Low emissions, high burden: climate change and the spread of vector-borne disease
Published in Earth & Environment and Ecology & Evolution

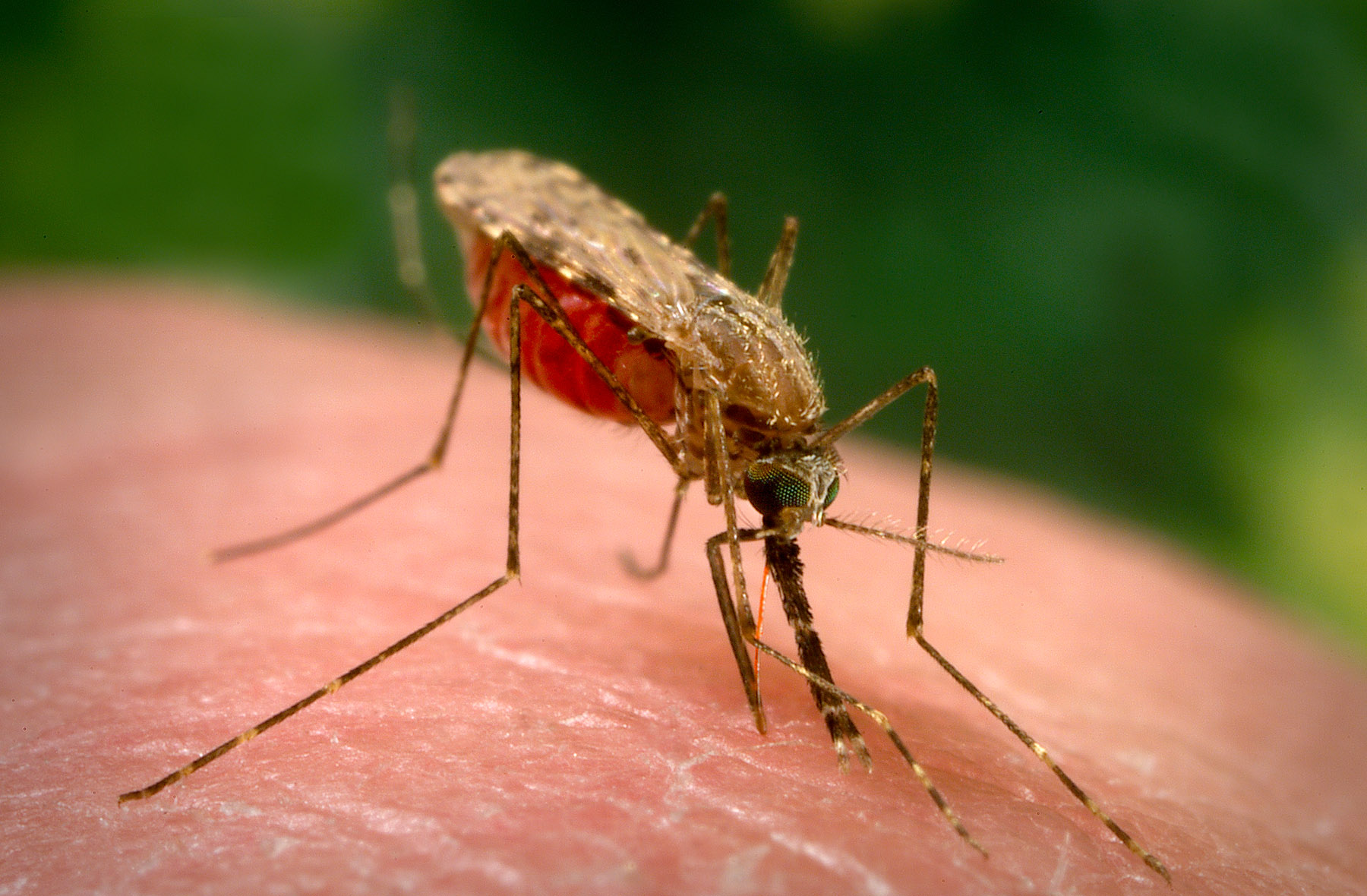
Featured image: Frederick Depuydt, CC BY-SA 4.0
Invertebrates, which includes mosquitoes, ticks, flies, and other vectors of disease, are ectothermic creatures. This means they are unable to regulate their own temperature, making them highly dependent on their surrounding environment.
