How the immune defect and epithelial defect contribute to CF
Published in Microbiology
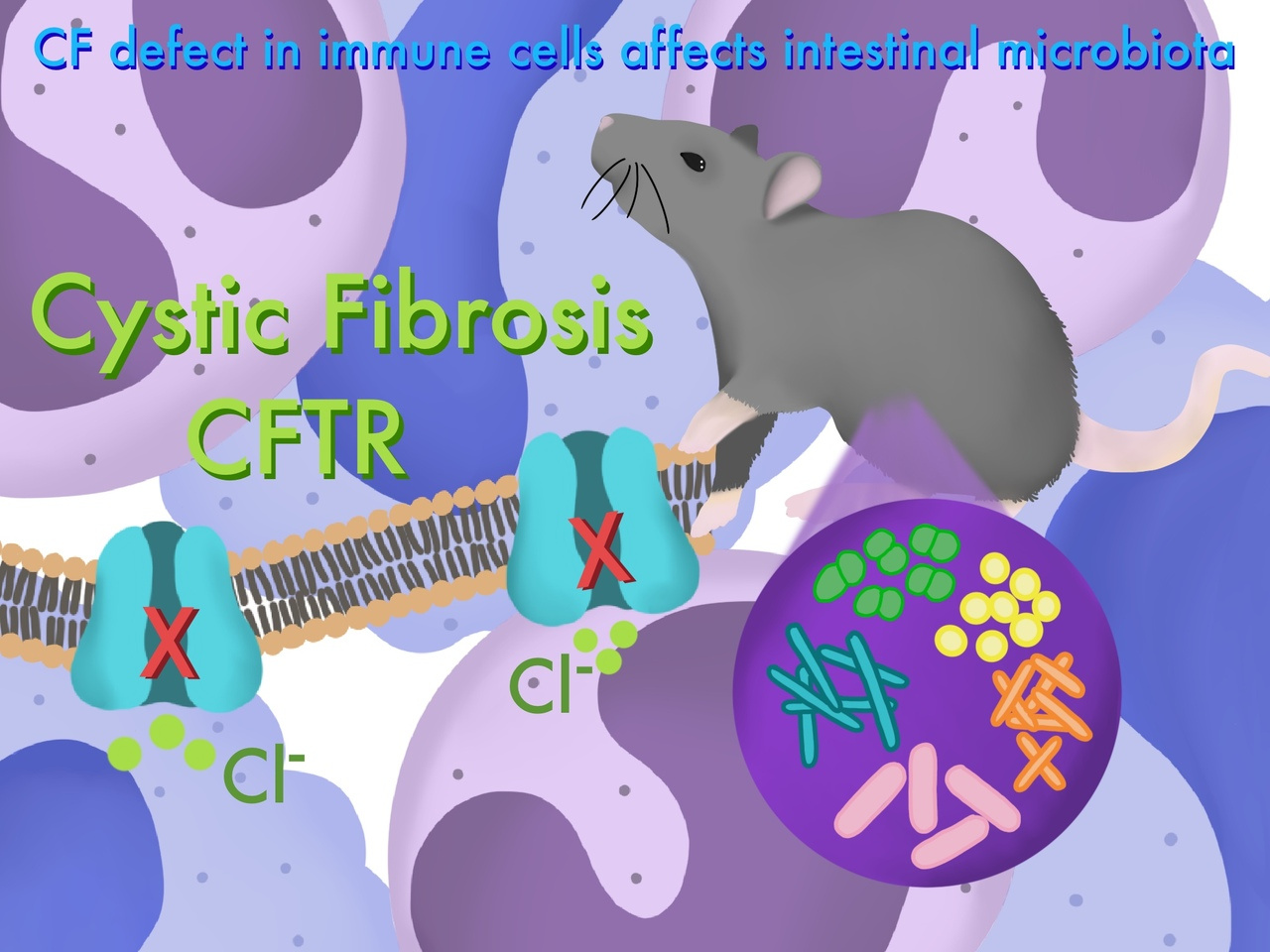
Cystic fibrosis…..not just a lung disease.
Cystic fibrosis (CF) is a genetic disease that affects ~100,000 people worldwide and ~40,000 people in the United States. It mainly affects Caucasians, with 1 in 3000 babies being born with CF. Other demographics are affected by CF as well, with 1 in 17,000 African Americans and 1 in 31,000 Asian American babies being affected. This disease is caused by mutations in the cystic fibrosis transmembrane conductance regulator (cftr) gene, which encodes a chloride channel.
