Single-shot 3D photoacoustic tomography based on a single-element detector for ultrafast imaging of hemodynamics
Published in Bioengineering & Biotechnology

Vascular diseases like atherosclerosis, blood clots, aneurysms, and poor blood circulation in the lower extremities are significant health hazards. These conditions can lead to severe outcomes such as heart attacks, strokes, and even organ failure. They are particularly risky for diabetic patients, potentially causing serious leg and foot complications, including amputation. Early detection is essential, making the use of imaging technologies that visualize blood flow—known as “hemodynamics”—critical. These imaging technologies help diagnose, treat, and prevent vascular diseases. Additionally, they offer ways to evaluate the effectiveness of drugs and surgeries and help to personalize future treatment options.
Traditionally, healthcare providers use imaging technologies like magnetic resonance imaging (MRI), x-ray computed tomography (CT) angiography, and positron emission tomography (PET) to study blood vessels and blood flow. However, these methods often expose patients to potentially harmful radiation or require the undesirable injection of contrast agents. Additionally, these machines are generally unwieldy and expensive, making them difficult to deploy in smaller healthcare settings or mobile clinics.
Optical imaging techniques like fluorescence imaging and optical coherence tomography (OCT) offer non-invasive ways to visualize hemodynamics. However, these methods provide only penetration up to ~1–2 mm into tissues, and they are not particularly good at highlighting blood-specific factors like hemoglobin. Doppler ultrasound, another option, requires a large number of detector elements and data acquisition channels.
In this context, photoacoustic tomography (PAT) emerges as a promising alternative. Unlike other techniques, it avoids the use of harmful radiation or injection of chemicals. Instead, it relies on the photoacoustic effect, where optical absorbers like hemoglobin in tissues absorb light and emit ultrasonic waves. These waves are captured and used to construct high-resolution images at depths far greater than 1 mm. Two primary variations of PAT exist: photoacoustic microscopy (PAM) and photoacoustic computed tomography (PACT). While PAM offers simplicity at lower imaging speeds, PACT is faster but more complex and costly.
To make PACT systems simpler, cheaper, and smaller, researchers have been trying to use fewer sensors to acquire 3D images. Existing approaches like “compressed sensing” can function with just one sensor, but they are time-consuming as they require multiple, sequential measurements. Newer techniques have been developed that use an “ergodic relay” to quickly capture images with fewer sensors; however, these are generally limited to 2D imaging and need frequent recalibration, making them unsuitable for long-term usage.
To overcome these challenges, we have developed a new technique called photoacoustic computed tomography through an ergodic relay (PACTER). This innovative technique offers a non-invasive, efficient, and cost-effective solution for detailed hemodynamic imaging. Notably, PACTER uses a single-element detector but achieves the performance equivalent to that of a PACT system based on thousands of actual detector elements. Enabled by the integrated ultrasonic transducer and the object-independent universal calibration, the system only needs to be calibrated once and is suitable for long-term imaging in changing environments.
In PACTER, a single-element detector gathers the information normally collected by thousands of physical detectors (Figure 1a). This design allows for 3D imaging of blood vessels using just a single laser pulse, enabling real-time capture of fast-changing blood dynamics. Traditionally, a single-element ultrasonic transducer can only acquire a 1D signal in the time domain (Figure 1b). However, PACTER can use the single-element transducer to encode spatiotemporal information equivalent to those captured by thousands of detectors, which can then be used to reconstruct a 3D map of the optical absorbers in the imaging volume. With a kilohertz laser repetition rate, PACTER can use the 1D (in time) signals to generate a thousand 3D (in space) volumes per second, leading to a high-speed 4D (in space and time) image of optical absorption in, e.g., blood vessels in human palms (Figure 1c).