In fact, climate, droughts, floods, and extreme weather can all significantly influence these vectors and the diseases they transmit:
- Warmer temperatures change their geographical distribution, leading diseases to new places, or decreasing the time pathogens need to reach their infectious stages.
- Milder winters mean ticks and mosquitoes are active longer in the year, increasing the risks of infection.
- Excess rainfall may produce countless breeding sites, while floods hinder control efforts and overwhelm health systems.
The climate crisis is redrawing the map of infectious disease, and the communities least responsible for greenhouse gas emissions are the ones watching vector-borne illnesses surge through their towns, hospitals, and communities.
The emissions gap
Countries like Pakistan, Bangladesh, Mozambique, Kenya, and Ethiopia each contribute a tiny fraction of global CO2 emissions. Pakistan, for instance, is responsible for roughly 1% of the world's carbon output. Many African nations emit less than 0.1 tonnes of CO₂ per person per year, compared with 14.2 tonnes in the United States, 14.5 tonnes in Australia, or 21 tonnes in Saudi Arabia just in 2024. Yet low emitters can be disproportionately affected by the environmental crisis – not because of what they've emitted, but because of where they are and how little their health systems can absorb the shock.
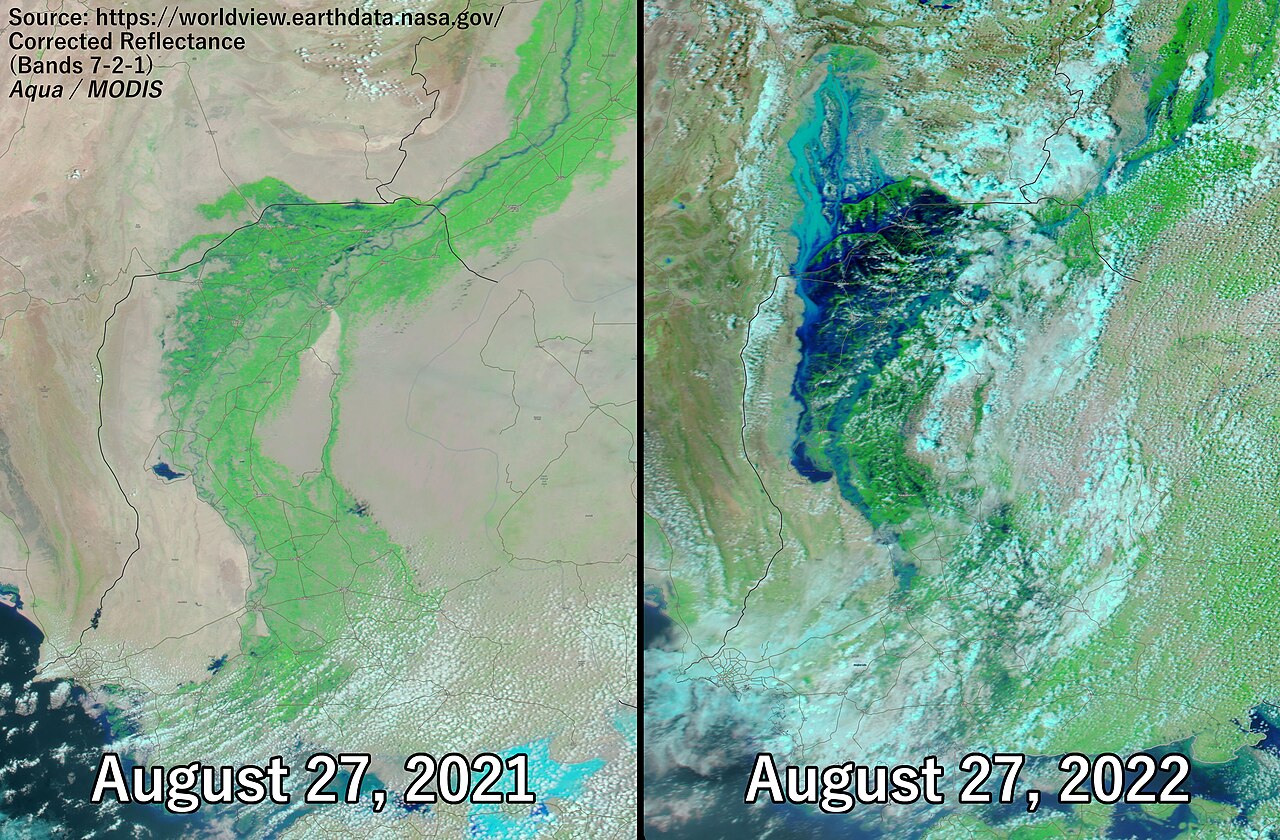
Pakistan: first came the floods, then came the outbreaks
In 2022, Pakistan experienced catastrophic flooding that submerged a third of the country, displacing 8 million people and causing over USD 30 billion in damages. The UN Secretary-General called it a “monsoon on steroids” . But the disaster didn't end when the rains stopped. Stagnant floodwaters turned into vast mosquito breeding grounds, triggering an alarming surge in malaria, from 500,000 to 2.6 million cases in a single year. Dengue cases spiked alongside, accounting for 75% of mosquito-borne illness in the Sindh province. The World Health Organization described it as “the perfect storm for malaria”.
Bangladesh: record-breaking dengue
Bangladesh, another low-emitter, recorded its deadliest dengue outbreak in history in 2023: over 321,000 hospitalisations and 1,705 deaths. This was the highest dengue death toll of any country that year. Scientists directly linked the severity to climate change: extended monsoons, out-of-season rainfall, and rising temperatures lengthened the breeding season for Aedes mosquitoes and pushed the disease far beyond the capital Dhaka into previously unaffected rural districts. The crisis continued into 2024, and over 400 more deaths were recorded.