Clinically, adult CF patients typically suffer from severe lung disease, which often requires life-long treatments and sometimes, even lung transplants. Yet, what’s far less known, is that individuals with CF develop intestinal problems before and after birth. CF newborns have to be monitored closely for potential development of intestinal complications and blockage, called meconium ileus. If they do present with blockage, they must be treated urgently, to ensure survival. With the use of constant laxative supplementation, antibiotic regimens, and specialized diets, the intestinal component of CF disease is manageable, but constipation and distal intestinal obstruction syndrome persist through life. Furthermore, bacterial overgrowth in the small intestine (SI) and bacterial dysbiosis in the large intestine (LI) constitute a major condition in CF.
CF intestinal dysbiosis
Studies have looked at the microbiota of various CF models, from human, to rabbits, mice and ferrets. All studies conclusively state that CF individuals/models have an altered microbiota when compared to their healthy cohorts. Studies also found that they have less diversity in the bacterial taxa present, indicating an unhealthy gut milieu.
Our study investigated this matter from a different angle to address if the immune system had any part in the intestinal disease of CF.
Our lab generated 3 immune knockout mouse models to directly assess how the loss of CFTR on neutrophils (Neu-CF), macrophages (Mac-CF), and myeloid lineage cells (Mye-CF) contributed to the altered microbiota in CF mice. We found that the immune defect does play a role in influencing the intestinal microbiota, as the Neu-CF mice and Mye-CF mice had differing taxa when compared to WT mice.
We also saw that when CFTR was non-functional on all myeloid lineage cells (Mye-CF), the microbiota of these mice was more similar to the microbiota of CF mice (Pan-CF; whole body CFTR deletion) when measuring the bacterial population evenness (Shannon Index), and the phylogenetic diversity (Faith’s PD) of the bacterial taxa.
To take things a bit further, we performed bone marrow transplantation (BMT) on sibling CF and WT mice. This allowed us to control for any genetic differences in the mice. We created 3 BMT conditions: WT bone marrow (BM) given to WT mice (WT-to-WT); WT BM given to CF mice (WT-to-CF); and CF BM given to CF mice (CF-to-CF).
By doing this, we were able to directly assess how the immune defect contributes to changes in the microbiota by comparing WT-to-CF vs CF-to-CF. These mice have the same epithelia (CF) but now the WT-to-CF mice have a WT (CFTR+/+) immune system.
To compare how the epithelial defect contributes to the altered microbiota, we compared WT-to-WT vs WT-to-CF. These mice both have functional CFTR on their immune cells, but the CF mice (WT-to-CF) still have non-functional CFTR on their epithelia.
What we found was that the immune defect contributed the most to the altered gut microbiota in the small intestine. This suggests that the altered taxa seen in the small intestine is due to the ill functioning immune system. Interestingly, we also performed bacterial predictive functional analysis using PICRUSt2 and saw that when comparing WT-to-CF vs CF-to-CF mice, bacterial predictive functions involved in bacterial virulence were decreased in the WT-to-CF mice. Suggesting the healthy immune system selected for healthier and less virulent bacteria.
When looking at WT-to-WT vs WT-to-CF comparisons, we see that the epithelial defect contributed the most to the difference in taxa in the large intestine. Thus, both of these findings suggest that the immune defect and epithelial defect play a role in the altered gut microbiota seen in CF individuals and animal models.
Take away
Here, we see that both the epithelial defect and the immune defect contribute to the CF intestinal disease and need to be equally investigated in future studies. These findings help to broaden the current knowledge and scope of CF research today. By understanding how the loss of a functional CFTR contributes to altered immune function and influences the gut microbiome, scientists can continue to make bounds in finding a cure for CF.
Follow the Topic
-
Communications Biology

An open access journal from Nature Portfolio publishing high-quality research, reviews and commentary in all areas of the biological sciences, representing significant advances and bringing new biological insight to a specialized area of research.
Related Collections
With Collections, you can get published faster and increase your visibility.
From RNA Detection to Molecular Mechanisms
Publishing Model: Open Access
Deadline: May 05, 2026
Advances in neurodegenerative diseases
Publishing Model: Hybrid
Deadline: Jun 30, 2026

Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in