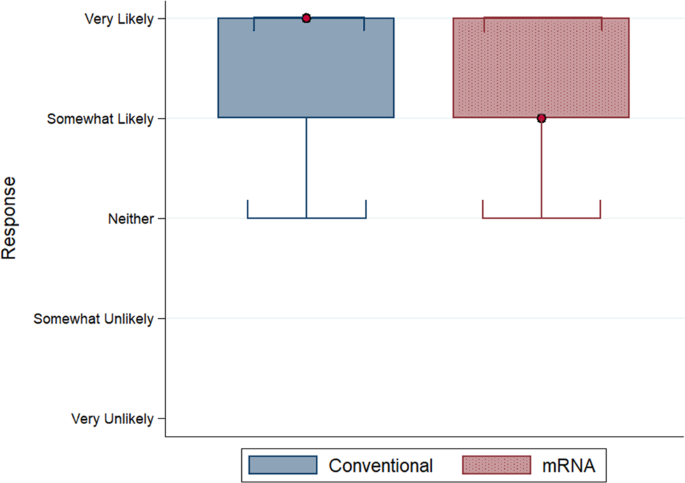
Second, our study shows that the difference between people’s willingness to get the mRNA vaccine is only 3.4% lower than their willingness to get the conventional vaccine. Given the much higher level of efficacy of an mRNA vaccine (94%-95%) when compared to a conventional vaccine (below 70%), herd immunity achieved through vaccinations may be more likely in countries offering an mRNA vaccine.
Next, we asked three questions relating to subjects’ willingness to accept Covid-19 vaccines. First, we asked for the likelihood of Covid-19 vaccine acceptance before showing a hypothetical adoption rate in the country; second, we asked the same question after randomly showing one of five hypothetical adoption rates in the country (0%, 20%, 40%, 60%, 80%); and finally, we asked the likelihood of subjects recommending getting a Covid-19 vaccine to their loved ones.
When no one in the country is vaccinated, only 31.7% of people responded that they are very likely to get an mRNA vaccine for Covid-19 and 35.1% a conventional vaccine. Upon learning that 20% of their peers have been vaccinated, the proportion jumps to 49.6% for an mRNA vaccine and 52.4% for a conventional vaccine. Above 20%, the proportion of people responding that they are very likely to receive the vaccine continues to increase although less dramatically.
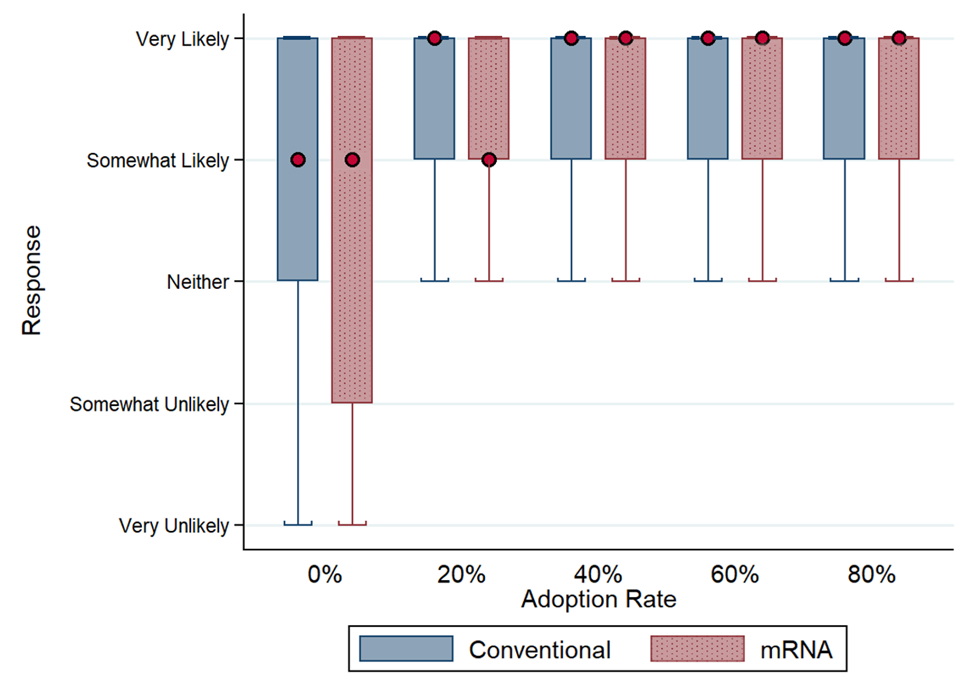
Figure1: Shows how the adoption rate is influenced by a small number of people agreeing to take the vaccine.
Overall, therefore, we show that the novelty of the mRNA vaccine technology reduces the odds of a higher level of vaccine acceptance by 14.2% (odds ratio 0.858; p < 0.001). On the other hand, we find that social conformity reduces vaccine hesitancy. At a 0% inoculation rate, 31.7% report that they are “very likely” to get an mRNA vaccine while at a 20% inoculation rate, willingness jumps to 49.6%.
In short - the novelty of the mRNA vaccine increases hesitancy, but social conformity reduces it. A small group of early adopters can provide momentum for vaccination.
Poster image: A COVID-19 vaccination exercise held at Singapore’s National University Hospital in January 2021 [credit: National University Hospital]
Follow the Topic
-
Communications Medicine
A selective open access journal from Nature Portfolio publishing high-quality research, reviews and commentary across all clinical, translational, and public health research fields.
Related Collections
With Collections, you can get published faster and increase your visibility.
Public health and health governance in China
Publishing Model: Open Access
Deadline: Jul 31, 2026
Life Course Epidemiology
Publishing Model: Open Access
Deadline: Jun 30, 2026



Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in