East Africa: malaria up the highlands
In Kenya and Ethiopia, warming temperatures are pushing malaria-carrying mosquitoes into highland areas that were historically too cool for them. Communities around Nairobi and in Ethiopia's western highlands (where malaria was rare) are now reporting outbreaks. Ethiopia recorded over 7.3 million malaria cases in 2024 alone, the highest in seven years. These are populations with limited prior immunity and health systems that were never built to handle endemic malaria, making them especially vulnerable.
Mozambique: cyclone Freddy
Cyclone Freddy, was one of the longest-lasting tropical cyclones ever recorded. When it struck Mozambique in 2023, the immediate destruction was followed by surging cholera and malaria. Damaged water infrastructure, flooded sanitation systems, and displaced populations created ideal conditions for disease transmission. Malawi was also severely affected by cholera outbreaks, after “the equivalent of six months of rainfall in six days” which resulted flash floods washing away homes and crops, and weakening hygiene and sanitation systems.

What can be done?
A 2025 Oxford University study warned of a “creeping catastrophe”, not a single dramatic event, but a slow, compounding rise in climate-sensitive infectious diseases across the Global South. Of course, climate change attributions may be tricky to identify, as they can be complex and difficult to disentangle from other factors. Studies like those by Erazo and colleagues, looking at the expansion of West Nile virus in Europe and at malaria in East Africa, are interesting examples of how it can be done.
Climate justice demands that high-emitting nations take responsibility for the consequences of their (in)actions, invest meaningfully in adaptation, and support funding for vulnerable countries to lead their own research, surveillance, and public health responses. Crucially, that support must respect local leadership. As Pai and colleagues argue, meaningful change requires the Global South to lead, not merely receive aid shaped by distant priorities.
The countries highlighted here are not isolated cases. Across the Global South, from islands facing rising seas to Latin American cities battling record-shattering dengue, the pattern is the same: those who emitted the least are adapting the hardest. What is needed is climate-informed disease surveillance, locally led research capacity, and health systems resilient enough to absorb repeated shocks.
Follow the Topic
-
BugBitten
A blog for the parasitology and vector biology community.






Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in