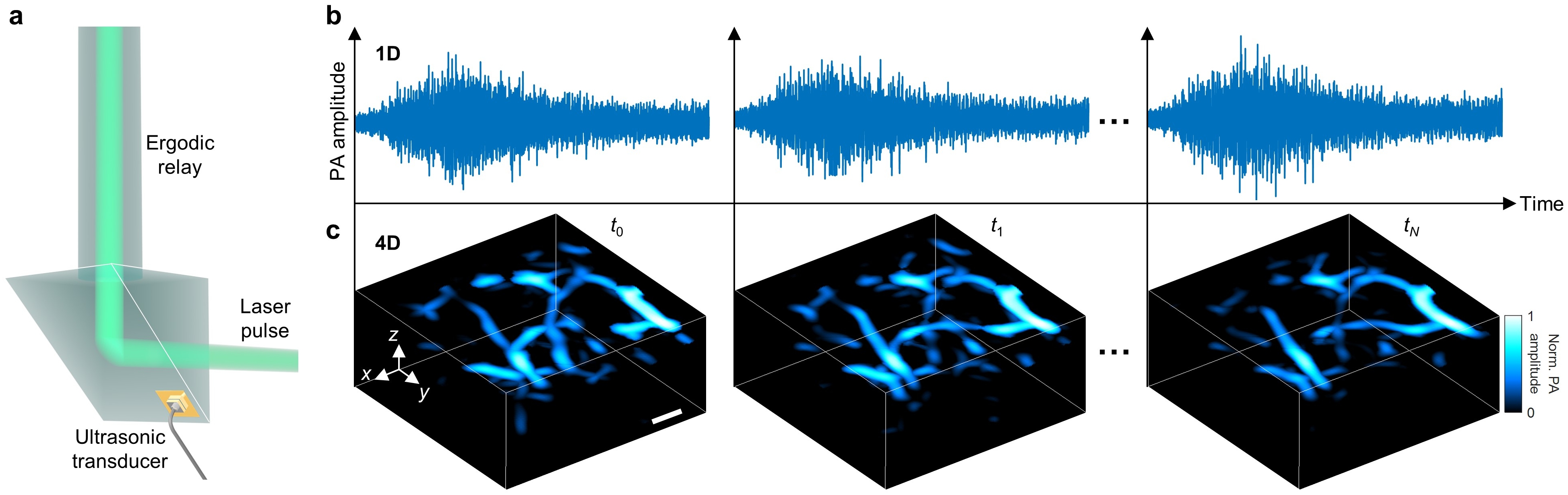
Figure 1 PACTER. a, Schematic of the single-element ultrasonic transducer in PACTER. b, 1D (in time) PACTER signals detected by the ultrasonic transducer at different time instances. c, Reconstructed 3D images of human palmar vessels from the corresponding signals in b. Norm., normalized. Scale bar, 1 mm.
Our PACTER system has shown promise in monitoring vital signs in small animals and in visualizing blood flow changes in human extremities. It can even detect the subtle differences in blood flow speed when the blood supply is artificially blocked and released, showing its potential as a powerful tool for assessing vascular health in the limbs. Because the system uses a single-element detector, it is far more affordable and compact than traditional setups. This feature improves the accessibility of the technology for various applications, from home-care monitoring to use in intensive care units.
The PACTER system's innovative design opens new doors in the diagnosis and treatment of vascular diseases, offering a more personalized approach to healthcare. Beyond its immediate application in vascular imaging, the core technology could also find uses in other imaging domains like ultrasonography, sonar, and radar. Overall, PACTER stands as a transformative solution that promises to advance both the quality and accessibility of healthcare.
These results were recently published in Nature Biomedical Engineering: Y. Zhang, P. Hu, L. Li, R. Cao, A. Khadria, K. Maslov, X. Tong, Y. Zeng, L. Jiang, Q. Zhou, and L. V. Wang, “Ultrafast longitudinal imaging of haemodynamics via single-shot volumetric photoacoustic tomography with a single-element detector”, Nature Biomedical Engineering, 2023, 10.1038/s41551-023-01149-4.
Follow the Topic
-
Nature Biomedical Engineering
This journal aspires to become the most prominent publishing venue in biomedical engineering by bringing together the most important advances in the discipline, enhancing their visibility, and providing overviews of the state of the art in each field.
Related Collections
With Collections, you can get published faster and increase your visibility.
Implantable wireless communication technologies
Publishing Model: Hybrid
Deadline: Nov 28, 2026
Microphysiological systems for advanced modeling, high-throughput evaluation, and clinical translation
Publishing Model: Hybrid
Deadline: Dec 30, 2026





Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in